Abstract
The recreational use of cannabis products has risen considerably worldwide over the past decade. As the cannabis legal market grows, a critical challenge has been to make substantiated claims about the benefits and adverse health problems triggered by cannabis exposure. Despite accumulating evidence from animal studies demonstrating the role of cannabinoids on bone metabolism, there are conflicting results in clinical literature regarding their effects on bone health outcomes.
We undertook a systematic review to assess the evidence for the safety of cannabis use on bone health. We searched the databases MEDLINE, EMBASE, Cochrane Library, and Web of Science up to March 2023 for studies evaluating the effect of the recreational use of cannabis on the bone mineral density (BMD) of adults.
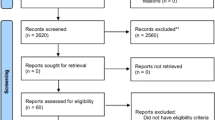
Among the 2620 studies reviewed, three cross-sectional studies and one randomized controlled trial comprised 4032 participants from 18 to 60 years who met the inclusion criteria. Two studies showed that cannabis exposure decreased BMD, while the other 2 indicated no alteration. Despite the different study designs, the included studies showed a low risk of bias according to the Joanna Briggs Institute tool.
Eligible studies present differences in cannabis products, administration routes, and exposure determination. Further longitudinal research is needed to establish multiple clinical predictors associated with potentially negative consequences of cannabis exposure, especially in vulnerable populations such as elderly individuals.

Similar content being viewed by others
Data availability
Data used in this study are available upon request.
References
Ferland J-MN, Hurd YL (2020) Deconstructing the neurobiology of cannabis use disorder. Nat Neurosci 23:600–610
Connor JP, Stjepanović D, Le Foll B et al (2021) Cannabis use and cannabis use disorder. Nat Rev Dis Primers 7:16
United Nations (2023) Office on drugs and crime. World drug report. www.unodc.org/unodc/en/data-and-analysis/world-drug-report-2023.html
Hall W, Leung J, Lynskey M (2020) The effects of cannabis use on the development of adolescents and young adults. Annu Rev Dev Psychol 2:461–483
Gruber SA, Dahlgren MK, Sagar KA et al (2012) Age of onset of marijuana use impacts inhibitory processing. Neurosci Lett 511:89–94
Meier MH, Caspi A, Ambler A et al (2012) Persistent cannabis users show neuropsychological decline from childhood to midlife. Proc Natl Acad Sci 109:E2657–E2664
Zalesky A, Solowij N, Yücel M et al (2012) Effect of long-term cannabis use on axonal fibre connectivity. Brain 135:2245–2255
Di Forti M, Quattrone D, Freeman TP et al (2019) The contribution of cannabis use to variation in the incidence of psychotic disorder across Europe (EU-GEI): a multicentre case-control study. Lancet Psychiatry 6:427–436
Lev-Ran S, Roerecke M, Le Foll B et al (2014) The association between cannabis use and depression: a systematic review and meta-analysis of longitudinal studies. Psychol Med 44:797–810
Feingold D, Weiser M, Rehm J, Lev-Ran S (2015) The association between cannabis use and mood disorders: a longitudinal study. J Affect Disord 172:211–218
Han B, Compton WM, Einstein EB, Volkow ND (2021) Associations of suicidality trends with cannabis use as a function of sex and depression status. JAMA Netw Open 4:e2113025–e2113025
Chami T, Kim CH (2019) Cannabis abuse and elevated risk of myocardial infarction in the young: a population-based study. In: Mayo clinic proceedings. Elsevier, 1647–1649
Braymiller JL, Barrington-Trimis JL, Leventhal AM et al (2020) Assessment of nicotine and cannabis vaping and respiratory symptoms in young adults. JAMA Netw Open 3:e2030189–e2030189
