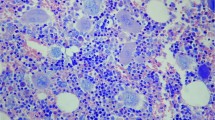
Abstract
A set of clinical and pathological criteria for the diagnosis and staging of Philadelphia chromosome-negative myeloproliferative disorders (Ph1--MPDs) is presented by including bone marrow histopathology as a significant tool to identify the early, manifest, and advanced stages of essential thrombocythemia (ET), polycythemia vera (PV), and idiopathic myelofibrosis/agnogenic myeloid metaplasia (IMF/AMM). This combined approach provides a pathognomonic clue to each of the different subtypes of Ph1--MPDs and further enables recognition of the various steps in the evolution of the myeloproliferative process. Increase and clustering of giant to large megakaryocytes with mature cytoplasm and multilobulated staghorn-like nuclei in a normal or only slightly increased cellular bone marrow represent major hallmarks of ET. Loose assemblies of small to giant pleiomorphic mega-karyocytes containing deeply lobulated nuclei together with a proliferation of erythro- and granulopoiesis (panmyelosis) are the specific lesions of PV. The initial prefibrotic and the overt and more advanced myelofibrotic stages of IMF/AMM show a pronounced proliferation of an abnormal megakaryo- and granulopoiesis dominated by clustered atypical medium-sized to giant megakaryocytes with cloud-like, bulbous, and often hyperchromatic nuclei, which are not seen in allied subtypes of MPDs including chronic myeloid leukemia (Ph1+-CML) and myelodysplastic syndromes (MDS). The presented clinical and pathological criteria modify the Polycythemia Vera Study Group (PVSG) proposals for the Ph1--MPDs by including bone marrow histopathology and are in keeping with features outlined in the new World Health Organization classification.The latter allows the differentiation of true ET from reactive thrombocytosis and from thrombocythemias as an eventually presenting finding in PV, IMF/AMM, MDS, and Ph1+-CML. Moreover, these diagnostic guidelines are able to separate latent and early PV from secondary erythrocytosis and to detect the prefibrotic and early stages of IMF/AMM. Myelofibrosis is not a feature of ET and is rarely observed in PV at time of diagnosis, but it becomes apparent during long-term follow-up and constitutes a prominent lesion during the course of IMF/ AMM. Life expectancy is almost normal in ET and is also not significantly altered during the first, but compromised during the second, decade of follow-up in PV. On the other hand, survival is substantially shortened in IMF/AMM, even for patients with throm-bocythemia as a frequent finding of prefibrotic and early stage IMF/AMM.
Similar content being viewed by others
References
Murphy S, Peterson P, Iland H, Laszlo J. Experience of the Poly-cythemia Vera Study Group with essential thrombocythemia: a final report on diagnostic criteria, survival, and leukemic transition by treatment.Semin Hematol. 1997;34:29–39.
Murphy S. Diagnostic criteria and prognosis in polycythemia vera and essential thrombocythemia.Semin Hematol. 1999;36:9–13.
Kutti J, Wadenvik H. Diagnostic and differential criteria of essential thrombocythemia and reactive thrombocytosis.Leuk Lymphoma. 1996;22(suppl 1):41–45.
Jantunen R, Juvonen E, Ikkala E, et al. Essential thrombocythemia at diagnosis: causes of diagnostic evaluation and presence of positive diagnostic findings.Ann Hematol. 1998;77:101–106.
Pearson TC. Diagnosis and classification of erythrocytoses and thrombocytoses.Baillieres Clin Haematol. 1998;11:695–720.
Michiels JJ, Abels J, Steketee J, van Vliet HH, Vuzevski VD. Erythromelalgia caused by platelet-mediated arteriolar inflammation and thrombosis in thrombocythemia.Ann Intern Med. 1985;102: 466–471.
Michiels JJ, van Genderen PJ, Lindemans J, van Vliet HH. Erythromelalgic, thrombotic and hemorrhagic manifestations in 50 cases of thrombocythemia.Leuk Lymphoma. 1996;22(suppl 1):47–56.
