Abstract
Aims/hypothesis
Diabetic dyslipidaemia contributes to the excess morbidity and mortality in patients with type 2 diabetes. Exogenous glucagon-like peptide 1 (GLP-1) lowers postprandial glycaemia predominantly by slowing gastric emptying. Therefore, the effects of GLP-1 on postprandial lipid levels and gastric emptying were assessed.
Methods
14 healthy male volunteers were studied with an i.v. infusion of GLP-1 (1.2 pmol kg−1 min−1) or placebo over 390 min in the fasting state. A solid test meal was served and gastric emptying was determined using a 13C-labelled sodium octanoate breath test. Venous blood was drawn frequently for measurement of glucose, insulin, C-peptide, glucagon, GLP-1, triglycerides and NEFA.
Results
GLP-1 administration lowered fasting and postprandial glycaemia (p<0.0001). Gastric emptying was delayed by GLP-1 compared with placebo (p<0.0001). During GLP-1 administration, insulin secretory responses were higher in the fasting state but lower after meal ingestion. After meal ingestion, triglyceride plasma levels increased by 0.33±0.14 mmol/l in the placebo experiments (p<0.0001). In contrast, the postprandial increase in triglyceride levels was completely abolished by GLP-1 (change in triglycerides, −0.023±0.045 mmol/l; p<0.05). During GLP-1 infusion, plasma concentrations of NEFA were suppressed by 39% in the fasting state (p<0.01) and by 31±5% after meal ingestion (p<0.01).
Conclusions/interpretation
GLP-1 improves postprandial lipidaemia, presumably as a result of delayed gastric emptying and insulin-mediated inhibition of lipolysis. Thus, by lowering both glucose and lipid concentrations, GLP-1 administration may reduce the cardiovascular risk in patients with type 2 diabetes.
Similar content being viewed by others
Introduction
Diabetic dyslipidaemia contributes to the excess morbidity and mortality in type 2 diabetes [1]. A number of studies have provided evidence for the association between postprandial triglyceride and NEFA levels and the risk of macrovascular diseases, such as myocardial infarction or stroke [2, 3]. Indeed, increased carotid intima–media thickness as well as impaired endothelial function can be detected in patients with postprandial hypertriglyceridaemia [4, 5]. Moreover, elevated NEFA levels are a strong predictor of insulin resistance, thereby aggravating hyperglycaemia in type 2 diabetes [1, 6]. Thus, therapeutic approaches aiming to reduce postprandial lipid concentrations may reduce the cardiovascular mortality in patients with and without type 2 diabetes.
The incretin hormone glucagon-like peptide 1 (GLP-1) and its analogues/derivatives (the so-called incretin mimetics) are promising candidates for future therapy of type 2 diabetes [7, 8]. The antidiabetic effects of GLP-1 include a glucose-dependent insulinotropic and glucagonostatic effect as well as deceleration of gastric emptying, which causes delayed entry of nutrients into the circulation [7, 9–12]. Because of these effects, postprandial hyperglycaemia can be efficiently counteracted by the administration of GLP-1 [11]. A number of different incretin mimetics are currently undergoing clinical trials for their therapeutic application in the pharmacotherapy of type 2 diabetes [7, 8]. However, while various studies have demonstrated the glucose-lowering potential of GLP-1 [7, 8], its effects on postprandial lipid metabolism have not yet been elucidated in detail.
In the present studies we hypothesised that slowing of gastric emptying by GLP-1 would abolish the rise in triglyceride concentrations after the ingestion of a mixed meal. Therefore, we assessed gastric emptying of a solid test meal and postprandial glucose and lipid homeostasis during i.v. administration of GLP-1 and placebo in healthy human subjects.
Subjects and methods
Study protocol
The study protocol was approved by the ethics committee of the Ruhr University of Bochum on 4 February 2003 (registration number 2074) before the study. Written informed consent was obtained from all participants.
