Abstract
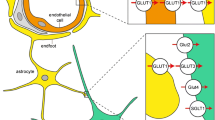
Blood-borne substances can invade into the extracellular spaces of the brain via endothelial cells in sites without the blood–brain barrier (BBB), and can travel through the interstitial fluid (ISF) of the brain parenchyma adjacent to non-BBB sites. It has been shown that cerebrospinal fluid (CSF) drains directly into the blood via the arachnoid villi and also into lymph nodes via the subarachnoid spaces of the brain, while ISF drains into the cervical lymph nodes through perivascular drainage pathways. In addition, the glymphatic pathway of fluids, characterized by para-arterial pathways, aquaporin4-dependent passage through astroglial cytoplasm, interstitial spaces, and paravenous routes, has been established. Meningeal lymphatic vessels along the superior sagittal sinus were very recently discovered. It is known that, in mice, blood-borne substances can be transferred to areas with intact BBB function, such as the medial regions of the hippocampus, presumably through leaky vessels in non-BBB sites. In the present paper, we review the clearance mechanisms of interstitial substances, such as amyloid-β peptides, as well as summarize models of BBB deterioration in response to different types of insults, including acute ischemia followed by reperfusion, hypertension, and chronic hypoperfusion. Lastly, we discuss the relationship between perivascular clearance and brain disorders.


Similar content being viewed by others
Abbreviations
- ABC:
-
ATP-binding cassette
- Aβ:
-
Amyloid-β
- AD:
-
Alzheimer’s disease
- BBB:
-
Blood–brain barrier
- BCSFB:
-
Blood–cerebrospinal fluid barrier
- CAA:
-
Cerebral amyloid angiopathy
- CSF:
-
Cerebrospinal fluid
- FPRL1:
-
Formylpeptide receptor-like-1
- IDE:
-
Insulin-degrading enzyme
- ISF:
-
Interstitial fluid
- LDLR:
-
Low-density-lipoprotein receptor
- LRP:
-
LDLR-related protein
- MRI:
-
Magnetic resonance imaging
- NMO:
-
Neuromyelitis optica
- P-gp:
-
P-glycoprotein
- RAGE:
-
Receptor for advanced glycation end product
References
Reese TS, Karnovsky MJ (1967) Fine structural localization of a blood-brain barrier to exogenous peroxidase. J Cell Biol 34:207–217
Brightman MW, Reese TS (1969) Junctions between intimately apposed cell membranes in the vertebrate brain. J Cell Biol 40:648–677
Davson H, Welch K, Segal MB (1987) Morphological aspects of the barriers. In: Davson H, Welch K, Segal MB (eds) Physiology and pathophysiology of the cerebrospinal fluid. Churchill Livingstone, Edinburgh, pp 105–188
Brightman MW, Klatzo I, Olsson Y, Reese TS (1970) The blood-brain barrier to proteins under normal pathological conditions. J Neurol Sci 10:215–239
Broadwell RD, Sofroniew MV (1993) Serum proteins bypass the blood-brain fluid barriers for extracellular entry to the central nervous system. Exp Neurol 120:245–263
Ueno M, Akiguchi I, Hosokawa M, Yagi H, Takemura M, Kimura J, Takeda T (1994) Accumulation of blood-borne horseradish peroxidase in medial portions of the mouse hippocampus. Acta Neurol Scand 90:400–404
Ueno M, Akiguchi I, Hosokawa M, Kotani H, Kanenishi K, Sakamoto H (2000) Blood-brain barrier permeability in the periventricular areas of the normal mouse brain. Acta Neuropathol 99:385–392
Ueno M, Akiguchi I, Hosokawa M, Kotani H, Kanenishi K, Sakamoto H (1999) The passage of blood-borne horseradish peroxidase into the amygdaloid area of the mouse brain. Histochem Cell Biol 11:265–270
Bradbury MW, Cserr HF, Westrop RJ (1981) Drainage of cerebral interstitial fluid into deep cervical lymph of the rabbit. Am J Physiol 240:F329–F336
Carare RO, Bernardes-Silva M, Newman TA, Page AM, Nicoll JAR, Perry VH, Weller RO (2008) Solutes, but not cells, drain from the brain parenchyma along basement membranes of capillaries and arteries. Significance for cerebral amyloid angiopathy and neuroimmunology. Neuropathol Appl Neurobiol 34:131–144
