Abstract
Objective
To evaluate the effect of the prolonged systematic use of topical SDD (tobramycin 80 mg, polymyxin E 100 mg, amphotericin B 500 mg) on ICU ecology as expressed by changes in tracheal colonization and bacterial resistances.
Design
Prospective microbiological survey.
Setting
Polyvalent ICU of a 2000 beds general hospital.
Patients
Data concerning bacterial strains isolated from the tracheo-bronchial aspirates of all the patients admitted to a polyvalent ICU over 3 consecutive periods of 12 months ('88, '89, '90) were prospectively entered in a database and subsequently analyzed. During a 3-year period 502 patients required artificial ventilation for more than 72 h and 332 of them ('89 and '90) were treated with SDD. All samples collected within 72 h from ICU admission were excluded as well as duplicate samples from the same patients.
Intervention
All the patients admitted to the ICU in '89 and '90 and submitted to artificial ventilation for at least 24 h were routinely treated with topical SDD without i.v. antibiotic prophylaxis; in '88 SDD was not empoloyed.
Measurements and results
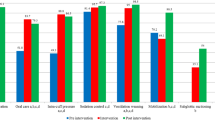
Criteria for collecting sputum samples and microbiological procedures remained unchanged troughout the study-time. Positive sputum were significantly less in '89 (80.8% versus 92.3%p<0.001) and this was due to a very sharp decrease in the isolation of Gram-negative strains from 43–28% (−64%p<0.0001) involving both:Enterobacteriaceae (−45%) andPseudomonaceae (−77%). In 1990; however, a new increase in Gram negative was observed, although the overall amount of Gram-negative was still 49% lower in '90 if compared to '88 (p<0.0001). A dramatic increase inPseudomonas isolation was the only factor responsible for the “rebound” observed. An increasing percentage ofPseudomonas developed a resistance towards tobramycin and only 45% ofPseudomonas strains turned out to be sensible to tobramycin in '90 against 79% in '88. A similar trend was registered for all aminoglycosides with the exception of amikacin. Gram-positive colonizations tended to increase (+63%) (p<0.0001) and this was mainly due to Coagulase negativeStaphylococci (+290%p<0.0001) andS. pneumoniae, whereasS. aureus isolations decreased (−18%) but not significantly.
Conclusions
Our data suggest that the prolonged use of SDD is associated with dramatic changes in ICU ecology: the incidence of Gram negative colonization is significantly diminished by SDD whereas Gram positive tend to increase.Pseudomonas developed an increasing resistance towards tobramycin one of the components of the SDD formula we used.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Stoutenbeek CP, van Saane HKF, Miranda DR, Zandstra DF (1984) The effect of selective decontamination of the digestive tract on colonization and infection rate in multiple trauma patients. Intensive Care Med 10:185–192
Alcock SR (1988) Prospective study of colonization in ICU patients treated with SDD and systemic cefotaxime: Glasgow results. In: Vincent JL (ed) Infection control by Selective Decontamination. Springer, Berlin Heidelberg New York Tokyo, pp 117
Kerver AJH, Rommes JH, Mevissen-Verhage EAE, Hulstaert PF, Vos A, Verhoef J, Wittebol P (1988) Prevention of colonization and infection in critically ill patients: a prospective randomized study. Crit Care Med 16:1087–1093
Konrad F, Swalbe B, Heeg K, Wagner H, Wiedeck H, Kilian J (1989) Frequency of colonization and pneumonia and development of resistance in long-term ventilated intensive care patients subjected to selective decontamination of the digestive tract. Anaesthesist 38:99–109
Ledingham LM, Alcock SR, Eastway AT, McDonal JC, McKay IC, Ramsay G (1988) Triple regimen of selective digestive decontamination of the digestive tract, systemic cefotaxime and microbiological surveillance for prevention of acquired infection. Intensive care. Lancet 8589:785–790
Mc Clelland P, Murray AE, Williams PS, van Saene HK, Gilbertson AA, Mostafa SM, Bone JM (1990) Reducing sepsis in severe combined acute renal and respiratory failure by selective decontamination of the digestive tract. Crit Care Med 18:935–939
Thulig B, Hartenauer U, Diemer W, Lawin P, Ritzerfeld W (1988) Infection control by selective flora suppression in critically ill patients. In: Vincent JL (ed) Infection control by selective decontamination. Springer, Berlin Heidelberg New York Tokyo, pp 120
Alcock SR (1990) Short term parenteral antibiotic used as a supplement to SDD regimens. Infection 18 [Suppl 1]:S14–18
Vandenbroucke CM, Vandenbroucke JP (1991) Effect of selective decontamination of the digestive tract on respiratory tract infections and mortality in the intensive unit. Lancet 338:859–862
Vollard EJ, Clasener HA, Janssen AJ, Wynne HJ (1990) Influence of cefotaxime on microbial colonization resistance in healthy volunteers. J Antimicrob Chemother 26:117–123
Flaherty J, Nathan C, Kabins SA, Weinstein RA (1990) Pilot trial of selective digestive decontamination for prevention of bacterial infection in an intensive care unit. J Infect Dis 162:1393–1397
Nardi G, Valentinis U, Bartaletti R, Bello A, De Monte A, Muzzi R, Giordano F, Troncon MG (1990) Effectiveness of topical selective decontamination without any systemic antibiotic prophylaxis, in the prevention of pulmonary infections in ICU patients. Minerva Anesthesiol 56:19–26