Patel RS, Manocha P, Patel J et al (2020) Cannabis use is an independent predictor for acute myocardial infarction related hospitalization in younger population. J Adolesc Health 66:79–85
Richards JR, Blohm E, Toles KA et al (2020) The association of cannabis use and cardiac dysrhythmias: a systematic review. Clin Toxicol 58:861–869
Cota D, Marsicano G, Lutz B et al (2003) Endogenous cannabinoid system as a modulator of food intake. Int J Obes 27:289–301
Rodondi N, Pletcher MJ, Liu K et al (2006) Marijuana use, diet, body mass index, and cardiovascular risk factors (from the CARDIA study). Am J Cardiol 98:478–484
DiPatrizio NV, Astarita G, Schwartz G et al (2011) Endocannabinoid signal in the gut controls dietary fat intake. Proc Natl Acad Sci 108:12904–12908
Bab I, Zimmer A (2008) Cannabinoid receptors and the regulation of bone mass. Br J Pharmacol 153:182–188
Tam J, Ofek O, Fride E et al (2006) Involvement of neuronal cannabinoid receptor CB1 in regulation of bone mass and bone remodeling. Mol Pharmacol 70:786–792
Ofek O, Karsak M, Leclerc N et al (2006) Peripheral cannabinoid receptor, CB2, regulates bone mass. Proc Natl Acad Sci 103:696–701
Idris AI, van’t Hof RJ, Greig IR et al (2005) Regulation of bone mass, bone loss and osteoclast activity by cannabinoid receptors. Nat Med 11:774–779
Sophocleous A, Marino S, Kabir D et al (2017) Combined deficiency of the Cnr1 and Cnr2 receptors protects against age-related bone loss by osteoclast inhibition. Aging Cell 16:1051–1061
Idris AI, Sophocleous A, Landao-Bassonga E et al (2008) Regulation of bone mass, osteoclast function, and ovariectomy-induced bone loss by the type 2 cannabinoid receptor. Endocrinology 149:5619–5626
da Nogueira-Filho GR, Cadide T, Rosa BT et al (2008) Cannabis sativa smoke inhalation decreases bone filling around titanium implants: a histomorphometric study in rats. Implant Dent 17:461–470
Samir SM, Malek HA (2014) Effect of cannabinoid receptors 1 modulation on osteoporosis in a rat model of different ages. J Physiol Pharmacol 65:687–694
Kogan NM, Melamed E, Wasserman E et al (2015) Cannabidiol, a major non-psychotropic cannabis constituent enhances fracture healing and stimulates lysyl hydroxylase activity in osteoblasts. J Bone Miner Res 30:1905–1913
Kamali A, Oryan A, Hosseini S et al (2019) Cannabidiol-loaded microspheres incorporated into osteoconductive scaffold enhance mesenchymal stem cell recruitment and regeneration of critical-sized bone defects. Mater Sci Eng, C 101:64–75
Idris AI, Sophocleous A, Landao-Bassonga E et al (2009) Cannabinoid receptor type 1 protects against age-related osteoporosis by regulating osteoblast and adipocyte differentiation in marrow stromal cells. Cell Metab 10:139–147
Sophocleous A, Sims AH, Idris AI, Ralston SH (2014) Modulation of strain-specific differences in gene expression by cannabinoid type 2 receptor deficiency. Calcif Tissue Int 94:423–432
Kanis JA, Cooper C, Rizzoli R et al (2019) European guidance for the diagnosis and management of osteoporosis in postmenopausal women. Osteoporos Int 30:3–44
Karsak M, Malkin I, Toliat MR et al (2009) The cannabinoid receptor type 2 (CNR2) gene is associated with hand bone strength phenotypes in an ethnically homogeneous family sample. Hum Genet 126:629–636
Karsak M, Cohen-Solal M, Freudenberg J et al (2005) Cannabinoid receptor type 2 gene is associated with human osteoporosis. Hum Mol Genet 14:3389–3396
Zhang C, Ma J, Chen G et al (2015) Evaluation of common variants in CNR2 gene for bone mineral density and osteoporosis susceptibility in postmenopausal women of Han Chinese. Osteoporos Int 26:2803–2810
Higgins JPT, Thomas J, Chandler J et al (2019) Cochrane handbook for systematic reviews of interventions. Wiley
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Ouzzani M, Hammady H, Fedorowicz Z, Elmagarmid A (2016) Rayyan—a web and mobile app for systematic reviews. Syst Rev 5:1–10
