Abstract
Summary
Sarcopenia was reported to be significantly associated with osteoporosis. In this study, we reported for the first time that sarcopenia was an independent risk predictor of osteoporotic vertebral compression refractures (OVCRFs). Other risk factors of OVCRFs are low bone mass density T-scores, female sex, and advanced age.
Introduction
The purpose of this study was to investigate the association between osteoporotic vertebral compression refractures (OVCRFs) and sarcopenia, and to identify other risk factors of OVCRFs.
Methods
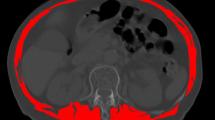
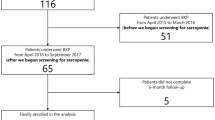
We evaluated 237 patients with osteoporotic vertebral compression fracture who underwent percutaneous kyphoplasty (PKP) in our hospital from August 2016 to December 2017. To diagnose sarcopenia, a cross-sectional computed tomography (CT) image at the inferior aspect of the third lumbar vertebra (L3) was selected for estimating muscle mass. Grip strength was used to assess muscle strength. Possible risk factors, such as age, sex, body mass index (BMI), bone mineral density (BMD), location of the treated vertebra, anterior-posterior ratio (AP ratio) of the fractured vertebra, cement leakage, and vacuum clefts, were assessed. The multivariable analysis was used to determine the risk factors of OVCRFs.
Results
During the follow-up period, OVCRFs occurred in 64 (27.0%) patients. Sarcopenia was present in 48 patients (20.3%), including 21 OVCRFs and 27 non-OVCRFs patients. Sarcopenia was significantly correlated with advanced age, lower BMI, lower BMD, and hypoalbuminemia. Compared with non-sarcopenic patients, sarcopenic patients had higher OVCRFs risk. In univariate analysis, sarcopenia (p = 0.003), female (p = 0.024), advanced age (≥ 75 years; p < 0.001), lower BMD (p < 0.001), lower BMI (p = 0.01), TL junction (vertebral levels at the thoracolumbar junction) (p = 0.01), cardiopulmonary comorbidity (p = 0.042), and hypoalbuminemia (p = 0.003) were associated with OVCRFs. Multivariable analysis revealed that sarcopenia (OR 2.271; 95% CI 1.069–4.824, p = 0.033), lower BMD (OR 1.968; 95% CI 1.350–2.868, p < 0.001), advanced age (≥ 75 years; OR 2.431; 95% CI 1.246–4.744, p = 0.009), and female sex (OR 4.666; 95% CI 1.400–15.552, p = 0.012) were independent risk predictors of OVCRFs.
Conclusions
Sarcopenia is an independent risk predictor of osteoporotic vertebral compression refractures. Other factors affecting OVCRFs are low BMD T-scores, female sex, and advanced age.



Similar content being viewed by others
References
Kim DH, Vaccaro AR (2006) Osteoporotic compression fractures of the spine; current options and considerations for treatment. Spine J 6:479–487
Garfin SR, Yuan HA, Reiley MA (2001) New technologies in spine - Kyphoplasty and vertebrosplasty for the treatment of painful osteoporotic compression fractures. Spine 26:1511–1515
Buchbinder R, Johnston RV, Rischin KJ, Homik J, Jones CA, Golmohammadi K, Kallmes DF (2018) Percutaneous vertebroplasty for osteoporotic vertebral compression fracture. Cochrane Database Syst Rev 4:CD006349
Syed MI, Patel NA, Jan S, Shaikh A, Grunden B, Morar K (2006) Symptomatic refractures after vertebroplasty in patients with steroid-induced osteoporosis. Am J Neuroradiol 27:1938–1943
Lin EP, Ekholm S, Hiwatashi A, Westesson PL (2004) Vertebroplasty: cement leakage into the disc increases the risk of new fracture of adjacent vertebral body. Am J Neuroradiol 25:175–180
Lin CC, Chen IH, Yu TC, Chen A, Yen PS (2007) New symptomatic compression fracture after percutaneous vertebroplasty at the thoracolumbar junction. AJNR Am J Neuroradiol 28:1042–1045
Chen LK, Lee WJ, Peng LN, Liu LK, Arai H, Akishita M, Asian Working Group for S (2016) Recent advances in sarcopenia research in Asia: 2016 update from the Asian Working Group for Sarcopenia. J Am Med Dir Assoc 17:–767 e761–767
Janssen I, Shepard DS, Katzmarzyk PT, Roubenoff R (2004) The healthcare costs of sarcopenia in the United States. J Am Geriatr Soc 52:80–85
Wu CH, Yang KC, Chang HH, Yen JF, Tsai KS, Huang KC (2013) Sarcopenia is related to increased risk for low bone mineral density. J Clin Densitom 16:98–103
Edwards MH, Dennison EM, Aihie Sayer A, Fielding R, Cooper C (2015) Osteoporosis and sarcopenia in older age. Bone 80:126–130
Binkley N, Krueger D, Buehring B (2013) What’s in a name revisited: should osteoporosis and sarcopenia be considered components of “dysmobility syndrome?”. Osteoporos Int 24:2955–2959
Hirschfeld HP, Kinsella R, Duque G (2017) Osteosarcopenia: where bone, muscle, and fat collide. Osteoporos Int 28:2781–2790