Ravandi-Kashani F, Schafer AI. Microvascular disturbances, thrombosis, and bleeding in thrombocythemia: current concepts and perspectives.Semin Thromb Hemost. 1997;23:479–488.
Griesshammer M, Bangerter M, van Vliet HH, Michiels JJ. Aspirin in essential thrombocythemia: status quo and quo vadis.Semin Thromb Hemost. 1997;23:371–377.
Dudley JM, Messinezy M, Eridani S, et al. Primary thrombo-cythaemia: diagnostic criteria and a simple scoring system for positive diagnosis.Br J Haematol. 1989;71:331–335.
Eridani S, Sawyer B, Pearson TC. Patterns of in vitro BFU-E proliferation in different forms of polycythaemia and in thrombo-cythaemia.Eur J Haematol. 1987;38:363–369.
Juvonen E, Ikkala E, Oksanen K, Ruutu T. Megakaryocyte and erythroid colony formation in essential thrombocythaemia and reactive thrombocytosis: diagnostic value and correlation to complications.Br J Haematol. 1993;83:192–197.
Shih LY, Lee CT. Identification of masked polycythemia vera from patients with idiopathic marked thrombocytosis by endogenous erythroid colony assay.Blood. 1994;83:744–748.
Florensa L, Besses C, Woessner S, et al. Endogenous megakaryo-cyte and erythroid colony formation from blood in essential throm-bocythaemia.Leukemia. 1995;9:271–273.
Yan L, Elkassar N, Gardin C, Briere J. Clonality assays and mega-karyocyte culture techniques in essential thrombocythemia.Leuk Lymphoma. 1996;22(suppl 1):31–40.
Westwood NB, Pearson TC. Diagnostic applications of haemopoietic progenitor culture techniques in polycythaemias and thrombo-cythaemias.Leuk Lymphoma. 1996;22(suppl 1):95–103.
Fialkow PJ, Faguet GB, Jacobson RJ, Vaidya K, Murphy S. Evidence that essential thrombocythemia is a clonal disorder with origin in a multipotent stem cell.Blood. 1981;58:916–919.
El-Kassar N, Hetet G, Briere J, Grandchamp B. Clonality analysis of hematopoiesis in essential thrombocythemia: advantages of studying T lymphocytes and platelets.Blood. 1997;89:128–134.
Harrison CN, Gale RE, Machin SJ, Linch DC. A large proportion of patients with a diagnosis of essential thrombocythemia do not have a clonal disorder and may be at lower risk of thrombotic complications.Blood. 1999;93:417–424.
Berlin NI. Diagnosis and classification of the polycythemias.Semin Hematol. 1975;12:339–351.
Berk PD, Goldberg JD, Donovan PB, Fruchtman SM, Berlin NI, Wasserman LR. Therapeutic recommendations in polycythemia vera based on Polycythemia Vera Study Group protocols.Semin Hematol. 1986;23:132–143.
Bilgrami S, Greenberg BR. Polycythemia rubra vera.Semin Oncol. 1995;22:307–326.
Pearson TC, Messinezy M.The diagnostic criteria of polycythaemia rubra vera.Leuk Lymphoma. 1996;22(suppl 1):87–93.
Messinezy M, Pearson TC. Diagnosis of polycythaemia.J Clin Pathol. 1998;51:1–2.
Kurnick JE, Ward HP, Block MH. Bone marrow sections in the differential diagnosis of polycythemia.Arch Pathol. 1972;94:489–499.
Vykoupil KF, Thiele J, Stangel W, Krmpotic E, Georgii A. Poly-cythemia vera, I: histopathology, ultrastructure and cytogenetics of the bone marrow in comparison with secondary polycythemia.Virchows Arch [Pathol Anat]. 1980;389:307–324.
Ellis JT, Silver RT, Coleman M, Geller SA. The bone marrow in polycythemia vera.Semin Hematol. 1975;12:433–444.
Ellis JT, Peterson P, Geller SA, Rappaport H. Studies of the bone marrow in polycythemia vera and the evolution of myelofibrosis and second hematologic malignancies.Semin Hematol. 1986;23: 144–155.