Joanna Briggs Institute (2017) Checklist for systematic reviews and research syntheses. In: https://jbi.global/critical-appraisal-tools
Guyatt G, Oxman AD, Akl EA et al (2011) GRADE guidelines: 1. Introduction - GRADE evidence profiles and summary of findings tables. J Clin Epidemiol 64:383–394. https://doi.org/10.1016/j.jclinepi.2010.04.026
Barreiro MA, Rosado LM, Peniche DB, García ME (2017) Efecto de los estilos de vida en jóvenes universitarios Mexicanos sobre la densidad mineral ósea. Rev esp nutr comunitaria 23(1)
Bourne D, Plinke W, Hooker ER, Nielson CM (2017) Cannabis use and bone mineral density: NHANES 2007–2010. Arch Osteoporos 12:1–6
Sophocleous A, Robertson R, Ferreira NB et al (2017) Heavy cannabis use is associated with low bone mineral density and an increased risk of fractures. Am J Med 130:214–221
Lopez HL, Cesareo KR, Raub B et al (2020) Effects of hemp extract on markers of wellness, stress resilience, recovery and clinical biomarkers of safety in overweight, but otherwise healthy subjects. J Diet Suppl 17:561–586
Shen Y, Huang X, Wu J, et al (2022) The global burden of osteoporosis, low bone mass, and its related fracture in 204 countries and territories, 1990–2019. Front Endocrinol (Lausanne) 13 https://doi.org/10.3389/fendo.2022.882241
Xiao P-L, Cui A-Y, Hsu C-J et al (2022) Global, regional prevalence, and risk factors of osteoporosis according to the World Health Organization diagnostic criteria: a systematic review and meta-analysis. Osteoporos Int 33:2137–2153. https://doi.org/10.1007/s00198-022-06454-3
Sophocleous A, Yiallourides M, Zeng F et al (2022) Association of cannabinoid receptor modulation with normal and abnormal skeletal remodelling: a systematic review and meta-analysis of in vitro, in vivo and human studies. Pharmacol Res 175:105928. https://doi.org/10.1016/j.phrs.2021.105928
Ofek O, Attar-Namdar M, Kram V et al (2011) CB2 cannabinoid receptor targets mitogenic Gi protein-cyclin D1 axis in osteoblasts. J Bone Miner Res 26:308–316. https://doi.org/10.1002/jbmr.228
Rossi F, Bellini G, Tortora C et al (2015) CB2 and TRPV1 receptors oppositely modulate in vitro human osteoblast activity. Pharmacol Res 99:194–201. https://doi.org/10.1016/j.phrs.2015.06.010
Li D, Lin Z, Meng Q et al (2017) Cannabidiol administration reduces sublesional cancellous bone loss in rats with severe spinal cord injury. Eur J Pharmacol 809:13–19. https://doi.org/10.1016/j.ejphar.2017.05.011
Smoum R, Baraghithy S, Chourasia M et al (2015) CB2 cannabinoid receptor agonist enantiomers HU-433 and HU-308: an inverse relationship between binding affinity and biological potency. Proc Natl Acad Sci 112:8774–8779. https://doi.org/10.1073/pnas.1503395112
Sophocleous A, Börjesson AE, Salter DM, Ralston SH (2015) The type 2 cannabinoid receptor regulates susceptibility to osteoarthritis in mice. Osteoarthritis Cartilage 23:1586–1594. https://doi.org/10.1016/J.JOCA.2015.04.020
Whyte LS, Ryberg E, Sims NA et al (2009) The putative cannabinoid receptor GPR55 affects osteoclast function in vitro and bone mass in vivo. Proc Natl Acad Sci U S A 106:16511–16516. https://doi.org/10.1073/PNAS.0902743106/SUPPL_FILE/0902743106SI.PDF
Ryberg E, Larsson N, Sjögren S et al (2007) The orphan receptor GPR55 is a novel cannabinoid receptor. Br J Pharmacol 152:1092–1101. https://doi.org/10.1038/SJ.BJP.0707460
Lauckner JE, Jensen JB, Chen HY et al (2008) GPR55 is a cannabinoid receptor that increases intracellular calcium and inhibits M current. Proc Natl Acad Sci U S A 105:2699–2704. https://doi.org/10.1073/PNAS.0711278105/SUPPL_FILE/11278FIG6.JPG
Duane B, Zeng J, Williams SM et al (2014) Further evidence that periodontal bone loss increases with smoking and age. Evid Based Dent 15:72–73. https://doi.org/10.1038/SJ.EBD.6401038