Participants
Fourteen healthy male volunteers participated in the study. Their age was 24.2±2.0 years (mean±SD) and their BMI was 24.7±2.2 kg/m2. HbA1c was 5.4±0.2% (normal range 4.8–6.0%), total cholesterol concentration was 4.5±0.62 mmol/l (174±24 mg/dl), HDL-cholesterol concentration was 1.1±0.23 mmol/l (43±9 mg/dl), LDL-cholesterol concentration was 3.1±0.62 mmol/l (119±24 mg/dl), VLDL-cholesterol concentration was 0.31±0.16 mmol/l (12±6 mg/dl), triglyceride concentration was 0.95±0.24 mmol/l (84±21 mg/dl) and fasting glucose concentration was 5.2±0.38 mmol/l (94±7 mg/dl). None of the participants had a history of gastrointestinal disorders, had previously undergone abdominal surgery or was taking any medication with a known modulating effect on gastrointestinal motility or glucose and lipid metabolism. All participants were advised to maintain their usual dietary habits and to avoid strenuous exercise before the experiments.
Blood was drawn from all participants in the fasting state for measurements of standard haematological and clinical chemistry parameters. None of the participants had any abnormalities, either in terms of (1) anaemia (haemoglobin <120 g/l), or (2) an elevation of liver enzymes (alanine aminotransferase, aspartate aminotransferase, alkaline phosphatase, γ-glutamyl transferase) to activities higher than double the respective normal value, or (3) elevated creatinine concentrations (>1.5 mg/dl [114 μmol/l]).
Study design
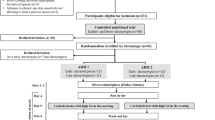
All participants were studied on three occasions. At a screening visit blood was drawn in the fasting state for determination of laboratory parameters and a clinical examination was performed. If subjects met the inclusion criteria, they were recruited for further tests as follows. On separate occasions, either GLP-1 (7–36)amide (1.2 pmol kg−1 min−1) or placebo was administered i.v. over 390 min (−30 to 360 min). In both experiments, a mixed test meal (1.05 MJ [250 kcal]) was ingested at 0 min. Capillary and venous blood samples were collected frequently throughout the experiments for measurement of glucose, GLP-1, insulin, C-peptide, glucagon, NEFA and triglycerides. Gastric emptying was also determined over 360 min. The two experiments were carried out in randomised order. An interval of at least 2 days was kept between the tests in order to avoid carryover effects.
Peptides
Synthetic GLP-1 (7–36)amide was a kind gift from Restoragen, Lincoln, NE, USA. Peptides were sterile filtered and processed for infusion as described [11].
Experimental procedures
The tests were performed in the morning after an overnight fast, with subjects in a supine position throughout the experiments and with the upper body raised by 30°. Two forearm veins were punctured with a Teflon cannula (Moskito 123, 18 gauge; Vygon, Aachen, Germany), and kept patent using 0.9% NaCl (for blood sampling and GLP-1/placebo administration respectively).
The experiments were started after drawing basal blood samples (−45 and −30 min) with the infusion of GLP-1 (7–36) amide or placebo at −30 min. At 0 min, each participant was given a standard test meal (one egg, two slices of white bread, 5 g margarine, 150 ml water; 55% carbohydrates, 15% protein, 30% lipids; total energy content 1.05 MJ-labelled) containing 100 mg 13C-sodium octanoate, which was mixed into the raw egg before careful cooking. Breath samples were collected at 15-min intervals during the first 180 min and at 20-min intervals during the last 180 min. Capillary and venous blood samples were collected at 30-min intervals.
Blood specimens
Venous blood was drawn into chilled tubes containing EDTA and aprotinin (Trasylol; 20,000 kIU/ml, 200 μl per 10 ml blood; Bayer, Leverkusen, Germany) and kept on ice. After centrifugation at 4°C, plasma for hormone analyses was kept frozen at −28°C. Capillary blood samples (approximately 100 μl) were added to NaF (Microvette CB 300; Sarstedt, Nümbrecht, Germany) for the immediate measurement of glucose.
Determination of gastric emptying
Gastric emptying was determined as described [11]. Briefly, 13C-labelled sodium octanoate (100 mg; Euriso-top, Saint-Aubin, France) was used to label the solid component of the test meal. At intervals of 15 or 20 min, breath specimens were sampled into gas-tight plastic bags and the 13CO2 content was determined within 24 h by non-dispersive infrared spectrometry (Wagner Analysentechnik, Bremen, Germany).
To measure the proportion of the substrate given by mouth that was metabolised, the results were expressed as the percentage of the dose of 13C recovered (PDR) over time for each time interval, from which the cumulative PDR (cPDR) for each time interval was calculated according to Ghoos et al. [13].
