Abstract
Purpose
The purpose of this systematic review and meta-analysis was to investigate the variability in tibial geometric ratios among knees of different sexes and races to determine whether commercially-available tibial baseplates accommodate the morphologic diversity. The hypothesis was that anthropometric studies report considerable variability of tibial geometric ratios among sexes and races.
Methods
This systematic review and meta-analysis was performed according to the preferred reporting items for systematic reviews and meta-analyses (PRISMA) criteria. Two authors independently conducted an electronic search using MEDLINE® and Embase® on 28 January 2021 for clinical studies reporting on tibial geometric ratios. Tibial geometric ratios, as reported by the clinical studies, were represented by plotting their means and two standard deviations for comparison to two symmetric and two asymmetric commercially-available tibial baseplates.
Results
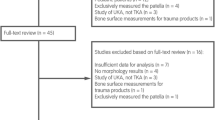
A total of 27 articles that reported on a combined total of 20,944 knees were eligible for data extraction. Variation in tibial aspect ratios was equal among sexes. The greatest variation in aspect ratio was observed among East Asians, followed by Caucasians, African-Americans, Indian and Middle Easterns. The variation in tibial asymmetry ratio was larger among men compared to women. The greatest variation in asymmetry ratio was observed among African-Americans, followed by Caucasians, East Asians, Indian and Middle Easterns. Bone-implant mismatch of > 3 mm overhang or > 4 mm under-coverage with four commercially-available tibial baseplates occurred in large proportions of knees due to variations in aspect ratio (in 17–100% of knees) and asymmetry ratio (in 7–100% of knees).
Conclusion
Anthropometric studies reported considerable inter-individual variability of tibial geometric ratios, which exceeded effects of sexual dimorphism and racial diversity. Bone–implant mismatch may be unavoidable in a large proportion of knees, when considering that a surgeon generally only uses one or a few TKA brands. These findings support the drive towards patient-specific implants to potentially achieve accurate bone–implant fit by implant customisation.
Level of evidence
IV.








Similar content being viewed by others
References
Asseln M, Hänisch C, Schick F, Radermacher K (2018) Gender differences in knee morphology and the prospects for implant design in total knee replacement. Knee 25(4):545–558
Bansal V, Mishra A, Verma T, Maini D, Karkhur Y, Maini L (2018) Anthropometric assessment of tibial resection surface morphology in total knee arthroplasty for tibial component design in Indian population. JAJS 5(1):24–28
Beckers L, Müller JH, Daxhelet J, Saffarini M, Aït-Si-Selmi T, Bonnin MP (2021) Sexual dimorphism and racial diversity render bone-implant mismatch inevitable after off-the-shelf total knee arthroplasty: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06447-5
Bellemans J, Carpentier K, Vandenneucker H, Vanlauwe J, Victor J (2010) The John Insall Award: both morphotype and gender influence the shape of the knee in patients undergoing TKA. Clin Orthop 468(1):29–36
Bonnin MP, de Kok A, Verstraete M, Van Hoof T, Van Der Straten C, Saffarini M, Victor J (2017) Popliteus impingement after TKA may occur with well-sized prostheses. Knee Surg Sports Traumatol Arthrosc 25(6):1720–1730
Bonnin MP, Saffarini M, Mercier PE, Laurent JR, Carrillon Y (2011) Is the anterior tibial tuberosity a reliable rotational landmark for the tibial component in total knee arthroplasty? J Arthroplasty 26(2):260–267
