Abstract
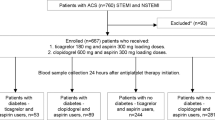
Switching P2Y12 inhibitors is common in clinical practice. However, data on the pharmacodynamic (PD) effects of switching in clinical settings characterized by high platelet reactivity, such as diabetes mellitus (DM), are limited. This is a post-hoc analysis from a prospective, randomized, open-label study conducted in coronary artery disease patients comparing the PD effects of loading dose (LD) and maintenance dose regimens of prasugrel vs ticagrelor according to DM status. A total of 110 patients were enrolled: 42 (38%) with DM and 68 (62%) without DM. All patients were on maintenance dual antiplatelet therapy with aspirin and clopidogrel. PD assessments were performed using whole blood vasodilator-stimulated phosphoprotein (VASP), with results quantified by the platelet reactivity index (PRI), VerifyNow P2Y12 (VN-P2Y12) with results reported as P2Y12 reaction units (PRU), and light transmittance aggregometry (LTA) following 20 and 5 µM adenosine diphosphate stimuli with results reported as maximum platelet aggregation (MPA). PD assessments were performed at baseline (while on clopidogrel), 30 min after LD, 2 h after LD, and 1 week after LD. Overall, platelet reactivity was higher in DM than in non-DM patients while on clopidogrel therapy. After switching to either prasugrel or ticagrelor, platelet reactivity dropped but remained significantly higher among patients with DM at 30 min with all tests (VN-PRU p < 0.01, MPA 20 µM p < 0.01, VASP-PRI p = 0.02) and at 2 h with VN-PRU (p < 0.01) and LTA-MPA 20 µM (p < 0.01) but not with VASP-PRI (p = 0.19). There were no significant differences between prasugrel and ticagrelor both among patients with or without DM, except for lower LTA-MPA 20 at 30 min (p < 0.01) among non-DM patients treated with prasugrel. Patients with DM treated with clopidogrel have higher platelet reactivity compared to patients without DM. Although platelet reactivity markedly reduces to a similar extent after switching to prasugrel or ticagrelor, patients with DM persist with increased platelet reactivity compared to patients without DM.
Study registration: ClinicalTrials.gov identifier: NCT01852175






Similar content being viewed by others
References
Capodanno D, Angiolillo DJ (2020) Antithrombotic therapy for atherosclerotic cardiovascular disease risk mitigation in patients with coronary artery disease and diabetes mellitus. Circulation 142(22):2172–2188
Patti G, Cavallari I, Andreotti F, Calabrò P, Cirillo P, Denas G et al (2019) Prevention of atherothrombotic events in patients with diabetes mellitus: from antithrombotic therapies to new-generation glucose-lowering drugs. Nat Rev Cardiol 16(2):113–130
Rollini F, Franchi F, Muñiz-Lozano A, Angiolillo DJ (2013) Platelet function profiles in patients with diabetes mellitus. J Cardiovasc Transl Res 6(3):329–345
Franchi F, Rollini F, Aggarwal N, Hu J, Kureti M, Durairaj A et al (2016) Pharmacodynamic comparison of prasugrel versus ticagrelor in patients with type 2 diabetes mellitus and coronary artery disease: the OPTIMUS (optimizing antiplatelet therapy in diabetes mellitus)-4 study. Circulation 134(11):780–792
Angiolillo DJ, Jakubowski JA, Ferreiro JL, Tello-Montoliu A, Rollini F, Franchi F et al (2014) Impaired responsiveness to the platelet P2Y12 receptor antagonist clopidogrel in patients with type 2 diabetes and coronary artery disease. J Am Coll Cardiol 64(10):1005–1014
Ferreiro JL, Angiolillo DJ (2011) Diabetes and antiplatelet therapy in acute coronary syndrome. Circulation 123(7):798–813
Zhang R, Mamza JB, Morris T, Godfrey G, Asselbergs FW, Denaxas S et al (2022) Lifetime risk of cardiovascular-renal disease in type 2 diabetes: a population-based study in 473,399 individuals. BMC Med 20(1):63
Angiolillo DJ, Galli M, Collet JP, Kastrati A, O’Donghue M (2022) Antiplatelet therapy after percutaneous coronary intervention. EuroIntervention 17(17):e1371–e1396