Results of the octanoate breath test for gastric emptying were evaluated by non-linear regression analysis (Prism version 2; Graphpad, San Diego, CA, USA) of the 13CO2 excretion curves (PDR), using the formula: PDR(t)=at be−ct, which was derived from the χ2 distribution. The expression ln a, as the gastric emptying coefficient, is a reliable parameter to describe the rate at which the stomach empties [13].
Values of the cumulative percentage of 13CO2 were fitted using a model given by \(cPDR{\left( t \right)} = M{\left( {1 - e^{{ - kt}} } \right)}^{\beta } \), where cPDR is the cumulative percentage dose of 13C recovered at time t in hours, and M, k and β are regression estimated constants, with M the total amount of 13CO2 expired when time is infinite.
Gastric emptying was expressed as the percentage of the initial gastric content (M=100%) by computing the difference from this initial value at each time point according to the following formula: gastric content (t)=([M−cPDR(t)]/M)100 (%).
Laboratory determinations
Glucose was measured as described [11, 14] using a Glucose Analyser 2 (Beckman Instruments, Munich, Germany).
Insulin was measured as described [11] using an insulin microparticle enzyme immunoassay (MEIA; IMx Insulin, Abbott Laboratories, Wiesbaden, Germany). The intra-assay CV was ∼4%.
C-peptide was measured as described [11] using an ELISA from Dako, Ely, UK. Intra-assay CV were 3.3–5.7% and inter-assay CV was 4.6–5.7%. Human insulin and C-peptide were used as standards.
Immunoreactive glucagon was measured using porcine antibody 4305 in ethanol-extracted plasma, as previously described [15]. The detection limit was <1 pmol/l. The intra-assay CV was 6.7% and the inter-assay CV was 16%.
GLP-1 immunoreactivity was determined using a radioimmunoassay specific for the C-terminus of the peptide [11]. This assay measures the sum of the intact peptide plus the primary metabolite, GLP-1 (9–36) amide using the antiserum 89390 and synthetic GLP-1 (7–36 amide) as standard. This assay cross-reacts less than 0.01% with C-terminally truncated fragments and 83% with GLP-1 (9–36) amide. The detection limit was 3 pmol/l.
Triglycerides were measured using an enzymatic colour test system (Olympus System Reagent triglyceride OSR 6133; Olympus, Hamburg, Germany). NEFA were determined using reagents from Wako Chemicals, Neuss, Germany, by spectrophotometric analysis.
Statistical analysis
Results are reported as mean±SEM. For integrated incremental responses of triglycerides, the positive area under the curve was calculated using the trapezoidal rule (baseline subtracted). All statistical calculations of concentration time series were carried out using paired repeated measures ANOVA using Statistica Version 5.0 (Statsoft Europe, Hamburg, Germany). This analysis provides p values for the overall differences between the experiments, differences over time, and for the interaction of experiment with time. If a significant interaction of treatment and time was documented (p<0.05), and for the comparison of time-independent variables, individual values were compared by paired one-way ANOVA. A two-sided p value <0.05 was taken to indicate a significant difference.
Results
Plasma concentrations of total GLP-1 were significantly higher during the exogenous infusion than with placebo (139±15 vs 12±2 pmol/l; p<0.0001). Glucose concentrations rose significantly after meal ingestion during the placebo experiments (p<0.0001). As expected, glucose levels were significantly reduced by GLP-1 in the fasting state and declined further after ingestion of the test meal (Fig. 1). GLP-1 administration led to increases in fasting insulin and C-peptide concentrations compared with placebo (p<0.05 at t=−15 and 0 min). However, immediately after meal ingestion (from t=15 to t=90 min) insulin and C-peptide levels were even lower in the experiments with GLP-1 infusion than in those with placebo (p<0.05; Fig. 1). Consistent with previous reports [11, 16], GLP-1 led to suppression of the glucagon concentration (t=0 min) both under fasting conditions and after the test meal (from 210 to 300 min; Fig. 2).