Bonnin MP, Saffarini M, Shepherd D, Bossard N, Dantony E (2016) Oversizing the tibial component in TKAs: incidence, consequences and risk factors. Knee Surg Sports Traumatol Arthrosc 24(8):2532–2540
Calek AK, Hochreiter B, Hess S, Amsler F, Leclerq V, Hirschmann MT, Behrend H (2021) High inter- and intraindividual differences in medial and lateral posterior tibial slope are not reproduced accurately by conventional TKA alignment techniques. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06477-z
Chaichankul C, Tanavalee A, Itiravivong P (2011) Anthropometric measurements of knee joints in Thai population: correlation to the sizing of current knee prostheses. Knee 18(1):5–10
Cheng FB, Ji XF, Lai Y, Feng JC, Zheng WX, Sun YF, Fu YW, Li YQ (2009) Three dimensional morphometry of the knee to design the total knee arthroplasty for Chinese population. Knee 16(5):341–347
Cho BW, Kwon HM, Hong YJ, Park KK, Yang IH, Lee WS (2021) Anatomical tibial component is related to more medial tibial stress shielding after total knee arthroplasty in Korean patients. Knee Surg Sports Traumatol Arthrosc 29(3):710–717
Clary C, Aram L, Deffenbaugh D, Heldreth M (2014) Tibial base design and patient morphology affecting tibial coverage and rotational alignment after total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 22(12):3012–3018
Dai Y, Bischoff JE (2013) Comprehensive assessment of tibial plateau morphology in total knee arthroplasty: influence of shape and size on anthropometric variability. J Orthop Res 31(10):1643–1652
Dai Y, Cross MB, Angibaud LD, Hamad C, Jung A, Jenny JY (2018) Posterior tibial slope impacts intraoperatively measured mid-flexion anteroposterior kinematics during cruciate-retaining total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26(11):3325–3332
Dai Y, Scuderi GR, Bischoff JE, Bertin K, Tarabichi S, Rajgopal A (2014) Anatomic tibial component design can increase tibial coverage and rotational alignment accuracy: a comparison of six contemporary designs. Knee Surg Sports Traumatol Arthrosc 22(12):2911–2923
Dargel J, Michael JW, Feiser J, Ivo R, Koebke J (2011) Human knee joint anatomy revisited: morphometry in the light of sex-specific total knee arthroplasty. J Arthroplasty 26(3):346–353
Erkocak OF, Kucukdurmaz F, Sayar S, Erdil ME, Ceylan HH, Tuncay I (2016) Anthropometric measurements of tibial plateau and correlation with the current tibial implants. Knee Surg Sports Traumatol Arthrosc 24(9):2990–2997
Fan L, Xu T, Li X, Zan P, Li G (2017) Morphologic features of the distal femur and tibia plateau in Southeastern Chinese population: a cross-sectional study. Medicine (Baltimore) 96(46):e8524
Galea VP, Botros MA, Madanat R, Nielsen CS, Bragdon C (2019) Promising early outcomes of a novel anatomic knee system. Knee Surg Sports Traumatol Arthrosc 27(4):1067–1074
Gustke KA, Golladay GJ, Roche MW, Elson LC, Anderson CR (2017) A targeted approach to ligament balancing using kinetic sensors. J Arthroplasty 32(7):2127–2132
Hafez MA, Sheikhedrees SM, Saweeres ES (2016) Anthropometry of Arabian arthritic knees: comparison to other ethnic groups and implant dimensions. J Arthroplasty 31(5):1109–1116
Hartel MJ, Loosli Y, Delfosse D, Diel P, Thali M, Ross S, Kohl S, Eggli S (2014) The influence of tibial morphology on the design of an anatomical tibial baseplate for TKA. Knee 21(2):415–419
Hartel MJ, Loosli Y, Gralla J, Kohl S, Hoppe S, Röder C, Eggli S (2009) The mean anatomical shape of the tibial plateau at the knee arthroplasty resection level: an investigation using MRI. Knee 16(6):452–457
Hitt K, Shurman JR 2nd, Greene K, McCarthy J, Moskal J, Hoeman T, Mont MA (2003) Anthropometric measurements of the human knee: correlation to the sizing of current knee arthroplasty systems. J Bone Joint Surg Am 85A(Suppl 4):115–122
