Abstract
Objective: To determine how physicians weigh iatrogenic complications when making clinical decisions.
Design: Physicians were mailed a questionnaire describing two simplified scenarios—one involving a patient with a cerebral embolism and the other involving a patient with a life-threatening arrhythmia. In each scenario there was one potential natural adverse outcome (which could be prevented with drug therapy) and one potential drug side effect (iatrogenic adverse outcome), which would be clinically indistinguishable from the natural adverse outcome. Half the respondents were given the probability of the natural adverse outcome (PN) and were asked to specify the probability of the iatrogenic adverse outcome (P1) at which they felt that giving and withholding the therapy were equivalent strategies. The other respondents were given the P, and asked to specify the PN at which they felt the two strategies were equivalent.
Setting: Academic medical center.
Participants: Staff physicians.
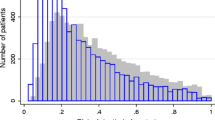
Measurements and main results: Results are expressed as the ratio P1/PN at which the respondent felt that giving and not giving therapy were equivalent strategies. A ratio less than 1 indicates that errors of commission (iatrogenic adverse outcomes) were given more weight than were errors of omission (natural adverse outcomes when therapy was withheld). Ratios less than 1 were provided in 56% of the responses (n=230). The mean P1/PN in the group with ratios less than 1 was 0.53±0.26 (SD;n=129).
Conclusions: In making decisions, some physicians appear to weigh errors of commission more heavily than they do errors of omission, while others weigh them equally. This diversity of physicians’ attitudes may explain some of the variation observed in clinical practice in settings where the possibility of iatrogenic complications is of concern.
Key words|iatrogenic complications|medical decision making|physicians
Similar content being viewed by others
References
Elstein AS, Holzman GB, Ravitch MM, et al. Comparison of physicians’ decisions regarding estrogen replacement therapy for menopausal women and decisions derived from a decision analytic model. Am J Med 1986;80:246–58.
Farquhar PH. Utility assessment methods. Management Sci. 1984;30:1283–300.
McNeil BJ, Pauker SG, Sox HC, Tversky A. On the elicitation of preferences for alternative therapies. N Engl J Med. 1982;306:1259–62.
Tversky A, Kahneman D. The framing of decisions and the psychology of choice. Science. 1981;211:453–8.
Bell DE. Regret in decision making under uncertainty. Oper Res. 1982;30:961–81.
Feinstein AR. The “chagrin factor” and qualitative decision analysis. Arch Intern Med. 1985;145:1257–9.
Spranca M, Minsk E, Baron J. Omission and commission in judgment and choice. J Exp Soc Psychol. 1991;27:76–105.
Hershey JC, Baron J. Clinical reasoning and cognitive processes. Med Decis Making. 1987;7:203–11.
Author information
Authors and Affiliations
Additional information
Received from the Division of Clinical Decision Making, Department of Medicine, New England Medical Center, Tufts University School of Medicine, Boston, Massachusetts.
Supported in part by Grants TG LM-7044 and LM-4493 from the National Library of Medicine, Bethesda, Maryland.
Rights and permissions
About this article
Cite this article
Cohen, B.J., Pauker, S.G. How do physicians weigh iatrogenic complications?. J Gen Intern Med 9, 20–23 (1994). https://doi.org/10.1007/BF02599137
Issue Date:
DOI: https://doi.org/10.1007/BF02599137