Pearson TC, Wetherley-Mein G. The course and complications of idiopathic erythrocytosis.Clin Lab Haematol. 1979;1:189–196.
Najean Y, Triebel F, Dresch C. Pure erythrocytosis: reappraisal of a study of 51 cases.Am J Hematol. 1981;10:129–136.
Lemoine F, Najman A, Baillou C, et al. A prospective study of the value of bone marrow erythroid progenitor cultures in poly-cythemia.Blood. 1986;68:996–1002.
Partanen S, Juvonen E, Ikkala E, Ruutu T. Spontaneous erythroid colony formation in the differential diagnosis of erythrocytosis.Eur J Haematol. 1989;42:327–330.
Adamson JW, Fialkow PJ, Murphy S, Prchal JF, Steinmann L. Poly-cythemia vera: stem-cell and probable clonal origin of the disease.N Engl J Med. 1976;295:913–916.
Westwood N, Dudley JM, Sawyer B, Messinezy M, Pearson TC. Primary polycythaemia: diagnosis by non-conventional positive criteria.Eur J Haematol. 1993;51:228–232.
Birgegard G, Wide L. Serum erythropoietin in the diagnosis of polycythaemia and after phlebotomy treatment.Br J Haematol. 1992;81:603–606.
Messinezy M, Westwood NB, Woodcock SP, Strong RM, Pearson TC. Low serum erythropoietin—a strong diagnostic criterion of primary polycythaemia even at normal haemoglobin levels.Clin Lab Haematol. 1995;17:217–220.
Carneskog J, Kutti J, Wadenvik H, Lundberg PA, Lindstedt G. Plasma erythropoietin by high-detectability immunoradiometric assay in untreated and treated patients with polycythaemia vera and essential thrombocythaemia.Eur J Haematol. 1998;60:278–282.
Georgii A, Vykoupil KF, Buhr T, et al. Chronic myeloproliferative disorders in bone marrow biopsies.Pathol Res Pract. 1990;186:3–27.
Varki A, Lottenberg R, Griffith R, Reinhard E. The syndrome of idiopathic myelofibrosis: a clinicopathologic review with emphasis on the prognostic variables predicting survival.Medicine (Baltimore). 1983;62:353–371.
Smith RE, Chelmowski MK, Szabo EJ. Myelofibrosis: a concise review of clinical and pathologic features and treatment.Am J Hematol. 1988;29:174–180.
Barosi G,Ambrosetti A, Finelli C, et al.The Italian Consensus Conference on diagnostic criteria for myelofibrosis with myeloid metaplasia.Br J Haematol. 1999;104:730–737.
Tefferi A, Silverstein MN, Noel P. Agnogenic myeloid metaplasia.Semin Oncol. 1995;22:327–333.
Reilly JT. Pathogenesis and management of idiopathic myelofibrosis.Baillieres Clin Haematol. 1998;11:751–767.
Tefferi A. Myelofibrosis with myeloid metaplasia.N Engl J Med. 2000;342:1255–1265.
Njoku OS, Lewis SM, Catovsky D, Gordon-Smith EC. Anaemia in myelofibrosis: its value in prognosis.Br J Haematol. 1983;54:79–89.
Visani G, Finelli C, Castelli U, et al. Myelofibrosis with myeloid metaplasia: clinical and haematological parameters predicting survival in a series of 133 patients.Br J Haematol. 1990;75:4–9.
Hasselbalch H, Jensen BA. Prognostic factors in idiopathic myelofibrosis: a simple scoring system with prognostic significance.Eur J Haematol. 1990;44:172–178.
Rupoli S, Da Lio L, Sisti S, et al. Primary myelofibrosis: a detailed statistical analysis of the clinicopathological variables influencing survival.Ann Hematol. 1994;68:205–212.
Thiele J, Kvasnicka HM,Werden C, Zankovich R, Diehl V, Fischer R. Idiopathic primary osteo-myelofibrosis: a clinico-pathological study on 208 patients with special emphasis on evolution of disease features, differentiation from essential thrombocythemia and variables of prognostic impact.Leuk Lymphoma. 1996;22:303–317.
