Abstract
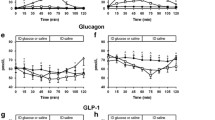
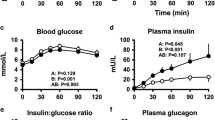
In healthy volunteers, the effects of intravenously administered glucagon on small intestinal function was investigated. Bolus doses resulting in plasma glucagon concentrations of >800 pg/ml (5 min after injection) abolished jejunal contractions for 4.4±0.4 (sem) min after a latency period of 49±4 sec. During continuous intravenous glucagon infusion, jejunal dilatation and increase in mean transit time (MTT) occurred at plasma levels >720 pg/ml, while inhibition of water and electrolyte absorption was observed only with plasma glucagon concentrations of 1760±114 pg/ml. Under these conditions, the propulsion of fasting intestinal contents was slowed without change in flow rate. The observed effects cannot be attributed to the simultaneously occurring rise in plasma insulin and glucose concentrations. Short-term increases in circulating glucagon concentration inhibit intestinal tone, contractions, and propulsion with only a minor effect on water and electrolyte absorption limited to a narrow concentration range of plasma glucagon. Neither effect occurs at glucagon levels likely to occur under physiologic concentrations. The latency period preceding the abolition of jejunal contractions suggests that glucagon does not act directly on intestinal smooth muscle cells.
Similar content being viewed by others
References
Ganeshappa KP, Whalen GE, Meade RC, Soergel KH: The effect of glucagon on jejunal motility, electrolyte and water absorption in man. Clin Res 19:658, 1971 (abstract)
Ganeshappa KP, Whalen GE, Soergel KH: The effect of glucagon on small intestine absorption in man. Gastroenterology 62:750, 1972 (abstract)
Stunkard AJ, van Itallie TB, Reiss BB: The mechanism of satiety: Effect of glucagon on gastric hunger contractions in man. Proc Soc Exp Biol Med 89:258–261, 1952
Dotevall G, Kock NG: The effect of glucagon on intestinal motility in man. Gastroenterology 45:364–367, 1963
Kock N, Darle N, Dotevall G: Inhibition of intestinal motility in man by glucagon given intraportally. Gastroenterology 53:88–92, 1967
Mekhjian H, King DR, Sanzenbacher L, Zollinger R: Glucagon and secretin inhibit water and electrolyte absorption in the human jejunum. Gastroenterology 62:782, 1972 (abstract)
Hicks T, Turnberg LA: Influence of glucagon on the human jejunum. Gastroenterology 67:1114–1118, 1974
Barbezat GO, Grossman MI: Intestinal secretion: Stimulation by peptides. Science 174:422–424, 1971
Barbezat GO, Grossman MI: Cholera-like diarrhea induced by glucagon plus gastrin. Lancet 1:1025–1026, 1971
Sanzenbacker L, Mekhjian H, King DR, Zollinger R: Studies on the potential role of secretin in the islet cell tumor diarrheogenic syndrome. Ann Surg 176:394–402, 1972
Moore EW, Longacher JW: The effect of peptide hormones on simultaneous jejunal and ileal H2O and electrolyte transport in the rabbit. I. Glucagon: The nature of the effect. Gastroenterology 66:749, 1974 (abstract)
Moore EW, Tavano PJ: The effect of peptide hormones on simultaneous jejunal and ileal H2O and electrolyte transport in the dog. II. Glucagon: Some paradoxical effects. Gastroenterology 66:749, 1974 (abstract)
Ingelfinger FJ, Abbott WO: Intubation studies of the human small intestine. The diagnostic significance of motor disturbances. Am J Dig Dis 7:468–474, 1940
Soergel KH, Whalen GE, Harris JA, Geenen JE: Effect of antidiuretic hormone on human small intestinal water and solute transport. J Clin Invest 47:1071–1082, 1968
Whalen GE, Geenen JE, Harris JA, Soergel KH: Sodium and water absorption from the human small intestine. Accuracy of the perfusion technique. Gastroenterology 51:975–984, 1966
Costrini NV, Ganeshappa KP, Wu WC, Whalen GE, Soergel KH: Effect of insulin, glucose, and controlled diabetes mellitus on human jejunal function. Am J Physiol 233:E181–187, 1977
Dillard RL, Eastman H, Hordtran JS: Volume flow relationships during the transport of fluid through the human small intestine. Gastroenterology 49:58–66, 1965
Zierler KL: Circulation times and the theory of indicatordilution methods for determining the blood flow and volume. Handbook of Physiology. WF Hamilton, P Dow (eds). Washington, D.C., Am Physiol Soc, 1962, pp 585–615