Plasma concentrations of glucose (a), insulin (b) and C-peptide (c) during i.v. administration of GLP-1 (1.2 pmol kg−1 min−1, filled circles) or placebo (open circles) in 14 healthy male subjects. At t=0 min, a mixed test (1.05 MJ) meal was served (arrows). Data are mean±SEM. p values were calculated using paired repeated measures ANOVA as follows: p=0.053 (a), p=0.85 (b), p=0.54 (c) for differences between experiments; p<0.00001 (a–c) for differences over time; and p<0.00001 (a–c) for differences due to the interaction of experiment and time. *p<0.05 for differences vs placebo at individual time points (one-way ANOVA)
Plasma concentrations of glucagon during i.v. administration of GLP-1 (1.2 pmol kg−1 min−1, filled circles) or placebo (open circles) in 14 healthy male subjects. At t=0 min, a mixed test (250 kcal) meal was served (arrow). Data are mean±SEM. The p values were calculated using paired repeated measures ANOVA as follows: p=0.12 for differences between experiments; p<0.00001 for differences over time and for differences due to the interaction of experiment and time. * p<0.05 for differences vs placebo at individual time points (one-way ANOVA)
Fasting triglyceride levels were not different between the experiments with the administration of GLP-1 and placebo (Fig. 3). During the placebo experiments triglyceride levels increased significantly after the test meal (p<0.0001), peak levels being reached after 180 min (mean increase after 180 min, 0.33±0.14 mmol/l [29±12 mg/dl]). In contrast, the postprandial increase in triglyceride levels was completely abolished by GLP-1 (mean change after 180 min, −0.023±0.045 mmol/l [−2±4 mg/dl]; p<0.05). During GLP-1 administration, postprandial triglyceride concentrations were lower than with placebo (p=0.00011; Fig. 3). Also, the area under the triglyceride concentration curve was significantly lower during GLP-1 administration (14.3±4.9 vs 82.8±20.9 mmol l−1 min [1263±436 vs 7331±1850 mg dl−1 min] during GLP-1 and placebo administration, respectively; p=0.011).
Plasma concentrations of triglycerides (a) and NEFA (b) during i.v. administration of GLP-1 (1.2 pmol kg−1 min−1, filled circles) or placebo (open circles) in 14 healthy male subjects. At t=0 min, a mixed test (1.05 MJ) meal was served (arrows). Data are mean±SEM. The p-values were calculated using paired repeated measures ANOVA as follows: p=0.35 (a) and p=0.0027 (b) for differences between the experiments, p<0.0001 (a, b for differences over time, and p=0.00011 (a) and p<0.0001 b for differences due to the interaction of time and experiment. *p<0.05 for differences vs placebo at individual time points (one-way ANOVA)
Plasma concentrations of NEFA were suppressed over the initial 120 min after meal ingestion and rose significantly afterwards in the placebo experiments (p<0.0001; Fig. 3). GLP-1 administration lowered NEFA concentrations by 39% in the fasting state (at t=0 min; p=0.0036). After ingestion of the test meal, NEFA levels increased somewhat from t=60 to 120 min, but remained significantly lower than during the placebo experiments during the subsequent 180 min (p<0.0001). The mean concentrations of NEFA during the 360 min after meal ingestion were 31±5% lower in the GLP-1 experiments than during placebo administration (p=0.0029).
Gastric emptying was almost complete after 6 h during the placebo experiments (Fig. 4). In contrast, with GLP-1 ∼50% of the initial content was still in the stomach after 360 min (p<0.0001). The time course of gastric emptying was significantly delayed by GLP-1 over the entire study period (p<0.0001).
Time course of gastric emptying of a solid test meal (arrow) during i.v. administration of GLP-1 (1.2 pmol kg−1 min−1, filled circles) or placebo (open circles) in 14 healthy male subjects. Data are mean±SEM. The p values were calculated using paired repeated measures ANOVA as follows: p<0.0001 for differences between experiments, differences over time, and for differences due to the interaction of experiment and time. *p<0.05 for differences vs placebo at individual time points (one-way ANOVA)
Discussion
The excess postprandial rises in triglyceride and NEFA concentrations are independent risk factors for the development of macrovascular complications in patients with type 2 diabetes [1–3]. Thus, postprandial triglyceride concentrations have been associated with increased intima–media thickness as well as impaired endothelial function [4, 6]. The present data show that i.v. administration of GLP-1 during the ingestion of a mixed test meal not only reduces glycaemia but also fully abolishes the postprandial rise in triglyceride levels. Moreover, both fasting and postprandial NEFA levels were markedly reduced by the incretin hormone. Given the importance of NEFA for the regulation of hepatic glucose production [17], this effect may explain the previously observed effects of GLP-1 on insulin sensitivity [18]. The improvement in postprandial lipidaemia therefore adds to the multiple beneficial effects of GLP-1 in the treatment of patients with type 2 diabetes.