Aradi D, Kirtane A, Bonello L, Gurbel PA, Tantry US, Huber K et al (2015) Bleeding and stent thrombosis on P2Y12-inhibitors: collaborative analysis on the role of platelet reactivity for risk stratification after percutaneous coronary intervention. Eur Heart J 36(27):1762–1771
Sibbing D, Aradi D, Alexopoulos D, Ten Berg J, Bhatt DL, Bonello L et al (2019) Updated expert consensus statement on platelet function and genetic testing for guiding P2Y(12) receptor inhibitor treatment in percutaneous coronary intervention. JACC Cardiovasc Interv 12(16):1521–1537
Angiolillo DJ, Bernardo E, Sabaté M, Jimenez-Quevedo P, Costa MA, Palazuelos J et al (2007) Impact of platelet reactivity on cardiovascular outcomes in patients with type 2 diabetes mellitus and coronary artery disease. J Am Coll Cardiol 50(16):1541–1547
Angiolillo DJ, Fernandez-Ortiz A, Bernardo E, Ramírez C, Sabaté M, Jimenez-Quevedo P et al (2006) Clopidogrel withdrawal is associated with proinflammatory and prothrombotic effects in patients with diabetes and coronary artery disease. Diabetes 55(3):780–784
Navarese EP, Khan SU, Kołodziejczak M, Kubica J, Buccheri S, Cannon CP et al (2020) Comparative efficacy and safety of oral P2Y(12) inhibitors in acute coronary syndrome: network meta-analysis of 52 816 patients from 12 randomized trials. Circulation 142(2):150–160
Rollini F, Franchi F, Cho JR, DeGroat C, Bhatti M, Muniz-Lozano A et al (2016) A head-to-head pharmacodynamic comparison of prasugrel vs ticagrelor after switching from clopidogrel in patients with coronary artery disease results of a prospective randomized study. Eur Heart J 37(35):2722–2730
Galli M, Benenati S, Franchi F, Rollini F, Capodanno D, Biondi-Zoccai G et al (2022) Comparative effects of guided vs potent P2Y12 inhibitor therapy in acute coronary syndrome: a network meta-analysis of 61 898 patients from 15 randomized trials. Eur Heart J 43(10):959–967
Franchi F, Angiolillo DJ (2015) Novel antiplatelet agents in acute coronary syndrome. Nat Rev Cardiol 12(1):30–47
Ndrepepa G, Kastrati A, Menichelli M, Neumann FJ, Wöhrle J, Bernlochner I et al (2020) Ticagrelor or prasugrel in patients with acute coronary syndromes and diabetes mellitus. JACC Cardiovasc Interv 13(19):2238–2247
Schüpke S, Neumann FJ, Menichelli M, Mayer K, Bernlochner I, Wöhrle J et al (2019) Ticagrelor or prasugrel in patients with acute coronary syndromes. N Engl J Med 381(16):1524–1534
Steg PG, Bhatt DL, Simon T, Fox K, Mehta SR, Harrington RA et al (2019) Ticagrelor in patients with stable coronary disease and diabetes. N Engl J Med 381(14):1309–1320
Collet JP, Thiele H, Barbato E, Barthélémy O, Bauersachs J, Bhatt DL et al (2021) 2020 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J 42(14):1289–1367
Angiolillo DJ, Rollini F, Storey RF, Bhatt DL, James S, Schneider DJ et al (2017) International expert consensus on switching platelet P2Y(12) receptor-inhibiting therapies. Circulation 136(20):1955–1975
Virani SS, Alonso A, Benjamin EJ, Bittencourt MS, Callaway CW, Carson AP et al (2020) Heart disease and stroke statistics-2020 update: a report from the American Heart Association. Circulation 141(9):e139–e596
Erlinge D, Varenhorst C, Braun OO, James S, Winters KJ, Jakubowski JA et al (2008) Patients with poor responsiveness to thienopyridine treatment or with diabetes have lower levels of circulating active metabolite, but their platelets respond normally to active metabolite added ex vivo. J Am Coll Cardiol 52(24):1968–1977
Franchi F, James SK, Ghukasyan Lakic T, Budaj AJ, Cornel JH, Katus HA et al (2019) Impact of diabetes mellitus and chronic kidney disease on cardiovascular outcomes and platelet P2Y(12) receptor antagonist effects in patients with acute coronary syndromes: insights from the PLATO trial. J Am Heart Assoc 8(6):e011139
