Bone-Targeting Drugs: From vesicle to cytosol
Despite its appearance, bone is a highly metabolic and dynamic tissue that is composed of a vast network of cells called osteocytes that are embedded in a matrix made mostly of collagen and various salts of calcium and phosphate. These osteocytes sense regions of damaged or weakened bone, and 'instruct' bone-destroying cells (called osteoclasts) and bone-forming cells (osteoblasts) to, respectively, remove old bone and deposit new bone (Figure 1). Hence, like a team of road-repairers, the osteocytes, osteoclasts and osteoblasts work together to repair bone and maintain our skeleton in good health (Crockett et al., 2011).
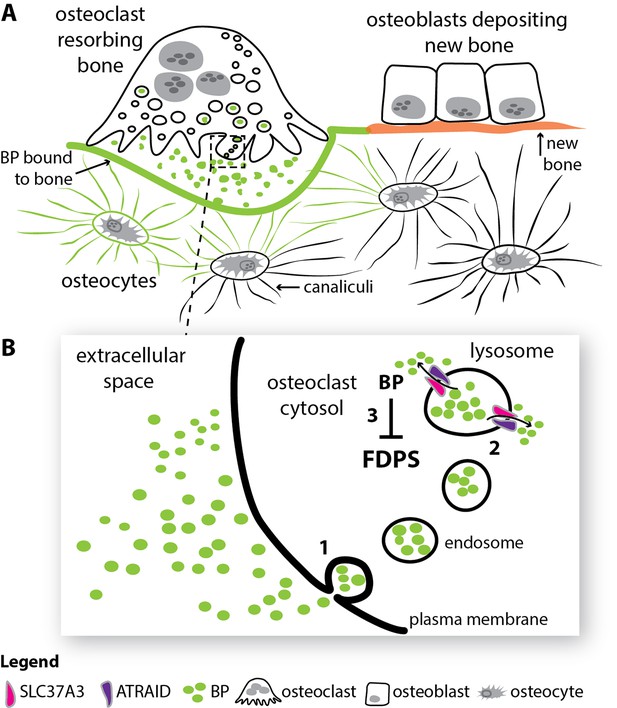
How bisphosphonates act in bone.
(A) Old and damaged bone is constantly being broken down by cells called osteoclasts in a process called resorption (top left), while new bone is deposited by cells called osteoblasts (top right). Cells called osteocytes (bottom) influence both of these processes through a spidery system of tiny canals called canaliculi. After entering the circulation, the drug bisphosphonate (green) binds very effectively to calcium ions on the bone mineral surface. During resorption, the bisphosphonate on the bone surface is released into the acidic extracellular space beneath the osteoclast. (B) The bisphosphonate in the extracellular space is engulfed into osteoclasts via a process called endocytosis (1). The resulting endosomes mature to form structures called lysosomes, and two proteins, SLC37A3 and ATRAID, then interact in the membrane of the lysosome to allow the bisphosphonate to enter the cytosol (2). Once in the cytosol, the nitrogen-containing bisphosphonates inhibit an enzyme called FDPS and prevent the osteoclast from breaking down bone (3). BP: bisphosphonate; FDPS: farnesyl diphosphate synthase; SLC37A3: solute carrier family 37 member A3.
In young adult life there is usually a balance between the amount of old bone broken down and the amount of new bone formed by this repair process, so there is no net gain or loss of bone mass. However, in diseases that affect the skeleton, such as post-menopausal osteoporosis or cancers growing in bone, this delicate balance can be disturbed by osteoclasts being over-active, which leads to excessive bone destruction and fractures. Drugs called bisphosphonates – which inhibit osteoclasts – have been used for more than three decades to treat such diseases and protect the skeleton from potentially catastrophic bone loss, although researchers still do not fully understand how they work. Now, in eLife, Erin O'Shea of Harvard University and the Howard Hughes Medical Institute (HHMI) and colleagues – including Zhou Yu as first author – report the answer to one of the remaining questions about these drugs (Yu et al., 2018).