One obvious question arising from these data is: which mechanism mediated the effects of GLP-1 on postprandial lipid concentrations? Regarding the triglyceride concentrations, the most likely candidate appears to be the GLP-1-induced deceleration of gastric emptying. Thus, it seems plausible that delayed entry of nutrients into the duodenum prevented the increase in triglyceride plasma levels that is typically found after meal ingestion. Indeed, the glucose-lowering effects of GLP-1 in the postprandial state can largely be explained the deceleration of gastric emptying [11, 19], and direct intraduodenal glucose administration raises glucose plasma concentrations even in the presence of increased GLP-1 concentrations [20]. Alternatively, it seems possible that GLP-1 directly inhibited triglyceride absorption from the gut, potentially through inhibition of gastric lipases [21]. This explanation would be consistent with a recent series of elegant experiments in rats demonstrating that GLP-1 reduces the intestinal absorption of triolein and inhibits intestinal lymph flow [22]. It therefore appears possible that a combination of delayed gastric emptying and reduced intestinal lipid absorption prevented the postprandial increase in triglyceride levels.
Regarding the effects of GLP-1 on NEFA levels, the inhibition of gastric emptying and lipid absorption alone cannot explain the changes in the concentration–time pattern, because a significant reduction in NEFA concentrations was already observed during the administration of GLP-1 in the fasting state. It is more likely that the effects of GLP-1 on NEFA concentrations were mediated by the changes in insulin plasma levels. This explanation would be consistent with the pivotal role of insulin in suppressing lipolysis [23]. In fact, whenever insulin concentrations were high, NEFA levels were suppressed (e.g. at t=0 min during GLP-1 administration), whereas NEFA concentrations tended to increase when insulin levels dropped (e.g. from 60 to 120 min during GLP-1 administration). In addition, glucagon concentrations during GLP-1 infusion seemed to closely mirror the NEFA levels. Thus, the reduction in glucagon levels might have contributed to the suppression of lipolysis during GLP-1 infusion [23, 24]. It is, however, difficult to distinguish direct GLP-1 effects on alpha-cell secretion from indirect effects via increased insulin secretion, since glucagon secretion may be regulated by the intra-islet release of insulin [24–26].
It is important to note that in the present studies the test meal had a relatively low energy content (1.05 MJ), which led to a rather modest increase in postprandial triglyceride levels (44% at t=180 min vs baseline). This was done because this test meal has been validated previously for the determination of gastric emptying of solid meals [27]. Therefore, despite the complete lack of an increase in postprandial lipid concentrations observed after a low-energy test meal in this study, it is possible that a meal with a higher lipid content would elevate lipid plasma concentrations even in the presence of GLP-1.
While the present results imply a potent lipid-lowering effect of i.v. GLP-1 in healthy human subjects, results may vary during the long-term subcutaneous administration of GLP-1 analogues/derivatives in patients with type 2 diabetes. In fact, the antihyperglycaemic effect of GLP-1 appears to be greater during i.v. than during s.c. administration [16, 18, 28]. Moreover, in previous studies that have investigated the effects of chronic s.c. administration of GLP-1 or the incretin mimetic exenatide, only very modest reductions in fasting triglycerides and NEFA have been reported [18, 29–32]. In the light of the present data showing significant reductions in the postprandial concentrations of both NEFA and triglycerides during an acute i.v. infusion of GLP-1, it seems worthwhile to examine further the effect of incretin mimetics on postprandial lipid excursions after chronic s.c. administration in patients with type 2 diabetes.
Since the present experiments were carried out over an observation period of 6 h, it is theoretically possible that a later compensatory increase in triglyceride plasma levels was overlooked. However, no increase in triglyceride concentrations was detected until the end of the observation period during GLP-1 administration despite ∼50% emptying of the stomach. In contrast, when a similar degree of gastric emptying was reached during the placebo experiments (at t=180 min), triglyceride plasma concentrations had reached their peak levels already. Therefore, it seems unlikely that triglyceride concentrations would have increased much at a later time point after meal ingestion. This finding may also be interpreted as an indication that the lipid-lowering effects of GLP-1 were not only due to delayed gastric emptying, but also due to other mechanisms, such as increased clearance or reduced endogenous synthesis of triglycerides. Future studies employing direct intraduodenal lipid infusions [33] or using prokinetic drugs to counterbalance the GLP-1-induced deceleration of gastric emptying [12] may be more suited to the further elucidation of these mechanisms.