Pugin J, Auckenthale R, Lew DP, Suter PM (1991) Oropharyngeal decontamination decreases incidence of ventilator-associated pneumonia. JAMA 265:2704–2710
Nardi G, Bartaletti R, De Monte A, Giordano F, Muzzi R (1990) It is necessary to associate a systemic antibiotic prophylaxis to selective digestive decontamination? (Abstract) Intensive Care Med 16 [Suppl 1]:S33
Gastinne H, Wolff M, Delatour F, Faurisson F, Chevret S (1992) A controlled trial in intensive care units of selective decontamination of the digestive tract with nonabsorbable antibiotics. N Engl J Med 326:594–599
Johanson WG, Pierce AK, Sanford JP, Thomas GD (1972) Nosocomial respiratory infections with Gram negative bacilli: the significance of colonization of the respiratory tract. Ann Intern Med 77:701–706
Andrews CP, Coalson JJ, Smith JD (1981) Diagnosis of nosocomial bacterial pneumonia in acute diffuse lung injury. Chest, 80:254–260
Bell RC, Coalson JJ, Smith JD (1983) Multiple organ system failure and infection in adult respiratory distress syndrome. Ann Intern Med (1983) 99:293–297
Chastre J, Fagon JY, Lamer C (1991) Diagnosis of lung infection in intensive care unit patients using the protected specimen Brush technique. In: Vinvent JL (ed) Update in intensive care and emergency medicine 91. Springer, Berlin Heidelberg New York Tokyo, pp 357–364
Rouby JJ, Poete P, Bodin L (1991) The protected minialveolar lavage technique for the diagnosis of nosocomial pneumonia. In: Vincent JL (ed) Update in intensive care and emergency medicine 91. Springer, Berlin Heidelberg New York Tokyo, pp 365–378
Geckler RW, Gremillion DH, Mc Allister CK, Ellenbogen C (1977) Microscopy and batteriological comparison of paired sputa and transtracheal aspirates. J Clin Microbiol 6:396–399
Murray PR, Washington JA (1975) Microscopy and bacteriological anallysis of expectorated sputum. Mayo Clin Proc 50:339–344
Lennette EH, Spaulding EH, Truant JP (1974) In: Truant JP (ed) Manual of clinical microbiology, 2nd edn. American Society for Microbiology Washington DC
National Committee for Clinical Laboratory Standard (1985) Methods for dilution antimicrobial susceptibility tests for bacteria that grow aerobically; approvated standards. NCCLS Pubblication M7-A
Van Saene HKF, Stoutenbeek CP, Zandstra DF (1988) Cefotaxime combined with selective digestive decontamination in long-term intensive care unit patients: virtual absence of emergence of resistance (Abstr). In: Vincent JL (ed) Infection control by selective decontamination. Springer, Berlin Heidelberg New York Tokyo, pp 146
Unertl K, Ruckdeschel G, Selbmann HK, Jensen U, Forst H, Lenhardt FP, Peter K (1987) Prevention of colonization and respiratory infections in long-term ventilated patients by local antimicrobial prophylaxis. Intensive Care Med 13:106–113
Heeg K, Bigos K, Konrad F, Wiedeck H, Wagner H (1988) Colonization and resistance patterns of microbial isolates following SDD in association with short-course Cefotaxime. In: Vincent JL (ed) Infection control by selective decontamination. Springer, Berlin Heidelberg New York Tokyo, pp 158
Sidow M, Burchardi H, Crozier TA, Ruchel R, Busse C, Seyde WC (1990) The effect of selective decontamination on nosocomial infections, their causative agents and antibiotic resistance in long-term intubated intensive care patients. Anasth Intensivther Notfallmed 25:416–423
Tetteroo GW, Wagenvoort JH, Ince C, Bruining HA (1990) Effects of selective decontamination on Gram-negative colonization, infections and development of bacterial resistance in esophageal resection. Intensive Care Med 16 [Suppl 3]:S224-S228
Godard J, Gillaume C, Reverdy M-E, Bachmann P, Bui-Xuan B, Nageotte A, Motin J (1990) Intestinal decontamination in a polyvalent ICU. A double-blind study. Intensive Care Med 16:307–311
Eastway A (1988) Emergence of resistance during Selective Decontamination: Glasgow results. In: Vincent JL (ed) Infection control by selective decontamination. Springer, Berlin Heidelberg New York Tokyo, pp 154
Botha P, de Kock MJ, van Vuuren CJ, Fourie S, van Heerden C (1990) Evaluation of clinical isolates ofPseudomonas aeruginosa for ribosomal resistance to Tobramycin. S Afr Med J 78:258–259
Sciarra M, Cavaliere F, Crociani E (1988) Tobramycin levels during selective decontamination of the digestive tract (Abstract). Intensive Care Med 14 [Suppl 1]:S311
Stoutenbeek CP, van Saane HKF, Zandstra DF (1987) The effect of oral non-absorbable antibiotics on the emergence of resistant bacteria in patients in an intensive care unit. J Antimicrob Chemother 19:513–520
Ramsay G, Reidy JJ (1990) Selective decontamination in intensive care practice: a review of clinical experience. Intensive Care Med 16 [Suppl 3]:S217–223
Christensen GD, Bisno AL, Parisi JJ (1982) Nosocomial septicemia due to multiply antibiotic resistantStaphylococcus epidermidis. Ann Intern Med 96:1–6
Author information
Authors and Affiliations
Additional information
This work was founded by the Epidemiological Research Program of the Regional Government of the Region Friuli Venezia Giulia
Rights and permissions
About this article
Cite this article
Nardi, G., Valentinis, U., Proietti, A. et al. Epidemiological impact of prolonged systematic use of topical SDD on bacterial colonization of the tracheobronchial tree and antibiotic resistance. Intensive Care Med 19, 273–278 (1993). https://doi.org/10.1007/BF01690547
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF01690547