Abstract
Introduction and hypothesis
The objective of this study was to determine whether differences in the cumulative dietary intake of choline, is associated with the risk of developing urge urinary incontinence (UUI).
Methods
This was an analysis within the Nurses’ Health Study (NHS) I and II. The main exposure was the cumulative daily intake for each choline-containing compound obtained from a detailed daily food frequency questionnaire. The primary outcome was UUI, defined as urine loss with a sudden feeling of bladder fullness or when a toilet is inaccessible, occurring >1/month. Cox proportional hazards regression models were used to calculate multivariate-adjusted relative risks and 95% confidence intervals (CIs) for the association between total choline and choline derivatives and risk of UUI. Fixed effects meta-analyses of results from NHSI and NHSII were performed for postmenopausal women only to obtain a pooled estimate of the impact of choline consumption on UUI.
Results
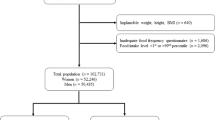
There were 33,273 participants in NHSI and 38,732 in NHSII who met all the criteria for inclusion in the analysis. The incidence of UUI was 9.41% (n=3,139) in NHSI and 4.25% (n=1,646) in NHSII. After adjusting for confounders choline was not found to be associated with UUI in postmenopausal women. However, in premenopausal women, relative to the lowest quartile, the highest quartile of consumption of total choline (aRR = 0.79, 95% CI: 0.64–0.99), free choline (aRR = 0.74, 95% CI: 0.58–0.94), and phosphocholine (aRR = 0.77, 95% CI: 0.61–0.96) were associated with a reduced risk of UUI.
Conclusions
Increased dietary choline consumption was associated with a reduced risk of UUI among premenopausal women.

Similar content being viewed by others
Data Availability
The data used for this study are available through request submitted to Brigham and Women’s Hospital and the Harvard T.H. Chan School of Public Health.
References
Stewart WF, Corey R, Herzog AR, et al. Prevalence of overactive bladder in women: results from the NOBLE program. Int Urogynecol J. 2001;12:S66.
Lukacz ES, Santiago-Lastra Y, Albo ME, Brubaker L. Urinary incontinence in women: a review. JAMA. 2017;318(16):1592–604. https://doi.org/10.1001/jama.2017.121.
Sakakibara R. Lower urinary tract dysfunction in patients with brain lesions. Handb Clin Neurol. 2015;130:269–87. https://doi.org/10.1016/B978-0-444-63247-0.00015-.
Lightner DJ, Gomelsky A, Souter L, Vasavada SP. Diagnosis and treatment of overactive bladder (non-neurogenic) in adults: AUA/SUFU Guideline Amendment 2019. J Urol. 2019;202(3):558–63. https://doi.org/10.1097/JU.0000000000000309.
Maman K, Aballea S, Nazir J, et al. Comparative efficacy and safety of medical treatments for the management of overactive bladder: a systematic literature review and mixed treatment comparison. Eur Urol. 2014;65(4):755–65. https://doi.org/10.1016/j.eururo.2013.11.010.
Chacko S, Cortes E, Drake MJ, Fry CH. Does altered myogenic activity contribute to OAB symptoms from detrusor overactivity? ICI-RS 2013. Neurourol Urodyn. 2014;33(5):577–80. https://doi.org/10.1002/nau.22599.
Amundsen CL, Richter HE, Menefee SA, et al. OnabotulinumtoxinAvs sacral neuromodulation on refractory urgency urinary incontinence in women: a randomized clinical trial. JAMA. 2016;316:1366–74.
Chancellor MB, Migliaccio-Walle K, Bramley TJ, Chaudhari SL, Corbell C, Globe D. Long-term patterns of use and treatment failure with anticholinergic agents for overactive bladder. Clin Ther. 2013;35(11):1744–51.
Tyagi P. Pathophysiology of the urothelium and detrusor. Can Urol Assoc J. 2011;5(5 Suppl 2):S128–30. https://doi.org/10.5489/cuaj.11181.
Smith AL. Understanding overactive bladder and urgency incontinence: what does the brain have to do with it? F1000Res. 2018;7:F1000 Faculty Rev-1869. https://doi.org/10.12688/f1000research.16418.1.
Tsetlin VI. Acetylcholine and acetylcholine receptors: textbook knowledge and new data. Biomolecules. 2020;10(6):852. https://doi.org/10.3390/biom10060852.
Wiedeman AM, Barr SI, Green TJ, Xu Z, Innis SM, Kitts DD. Dietary choline intake: current state of knowledge across the life cycle. Nutrients. 2018;10(10):1513. https://doi.org/10.3390/nu10101513.
Zeisel SH, Da Costa KA, Franklin PD, et al. Choline, an essential nutrient for humans. FASEB J. 1991;5(7):2093–8.
Yoo W, Zieba JK, Foegeding NJ, et al. High-fat diet-induced colonocyte dysfunction escalates microbiota-derived trimethylamine N-oxide. Science. 2021;373(6556):813–8. https://doi.org/10.1126/science.aba3683.
Farrell GC, Haczeyni F, Chitturi S. Pathogenesis of NASH: how metabolic complications of overnutrition favour lipotoxicity and pro-inflammatory fatty liver disease. Adv Exp Med Biol. 2018;1061:19–44. https://doi.org/10.1007/978-981-10-8684-7_3.
Sheyn D, Hijaz AK, Hazlett FE Jr, et al. Evaluation of urine choline levels in women with and without overactive bladder syndrome. Female Pelvic Med Reconstr Surg. 2020;26(10):644–8. https://doi.org/10.1097/SPV.0000000000000639.
