Summary
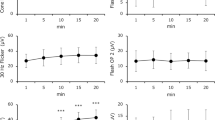
The pupillary response to light was examined by infrared television-videopupillography in 93 Type 1 (insulin-dependent) diabetic patients (aged 25–42 years, duration of diabetes 0–32 years), and 37 control subjects (aged 26–41 years) with techniques ensuring equality of stimulus and retinal sensitivity, and allowing a detailed computerized calculation of the various parameters of the response. There was no difference in latency time or constriction time between diabetic patients and control subjects. The diabetic patients had a smaller initial pupil size (p=0.012) and a smaller response amplitude (p<0.001) than the control subjects, and these two parameters were correlated to each other (r=0.49, p<0.000001) and inversely correlated to the duration of diabetes (r=−0.26, p=0.013 and r=−0.29, p=0.0051, respectively). As a group, the diabetic patients had a relative response amplitude that was similar to that of the control subjects. However, more detailed analysis showed that the diabetic patients with pupil size in the normal range had a small, but significant, reduction in relative response amplitude (p=0.0021). The maximal velocities of constriction and re-dilatation were reduced in the diabetic patients (p<0.001 in either case), but both parameters were intimately correlated to the response amplitude (r=0.91, p<0.000001, and r=0.79, p<0.000001, respectively), and this relationship was identical in the control subjects. Analysis of velocity-size plot for long-term diabetic patients showed no systematic deviation from that of non-diabetic subjects, indicating unaltered dynamic properties of the small pupil within the altered dynamic range in diabetic patients. The foremost change in the pupils of long-term diabetic patients is a reduction in size. Since normal iris dynamics are preserved, the small pupil must be due to loss of sympathetic tone. When diabetic patients with a normal or near-normal sensory pathway are stimulated by light, they have a normal latency time and response parameters that are normal for the size of their pupil. The only exception seems to be a minor reduction in response amplitude, possibly indicating damage to the efferent, parasympathetic pathways, as is known to develop in other organs.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Pryce TD (1887) Perforating ulcers of both feet associated with diabetes and ataxic symptoms. Lancet 2: 11–12
Pitres MA (1902) Note sur l'état des réflexes cutanés et pupillaires er des sensibilités testiculaire et épigastrique profondes chez les diabetiques. CR Soc Biol 4: 1286–1287
Major RH (1924) Tabes diabetica. JAMA 83: 2004
Waite JH, Beetham WP (1935) The visual mechanism in diabetes mellitus. A comparative study of 2002 diabetics, and 457 non-diabetics for control. N Engl J Med 212: 367–379
Jordan WR (1936) Neuritic manifestations in diabetes mellitus. Arch Intern Med 57: 307–366
Rundles RW (1945) Diabetic neuropathy. General review with report of 125 cases. Medicine 24: 111–160
Martin MM (1953) Diabetic neuropathy. A clinical study of 150 cases. Brain 76: 594–624
Ohrt V (1967) Diabetic iridopathy. Thesis. Universitetsforlaget, Aarhus
Friedman SA, Feinberg R, Podolak E, Bedell RHS (1967) Pupillary abnormalities in diabetic neuropathy. A preliminary study. Ann Intern Med 67: 977–983
Gliem H (1971) Pupillomotorische Veränderungen bei Diabetikern. Acta Ophthalmol (Kbh) 49: 955–963
Hreidarsson ÁB (1982) Pupil size in insulin-dependent diabetes, relationship to duration, metabolic control, and long-term manifestations. Diabetes 31: 442–448
Gundersen HJG (1976) Nervous and muscular dynamics of the pupil in long-term diabetics. In: Bajaj JS (ed) Current topics in diabetes research. IX Congress of the International Diabetes Federation. Excerpta Medica, Amsterdam, p 131–132
Steiness I (1957) Vibratory perception in diabetics. Acta Med Scand 158: 327–335
Gundersen HJG (1976) A new photostimulator and videopupillograph for quantitative neuroophthalmological studies. Ophthalmologica 172: 62–68
Stark L (1968) Neurological control systems. Studies in bioengineering. Plenum, New York
Gundersen HJG (1974) An abnormality of the central autonomic nervous system in long-term diabetes: absence of hippus. Diabetologia 10: 366 (Abstract)
Smith SE, Smith SA, Brown PM, Fox C, Sönksen PH (1978) Pupillary signs in diabetic autonomic neuropathy. Br Med J 4: 924–927
Pfeifer MA, Cook D, Brodsky J, Tice D, Parrish D, Reenan A, Halter JB, Porte Jr D (1982) Quantitative evaluation of sympathetic and parasympathetic control of iris function. Diabetes Care 5: 518–528
Hreidarsson ÁB (1979) Pupil motility in long-term diabetes. Diabetologia 17: 145–150
Smith SA, Smith SE (1983) Reduced pupillary light reflexes in diabetic autonomic neuropathy. Diabetologia 24: 330–332
Gartner S, Henkind P (1978) Neovascularization of the iris (Rubeosis Iridis). Surv Ophthalmol 22: 291–312
Semmlow J, Stark L (1973) Pupil movements to light and accommodative stimulation: a comparative study. Vision Res 13: 1087–1100
Lundbæk K (1953) Long-term diabetes. The clinical picture in diabetes mellitus after 15–25 years duration, with a follow-up of a regional series of cases. (The ophthalmological section in collaboration with VA Jensen). Munksgaard, Copenhagen
Hreidarsson ÁB (1981) Acute, reversible autonomic nervous system abnormalities in juvenile insulin-dependent diabetes. Diabetologia 20: 475–481
Hayashi M, Ishikawa S (1979) Pharmacology of pupillary responses in diabetics — correlative study of the responses and grade of retinopathy. Jap J Ophthalmol 23: 65–72
Smith SA, Smith SE (1983) Evidence for a neuropathic aetiology in the small pupil of diabetes mellitus. Br J Ophthalmol 67: 89–93
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Hreidarsson, Á.B., Gundersen, H.J.G. The pupillary response to light in Type 1 (insulin-dependent) diabetes. Diabetologia 28, 815–821 (1985). https://doi.org/10.1007/BF00291070
Received:
Revised:
Issue Date:
DOI: https://doi.org/10.1007/BF00291070