Abstract
Purpose
This study evaluated the relationship between dose–volume histogram (DVH) parameters and pulmonary complications after neoadjuvant chemoradiotherapy (NACRT) followed by surgery for lung cancer. We also examined a new DVH parameter, because the unresected lung should be more spared than the later resected lung.
Patients and methods
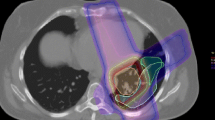
Data from 43 non-small cell lung cancer patients were retrospectively analyzed. The DVH parameters of the lung were calculated from the total bilateral lung volume minus (1) the gross tumor volume (DVHg) or (2) the later resected lung volume (DVHr). Radiation pneumonitis (RP) and fistula, including bronchopleural and pulmonary fistula, were graded as the pulmonary complications. Factors affecting the incidences of grade 2 or higher RP (≥G2 RP) and fistula were analyzed.
Results
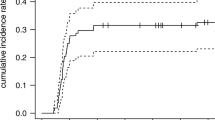
Sixteen patients (37 %) experienced ≥G2 RP and a V20 value of the total lung minus the later resected lung (V20r) ≥ 12 % was a significant factor affecting the incidence of ≥G2 RP (p = 0.032). Six patients (14 %) developed a fistula and a V35 value of the total lung minus the gross tumor (V35g) ≥ 19 % and a V40g ≥ 16 % were significant factors affecting the incidence of fistula (p = 0.002 and 0.009, respectively).
Conclusion
These DVH parameters may be related to the incidences of ≥G2 RP and fistula.
Zusammenfassung
Zielsetzung
In dieser Studie wurde die Beziehung zwischen Dosis-Volumen-Histogramm-(DVH-)Parametern und pulmonalen Komplikationen nach neoadjuvanter Radiochemotherapie (NARCT) und nachfolgender Operation beim Lungenkarzinom untersucht. Zudem wurde ein neuer DVH-Parameter untersucht, da das nichtresezierte Lungengewebe mehr geschont werden sollte als reseziertes Gewebe.
Patienten und Methoden
Daten von 43 Patienten mit nicht-kleinzelligem Bronchialkarzinom wurden retrospektiv analysiert. Die DVH-Parameter der Lunge wurden aus dem gesamten beidseitigen Lungenvolumen minus (1) das makroskopische Tumorvolumen (DVHg) oder (2) das resezierte Lungenvolumen (DVHr) ermittelt. Strahlenpneumonitis (RP) und Fisteln, einschließlich bronchopleuraler und pulmonaler Fisteln, wurden als pulmonale Komplikationen nach Graden abgestuft. Außerdem erfolgte eine Analyse der Faktoren, welche die Inzidenz einer RP von Grad 2 oder höher (≥G2 RP) und von Fisteln beeinflussen.
Ergebnisse
Bei 16 Patienten (37 %) wurde eine RP ≥G2 festgestellt, wobei der V20-Wert des Gesamtlungenvolumens minus dem später resezierten Lungenvolumen (V20r)≥ 12 % ein signifikanter Einflussfaktor bezüglich der Inzidenz einer RP ≥G2 war (p = 0,032). Insgesamt 6 Patienten (14 %) entwickelten eine Fistel. Signifikante Einflussfaktoren bezüglich der Inzidenz von Fisteln waren ein V35- bzw. V40-Wert des Gesamtlungenvolumens minus dem Gesamttumorvolumen V35g ≥ 19 % und V40g ≥ 16 % (p = 0,002 bzw. 0,009).
Schlussfolgerung
Diese DVH-Parameter stehen möglicherweise im Zusammenhang mit einer RP ≥G2 und Fisteln.




Similar content being viewed by others
References
National Comprehensive Cancer Network Non-small cell lung cancer, NCCN Clinical Practice Guidelines in Oncology: version 7.2015. http://www.nccn.org/professionals/physician_gls/pdf/nscl.pdf. Accessed 07/14/2015
Stamatis G, Djuric D, Eberhardt W et al (2002) Postoperative morbidity and mortality after induction chemoradiotherapy for locally advanced lung cancer: an analysis of 350 operated patients. Eur J Cardiothorac Surg 22:292–297
Cerfolio RJ (2001) The incidence, etiology, and prevention of postresectional bronchopleural fistula. Semin Thorac Cardiovasc Surg 13:3–7
Lois M, Noppen M (2005) Bronchopleural fistulas: an overview of the problem with special focus on endoscopic management. Chest 128:3955–3965
Fujita S, Katakami N, Takahashi Y et al (2006) Postoperative complications after induction chemoradiotherapy in patients with non-small-cell lung cancer. Eur J Cardiothorac Surg 29:896–901
Birdas TJ, Morad MH, Okereke IC et al (2012) Risk factors for bronchopleural fistula after right pneumonectomy: does eliminating the stump diverticulum provide protection? Ann Surg Oncol 19:1336–1342
Marks LB, Bentzen SM, Deasy JO et al (2010) Radiation dose-volume effects in the lung. Int J Radiat Oncol Biol Phys 76:70–76
Yokomise H, Gotoh M, Okamoto T et al (2007) Induction chemoradiotherapy (carboplatin-taxane and concurrent 50-Gy radiation) for bulky cN2, N3 non-small cell lung cancer. J Thorac Cardiovasc Surg 133:1179–1185
Yokomise H, Liu D, Ishikawa S et al (2013) Chemotherapy followed by surgery on the basis of biomarker examination for patients with advanced non-small cell lung cancer. Anticancer Res 33:5597–5602
Kong FM, Wang S (2015) Nondosimetric risk factors for radiation-induced lung toxicity. Semin Radiat Oncol 25:100–109
Vogelius IR, Bentzen SM (2012) A literature-based meta-analysis of clinical risk factors for development of radiation induced pneumonitis. Acta Oncol 51:975–983
Yamamoto R, Tada H, Kishi A et al (2000) Effects of preoperative chemotherapy and radiation therapy on human bronchial blood flow. J Thorac Cardiovasc Surg 119:939–945
Inui K, Takahashi Y, Hasegawa S et al (1993) Effect of preoperative irradiation on wound healing after bronchial anastomosis in mongrel dogs. J Thorac Cardiovasc Surg 106:1059–1064
Acknowledgements
This study was supported by a Grant-in-Aid for Cancer Research (H23-009) from the Ministry of Health, Labour and Welfare of Japan, and JSPS KAKENHI Grant Numbers 26461892 and 15K19798.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S. Takahashi, T. Go, Y. Kasai, H. Yokomise, and T. Shibata state that there are no conflicts of interest.
Ethical standards
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Takahashi, S., Go, T., Kasai, Y. et al. Relationship between dose–volume parameters and pulmonary complications after neoadjuvant chemoradiotherapy followed by surgery for lung cancer. Strahlenther Onkol 192, 658–667 (2016). https://doi.org/10.1007/s00066-016-1021-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00066-016-1021-9