Dupriez B, Morel P, Demory JL, et al. Prognostic factors in agnogenic myeloid metaplasia: a report on 195 cases with a new scoring system.Blood. 1996;88:1013–1018.
Kvasnicka HM, Thiele J, Werden C, Zankovich R, Diehl V, Fischer R. Prognostic factors in idiopathic (primary) osteomyelofibrosis.Cancer. 1997;80:708–719.
Cervantes F, Pereira A, Esteve J, et al. Identification of ‘short-lived’ and ‘long-lived’ patients at presentation of idiopathic myelofibrosis.Br J Haematol. 1997;97:635–640.
Reilly JT, Snowden JA, Spearing RL, et al. Cytogenetic abnormalities and their prognostic significance in idiopathic myelofibrosis: a study of 106 cases.Br J Haematol. 1997;98:96–102.
Cervantes F, Barosi G, Demory JL, et al. Myelofibrosis with myeloid metaplasia in young individuals: disease characteristics, prognostic factors and identification of risk groups.Br J Haematol. 1998;102:684–690.
Georgii A, Vykoupil KF, Thiele J. Chronic megakaryocytic granulocytic myelosis-CMGM: a subtype of chronic myeloid leukemia.Virchows Arch [Pathol Anat]. 1980;389:253–268.
Thiele J, Holgado S, Choritz H, Georgii A. Abnormalities of mega-karyocytes in myelitis and chronic myeloproliferative diseases.Virchows Arch B Cell Pathol Incl Mol Pathol. 1982;41:67–81.
Georgii A, Buhr T, Buesche G, Kreft A, Choritz H. Classification and staging of Ph-negative myeloproliferative disorders by histopathology from bone marrow biopsies.Leuk Lymphoma. 1996;22(suppl 1):15–29.
Georgii A, Buesche G, Kreft A. The histopathology of chronic myeloproliferative diseases.Baillieres Clin Haematol. 1998;11: 721–749.
Thiele J, Kvasnicka HM, Diehl V, Fischer R, Michiels J. Clinico-pathological diagnosis and differential criteria of thrombo-cythemias in various myeloproliferative disorders by histopathology, histochemistry and immunostaining from bone marrow biopsies.Leuk Lymphoma. 1999;33:207–218.
Thiele J, Kvasnicka HM, Boeltken B, Zankovich R, Diehl V, Fischer R. Initial (prefibrotic) stages of idiopathic (primary) myelofibrosis (IMF): a clinicopathological study.Leukemia. 1999;13: 1741–1748.
Thiele J, Imbert M, Pierre R, Vardiman JW, Brunning RD, Flandrin G. Chronic idiopathic myelofibrosis. In: Jaffe ES, Harris NL, Stein H, Vardiman JW, eds.WHO Classification of Tumours: Tumours of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC Press; 2001:35–38.
Schaefer HE. How to fix, decalcify and stain paraffin embedded bone marrow biopsies. In: Lennert K, Huebner K, ed.Pathology of the Bone Marrow. Stuttgart, New York: G. Fischer; 1984:6–9.
Thiele J, Kvasnicka HM, Fischer R. Histochemistry and morphometry on bone marrow biopsies in chronic myeloproliferative disorders: aids to diagnosis and classification.Ann Hematol. 1999;78: 495–506.
Burkhardt R, Bartl R, Jaeger K, et al. Chronic myeloproliferative disorders (CMPD).Pathol Res Pract. 1984;179:131–186.
Bartl R, Frisch B, Wilmanns W. Potential of bone marrow biopsy in chronic myeloproliferative disorders (MPD).Eur J Haematol. 1993;50:41–52.
Bernhards J, Weitzel B, Werner M, Rimpler M, Georgii A. A new histological embedding method by low-temperature polymerisation of methyl methacrylate allowing immuno- and enzyme histochemical studies on semi-thin sections of undecalcified bone marrow biopsies.Histochemistry. 1992;98:145–154.