Wiviott SD, Braunwald E, Angiolillo DJ, Meisel S, Dalby AJ, Verheugt FW et al (2008) Greater clinical benefit of more intensive oral antiplatelet therapy with prasugrel in patients with diabetes mellitus in the trial to assess improvement in therapeutic outcomes by optimizing platelet inhibition with prasugrel-thrombolysis in myocardial infarction 38. Circulation 118(16):1626–1636
Bhatt DL, Bonaca MP, Bansilal S, Angiolillo DJ, Cohen M, Storey RF et al (2016) Reduction in ischemic events with ticagrelor in diabetic patients with prior myocardial infarction in PEGASUS-TIMI 54. J Am Coll Cardiol 67(23):2732–2740
Meredith IT, Tanguay JF, Kereiakes DJ, Cutlip DE, Yeh RW, Garratt KN et al (2016) Diabetes mellitus and prevention of late myocardial infarction after coronary stenting in the randomized dual antiplatelet therapy study. Circulation 133(18):1772–1782
Steg PG, Bhatt DL, Simon T, Fox K, Mehta SR, Harrington RA et al (2019) Ticagrelor in patients with stable coronary disease and diabetes. New Engl J Med 381(14):1309–1320
Angiolillo DJ, Capodanno D, Danchin N, Simon T, Bergmeijer TO, Ten Berg JM et al (2020) Derivation, validation, and prognostic utility of a prediction rule for nonresponse to clopidogrel: the ABCD-GENE score. JACC Cardiovasc Interv 13(5):606–617
Bhatt DL, Stone GW, Mahaffey KW, Gibson CM, Steg PG, Hamm CW et al (2013) Effect of platelet inhibition with cangrelor during PCI on ischemic events. N Engl J Med 368(14):1303–1313
Cosentino F, Bhatt DL, Marx N, Verma S (2022) The year in cardiovascular medicine 2021: diabetes and metabolic disorders. Eur Heart J 43(4):263–270
Galli M, Benenati S, Capodanno D, Franchi F, Rollini F, D’Amario D et al (2021) Guided versus standard antiplatelet therapy in patients undergoing percutaneous coronary intervention: a systematic review and meta-analysis. Lancet 397(10283):1470–1483
Galli M, Franchi F, Rollini F, Angiolillo DJ (2021) Role of platelet function and genetic testing in patients undergoing percutaneous coronary intervention. Trends Cardiovasc Med S1050–1738(21):00157–00162
Ferreiro JL, Ueno M, Tello-Montoliu A, Tomasello SD, Capodanno D, Capranzano P et al (2013) Effects of cangrelor in coronary artery disease patients with and without diabetes mellitus: an in vitro pharmacodynamic investigation. J Thromb Thrombolysis 35(2):155–164
Acknowledgements
The present study was funded by Institutional Grant of the University of Florida College of Medicine-Jacksonville.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M.G. declares that he has received honoraria from Terumo. F.F. declares that he has received payment as an individual for consulting fee or honorarium from AstraZeneca, Bayer and Sanofi. Institutional payments for grants from PLx Pharma, and The Scott R. MacKenzie Foundation. F.R. declares that he has received honoraria from Chiesi. D.J.A. declares that he has received consulting fees or honoraria from Abbott, Amgen, AstraZeneca, Bayer, Biosensors, Boehringer Ingelheim, Bristol-Myers Squibb, Chiesi, Daiichi-Sankyo, Eli Lilly, Haemonetics, Janssen, Merck, PhaseBio, PLx Pharma, Pfizer, and Sanofi,. D.J.A. also declares that his institution has received research grants from Amgen, AstraZeneca, Bayer, Biosensors, CeloNova, CSL Behring, Daiichi-Sankyo, Eisai, Eli Lilly, Gilead, Janssen, Matsutani Chemical Industry Co., Merck, Novartis, Osprey Medical, Renal Guard Solutions and Scott R. MacKenzie Foundation. The remaining authors report no disclosures.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Galli, M., Rollini, F., Been, L. et al. Impact of diabetes mellitus on the pharmacodynamic effects of prasugrel and ticagrelor after switching from clopidogrel in patients with coronary artery disease. J Thromb Thrombolysis 54, 461–469 (2022). https://doi.org/10.1007/s11239-022-02696-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-022-02696-4