Abstract
Introduction
Transient splenium corporis callosi (SCC) lesions are related to rapid reduction of antiepileptic drugs (AEDs). The range of substances with predilection for SCC changes, their pathophysiology and their occurrence are still unknown.
Methods
In a prospective 2-year study an epilepsy-dedicated MRI protocol supplemented by DWI and ADC maps was performed after AED withdrawal for diagnostic seizure provocation in all patients with pharmacoresistant seizures locally admitted to the Department of Epileptology.
Results
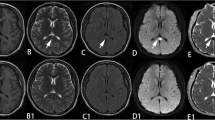
Of 891 presurgical epilepsy patients, 6 (0.7%) had SCC lesions with cytotoxic edema on DWI. Carbamazepine combined with other AEDs was administered in five of those patients. In the study period we observed identical lesions in a schizophrenic patient treated with olanzapine and citalopram, in a patient with oropharyngeal carcinoma treated with alkylating agents, and in a hypernatremic patient following neurohypophyseal granular cell tumor surgery.
Conclusion
Transient SCC lesions are related to rapid AED reduction but may occur in similar conditions with fluid balance alterations. We contribute further clinical data in this field to better classify the pharmaceuticals that are prone to the described cerebral cytotoxic side effects in the SCC and to clarify their incidence among presurgical epilepsy patients.


Similar content being viewed by others
References
Urbach H, Hattingen J, von OJ, Luyken C, Clusmann H, Kral T, Kurthen M, Schramm J, Blumcke I, Schild HH (2004) MR imaging in the presurgical workup of patients with drug-resistant epilepsy. AJNR Am J Neuroradiol 25:919–926
Kim SS, Chang KH, Kim ST, Suh DC, Cheon JE, Jeong SW, Han MH, Lee SK (1999) Focal lesion in the splenium of the corpus callosum in epileptic patients: antiepileptic drug toxicity? AJNR Am J Neuroradiol 20:125–129
Polster T, Hoppe M, Ebner A (2001) Transient lesion in the splenium of the corpus callosum: three further cases in epileptic patients and a pathophysiological hypothesis. J Neurol Neurosurg Psychiatry 70:459–463
Cohen-Gadol AA, Britton JW, Jack CR Jr, Friedman JA, Marsh WR (2002) Transient postictal magnetic resonance imaging abnormality of the corpus callosum in a patient with epilepsy. Case report and review of the literature. J Neurosurg 97:714–717
Oster J, Doherty C, Grant PE, Simon M, Cole AJ (2003) Diffusion-weighted imaging abnormalities in the splenium after seizures. Epilepsia 44:852–854
Mirsattari SM, Lee DH, Jones MW, Blume WT (2003) Transient lesion in the splenium of the corpus callosum in an epileptic patient. Neurology 60:1838–1841
Maeda M, Shiroyama T, Tsukahara H, Shimono T, Aoki S, Takeda K (2003) Transient splenial lesion of the corpus callosum associated with antiepileptic drugs: evaluation by diffusion-weighted MR imaging. Eur Radiol 13:1902–1906
Doherty MJ, Jayadev S, Watson NF, Konchada RS, Hallam DK (2005) Clinical implications of splenium magnetic resonance imaging signal changes. Arch Neurol 62:433–437
Friese SA, Bitzer M, Freudenstein D, Voigt K, Kuker W (2000) Classification of acquired lesions of the corpus callosum with MRI. Neuroradiology 42:795–802
Tada H, Takanashi J, Barkovich AJ, Oba H, Maeda M, Tsukahara H, Suzuki M, Yamamoto T, Shimono T, Ichiyama T, Taoka T, Sohma O, Yoshikawa H, Kohno Y (2004) Clinically mild encephalitis/encephalopathy with a reversible splenial lesion. Neurology 63:1854–1858
Nasrallah K, Silver B (2005) Hyponatremia associated with repeated use of levetiracetam. Epilepsia 46:972–973
Arnaout MS, Antun FP, Ashkar K (2001) Neuroleptic malignant syndrome with olanzapine associated with severe hypernatremia. Hum Psychopharmacol 16:279–281
Horak EL, Jenkins AJ (2005) Postmortem tissue distribution of olanzapine and citalopram in a drug intoxication. J Forensic Sci 50:679–681
Ogura H, Takaoka M, Kishi M, Kimoto M, Shimazu T, Yoshioka T, Sugimoto H (1998) Reversible MR findings of hemolytic uremic syndrome with mild encephalopathy. AJNR Am J Neuroradiol 19:1144–1145
Signorini E, Lucchi S, Mastrangelo M, Rapuzzi S, Edefonti A, Fossali E (2000) Central nervous system involvement in a child with hemolytic uremic syndrome. Pediatr Nephrol 14:990–992
