Abstract
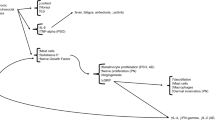
Rosacea is a common cutaneous disorder that has diverse clinical manifestations ranging from facial vascular hyperreactivity to sebaceous gland hyperplasia. It has been postulated that neurovascular interactions with release of proinflammatory and vasodilatory neuropeptides could be intergral to the pathogenesis of certain subtypes of this disorder. Stress, ultra-violet light or microbial antigens may stimulate release of these neurotransmitters and contribute to the flushing and erythema seen in some patients with rosacea. Study of the neurovascular interactive network in rosacea has provided understanding and insights in to the vascular reactivity which is a feature of the clinical disorder in some patients with rosacea.
Access this chapter
Tax calculation will be finalised at checkout
Purchases are for personal use only
Similar content being viewed by others
References
Marks R. Concepts in the pathogenesis of rosacea. Br J Dermatol. 1968;80:170–7.
Powell FC. Rosacea. N Eng J Med. 2005;352:793–803.
Wilkin JK. Rosacea: pathophysiology and treatment. Arch Dermatol. 1994;130:359–62.
Lonne-Rahn S, Nordlind K, Wiegleb Edstrõm D, Ros AM, Berg M. Laser treatment of rosacea. A pathoetiological study. Arch Dermatol. 2004;140:1345–9.
Griesemer R. Emotionally triggered disease in dermatological practice. Psychiar Ann. 1978;8:49–56.
Puchalski Z. Psychosomatic aspects in patients with alopecia areata, rosacea, and lichen rubber planus. Z Hautkr. 1983;58:1648–54.
Steinhoff M, Stander S, Seeliger S, Ansel JC, Schmelz M, Luger T. Modern aspects of cutaneous neurogenic inflammation. Arch Dermatol. 2003;139:1479–88.
Legat FJ, Armstrong CA, Ansel JC. The cutaneous neurosensory system in skin disease. Adv Dermatol. 2002;18:91–109.
Roosterman D, Goerge T, Schneider SW, Bunnett NW, Steinhoff M. Neuronal control of skin function: the skin as a neuroimmunoendocrine organ. Physiol Rev. 2006;86:1309–79.
Peters EMJ, Ericson ME, Hosoi J, Seiffert K, Hordinsky MK, Ansel JC, Paus R, Scholzen TE. Neuropeptide control mecahisms in cutaneous biology: physiological and clinical significance. J Invest Dermatol. 2006;126:1937–47.
Powell FC, Corbally N, Powell D. Substance P and rosacea. J Am Acad Dermatol. 1993;28(1):132–3.
Kϋrkçϋoğlu N, Alaybeyi F. Substance P immunoreactivity in rosacea. J Am Acad Dermatol. 1991;25:725–6.
Wollina U. Rhinophyma – unusual expression of simple-type keratins and S100A in sebocytes and abundance of VIP receptor-positive dermal cells. Histol Histopathol. 1996;11:111–5.
Piérard-Franchimont C, Quatresooz P, Piérard GE. Incidental control of rosacea by somatostatin. Dermatology. 2003;206:249–51.
Murphy A, Buchanan KD, Powell FC. Vasoactive intestinal peptide release is not a factor in roscaea. Br J Dermatol. 1997;137 Suppl 50:27.
Fimmel S, Glass E, Zouboulis CC. Neuropeptides and UV radiation are possible mediators of inflammation in rosacea. J Invest Dermatol. 2005;124(suppl):A16.
Zegaraska B, Lelińska A, Tyrakowski T. Clinical and experimental aspects of cutaneous neurogenic inflammation. Pharmacol Rep. 2006;58:13–21.
Lonne-Rahm S, Fischer T, Berg M. Stinging and rosacea. Acta Derm Venereol. 1999;79:460–1.
Scholzen T, Armstrong CA, Bunnett NW, Leger TA, Olerud JE, Ansel JC. Neuropeptides in the skin: interactions between the neuroendocrine and the skin immune systems. Exp Dermatol. 1998;7:81–96.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2014 Springer-Verlag Berlin Heidelberg
About this chapter
Cite this chapter
McAleer, M.A., Powell, F.C. (2014). Rosacea and Neuropeptides. In: Zouboulis, C., Katsambas, A., Kligman, A. (eds) Pathogenesis and Treatment of Acne and Rosacea. Springer, Berlin, Heidelberg. https://doi.org/10.1007/978-3-540-69375-8_82
Download citation
DOI: https://doi.org/10.1007/978-3-540-69375-8_82
Publisher Name: Springer, Berlin, Heidelberg
Print ISBN: 978-3-540-69374-1
Online ISBN: 978-3-540-69375-8
eBook Packages: MedicineMedicine (R0)