Sheyn D, Hijaz AK, Hazlett FE Jr, et al. Evaluation of choline and acetylcholine levels in responders and nonresponders to anticholinergic therapy for overactive bladder syndrome. Female Pelvic Med Reconstr Surg. 2020;26(12):e91–6. https://doi.org/10.1097/SPV.0000000000000787.
Colditz GA, Manson JE, Hankinson SE. The Nurses’ Health Study: 20-year contribution to the understanding of health among women. J Womens Health. 1997;6(1):49–62.
Michels KB, Willett WC. Self-administered semiquantitative food frequency questionnaires: patterns, predictors, and interpretation of omitted items. Epidemiology. 2009;20(2):295–301. https://doi.org/10.1097/EDE.0b013e3181931515.
US Department of Agriculture: Agricultural Research Division. 2021 http://www.ars.usda.gov/ba/bhnrc/ndl. Accessed 6 March 2021.
Li Y, Wang DD, Chiuve SE, et al. Dietary phosphatidylcholine intake and type 2 diabetes in men and women. Diabetes Care. 2015;38(2):e13–4. https://doi.org/10.2337/dc14-2093.
Craig SA. Betaine in human nutrition. Am J Clin Nutr. 2004;80(3):539–49.
U.S. Department of Agriculture, Agricultural Research Service. FoodData Central. 2023. https://fdc.nal.usda.gov/. Accessed 27 November 2023.
Grodstein F, Fretts R, Lifford K, Resnick N, Curhan G. Association of age, race, and obstetric history with urinary symptoms among women in the Nurses’ Health Study. Am J Obstet Gynecol. 2003;189(2):428–34. https://doi.org/10.1067/s0002-9378(03)00361-2.
Ridgway ND. The role of phosphatidylcholine and choline metabolites to cell proliferation and survival. Crit Rev Biochem Mol Biol. 2013;48(1):20–38.
Ramstedt B, Slotte JP. Membrane properties of sphingomyelins. FEBS Lett. 2002;531(1):33–7. https://doi.org/10.1016/s0014-5793(02)03406-3.
Tani M, Hannun YA. Analysis of membrane topology of neutral sphingomyelinase 2. FEBS Lett. 2007;581(7):1323–8. https://doi.org/10.1016/j.febslet.2007.02.046.
Wang Z, Klipfell E, Bennett BJ, et al. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature. 2011;472:57–63.
Tang WH, Wang Z, Levison BS, et al. Intestinal microbial metabolism of phosphatidylcholine and cardiovascular risk. N Engl J Med. 2013;368(17):1575–84. https://doi.org/10.1056/NEJMoa1109400.
Yancey PH. Organic osmolytes as compatible, metabolic and counteracting cytoprotectants in high osmolarity and other stresses. J Exp Biol. 2005;208:2819–30.
Okamoto T, Hatakeyama S, Imai A, et al. Altered gut microbiome associated with overactive bladder and daily urinary urgency. World J Urol. 2021;39(3):847–53. https://doi.org/10.1007/s00345-020-03243-7.
Fischer LM, DaCosta KA, Kwock L, et al. Sex and menopausal status influence human dietary requirements for the nutrient choline. Am J Clin Nutr. 2007;85(5):1275–85.
Resseguie M, Song J, Niculescu MD, da Costa KA, Randall TA, Zeisel SH. Phosphatidylethanolamine N-methyltransferase (PEMT) gene expression is induced by estrogen in human and mouse primary hepatocytes. FASEB J. 2007;21(10):2622–32. https://doi.org/10.1096/fj.07-8227com.
Zia Y, Al Rajabi A, Mi S, et al. Hepatic expression of PEMT, but not dietary choline supplementation, reverses the protection against atherosclerosis in Pemt−/−/Ldlr−/− mice. J Nutr. 2018;148(10):1513–20. https://doi.org/10.1093/jn/nxy165.
Bradley CS, Brown JS, Van Den Eeden SK, Schembri M, Ragins A, Thom DH. Urinary incontinence self-report questions: reproducibility and agreement with bladder diary. Int Urogynecol J. 2011;22(12):1565–71. https://doi.org/10.1007/s00192-011-1503-3.
Chughtai B, Kavaler E, Lee R, Te A, Kaplan SA, Lowe F. Use of herbal supplements for overactive bladder. Rev Urol. 2013;15(3):93–6.
Funding
Nurses' Health Study I is supported by UM1 CA186107 and Nurses' Health Study II is supported by U01 CA 176726 from the National Institutes of Health, Bethesda, MD, USA.
Author information
Authors and Affiliations
Contributions
D.S.: development, design, manuscript writing; K.L.P.: design, analysis, manuscript writing; A.H.: manuscript writing, development; H.M.: manuscript writing, analysis; V.M.: manuscript writing, development; O.Z.: analysis, manuscript writing.
Corresponding author
Ethics declarations
Conflicts of interest
D.S.: research support—Renalis; consulting fee—Caldera; A.H.: ownership stake—Collamedix; S.T.M.: consulting fee—Boston Scientific, AbbVie. Y.B.C.: Chief Medical Officer Renalis. V.M. and H.M. have no conflicts of interest.
Additional information
Handling Editor: Tony Bazi
Editor in Chief: Maria A. Bortolini
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below are the links to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sheyn, D., Momotaz, H., Hijaz, A. et al. Effect of Dietary Choline Consumption on the Development of Urinary Urgency Incontinence in a Longitudinal Cohort of Women. Int Urogynecol J 35, 667–676 (2024). https://doi.org/10.1007/s00192-024-05740-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00192-024-05740-4