Kobata R, Tsukahara H, Nakai A, Tanizawa A, Ishimori Y, Kawamura Y, Ushijima H, Mayumi M (2002) Transient MR signal changes in the splenium of the corpus callosum in rotavirus encephalopathy: value of diffusion-weighted imaging. J Comput Assist Tomogr 26:825–828
Takanashi J, Barkovich AJ, Yamaguchi K, Kohno Y (2004) Influenza-associated encephalitis/encephalopathy with a reversible lesion in the splenium of the corpus callosum: a case report and literature review. AJNR Am J Neuroradiol 25:798–802
Hlaihel C, Gonnaud PM, Champin S, Rousset H, Tran-Minh VA, Cotton F (2005) Diffusion-weighted magnetic resonance imaging in Marchiafava-Bignami disease: follow-up studies. Neuroradiology 47:520–524
Kobuchi N, Tsukahara H, Kawamura Y, Ishimori Y, Ohshima Y, Hiraoka M, Hiraizumi Y, Ueno M, Mayumi M (2003) Reversible diffusion-weighted MR findings of Salmonella enteritidis-associated encephalopathy. Eur Neurol 49:182–184
Kato Z, Kozawa R, Hashimoto K, Kondo N (2003) Transient lesion in the splenium of the corpus callosum in acute cerebellitis. J Child Neurol 18:291–292
Tha KK, Terae S, Sugiura M, Nishioka T, Oka M, Kudoh K, Kaneko K, Miyasaka K (2002) Diffusion-weighted magnetic resonance imaging in early stage of 5-fluorouracil-induced leukoencephalopathy. Acta Neurol Scand 106:379–386
Hackett PH, Yarnell PR, Hill R, Reynard K, Heit J, McCormick J (1998) High-altitude cerebral edema evaluated with magnetic resonance imaging: clinical correlation and pathophysiology. JAMA 280:1920–1925
Wong SH, Turner N, Birchall D, Walls TJ, English P, Schmid ML (2004) Reversible abnormalities of DWI in high-altitude cerebral edema. Neurology 62:335–336
Oaklander AL, Buchbinder BR (2005) Pregabalin-withdrawal encephalopathy and splenial edema: a link to high-altitude illness? Ann Neurol 58:309–312
Takayama H, Kobayashi M, Sugishita M, Mihara B (2000) Diffusion-weighted imaging demonstrates transient cytotoxic edema involving the corpus callosum in a patient with diffuse brain injury. Clin Neurol Neurosurg 102:135–139
Cordoliani YS, Sarrazin JL, Felten D, Caumes E, Leveque C, Fisch A (1998) MR of cerebral malaria. AJNR Am J Neuroradiol 19:871–874
Mito Y, Yoshida K, Kikuchi S (2002) Measles encephalitis with peculiar MRI findings. Neurol Med 56:251–256
Yamashita N, Tsukahara H, Kawamura Y, et al (2002) Reversible MR findings of Salmonella enteritidis-associated encephalopathy (in Japanese). Infect Immun Child 14:57
Kieburtz KD, Ketonen L, Zettelmaier AE, Kido D, Caine ED, Simon JH (1990) Magnetic resonance imaging findings in HIV cognitive impairment. Arch Neurol 47:643–645
Gass A, Birtsch G, Olster M, Schwartz A, Hennerici MG (1998) Marchiafava-Bignami disease: reversibility of neuroimaging abnormality. J Comput Assist Tomogr 22:503–504
Kawamura M, Shiota J, Yagishita T, Hirayama K (1985) Marchiafava-Bignami disease: computed tomographic scan and magnetic resonance imaging. Ann Neurol 18:103–104
Chang KH, Cha SH, Han MH, Park SH, Nah DL, Hong JH (1992) Marchiafava-Bignami disease: serial changes in corpus callosum on MRI. Neuroradiology 34:480–482
Caparros-Lefebvre D, Pruvo JP, Josien E, Pertuzon B, Clarisse J, Petit H (1994) Marchiafava-Bignami disease: use of contrast media in CT and MRI. Neuroradiology 36:509–511
Ruiz-Martinez J, Martinez Perez-Balsa A, Ruibal M, Urtasun M, Villanua J, Marti Masso JF (1999) Marchiafava-Bignami disease with widespread extracallosal lesions and favourable course. Neuroradiology 41:40–43
Gambini A, Falini A, Moiola L, Comi G, Scotti G (2003) Marchiafava-Bignami disease: longitudinal MR imaging and MR spectroscopy study. AJNR Am J Neuroradiol 24:249–253
Mendelsohn DB, Levin HS, Harward H, Bruce D (1992) Corpus callosum lesions after closed head injury in children: MRI, clinical features and outcome. Neuroradiology 34:384–388
Conflict of interest statement
We declare that we have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nelles, M., Bien, C.G., Kurthen, M. et al. Transient splenium lesions in presurgical epilepsy patients: incidence and pathogenesis. Neuroradiology 48, 443–448 (2006). https://doi.org/10.1007/s00234-006-0080-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-006-0080-5