Weller RO, Djuanda E, Yow H-Y, Carare RO (2009) Lymphatic drainage of the brain and the pathophysiology of neurological disease. Acta Neuropathol 117:1–14
Carare RO, Hawkes CA, Jeffrey M, Kalaria RN, Weller RO (2013) Cerebral amyloid angiopathy, prion angiopathy, CADASIL and spectrum of protein elimination failure angiopathies (PEFA) in neurodegenerative disease with a focus on therapy. Neuropathol Appl Neurobiol 39:593–611
Iliff JJ, Wang M, Liao Y, Plogg BA, Peng W, Gundersen GA, Benveniste H, Vates GE, Deane R, Goldman SA, Nagelhus EA, Nedergaard M (2012) A paravascular pathway facilitates CSF flow through the brain parenchyma and the clearance of interstitial solutes, including amyloid β. Sci Transl Med 4:147ra111. doi:10.1126/scitranslmed.3003748
Louveau A, Smirnov I, Keyes TJ, Eccles JD, Sj Rouhani, Peske JD, Derecki NC, Castle D, Mandell JW, Lee KS, Harris TH, Kipnis J (2015) Structural and functional features of central nervous system lymphatic vessels. Nature 523:337–341
Aspelund A, Antila S, Proulx ST, Karlsen V, Karaman S, Detmar M, Wiig H, Alitalo K (2015) A dural lymphatic vascular system that drains brain interstitial fluid and macromolecules. J Exp Med 212:991–999
Tarasoff-Conway JM, Carare RO, Osorio RS, Glodzik L, Butler T, Fieremans E, Axel L, Rusinek H, Nicholson C, Zlokovic BV, Frangione B, Blennow K, Menard J, Zetterberg H, Wisniewski T, de Leon MJ (2015) Clearance systems in the brain-implications for Alzheimer disease. Nat Rev Neurol 11:457–470
Castellano JM, Deane R, Gottesdiener AJ, Verghese PB, Stewart FR, West T, Paoletti AC, Kasper TR, DeMattos RB, Zlokovic BV (2012) Low-density lipoprotein receptor overexpression enhances the rate of brain-to-blood Aβ clearance in amouse model of & #x03B2;-amyloidosis. Proc Natl Acad Sci USA 109:15502–15507
Shibata M, Yamada S, Kumar SR, Calero M, Bading J, Frangione B, Holtzman DM, Miller CA, Strickland DK, Ghiso J, Zlokovic BV (2000) Clearance of Alzheimer’s amyloid-β1-40 peptide from brain by LDL-receptor-related protein-1 at the blood-brain barrier. J Clin Invest 106:1489–1499
Fujiyoshi M, Tachikawa M, Ohtsuki S, Ito S, Uchida Y, Akanuma S, Kamie J, Hashimoto T, Hosoya K, Iwatsubo T, Terasaki T (2011) Amyloid-β peptide(1-40) elimination from cerebrospinal fluid involves low-density lipoprotein receptor-related protein 1 at the blood-cerebrospinal fluid barrier. J Neurochem 118:407–415
Zlokovic BV, Martel CL, Matsubara E, McComb JG, Zheng G, McCluskey RT, Frangione B, Ghiso J (1996) Glycoprotein 330/megalin: probable role in receptor-mediated transport of apolipoprotein J alone and in a complex with Alzheimer disease amyloid beta at the blood-brain and blood-cerebrospinal fluid barriers. Proc Natl Acad Sci USA 93:4229–4234
Yazawa H, Yu ZX, Takeda K, Le Y, Gong W, Ferrans VJ, Oppenheim JJ, Li CC, Wang JM (2001) Beta Amyloid peptide (Aβ42) is internalized via the G-protein-coupled receptor FPRL1 and forms fibrillary aggregates in macrophages. FASEB J 15:2454–2462
Wahrle SE, Jiang H, Parsadanian M, Legleiter J, Han X, Fryer JD, Kowalewski T, Holtzman DM (2004) ABCA1 is required for normal central nervous system ApoE levels and for lipidation of astrocyte-secreted apoE. J Biol Chem 279:40987–40993
Krohn M, Lange C, Hofrichter J, Scheffler K, Stenzel J, Steffen J, Schumacher T, Bruning T, Plath AS, Alfen F, Schmidt A, Winter F, Rateitschak K, Wree A, Gsponer J, Walker LC, Pahnke J (2011) Cerebral amyloid-β proteostasis is regulated by the membrane transport protein ABCC1 in mice. J Clin Invest 121:3924–3931