Dickstein JI, Vardiman JW. Issues in the pathology and diagnosis of the chronic myeloproliferative disorders and the myelodysplastic syndromes.Am J Clin Pathol. 1993;99:513–525.
Dickstein JI, Vardiman JW. Hematopathologic findings in the myeloproliferative disorders.Semin Oncol. 1995;22:355–373.
Thiele J, Kvasnicka HM, Zankovich R, Diehl V. Relevance of bone marrow features in the differential diagnosis between essential thrombocythemia and early stage idiopathic myelofibrosis.Haematologica. 2000;85:1126–1134.
Thiele J, Fischer R. Megakaryocytopoiesis in haematological disorders: diagnostic features of bone marrow biopsies: an overview.Virchows Arch A Pathol Anat Histopathol. 1991;418:87–97.
Imbert M, Pierre R, Thiele J, Vardiman JW, Brunning RD, Flandrin G. Essential thrombocythaemia. In: Jaffe ES, Harris NL, Stein H, Vardiman JW, eds.WHO Classification of Tumours: Tumours of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC Press; 2001:39–41. tumor
Pierre R, Imbert M, Thiele J, Vardiman JW, Brunning RD, Flandrin G. Polycythaemia vera. In: Jaffe ES, Harris NL, Stein H,Vardiman JW, eds.WHO Classification of Tumors: Tumors of Haematopoietic and Lymphoid Tissues. Lyon, France: IARC Press; 2001: 32–38.
Michiels JJ, Juvonen E. Proposal for revised diagnostic criteria of essential thrombocythemia and polycythemia vera by the Throm-bocythemia Vera Study Group.Semin Thromb Hemost. 1997;23: 339–347.
Michiels JJ. Normal life expectancy and thrombosis-free survival in aspirin treated essential thrombocythemia.Clin Appl Thromb Hemost. 1999;5:30–36.
Lengfelder E, Hochhaus A, Kronawitter U, et al. Should a platelet limit of 600 x 109/l be used as a diagnostic criterion in essential thrombocythaemia? an analysis of the natural course including early stages.Br J Haematol. 1998;100:15–23.
Sacchi S, Vinci G, Gugliotta L, et al. Diagnosis of essential thrombocythemia at platelet counts between 400 and 600 x 109/L: Gruppo Italiano Malattie Mieloproliferative Croniche (GIMMC).Haematologica. 2000;85:492–495.
Thiele J, Funke S, Holgado S, Choritz H, Georgii A. Megakary-opoiesis in chronic myeloproliferative diseases: a morphometric evaluation with special emphasis on primary thrombocythemia.Anal Quant Cytol. 1984;6:155–167.
Thiele J, Zankovich R, Schneider G, Kremer B, Fischer R, Diehl V. Primary (essential) thrombocythemia versus polycythemia vera rubra: a histomorphometric analysis of bone marrow features in trephine biopsies.Anal Quant Cytol Histol. 1988;10:375–382.
Kaloutsi V, Fritsch RS, Buhr T, Restrepo-Specht I, Widjaja W, Georgii A. Megakaryocytes in chronic myeloproliferative disorders: numerical density correlated between different entities.Virchows Arch A Pathol Anat Histopathol. 1991;418:493–497.
Michiels JJ, Prins ME, Hagermeijer A, et al. Philadelphia chromosome-positive thrombocythemia and megakaryoblast leukemia.Am J Clin Pathol. 1987;88:645–652.
Morris CM, Fitzgerald PH, Hollings PE, et al. Essential thrombocythaemia and the Philadelphia chromosome.Br J Haematol. 1988; 70:13–19.
Blickstein D, Aviram A, Luboshitz J, et al. BCR-ABL transcripts in bone marrow aspirates of Philadelphia-negative essential thrombocytopenia patients: clinical presentation.Blood. 1997;90: 2768–2771.
Aviram A, Blickstein D, Stark P, et al. Significance of BCR-ABL transcripts in bone marrow aspirates of Philadelphia-negative essential thrombocythemia patients.Leuk Lymphoma. 1999;33:77–82.