In conclusion, these studies demonstrate that the postprandial increase in triglyceride concentrations was abolished completely by the i.v. infusion of GLP-1. This was probably a result of the marked deceleration of gastric emptying and, potentially, inhibition of intestinal lipid absorption by GLP-1. Moreover, both fasting and postprandial plasma concentrations of NEFA can be lowered efficiently by the i.v. administration of GLP-1. Given the close association of postprandial lipid concentrations with the increased risk of macrovascular diseases in patients with type 2 diabetes, these findings suggest additional beneficial effects of GLP-1 in the treatment of patients with diabetic dyslipidaemia.
Abbreviations
- GLP-1:
-
glucagon-like peptide 1
- PDR:
-
percentage of dose recovered
References
Taskinen MR (2003) Diabetic dyslipidaemia: from basic research to clinical practice. Diabetologia 46:733–749
Stampfer MJ, Krauss RM, Ma J et al (1996) A prospective study of triglyceride level, low-density lipoprotein particle diameter, and risk of myocardial infarction. JAMA 276:882–888
Patsch JR, Miesenbock G, Hopferwieser T et al (1992) Relation of triglyceride metabolism and coronary artery disease. Studies in the postprandial state. Arterioscler Thromb 12:1336–1345
Temelkova-Kurktschiev T, Hanefeld M (2004) The lipid triad in type 2 diabetes—prevalence and relevance of hypertriglyceridaemia/low high-density lipoprotein syndrome in type 2 diabetes. Exp Clin Endocrinol Diabetes 112:757–759
Lundman P, Eriksson MJ, Stuhlinger M et al (2001) Mild-to-moderate hypertriglyceridemia in young men is associated with endothelial dysfunction and increased plasma concentrations of asymmetric dimethylarginine. J Am Coll Cardiol 38:111–116
Hennig B, Toborek M, McClain CJ (2001) High-energy diets, fatty acids and endothelial cell function: implications for atherosclerosis. J Am Coll Nutr 20:97–105
Drucker DJ (2003) Enhancing incretin action for the treatment of type 2 diabetes. Diabetes Care 26:2929–2940
Meier JJ, Nauck MA (2005) Glucagon-like peptide 1 (GLP-1) in biology and pathology. Diabetes Metab Res Rev 21:91–117
Gutniak MK, Holst JJ, Ørskov C, Åhren B, Efendic S (1992) Antidiabetogenic effect of glucagon-like peptide-1 (7–36)amide in normal subjects and patients with diabetes mellitus. N Engl J Med 326:1316–1322
Wettergren A, Schjoldager B, Mortensen PE et al (1993) Truncated GLP-1 (proglucagon 78–107-amide) inhibits gastric and pancreatic functions in man. Dig Dis Sci 38:665–673
Meier JJ, Gallwitz B, Salmen S et al (2003) Normalization of glucose concentrations and deceleration of gastric emptying after solid meals during intravenous glucagon-like peptide 1 in patients with type 2 diabetes. J Clin Endocrinol Metab 88:2719–2725
Meier JJ, Kemmeries G, Holst JJ, Nauck MA (2005) Erythromycin antagonises the deceleration of gastric emptying by glucagon-like peptide 1 (GLP-1) and unmasks its insulinotropic effect in healthy subjects. Diabetes 54:2212–2218
Ghoos YF, Maes BD, Geypens BJ et al (1993) Measurement of gastric emptying rate of solid meals by means of a carbon-labeled octanoic acid breath test. Gastroenterology 104:1640–1647
Meier JJ, Hücking K, Holst JJ et al (2001) Reduced insulinotropic effect of gastric inhibitory polypeptide in first-degree relatives of patients with type 2 diabetes. Diabetes 50:2497–2504
Holst JJ (1997) Enteroglucagon. Annu Rev Physiol 59:257–271
Nauck MA, Kleine N, Ørskov C et al (1993) Normalization of fasting hyperglycaemia by exogenous glucagon-like peptide 1 (7–36 amide) in type 2 (non-insulin-dependent) diabetic patients. Diabetologia 36:741–744
Boden G, Jadali F (1991) Effects of lipid on basal carbohydrate metabolism in normal men. Diabetes 40:686–692