Do TM, Noel-Hudson MS, Ribes S, Besengez C, Smirnova M, Cisternino S, Buyse M, Calon F, Chimini G, Chacun H, Schermann JM, Farinotti R, Bourasset F (2012) ABCG2- and ABCG4-mediated efflux of amyloid-β peptide 1-40 at the mouse blood-brain barrier. J Alzheimers Dis 30:155–166
Daood M, Tsai C, Ahdab-Barmada M, Watchko JF (2008) ABC transporter (P-gp/ABCB1, MRP1/ABCC1, BCRP/ABCG2) expression in the developing human CNS. Neuropediatrics 39:211–218
Coraci IS, Husemann J, Berman JW, Hulette C, Dufour JH, Campanella GK, Luster AD, Silverstein SC, El-Khoury JB (2002) CD36, a class B scavenger receptor, is expressed on microglia in Alzheimer’s disease brains and can mediate production of reactive oxygen species in response to beta-amyloid fibrils. Am J Pathol 160:101–112
Behl M, Zhang Y, Zheng W (2009) Involvement of insulin-degrading enzyme in the clearance of beta-amyloid at the blood-CSF barrier: consequences of lead exposure. Cerebrospinal Fluid Res 6:11
Deane R, Du YS, Submamaryan RK, LaRue B, Jovanovic S, Hogg E, Welch D, Manness L, Liu C, Yu J, Zhu H, Ghiso J, Frangione B, Stern A, Stern A, Schmidt AM, Armstrong DL, Arnold B, Liliensiek B, Nawroth P, Hofman F, Kindy M, Stern D, Zlokovic B (2003) RAGE mediates amyloid-beta peptide transport across the blood-brain barrier and accumulation in brain. Nat Med 9:907–913
Matsumoto K, Chiba Y, Fujihara R, Kubo H, Sakamoto H, Ueno M (2015) Immunohistochemical analysis of transporters related to clearance of amyloid-β peptides through blood-cerebrospinal fluid barrier in human brain. Histochem Cell Biol 144:597–611
Chesser AS, Pritchard SM, Johnson GVW (2013) Tau clearance mechanisms and their possible role in the pathogenesis of Alzheimer disease. Front Neurol 4:122
Iliff J, Chen MJ, Plog BA, Zeppenfeld DM, Soltero M, Yang L, Singh I, Deane R, Nedergaard M (2014) Impairment of glymphatic pathway function promotes tau pathology after traumatic brain injury. J Neurosci 34:16180–16193
Zlokovic BV (2008) The blood-brain barrier in health and chronic neurodegenerative disorders. Neuron 57:178–201
Farrall AJ, Wardlaw JM (2009) Blood-brain barrier: ageing and microvascular disease-systematic review and meta-analysis. Neurobiol Aging 30:337–352
Montagne A, Barnes SR, Sweeney MD, Halliday MR, Sagare AP, Zhao Z, Toga AW, Jacobs RE, Liu CY, Amezcua L, Harrington MG, Chui HC, Law M, Zlokovic BV (2015) Blood-brain barrier breakdown in the aging human hippocampus. Neuron 85:296–302
Ueno M, Akiguchi I, Yagi H, Naiki H, Fujibayashi Y, Kimura J, Takeda T (1993) Age-related changes in barrier function in mouse brain. I. Accelerated age-related increase of brain transfer of serum albumin in accelerated senescence prone SAM-P/8 mice with deficits in learning and memory. Arch Gerontol Geriatr 16:233–248
Vorbrodt AW, Dobrogowska DH, Ueno M, Tarnawski M (1995) A quantitative immunocytochemical study of blood-brain barrier to endogenous albumin in cerebral cortex and hippocampus of senescence-accelerated mice (SAM). Folia Histochem Cytobiol 33:229–237
Ueno M, Dobrogowska DH, Vorbrodt AW (1996) Immunocytochemical evaluation of the blood-brain barrier to endogenous albumin in the olfactory bulb and pons of senescence-accelerated mice (SAM). Histochem Cell Biol 105:203–212
Ueno M, Akiguchi I, Hosokawa M, Shinnou M, Sakamoto H, Takemura M, Higuchi K (1997) Age-related changes in the brain transfer of blood-borne horseradish peroxidase in the hippocampus of senescence-accelerated mouse. Acta Neuropathol 93:233–240
Abboud H, Labreuche J, Meseguer E, Lavallee PC, Simon O, Olivot JM, Mazighi M, Dehoux M, Benessiano J, Steg PG, Amarenco P (2007) Ischemia-modified albumin in acute stroke. Cerebrovasc Dis 23:216–220
Gunduz A, Turedi S, Mentese A, Altunayoglu V, Turan I, Karahan SC, Topbas M, Aydin M, Eraydin I, Akcan B (2008) Ischemia-modified albumin levels in cerebrovascular accidents. Am J Emerg Med 26:874–878