Huijs S, Huysmans T, De Jong A, Arnout N, Sijbers J, Bellemans J (2018) Principal component analysis as a tool for determining optimal tibial baseplate geometry in modern TKA design. Acta Orthop Belg 84(4):452–460
Karimi E, Zandi R, Norouzian M, Birjandinejad A (2019) Correlation of anthropometric measurements of proximal tibia in iranian knees with size of current tibial implants. Arch Bone Jt Surg 7(4):339–345
Kim JK, Park JY, Lee HJ, Ro DH, Han HS, Lee MC (2020) Do the increment of femoral condyle curvature and the change of tibia shape improve clinical outcome in total knee arthroplasty? A propensity score matching analysis. Knee Surg Sports Traumatol Arthrosc 28(9):2980–2989
Kwak DS, Surendran S, Pengatteeri YH, Park SE, Choi KN, Gopinathan P, Han SH, Han CW (2007) Morphometry of the proximal tibia to design the tibial component of total knee arthroplasty for the Korean population. Knee 14(4):295–300
Li K, Saffarini M, Valluy J, Desseroit MC, Morvan Y, Telmon N, Cavaignac E (2019) Sexual and ethnic polymorphism render prosthetic overhang and under-coverage inevitable using off-the shelf TKA implants. Knee Surg Sports Traumatol Arthrosc 27(7):2130–2139
Li P, Tsai TY, Li JS, Zhang Y, Kwon YM, Rubash HE, Li G (2014) Morphological measurement of the knee: race and sex effects. Acta Orthop Belg 80(2):260–268
Liu Z, Yuan G, Zhang W, Shen Y, Deng L (2013) Anthropometry of the proximal tibia of patients with knee arthritis in Shanghai. J Arthroplasty 28(5):778–783
Ma Q-L, Lipman JD, Cheng C-K, Wang X-N, Zhang Y-Y, You B (2017) A comparison between chinese and caucasian 3-dimensional bony morphometry in presimulated and postsimulated osteotomy for total knee arthroplasty. J Arthroplasty 32(9):2878–2886
Mahfouz M, Abdel Fatah EE, Bowers LS, Scuderi G (2012) Three-dimensional morphology of the knee reveals ethnic differences. Clin Orthop 470(1):172–185
Mathis DT, Hirschmann MT (2021) Why do knees after total knee arthroplasty fail in different parts of the world? J Orthop 23:52–59
McCalden RW, Hart GP, MacDonald SJ, Naudie DD, Howard JH, Bourne RB (2017) Clinical results and survivorship of the GENESIS II total knee arthroplasty at a minimum of 15 years. J Arthroplasty 32(7):2161–2166
Meier M, Zingde S, Best R, Schroeder L, Beckmann J, Steinert AF (2020) High variability of proximal tibial asymmetry and slope: a CT data analysis of 15,807 osteoarthritic knees before TKA. Knee Surg Sports Traumatol Arthrosc 28(4):1105–1112
Moghtadaei M, Moghimi J, Farahini H, Jahansouz A (2015) Morphology of proximal tibia in Iranian population and its correlation with available prostheses. Med J Islam Repub Iran 29:225
Nakamura S, Morita Y, Ito H, Kuriyama S, Furu M, Matsuda S (2015) Morphology of the proximal tibia at different levels of bone resection in Japanese knees. J Arthroplasty 30(12):2323–2327
Nielsen CS, Nebergall A, Huddleston J, Kallemose T, Malchau H, Troelsen A (2018) Medial overhang of the tibial component is associated with higher risk of inferior knee injury and osteoarthritis outcome score pain after knee replacement. J Arthroplasty 33(5):1394–1398
Okazaki Y, Pujol N (2020) The use of an asymmetrical tibial tray in TKA optimises tibial rotation when fitted to the posterior tibial plateau border. Knee Surg Sports Traumatol Arthrosc 28(12):3821–3826
Reddy AVG, Sankineani SR, Agrawal R, Thayi C (2020) Comparative study of existing knee prosthesis with anthropometry of Indian patients and other races, a computer tomography 3D reconstruction-based study. J Clin Orthop Trauma 11(Suppl 2):S228-s233