Bisphosphonates are synthetic molecules that closely resemble the chemical structure of pyrophosphate, which is a natural by-product of numerous metabolic reactions. Importantly, bisphosphonates have two negatively-charged phosphonate groups that enable them to bind calcium ions very effectively, and hence to localize rapidly to any exposed calcium on the bone surface (Rogers et al., 2011). The mechanisms used by bisphosphonates to inhibit osteoclasts remained a mystery for several decades after they were first used in the clinic, but this did not stop the development of improved versions of the drugs (Russell et al., 2008). Eventually it was discovered that nitrogen-containing bisphosphonates (N-BPs), which are now widely used to treat osteoporosis and other bone diseases, work by inhibiting an enzyme called FDPS inside the osteoclasts (Luckman et al., 1998; Bergstrom et al., 2000; Dunford et al., 2001). The N-BP molecules displace the lipid substrates that the FDPS enzyme usually acts on, locking the enzyme in an inactive state (Kavanagh et al., 2006; Rondeau et al., 2006). Without FDPS activity, osteoclasts are no longer able to degrade bone (Rogers et al., 2011).
However, one question remained: how do the N-BPs and other bisphosphonates actually reach the FDPS enzyme, which is in the cytosol of the osteoclasts? There was little or no evidence that a receptor on the plasma membrane was involved (Thompson et al., 2006). Studies with fluorescently-tagged bisphosphonates showed that they first entered the osteoclasts via endocytosis – a process that involves the cell membrane folding inwards and then pinching off to create a vesicle inside the cell (Coxon et al., 2008). But how do the drugs leave these vesicles – which are enclosed by a membrane – to enter the cytosol? Bisphosphonate molecules have a large negative charge, which rules out passive diffusion across the vesicle membrane, which in turn suggests the possibility of a hitherto unidentified transport mechanism (Thompson et al., 2006).
Yu et al. – who are based at Harvard, HHMI, UCSF, MIT, the Broad, Koch and Whitehead Institutes, and Washington University – report that they have identified a protein called SLC37A3 that is required for the release of N-BP molecules from vesicles into the cytosol. Using a CRISPR-based approach to screen for genes that, when missing, confer resistance to bisphosphonates, they identified SLC37A3 as the gene with the strongest effect. Although the exact function of the SLC37A3 protein remains to be clarified, related members of this protein family are involved in the transport of charged molecules across membranes (Cappello et al., 2018).
Yu et al. found that SLC37A3 interacts and co-localizes with a protein called ATRAID at the vesicle membrane (Figure 1). Importantly, vesicles isolated from cells that did not express SLC37A3 or ATRAID appeared unable to release N-BP molecules, and these cells were much less sensitive to the pharmacological effect of N-BPs.
This new transport mechanism identified by Yu et al. raises interesting questions about how the SLC37A3/ATRAID complex specifically recognizes N-BP molecules, and how it transports them across the membrane of the vesicle. It will also be worthwhile to determine whether differences in the expression of SLC37A3 or ATRAID account for the different sensitivity of osteoclasts and other cell types to N-BP molecules, or whether variants in these genes affect the clinical responsiveness of patients to these drugs. Nevertheless, these elegant studies explain how negatively-charged N-BP molecules can gain access to the cell cytosol after endocytosis and, as a result, go on to benefit huge numbers of patients with potentially devastating bone diseases.
References
-
Alendronate is a specific, nanomolar inhibitor of farnesyl diphosphate synthaseArchives of Biochemistry and Biophysics 373:231–241.https://doi.org/10.1006/abbi.1999.1502
-
Bone remodelling at a glanceJournal of Cell Science 124:991–998.https://doi.org/10.1242/jcs.063032
-
Structure-activity relationships for inhibition of farnesyl diphosphate synthase in vitro and inhibition of bone resorption in vivo by nitrogen-containing bisphosphonatesJournal of Pharmacology and Experimental Therapeutics 296:235–242.