Shinnou M, Ueno M, Sakamoto H, Ide M (1998) Blood-brain barrier damage in reperfusion following ischemia in the hippocampus of the Mongolian gerbil brain. Acta Neurol Scand 98:406–411
Tomimoto H, Akiguchi I, Suenaga T, Nishimura M, Wakita H, Nakamura S, Kimura J (1996) Alterations of the blood-brain barrier and glial cells in white-matter lesions in cerebrovascular and Alzheimer’s disease patients. Stroke 27:2069–2074
Hanyu H, Asano T, Tanaka Y, Iwamoto T, Takasaki M, Abe K (2002) Increased blood-brain barrier permeability in white matter lesions of Binswanger’s disease evaluated by contrast-enhanced MRI. Dement Geriatr Cogn Disord 14:1–6
Ueno M, Tomimoto H, Akiguchi I, Wakita H, Sakamoto H (2002) Blood-brain barrier disruption in white matter of chronic cerebral hypoperfusion. J Cereb Blood Flow Metab 22:97–104
Verhaaren BFJ, Vernooij MW, de Boer R, Hofman A, Niessen WJ, van der Lugt A, Ikram MA (2013) High blood pressure and cerebral white matter lesion progression in the general population. Hypertension 61:1354–1359
Vaslievko V, Passos G, Quiring D, Head E, Fisher M, Cribbs DH (2010) Aging and cerebrovascular dysfunction: contribution of hypertension, cerebral amyloid angiopathy, and immunotherapy. Ann NY Acad Sci 1207:58–70
Okamoto K, Aoki K (1963) Development of a strain of spontaneously hypertensive rat. Jpn Circ J 27:282–293
Ueno M, Sakamoto H, Tomimoto H, Akiguchi I, Onodera M, Huang C, Kanenishi K (2004) Blood-brain barrier is impaired in the hippocampus of young adult spontaneously hypertensive rats. Acta Neuropathol 107:532–538
Starr JM, Wardlaw J, Ferguson K, MacLullich A, Deary IJ, Marshall I (2003) Increased blood-brain barrier permeability in type II diabetes demonstrated by gadolinium magnetic resonance imaging. J Neurol Neurosurg Psychiatry 74:70–76
Liao YJ, Ueno M, Nakagawa T, Huang C, Kanenishi K, Onodera M, Sakamoto H (2005) Oxidative damage in cerebral vessels of diabetic db/db mice. Diabetes Metab Res Rev 21:554–559
Hawkins BT, Lundeen TF, Norwood KM, Brooks HL, Egleton RD (2007) Increased blood-brain barrier permeability and altered tight junctions in experimental diabetes in the rat: condition of hyperglycaemia and matrix metalloproteinases. Diabetologia 50:202–211
Mooradian AD, Haas MJ, Batejko O, Hovsepyan M, Feman SS (2005) Statins ameliorate endothelial barrier permeability changes in the cerebral tissue of streptozotocin-induced diabetic rats. Diabetes 54:2977–2982
Iwanaga Y, Ueno M, Ueki M, Huang CL, Tomita S, Okamoto Y, Ogawa T, Ueda N, Maekawa N, Sakamoto H (2008) The expression of osteopontin is increased in vessels with blood-brain barrier impairment. Neuropathol Appl Neurobiol 34:145–154
Ueno M, Wu B, Nishiyama A, Huang C, Hosomi N, Kusaka T, Nakagawa T, Onodera M, Kido M, Sakamoto H (2009) The expression of matrix metalloproteinase-13 is increased in vessels with blood-brain barrier impairment in a stroke-prone hypertensive model. Hypertens Res 32:332–338
Ueno M, Nakagawa T, Nagai Y, Nishi N, Kusaka T, Kanenishi K, Onodera M, Hosomi N, Huang C, Yokomise H, Tomimot H, Sakamoto H (2011) The expression of CD36 in vessels with blood-brain barrier impairment in a stroke-prone hypertensive model. Neuropathol Appl Neurobiol 37:727–737
Fukami S, Watanabe K, Iwata N, Haraoka J, Lu B, Gerard NP, Gerard C, Fraser P, Westaway D, St. George-Hyslop P, Saido TC (2002) A beta-degrading endopeptidase, neprilysin, in mouse brain: synaptic and axonal localization inversely correlating with Abeta pathology. Neurosci Res 43:39–56
Leissring MA, Farris W, Chang AY, Walsh DM, Wu X, Sun X, Frosch MP, Selkoe DJ (2003) Enhanced proteolysis of beta-amyloid in APP transgenic mice prevents plaque formation, secondary pathology, and premature death. Neuron 40:1087–1093