Saffarini M, Nover L, Tandogan R, Becker R, Moser LB, Hirschmann MT, Indelli PF (2019) The original Akagi line is the most reliable: a systematic review of landmarks for rotational alignment of the tibial component in TKA. Knee Surg Sports Traumatol Arthrosc 27(4):1018–1027
Shah D, Ghyar R, Ravi B, Shetty V (2013) 3D morphological study of the Indian arthritic knee: comparison with other ethnic groups and conformity of current TKA implant. Open J Rheumatol Autoimmune Dis 3(4):263–269
Tanaka Y, Nakamura S, Kuriyama S, Nishitani K, Ito H, Lyman S, Matsuda S (2020) Intraoperative physiological lateral laxity in extension and flexion for varus knees did not affect short-term clinical outcomes and patient satisfaction. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-05862-4
Tandogan RN, Kort NP, Ercin E, van Rooij F, Nover L, Saffarini M, Hirschmann MT, Becker R, Dejour D (2021) Computer-assisted surgery and patient-specific instrumentation improve the accuracy of tibial baseplate rotation in total knee arthroplasty compared to conventional instrumentation: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06495-x
Westrich GH, Haas SB, Insall JN, Frachie A (1995) Resection specimen analysis of proximal tibial anatomy based on 100 total knee arthroplasty specimens. J Arthroplasty 10(1):47–51
Wevers HW, Simurda M, Griffin M, Tarrel J (1994) Improved fit by asymmetric tibial prosthesis for total knee arthroplasty. Med Eng Phys 16(4):297–300
Yang B, Song CH, Yu JK, Yang YQ, Gong X, Chen LX, Wang YJ, Wang J (2014) Intraoperative anthropometric measurements of tibial morphology: comparisons with the dimensions of current tibial implants. Knee Surg Sports Traumatol Arthrosc 22(12):2924–2930
Yang B, Yu J, Gong X, Chen L, Wang Y, Wang J, Wang H, Zhang J (2014) Intraoperative study on anthropometry and gender differences of the proximal tibial plateau at the arthroplasty resection surface. Chin Med J (Engl) 127(1):92–95
Yang B, Yu JK, Zheng ZZ, Lu ZH, Zhang JY, Cheng JH (2013) Computed tomography morphometric study of gender differences in osteoarthritis proximal tibias. J Arthroplasty 28(7):1117–1120
Yue B, Varadarajan KM, Ai S, Tang T, Rubash HE, Li G (2011) Differences of knee anthropometry between Chinese and white men and women. J Arthroplasty 26(1):124–130
Yue W, Theobald M, Deckx J, Lawrenchuk M, Angibaud L (2016) Evaluation of a western originated total knee arthroplasty design on the fit of small sized femora. J Orthop Res 34:0942
Zhang K, Han Q, Wang H, Yang K, Chen B, Zhang Y, Zhang S, Wang J, Chu H (2019) Measurement of proximal tibial morphology in northeast Chinese population based on three-dimensional reconstruction computer tomography. Medicine (Baltimore) 98(45):e17508
Zhang Y, Wang X, Wu Z, Xia Q, Shao Y (2017) Highly variable femoral morphology in osteoarthritic Chinese: are prostheses today sufficiently suitable? J Knee Surg 30(9):936–942
Funding
The authors are grateful to "GCS Ramsay Santé pour l’Enseignement et la Recherche" for funding the statistical analysis and manuscript preparation for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethicl approval
This study is a systematic review and meta-analysis of previously published clinicl studies. As such, ethical approval is not required, considering that the authors did not collect or analyse patient data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Beckers, L., Müller, J.H., Daxhelet, J. et al. Considerable inter-individual variability of tibial geometric ratios renders bone–implant mismatch unavoidable using off-the-shelf total knee arthroplasty: a systematic review and meta-analysis. Knee Surg Sports Traumatol Arthrosc 31, 1284–1298 (2023). https://doi.org/10.1007/s00167-021-06623-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-021-06623-7