Zander M, Madsbad S, Madsen JL, Holst JJ (2002) Effect of 6-week course of glucagon-like peptide 1 on glycaemic control, insulin sensitivity, and beta-cell function in type 2 diabetes: a parallel-group study. Lancet 359:824–830
Willms B, Werner J, Holst JJ et al (1996) Gastric emptying, glucose responses, and insulin secretion after a liquid test meal: effects of exogenous glucagon-like peptide-1 (GLP-1)-(7–36) amide in type 2 (noninsulin-dependent) diabetic patients. J Clin Endocrinol Metab 81:327–332
Schirra J, Nicolaus M, Roggel R et al. (2005) Endogenous GLP-1 controls endocrine pancreatic secretion and antro-pyloro-duodenal motility in humans. Gut 28. E-pub ahead of print
Wojdemann M, Wettergren A, Sternby B et al (1998) Inhibition of human gastric lipase secretion by glucagon-like peptide-1. Dig Dis Sci 43:799–805
Qin X, Shen H, Liu M et al (2005) GLP-1 reduces intestinal lymph flow, triglyceride absorption, and apolipoprotein production in rats. Am J Physiol Gastrointest Liver Physiol 288:G943–G949
Mahler R, Stafford WS, Tarrant ME, Ashmore J (1964) The effect of insulin on lipolysis. Diabetes 13:297–302
Samols E, Stagner JI, Ewart RB, Marks V (1988) The order of islet microvascular cellular perfusion is B–A–D in the perfused rat pancreas. J Clin Invest 82:350–353
Weir GC, Bonner-Weir S (1990) Islets of Langerhans: the puzzle of intraislet interactions and their relevance to diabetes. J Clin Invest 85:983–987.
Franklin I, Gromada J, Gjinovci A, Theander S, Wollheim CB (2005) Beta-cell secretory products activate alpha-cell ATP-dependent potassium channels to inhibit glucagon release. Diabetes 54:1808–1815
Braden B, Adams S, Duan LP et al (1995) The [13C]acetate breath test accurately reflects gastric emptying of liquids in both liquid and semisolid test meals. Gastroenterology 108:1048–1055
Nauck MA, Meier JJ (2005) Glucagon-like peptide 1 and its derivatives in the treatment of diabetes. Regul Pept 128:135–148
Toft-Nielsen M-B, Madsbad S, Holst JJ (1999) Continuous subcutaneous infusion of glucagon-like peptide 1 lowers plasma glucose and reduces appetite in type 2 diabetic patients. Diabetes Care 22:1137–1143
Fineman MS, Bicsak TA, Shen LZ et al (2003) Effect on glycemic control of exenatide (synthetic exendin-4) additive to existing metformin and/or sulfonylurea treatment in patients with type 2 diabetes. Diabetes Care 26:2370–2377
Defronzo RA, Ratner RE, Han J et al (2005) Effects of exenatide (exendin-4) on glycemic control and weight over 30 weeks in metformin-treated patients with type 2 diabetes. Diabetes Care 28:1092–1100
Buse JB, Henry RR, Han J et al (2004) Effects of exenatide (exendin-4) on glycemic control over 30 weeks in sulfonylurea-treated patients with type 2 diabetes. Diabetes Care 27:2628–2635
Schirra J, Houk P, Wank U et al (2000) Effects of glucagon-like peptide-1 (7–36)amide on antro-pyloro-duodenal motility in the interdigestive state and with duodenal lipid perfusion in humans. Gut 56:622–631
Acknowledgements
The technical assistance of B. Baller and L. Bagger is gratefully acknowledged. This study was supported by grants from the Deutsche Forschungsgemeinschaft (grants Me 2096/2-1 and Na 203/6-1), the Deutsche Diabetes Gesellschaft (to J. J. Meier), the Wilhelm-Sander-Stiftung (grant 2002.025.1 to J. J. Meier) and the Ruhr-University Bochum (FoRUM F382-03; to J. J. Meier).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Meier, J.J., Gethmann, A., Götze, O. et al. Glucagon-like peptide 1 abolishes the postprandial rise in triglyceride concentrations and lowers levels of non-esterified fatty acids in humans. Diabetologia 49, 452–458 (2006). https://doi.org/10.1007/s00125-005-0126-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-005-0126-y