Damaj G, Delabesse E, Le Bihan C, et al. Typical essential thrombocythaemia does not express bcr-abelson fusion transcript.Br J Haematol. 2002;116:812–816.
Koike T, Uesugi Y,Toba K, et al. 5q-syndrome presenting as essential thrombocythemia: myelodysplastic syndrome or chronic myeloproliferative disorders?Leukemia. 1995;9:517–518.
Neuwirtova R, Mocikova K, Musilova J, et al. Mixed myelodysplastic and myeloproliferative syndromes.Leuk Res. 1996;20: 717–726.
Gupta R, Abdalla SH, Bain BJ. Thrombocytosis with sideroblastic erythropoiesis: a mixed myeloproliferative myelodysplastic syndrome.Leuk Lymphoma. 1999;34:615–619.
Bain BJ. The relationship between the myelodysplastic syndromes and the myeloproliferative disorders.Leuk Lymphoma. 1999;34: 443–449.
Mathew P,Tefferi A, Dewald GW, et al.The 5q- syndrome: a single-institution study of 43 consecutive patients.Blood. 1993;81: 1040–1045.
Boultwood J, Lewis S,Wainscoat JS.The 5q-syndrome.Blood. 1994; 84:3253–3260.
Schmitt-Gräff A, Thiele J, Zuk I, Kvasnicka HM. Essential throm-bocythemia with ringed sideroblasts: a heterogeneous spectrum of diseases, but not a distinct entity.Haematologica. 2002;87: 393–400.
Michiels JJ, Barbui T, Finazzi G, et al. Diagnosis and treatment of polycythemia vera and possible future study designs of the PVSG.Leuk Lymphoma. 2000;36:239–253.
Thiele J, Kvasnicka HM, Muehlhausen K, Walter S, Zankovich R, Diehl V. Polycythemia rubra vera versus secondary polycythemias: a clinicopathological evaluation of distinctive features in 199 patients.Pathol Res Pract. 2001;197:77–84.
Thiele J, Kvasnicka HM, Zankovich R, Diehl V. The value of bone marrow histology in differentiating between early stage poly-cythemia vera and secondary (reactive) polycythemias.Haematologica. 2001;86:368–374.
Thiele J, Kvasnicka HM, Zankovich R, Diehl V. Clinical and morphological criteria for the diagnosis of prefibrotic idiopathic (primary) myelofibrosis.Ann Hematol. 2001;80:160–165.
Mesa RA, Silverstein MN, Jacobsen SJ, Wollan PC, Tefferi A. Population-based incidence and survival figures in essential thrombo-cythemia and agnogenic myeloid metaplasia: an Olmsted County Study, 1976–1995.Am J Hematol. 1999;61:10–15.
Annaloro C, Lambertenghi Deliliers G, Oriani A, et al. Prognostic significance of bone marrow biopsy in essential thrombocythemia.Haematologica. 1999;84:17–21.
Rozman C, Giralt M, Feliu E, Rubio D, Cortes MT. Life expectancy of patients with chronic nonleukemic myeloproliferative disorders.Cancer. 1991;67:2658–2663.
Najean Y, Arrago JP, Rain JD, Dresch C. The ‘spent’ phase of poly-cythaemia vera: hypersplenism in the absence of myelofibrosis.Br J Haematol. 1984;56:163–170.
Najean Y, Rain JD. The very long-term evolution of poly-cythemia vera: an analysis of 318 patients initially treated by phlebotomy or 32P between 1969 and 1981.Semin Hematol. 1997;34:6–16.
Meytes D, Katz D, Ramot B. Preleukemia and leukemia in poly-cythemia vera.Blood. 1976;47:237–241.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Michiels, J.J., Thiele, J. Clinical and Pathological Criteria for the Diagnosis of Essential Thrombocythemia, Polycythemia Vera, and Idiopathic Myelofibrosis (Agnogenic Myeloid Metaplasia). Int J Hematol 76, 133–145 (2002). https://doi.org/10.1007/BF02982575
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/BF02982575