Soergel KH: Flow measurements of test meals and fasting contents in the human small intestine. Gastrointestinal Motility. L Demling, R Ottenjann (eds). New York, Academic Press, 1971, pp 81–92
Hill BJ, Kessler G: An automated determination of glucose utilizing a glucose oxidase-peroxidase system. J Lab Clin Med 57:970–980, 1961
Morgan CR, Lazarow A: Immunoassay of insulin: Two antibody system, plasma insulin levels of normal subdiabetic and diabetic rats. Diabetes 12:115–126, 1963
Snedecor GW: Statistical Methods. Ames, Iowa State University Press, 1967
Connell AM, Texter EC, Vantrappen G: Classification and interpretation of motility records. Am J Dig Dis 10:481–483, 1965
Foulk WT, Code CF, Morlock CG, Bargen JA: A study of motility patterns and the basic rhythm in the duodenum and upper part of the jejunum of human beings. Gastroenterology 26:601–611, 1954
Vantrappen G, Janssens J, Hellemans J, Ghoos Y: The interdigestive motor complex of normal subjects and patients with bacterial overgrowth of the small intestine. J Clin Invest 59:1158–1166, 1977
Aquilar-Parada EA, Eisentraut AM, Unger RH: Effects of starvation on plasma pancreatic glucagon in normal man. Diabetes 18:717–723, 1969
Marliss EB, Aoki TT, Unger RH, Soeldner JS, Cahill GF: Glucagon levels and metabolic effects in fasting man. J Clin Invest 49:2256–2270, 1970
Scott LD, Summers RW: Correlation of contractions and transit in rat small intestine. Am J Physiol 230:132–137, 1976
Fasth S, Hultén L: Effect of glucagon on intestinal motility and blood flow. Acta Physiol Scand 83:169–193, 1970
Whalen GE, Soergel KH, Geenen JE: Diabetic diarrhea. A clinical and pathophysiological study. Gastroenterology 56:1021–1032, 1969
Cameron AH, Phillips SF, Summerskill WHJ: Comparison of the effects of gastrin, cholecystokinin-pancreozymin, secretin and glucagon on human stomach musclein vitro. Gastroenterology 59:539–545, 1970
Hinterberger H, Wilcken DEL: The effect of prolonged glucagon infusions on the urinary secretion of catecholamines and 4-hydroxy-3-methoxymandelic acid and on adrenal medullary tissue levels of catecholamines in patients with severe cardiac disease. Clin Chim Acta 52:153–161, 1974
Wingate DL, Pearce EA, Thomas PH, Boucher BJ: Glucagon stimulates intestinal myoelectric activity. Gastroenterology 74:1152, 1978 (abstract)
Schwartz CJ, Kimberg DV, Sheerin HE, Field M, Said SI: Vasoactive intestinal peptide stimulation of adenylate cyclase and active electrolyte secretion in intestinal mucosa. J Clin Invest 54:536–544, 1974
MacFerran SN, Mailman D: Effects of glucagon on canine intestinal sodium and water fluxes and regional blood flow. J Physiol 266:1–12, 1977
McGavran MH, Unger RH, Recant L, Polk HC, Kilo C, Levin ME: A glucagon secreting alpha-cell carcinoma in the pancreas. N Engl J Med 274:1408–1413, 1966
Mallinson CN, Bloom SR, Warin AP, Salmon PR, Cox B: A glucagonoma syndrome. Lancet 2:1–4, 1974
Boden G, Owen OE: Familial hyperglucagonomeia—an autosomal dominant disorder. N Engl J Med 296:534–538, 1977
Rudo ND, Rosenberg IH: Chronic glucagon administration enhances intestinal transport in the rat. Proc Soc Exp Biol Med 142:521–525, 1973
Caspary WF, Lucke H: Effect of chronic glucagon administration on the digestive and absorptive function of rat small intestinein vivo. Res Exp Med 167:1–13, 1976
Rigopoulou D, Valverde I, Marco J, Faloona G, Dunger RH: Large glucagon immunoreactivity in extracts of pancreas. J Biol Chem 245:496–501, 1970
Author information
Authors and Affiliations
Additional information
This work was supported by the Medical Research Service of the Verterans Administration and grant #AM-12985 from the National Institute for Arthritis, Metabolism and Digestive Diseases, National Institutes of Health, Bethesda, Maryland.
Rights and permissions
About this article
Cite this article
Patel, G.K., Whalen, G.E., Soergel, K.H. et al. Glucagon effects on the human small intestine. Digest Dis Sci 24, 501–508 (1979). https://doi.org/10.1007/BF01489316
Issue Date:
DOI: https://doi.org/10.1007/BF01489316