Article and author information
Author details
Publication history
- Version of Record published: June 27, 2018 (version 1)
Copyright
© 2018, Rogers et al.
This article is distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use and redistribution provided that the original author and source are credited.
Metrics
-
- 1,205
- views
-
- 133
- downloads
-
- 6
- citations
Views, downloads and citations are aggregated across all versions of this paper published by eLife.
Download links
Downloads (link to download the article as PDF)
Open citations (links to open the citations from this article in various online reference manager services)
Cite this article (links to download the citations from this article in formats compatible with various reference manager tools)
Further reading
-
- Biochemistry and Chemical Biology
- Structural Biology and Molecular Biophysics
DNA gyrase, a ubiquitous bacterial enzyme, is a type IIA topoisomerase formed by heterotetramerisation of 2 GyrA subunits and 2 GyrB subunits, to form the active complex. DNA gyrase can loop DNA around the C-terminal domains (CTDs) of GyrA and pass one DNA duplex through a transient double-strand break (DSB) established in another duplex. This results in the conversion from a positive (+1) to a negative (–1) supercoil, thereby introducing negative supercoiling into the bacterial genome by steps of 2, an activity essential for DNA replication and transcription. The strong protein interface in the GyrA dimer must be broken to allow passage of the transported DNA segment and it is generally assumed that the interface is usually stable and only opens when DNA is transported, to prevent the introduction of deleterious DSBs in the genome. In this paper, we show that DNA gyrase can exchange its DNA-cleaving interfaces between two active heterotetramers. This so-called interface ‘swapping’ (IS) can occur within a few minutes in solution. We also show that bending of DNA by gyrase is essential for cleavage but not for DNA binding per se and favors IS. Interface swapping is also favored by DNA wrapping and an excess of GyrB. We suggest that proximity, promoted by GyrB oligomerization and binding and wrapping along a length of DNA, between two heterotetramers favors rapid interface swapping. This swapping does not require ATP, occurs in the presence of fluoroquinolones, and raises the possibility of non-homologous recombination solely through gyrase activity. The ability of gyrase to undergo interface swapping explains how gyrase heterodimers, containing a single active-site tyrosine, can carry out double-strand passage reactions and therefore suggests an alternative explanation to the recently proposed ‘swivelling’ mechanism for DNA gyrase (Gubaev et al., 2016).
-
- Biochemistry and Chemical Biology
- Structural Biology and Molecular Biophysics
Vitamin B6 deficiency has been linked to cognitive impairment in human brain disorders for decades. Still, the molecular mechanisms linking vitamin B6 to these pathologies remain poorly understood, and whether vitamin B6 supplementation improves cognition is unclear as well. Pyridoxal 5’-phosphate phosphatase (PDXP), an enzyme that controls levels of pyridoxal 5’-phosphate (PLP), the co-enzymatically active form of vitamin B6, may represent an alternative therapeutic entry point into vitamin B6-associated pathologies. However, pharmacological PDXP inhibitors to test this concept are lacking. We now identify a PDXP and age-dependent decline of PLP levels in the murine hippocampus that provides a rationale for the development of PDXP inhibitors. Using a combination of small-molecule screening, protein crystallography, and biolayer interferometry, we discover, visualize, and analyze 7,8-dihydroxyflavone (7,8-DHF) as a direct and potent PDXP inhibitor. 7,8-DHF binds and reversibly inhibits PDXP with low micromolar affinity and sub-micromolar potency. In mouse hippocampal neurons, 7,8-DHF increases PLP in a PDXP-dependent manner. These findings validate PDXP as a druggable target. Of note, 7,8-DHF is a well-studied molecule in brain disorder models, although its mechanism of action is actively debated. Our discovery of 7,8-DHF as a PDXP inhibitor offers novel mechanistic insights into the controversy surrounding 7,8-DHF-mediated effects in the brain.