Heath D, Ghali A, Momtaz D et al (2022) Marijuana use results in increased time to union in surgically treated pediatric fracture patients. J Orthop Trauma 36:e106–e110. https://doi.org/10.1097/BOT.0000000000002242
Tao X, Matur A V., Khalid S, et al (2023) Cannabis use is associated with higher rates of pseudarthrosis following TLIF. Spine (Phila Pa 1976) https://doi.org/10.1097/BRS.0000000000004768
Ehrenkranz J, Levine MA (2019) Bones and joints: the effects of cannabinoids on the skeleton. J Clin Endocrinol Metab 104:4683–4694
Farokhnia M, McDiarmid GR, Newmeyer MN, et al (2020) Effects of oral, smoked, and vaporized cannabis on endocrine pathways related to appetite and metabolism: a randomized, double-blind, placebo-controlled, human laboratory study. Transl Psychiatry 2020 10:1 10:1–11 https://doi.org/10.1038/s41398-020-0756-3
Ohlsson A, Lindgren J-E, Andersson S et al (1986) Single-dose kinetics of deuterium-labelled cannabidiol in man after smoking and intravenous administration. Biomed Environ Mass Spectrom 13:77–83. https://doi.org/10.1002/BMS.1200130206
Grotenhermen F (2003) Pharmacokinetics and pharmacodynamics of cannabinoids. Clin Pharmacokinet 42:327–360. https://doi.org/10.2165/00003088-200342040-00003
Secades-Villa R, Garcia-Rodríguez O, Jin CJ et al (2015) Probability and predictors of the cannabis gateway effect: a national study. Int J Drug Policy 26:135–142
Hindley G, Beck K, Borgan F et al (2020) Psychiatric symptoms caused by cannabis constituents: a systematic review and meta-analysis. Lancet Psychiatry 7:344–353
Fontanella CA, Steelesmith DL, Brock G et al (2021) Association of cannabis use with self-harm and mortality risk among youths with mood disorders. JAMA Pediatr 175:377–384
Vozoris NT, Zhu J, Ryan CM et al (2022) Cannabis use and risks of respiratory and all-cause morbidity and mortality: a population-based, data-linkage, cohort study. BMJ Open Respir Res 9:e001216
Yamada Y, Ando F, Shimokata H (2007) Association of candidate gene polymorphisms with bone mineral density in community-dwelling Japanese women and men. Int J Mol Med. https://doi.org/10.3892/ijmm.19.5.791
Wang C, Zhang Z, Zhang H et al (2012) Susceptibility genes for osteoporotic fracture in postmenopausal Chinese women. J Bone Miner Res 27:2582–2591. https://doi.org/10.1002/jbmr.1711
Woo JH, Kim H, Kim JH, Kim JG (2015) Cannabinoid receptor gene polymorphisms and bone mineral density in Korean postmenopausal women. Menopause 22:512–519. https://doi.org/10.1097/GME.0000000000000339
ElSohly MA, Chandra S, Radwan M et al (2021) A comprehensive review of cannabis potency in the United States in the last decade. Biol Psychiatry Cogn Neurosci Neuroimaging 6:603–606. https://doi.org/10.1016/j.bpsc.2020.12.016
Le A, Han BH, Palamar JJ (2022) Underreporting of past-year cannabis use on a national survey by people who smoke blunts. Subst Abus 43:349–355. https://doi.org/10.1080/08897077.2021.1941520
Acknowledgements
CAPES for making available the web site www.periodicos.capes.gov.br
Funding
This study was supported by grant from Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – Finance Code 001 for LAVM.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
Luiz Alexandre Viana Magno, Lucas Ferreira Alves, Diego Tameirão and Nathalia Sernizon Guimarães declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Diego Ribeiro Taimerao died before publication of this work was completed.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Magno, L.A.V., Tameirão, D.R., Alves, L.F. et al. Effect of recreational cannabis use on bone mineral density: a systematic review. Osteoporos Int 35, 391–399 (2024). https://doi.org/10.1007/s00198-023-06992-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-023-06992-4