Summary
Since the magnitude of the response to a drug may depend upon the drug input rate, the concentration-effect relationship of the new dihydropyridine (±)-isradipine was investigated using different administration modalities.
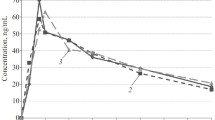
Ten normotensive healthy volunteers were given, double-blind and in a crossover fashion, isradipine as a 1 mg iv infusion, 5 mg oral solution, 5 mg standard tablet, 10 mg slow release formulation, and a placebo. Blood pressure, heart rate, and plasma isradipine concentrations were recorded for 24 h.
The maximal fall in diastolic blood pressure was similar after the infusion (-11.40 mmHg), the oral solution (-15.20 mmHg), and the standard tablet (-12.50 mmHg). In healthy volunteers the slow release form had no significant effect on blood pressure. The concentration-effect plots showed an increasing slope in the order infusion, solution, and tablet, and anticlockwise hysteresis. This was partly due to marked heart rate counter-regulation, the corresponding mean maximal heart rate increases being 24, 19, and 17 beats·min−1.
The pronounced counter-regulation of the heart rate implies that a slow isradipine input rate would be more effective in decreasing blood pressure.
Similar content being viewed by others
References
Staessen J, Lijnen P, Fagard R et al. (1989) Effects of the new calcium entry blockers isradipine (PN 200–110) in essential hypertension. J Cardiovasc Pharmacol 13: 271–276
Nelson EB, Pool JL, Taylor AA (1986) Antihypertensive activity of isradipine in humans: a new dihydropyridine calcium channel antagonist. Clin Pharmacol Ther 40: 694–697
Fitton A, Benfield P (1990) Isradipine. A review of its pharmacodynamic and pharmacokinetic properties and therapeutic use in cardiovascular disease. Drugs 40: 31–74
Rüegg UT, Hof RP (1990) Pharmacology of the calcium antagonist isradipine. Drugs 40 [Suppl 2]: 3–9
Kleinbloesem CH, van Brummelen P, Danhof M et al. (1986) Rate of increase in the plasma concentration of nifedipine as a major determinant of its hemodynamic effects in human. Clin Pharmacol Ther 41: 126–130
Sheiner LB, Beal SL, Sambol NC (1989) Study designs for dose-ranging. Clin Pharmacol Ther 46: 63–77
Goodman and Gilman's (1980) The pharmacological basis of therapeutics, 6th ed MacMillan, New York
Harris E, Lpool MB, Turner R (1954) 1-hydrazinophthalazine (Apresolin) in hypertension. Lancet I: 429–433
Soons PA, De Boer AG, Van Brummelen P et al. (1989) Oral absorption profile of nitrendipine in healthy subjects: a kinetic and dynamic study. Br J Clin Pharmacol 27: 179–189
Van Harten J, Van Brummelen P, Zeegers R et al. (1988) The influence of infusion rate on the pharmacokinetics and haemodynamic effects of nisoldipine in man. Br J Clin Pharmacol 25: 709–717
Abetel G, Haissly JC, Brunori A (1989) Evaluation d'un nouvel appareil tensionnel ambulatoire, le Sandoz Pressure System. Schweiz Med Wschr 119: 1786–1790
Clifton GD, Blouin RA, Dilea CS et al. (1988) The pharmacokinetics of oral isradipine in normal volunteers. J Clin Pharmacol 28: 36–42
SAS Institute (1982) SAS Users Guide: Statistics. Cary, NC, USA
Kiowski W, Bertel O, Erne P et al. (1983) Haemodynamic and reflex responses to acute and chronic antihypertensive therapy with the calcium entry blocker nifedipine. Hypertension 5 [Suppl I]: 170–174
Dorward PK, Andresen MC, Burke SL et al. (1982) Rapid resetting of the aortic baroreceptors in the rabbit and its implications for short-term and longer term reflex control. Circ Res 50: 428–329
Holford NHG, Sheiner LB (1981) Understanding the dose-effect relationship: clinical application of pharmacokinetic-pharmacodynamic models. Clin Pharmacokinet 6: 439–453
Sumner DJ, Meredith PA, Howie CA et al. (1988) Initial blood pressure as a predictor of the response to antihypertensive therapy. Br J Clin Pharmacol 26: 715–720
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Carrara, V., Porchet, H. & Dayer, P. Influence of input rates on (±)-isradipine haemodynamics and concentration-effect relationship in healthy volunteers. Eur J Clin Pharmacol 46, 29–33 (1994). https://doi.org/10.1007/BF00195912
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF00195912