Abstract
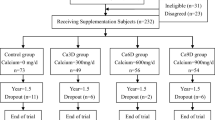
Diet and physical activity (PA) influence bone health in children. This study tested whether increasing milk and milk products and weight-bearing types of PA favorably changed bone outcomes assessed by dual-energy X-ray absorptiometry (DXA) and bone biomarkers in children with obesity participating in a 1-year family-centered lifestyle intervention. Children were randomized to one of three groups: Control (Ctrl; no intervention), Standard treatment (StnTx: two servings milk and milk products/day; meet PA guidelines plus weight-bearing PA three times/week), or Modified treatment (ModTx: four servings milk and milk products/day; meet PA guidelines plus daily weight-bearing PA). Baseline and 12-month measurements included DXA scans for whole body (WB), lumbar spine (LS), lumbar lateral spine (LLS), and ultra-distal (UD) ulna + radius for bone mineral content (BMC), areal bone mineral density (aBMD) and BMD z-scores. Fat mass index (FMI), fat-free mass index (FFMI), and biomarkers of bone metabolism were assessed. Seventy-eight children 6–8 years old were recruited (mean body mass index for-age z-score: 3.3 ± 1.2). Compared to baseline, all groups increased BMC of WB, LS, and LLS (p < 0.001), whereas only StnTx increased UD ulna + radius BMC at 12 months (p < 0.05). At 12 months, WB-BMD z-scores were significantly lower in Ctrl (p < 0.05), whereas WB and LLS aBMD increased in StnTx and ModTx (p < 0.001) but not in Ctrl. All groups increased FFMI (p < 0.001), while only Ctrl increased FMI (p < 0.001). Bone biomarkers did not change over time. Participating in a family-centered lifestyle intervention based on Canadian diet and PA guidelines maintained bone health in obese children.



Similar content being viewed by others
References
Julian-Almarcegui C, Gomez-Cabello A, Huybrechts I, Gonzalez-Aguero A, Kaufman JM, Casajus JA et al (2015) Combined effects of interaction between physical activity and nutrition on bone health in children and adolescents: a systematic review. Nutr Rev 73:127–139
Gurnani M, Birken C, Hamilton J (2015) Childhood obesity: causes, consequences, and management. Pediatr Clin North Am 62:821–840
Farr JN, Dimitri P (2016) The impact of fat and obesity on bone microarchitecture and strength in children. Calcif Tissue Int 100:500–513
Smith SM, Sumar B, Dixon KA (2014) Musculoskeletal pain in overweight and obese children. Int J Obes 38:11–15
Viljakainen HT, Pekkinen M, Saarnio E, Karp H, Lamberg-Allardt C, Makitie O (2011) Dual effect of adipose tissue on bone health during growth. Bone 48:212–217
Sioen I, Lust E, De Henauw S, Moreno LA, Jimenez-Pavon D (2016) Associations between body composition and bone health in children and adolescents: a systematic review. Calcif Tissue Int 99:557–577
Clark EM, Ness AR, Tobias JH (2006) Adipose tissue stimulates bone growth in prepubertal children. J Clin Endocrinol Metab 91:2534–2541
Rocher E, Chappard C, Jaffre C, Benhamou CL, Courteix D (2008) Bone mineral density in prepubertal obese and control children: relation to body weight, lean mass, and fat mass. J Bone Miner Metab 26:73–78
Goulding A, Taylor RW, Jones IE, McAuley KA, Manning PJ, Williams SM (2000) Overweight and obese children have low bone mass and area for their weight. Int J Obes Relat Metab Disord 24:627–632
Dimitri P, Jacques RM, Paggiosi M, King D, Walsh J, Taylor ZA et al (2015) Leptin may play a role in bone microstructural alterations in obese children. J Clin Endocrinol Metab 100:594–602
Cole ZA, Harvey NC, Kim M, Ntani G, Robinson SM, Inskip HM et al (2012) Increased fat mass is associated with increased bone size but reduced volumetric density in pre pubertal children. Bone 50:562–567
Yang L, Grey V (2006) Pediatric reference intervals for bone markers. Clin Biochem 39:561–568
Gajewska J, Weker H, Ambroszkiewicz J, Szamotulska K, Chelchowska M, Franek E et al (2013) Alterations in markers of bone metabolism and adipokines following a 3-month lifestyle intervention induced weight loss in obese prepubertal children. Exp Clin Endocrinol Diabetes 121:498–504
Reinehr T, Roth CL (2010) A new link between skeleton, obesity and insulin resistance: relationships between osteocalcin, leptin and insulin resistance in obese children before and after weight loss. Int J Obes 34:852–858
Rochefort GY, Rocher E, Aveline PC, Garnero P, Bab I, Chappard C et al (2011) Osteocalcin-insulin relationship in obese children: a role for the skeleton in energy metabolism. Clin Endocrinol 75:265–270
Gajewska J, Klemarczyk W, Ambroszkiewicz J, Szamotulska K, Chelchowska M, Weker H (2015) Associations between IGF-I, IGF-binding proteins and bone turnover markers in prepubertal obese children. J Pediatr Endocrinol Metab 28:563–569
Dimitri P, Wales JK, Bishop N (2011) Adipokines, bone-derived factors and bone turnover in obese children; evidence for altered fat-bone signalling resulting in reduced bone mass. Bone 48:189–196
Melamed ML, Kumar J (2010) Low levels of 25-hydroxyvitamin D in the pediatric populations: prevalence and clinical outcomes. Pediatric health 4:89–97