Miners JS, van Helmond Z, Chalmers K, Wilcock G, Love S, Kehoe PG (2006) Decreased expression and activity of neprilysin in Alzheimer’s disease are associated with cerebral amyloid angiopathy. J Neuropathol Exp Neurol 65:1012–1021
Koistinaho M, Lin S, Wu X, Esterman M, Koger D, Hanson J, Higgs R, Liu F, Malkani S, Bales KR, Paul SM (2004) Apolipoprotein E promotes astrocyte colocalization and degradation of deposited amyloid-β peptides. Nature Med 10:719–726
Lee CY, Landreth GE (2010) The role of microglia in amyloid clearance from the AD brain. J Neural Transm 117:949–960
Basak JM, Verghese PB, Yoon H, Kim J, Holtzman DM (2012) Low-density lipoprotein receptor represents and apolipoprotein E-independent pathway of Aβ uptake and degradation by astrocytes. J Biol Chem 287:13959–13971
Kenekiyo T, Liu C-C, Shinohara M, Li J, Bu G (2012) LRP1 in brain vascular smooth muscle cells mediates local clearance of Alzheimer’s amyloid-β. J Neurosci 32:16458–16465
Kenekiyo T, Crrito JR, Liu C-C, Shinohara M, Li J, Schuler DR, Shinohara M, Holtzman DM, Bu G (2013) Neuronal clearance of amyloid-β by endocytic receptor LRP1. J Neurosci 33:19276–19283
Zlokovic BV, Martel CL, Matsubara E, McComb JG, Zheng G, McCluskey RT, Frangione B, Ghiso J (1996) Glycoprotein 330/megalin: probable role in receptor-mediated transport of apolipoprotein J alone and in a complex with Alzheimer disease amyloid beta at the blood-brain and blood-cerebrospinal fluid barriers. Proc Natl Acad Sci USA 93:4229–4234
Zlokovic BV (2004) Cleaning amyloid through the blood-brain barrier. J Neurochem 89:807–811
Cirrito JR, Deane R, Fagan AM, Spinner ML, Parsadanian M, Finn MB, Jiang H, Prior JL, Sagare A, Bales KR, Paul SM, Zlokovic BV, Piwnica-Worms D, Holtzman DM (2005) P-glycoprotein deficiency at the blood-brain barrier increases amyloid-beta deposition in an Alzheimer’s disease mouse models. J Clin Invest 115:3285–3290
Deane R, Sagare A, Hamm K, Parisi M, Lane S, Finn MB, Holtzman DM, Zlokovic BV (2008) apoE isoform-specific disruption of amyloid β; peptide clearance from mouse brain. J Clin Invest 118:4002–4013
Weller RO, Massery A, Newman TA, Hutchings M, Kuo YM, Roher AE (1998) Cerebral amyloid angiopathy: amyloid beta accumulates in putative interstitial fluid drainage pathways in Alzheimer’s disease. Am J Pathol 153:725–733
Preston SD, Steart PV, Wilkinson A, Nicoll JAR, Weller RO (2003) Capillary and arterial amyloid angiopathy in Alzheimer’s disease: defining the perivascular route for the elimination of amyloid beta from the human brain. Neuropathol Appl Neurobiol 29:106–117
Crossgrove JS, Li GJ, Zheng W (2005) The choroid plexus removes beta-amyloid from brain cerebrospinal fluid. Exp Biol Med (Maywood) 230:771–776
Zlokovic BV (2005) Neurovascular mechanisms of Alzheimer’s neurodegeneration. Trends Neurosci 28:202–208
Bell RD, Zlokovic BV (2009) Neurovascular mechanisms and blood-brain barrier disorder in Alzheimer’s disease. Acta Neuropathol 118:103–113
Lennon VA, Kryzer TJ, Pittock SJ, Verkman AS, Hinson SR (2005) IgG marker of optic-spinal multiple sclerosis binds to the aquaporin-4 water channel. J Exp Med 202:473–477
Acknowledgments
This study was supported by a Grant-in-aid for Scientific Research (C) 26430055 (M.U.) from the Ministry of Education, Culture, Sports, Science and Technology of Japan. The authors thank Ms. K. Yasutomi for editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Ueno, M., Chiba, Y., Murakami, R. et al. Blood–brain barrier and blood–cerebrospinal fluid barrier in normal and pathological conditions. Brain Tumor Pathol 33, 89–96 (2016). https://doi.org/10.1007/s10014-016-0255-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10014-016-0255-7