Walsh MC, Hunter GR, Livingstone MB (2006) Sarcopenia in premenopausal and postmenopausal women with osteopenia, osteoporosis and normal bone mineral density. Osteoporos Int 17:61–67
Hida T, Shimokata H, Sakai Y, Ito S, Matsui Y, Takemura M, Kasai T, Ishiguro N, Harada A (2015) Sarcopenia and sarcopenic leg as potential risk factors for acute osteoporotic vertebral fracture among older women. Eur Spine J 25:3424–3431
Iolascon G, Giamattei MT, Moretti A, Di Pietro G, Gimigliano F, Gimigliano R (2013) Sarcopenia in women with vertebral fragility fractures. Aging Clin Exp Res 25(Suppl 1):S129–S131
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, Martin FC, Michel JP, Rolland Y, Schneider SM, Topinková E, Vandewoude M, Zamboni M, European Working Group on Sarcopenia in Older People (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on Sarcopenia in Older People. Age Ageing 39:412–423
Chen LK, Liu LK, Woo J, Assantachai P, Auyeung TW, Bahyah KS, Chou MY, Chen LY, Hsu PS, Krairit O, Lee JSW, Lee WJ, Lee Y, Liang CK, Limpawattana P, Lin CS, Peng LN, Satake S, Suzuki T, Won CW, Wu CH, Wu SN, Zhang T, Zeng P, Akishita M, Arai H (2014) Sarcopenia in Asia: consensus report of the Asian Working Group for Sarcopenia. J Am Med Dir Assoc 15:95–101
Iritani S, Imai K, Takai K, Hanai T, Ideta T, Miyazaki T, Suetsugu A, Shiraki M, Shimizu M, Moriwaki H (2015) Skeletal muscle depletion is an independent prognostic factor for hepatocellular carcinoma. J Gastroenterol 50:323–332
Boutin RD, Yao L, Canter RJ, Lenchik L (2015) Sarcopenia: current concepts and imaging implications. AJR Am J Roentgenol 205:W255–W266
Szulc P, Feyt C, Chapurlat R (2016) High risk of fall, poor physical function, and low grip strength in men with fracture-the STRAMBO study. J Cachexia Sarcopenia Muscle 7:299–311
Wang YJ, Wang Y, Zhan JK, Tang ZY, He JY, Tan P, Deng HQ, Huang W, Liu YS (2015) Sarco-osteoporosis: prevalence and association with frailty in Chinese community-dwelling older adults. Int J Endocrinol 2015:482940
Ilich JZ, Inglis JE, Kelly OJ, McGee DL (2015) Osteosarcopenic obesity is associated with reduced handgrip strength, walking abilities, and balance in postmenopausal women. Osteoporos Int 26:2587–2595
Kang SK, Lee CW, Park NK, Kang TW, Lim JW, Cha KY, Kim JH (2011) Predictive risk factors for refracture after percutaneous vertebroplasty. Ann Rehabil Med 35:844–851
Strom O, Borgstrom F, Kanis JA, Compston J, Cooper C, McCloskey EV, Jonsson B (2011) Osteoporosis: burden, health care provision and opportunities in the EU: a report prepared in collaboration with the International Osteoporosis Foundation (IOF) and the European Federation of Pharmaceutical Industry Associations (EFPIA). Arch Osteoporos 6:59–155
Kim SH, Kang HS, Choi JA, Ahn JM (2016) Risk factors of new compression fractures in adjacent vertebrae after percutaneous vertebroplasty. Acta Radiol 45:440–445
Lindsay R, Burge RT, Strauss DM (2005) One year outcomes and costs following a vertebral fracture. Osteoporos Int 16:78–85
Ahn Y, Lee JH, Lee HY, Lee SH, Keem SH (2008) Predictive factors for subsequent vertebral fracture after percutaneous vertebroplasty. J Neurosurg Spine 9:129–136
Sun G, Tang H, Li M, Liu X, Jin P, Li L (2014) Analysis of risk factors of subsequent fractures after vertebroplasty. Eur Spine J 23:1339–1345
De Laet C, Kanis JA, Oden A et al (2005) Body mass index as a predictor of fracture risk: a meta-analysis. Osteoporos Int 16:1330–1338
Karasik D, Kiel DP (2008) Genetics of the musculoskeletal system: a pleiotropic approach. J Bone Miner Res 23:788–802
Rho YJ, Choe WJ, Chun YI (2012) Risk factors predicting the new symptomatic vertebral compression fractures after percutaneous vertebroplasty or kyphoplasty. Eur Spine J 21:905–911
Uppin AA, Hirsch JA, Centenera LV, Pfiefer BA, Pazianos AG, Choi IS (2003) Occurrence of new vertebral body fracture after percutaneous vertebroplasty in patients with osteoporosis. Radiology 226:119–124
Lee WS, Sung KH, Jeong HT, Sung YS, Hyun YI, Choi JY, Lee KS, Ok CS, Choi YW (2006) Risk factors of developing new symptomatic vertebral compression fractures after percutaneous vertebroplasty in osteoporotic patients. Eur Spine J 15:1777–1783
Funding
This work was supported by the National Natural Science Foundation of China (81571190).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOC 83 kb)
Rights and permissions
About this article
Cite this article
Wang, WF., Lin, CW., Xie, CN. et al. The association between sarcopenia and osteoporotic vertebral compression refractures. Osteoporos Int 30, 2459–2467 (2019). https://doi.org/10.1007/s00198-019-05144-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-019-05144-x