Reinehr T, de Sousa G, Alexy U, Kersting M, Andler W (2007) Vitamin D status and parathyroid hormone in obese children before and after weight loss. Eur J Endocrinol 157:225–232
Cohen TR, Hazell TJ, Vanstone CA, Rodd C, Weiler HA (2016) A family-centered lifestyle intervention for obese 6–8 year-old children: results from a one-year randomized controlled trial conducted in Montreal, Canada. Can J Public Health 107:e453–e460
World Health Organization (2012) Growth reference data for 5–19 years, Geneva, Switzerland. [http://www.who.int/growthref/en/]. Accessed 17 Aug 2017
Cohen TR, Hazell TJ, Vanstone CA, Plourde H, Rodd CJ, Weiler HA (2013) A family-centered lifestyle intervention to improve body composition and bone mass in overweight and obese children 6 through 8 years: a randomized controlled trial study protocol. BMC Public Health 13:383
Health Canada (2011) Canada’s Food Guide to Healthy Eating, Ottawa, ON, Canada. [https://www.canada.ca/en/health-canada/services/canada-food-guides.html]. Accessed 17 Aug 17 2017
Canadian Society for Exericse Physiology (2015) Canadian physical activity guidelines for children 5–11. Ottawa, ON, Canada. [http://www.csep.ca/cmfiles/guidelines/csep_guidelines_handbook.pdf]. Accessed 17 Aug 2017
World Health Organization (2009) AnthroPlus for personal computers manual: software for assessing growth of the world’s children and adolescents, Geneva, Switzerland. [http://www.who.int/growthref/tools/who_anthroplus_manual.pdf]. Accessed 8 Aug 2017
Tanner JM (1962) Growth at adolescence. Blackwell Scientific, Oxford
Carter DR, Bouxsein ML, Marcus R (1992) New approaches for interpreting projected bone densitometry data. J Bone Miner Res 7:137–145
Crocker PR, Bailey DA, Faulkner RA, Kowalski KC, McGrath R (1997) Measuring general levels of physical activity: preliminary evidence for the Physical Activity Questionnaire for Older Children. Med Sci Sports Exerc 29:1344–1349
Bass S, Delmas PD, Pearce G, Hendrich E, Tabensky A, Seeman E (1999) The differing tempo of growth in bone size, mass, and density in girls is region-specific. J Clin Invest 104:795–804
Goulding A, Taylor RW, Jones IE, Manning PJ, Williams SM (2002) Spinal overload: a concern for obese children and adolescents? Osteoporos Int 13:835–840
Sung-Chan P, Sung YW, Zhao X, Brownson RC (2013) Family-based models for childhood-obesity intervention: a systematic review of randomized controlled trials. Obes Rev 14:265–278
Statistics Canada (2015) Directly measured physical activity of children and youth, 2012 and 2013. Ottawa, ON, Canada. [http://www.statcan.gc.ca/pub/82-625-x/2015001/article/14136-eng.htm]. Accessed 17 Aug 2017
Zibellini J, Seimon RV, Lee CM, Gibson AA, Hsu MS, Shapses SA et al (2015) Does diet-induced weight loss lead to bone loss in overweight or obese adults? a systematic review and meta-analysis of clinical trials. J Bone Miner Res 30:2168–2178
Calvo MS, Eyre DR, Gundberg CM (1996) Molecular basis and clinical application of biological markers of bone turnover. Endocr Rev 17:333–368
Wang JW, Tang QY, Ruan HJ, Cai W (2014) Relation between serum osteocalcin levels and body composition in obese children. J Pediatr Gastroenterol Nutr 58:729–732
Burrows T, Golley RK, Khambalia A, McNaughton SA, Magarey A, Rosenkranz RR et al (2012) The quality of dietary intake methodology and reporting in child and adolescent obesity intervention trials: a systematic review. Obes Rev 13:1125–1138
Livingstone MB, Robson PJ, Wallace JM (2004) Issues in dietary intake assessment of children and adolescents. Br J Nutr 92(Suppl 2):S213–S222
Lichtman SW, Pisarska K, Berman ER, Pestone M, Dowling H, Offenbacher E et al (1992) Discrepancy between self-reported and actual caloric intake and exercise in obese subjects. N Engl J Med 327:1893–1898
Acknowledgements
The authors would like to thank Sherry Agellon for her work with the biomarkers. This study was supported by an operating grant from the Dairy Research Cluster Initiative (Dairy Farmers of Canada, Agriculture and Agri-Food Canada, and the Canadian Dairy Commission). TC is supported by Frederick Banting and Charles Best Canada Graduate Doctoral Award (Canadian Institutes of Health Research). HW is supported by funding from the Canada Research Chairs Program and the Canada Foundation for Innovation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
Tamara R. Cohen, Tom J. Hazell, Catherine A. Vanstone, Celia Rodd, Hope A. Weiler declares that they have no conflict of interest.
Human and Animal Rights and Informed Consent
Ethics approvals were obtained from the McGill University Faculty of Medicine Institutional Review Board, Lester B. Pearson School Board and the English Montreal School Board (Trial Registration: ClinicalTrials.gov: NCT01290016). All procedures performed in this study that involved human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Cohen, T.R., Hazell, T.J., Vanstone, C.A. et al. Bone Health is Maintained, While Fat Mass is Reduced in Pre-pubertal Children with Obesity Participating in a 1-Year Family-Centered Lifestyle Intervention. Calcif Tissue Int 101, 612–622 (2017). https://doi.org/10.1007/s00223-017-0318-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00223-017-0318-8