Abstract
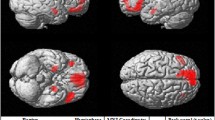
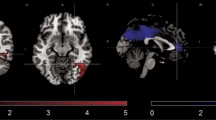
It has been proposed that the neural basis for cognitive vulnerability to depression involves an imbalance in frontolimbic activity during the processing of cues with a negative affective value. Although the question is central to cognitive theory, whether this association is amplified by diagnosis of an affective disorder or recent life stress has not been investigated. A composite cognitive vulnerability score based on questionnaire assessment was used to predict neural responses to negative emotional stimuli in N = 112 participants. Potential moderating effects of psychiatric diagnosis and negative life events were examined. Main and interaction effects were tested against a threshold of p < .05, family-wise error (FWE) corrected at the cluster level, and the results were small-volume corrected in regions of interest. Cognitive vulnerability predicted higher activation of superior parietal areas (p FWE < .01) for negative than for positive faces. The association was significantly stronger in healthy participants. For negative versus control stimuli, cognitive vulnerability predicted higher ventrolateral prefrontal and subgenual anterior cingulate activation (p FWE < .05) to equal extents in both groups. We found no evidence for an association with amygdala activation. Life events did not moderate the findings. We concluded that cognitive vulnerability was associated with higher activation of frontoparietal areas during an implicit emotional task. These higher levels of activation may potentially reflect increased effort being required to ignore irrelevant negative emotional information in vulnerable populations.


Similar content being viewed by others
References
Alloy, L., Abramson, L., Whitehouse, W., Hogan, M., Tashman, N., Steinberg, D., & Donovan, P. (1999). Depressogenic cognitive styles: Predictive validity, information processing and personality characteristics, and developmental origins. Behaviour Research and Therapy, 37, 503–531. doi:10.1016/S0005-7967(98)00157-0
American Psychiatric Association. (2004). Diagnostic and statistical manual of mental disorders (DSM-IV) (4th ed., Text rev.). Washington, DC: Author.
Banich, M. T., Mackiewicz, K. L., Depue, B. E., Whitmer, A. J., Miller, G. A., & Heller, W. (2009). Cognitive control mechanisms, emotion and memory: A neural perspective with implications for psychopathology. Neuroscience & Biobehavioral Reviews, 33, 613–630. doi:10.1016/j.neubiorev.2008.09.010
Barch, D. M. (2014). Risk for mood pathology: Neural and psychological markers of abnormal negative information processing. Journal of the American Academy of Child and Adolescent Psychiatry, 53, 497–499. doi:10.1016/j.jaac.2014.01.012
Beck, A. (1963). Thinking and depression: 1. Idiosyncratic content and cognitive distortions. Archives of General Psychiatry, 9, 324–333.
Beck, A. T. (2008). The evolution of the cognitive model of depression and its neurobiological correlates. American Journal of Psychiatry, 165, 969–977. doi:10.1176/appi.ajp.2008.08050721
Beevers, C. G., Clasen, P., Stice, E., & Schnyer, D. (2010). Depression symptoms and cognitive control of emotion cues: A functional magnetic resonance imaging study. Neuroscience, 167, 97–103. doi:10.1016/j.neuroscience.2010.01.047
Browning, M., Holmes, E. A., & Harmer, C. J. (2010). The modification of attentional bias to emotional information: A review of the techniques, mechanisms, and relevance to emotional disorders. Cognitive, Affective, & Behavioral Neuroscience, 10, 8–20. doi:10.3758/CABN.10.1.8
Brugha, T., Bebbington, P., Tennant, C., & Hurry, J. (1985). The List of Threatening Experiences—A subset of 12 life event categories with considerable long-term contextual threat. Psychological Medicine, 15, 189–194.
Costafreda, S. G., Brammer, M. J., David, A. S., & Fu, C. H. Y. (2008). Predictors of amygdala activation during the processing of emotional stimuli: A meta-analysis of 385 PET and fMRI studies. Brain Research Reviews, 58, 57–70. doi:10.1016/j.brainresrev.2007.10.012
Cremers, H. R., Demenescu, L. R., Aleman, A., Renken, R., van Tol, M. J., van der Wee, N. J., & Roelofs, K. (2010). Neuroticism modulates amygdala-prefrontal connectivity in response to negative emotional facial expressions. NeuroImage, 49, 963–970. doi:10.1016/j.neuroimage.2009.08.023
Cromheeke, S., & Mueller, S. C. (2014). Probing emotional influences on cognitive control: An ALE meta-analysis of cognition emotion interactions. Brain Structure and Function, 219, 995–1008. doi:10.1007/s00429-013-0549-z
De Raedt, R., & Koster, E. H. W. (2010). Understanding vulnerability for depression from a cognitive neuroscience perspective: A reappraisal of attentional factors and a new conceptual framework. Cognitive, Affective, & Behavioral Neuroscience, 10, 50–70. doi:10.3758/CABN.10.1.50
Demenescu, L. R., Renken, R., Kortekaas, R., van Tol, M. J., Marsman, J. B. C., van Buchem, M. A., & Aleman, A. (2011). Neural correlates of perception of emotional facial expressions in out-patients with mild-to-moderate depression and anxiety: A multicenter fMRI study. Psychological Medicine, 41, 2253–2264. doi:10.1017/S0033291711000596
Disner, S. G., Beevers, C. G., Haigh, E. A. P., & Beck, A. T. (2011). Neural mechanisms of the cognitive model of depression. Nature Reviews Neuroscience, 12, 467–477. doi:10.1038/nrn3027
Drevets, W. C., & Savitz, J. (2008). The subgenual anterior cingulate cortex in mood disorders. CNS Spectrums, 13, 663–681.
Glashouwer, K. A., & de Jong, P. J. (2010). Disorder-specific automatic self-associations in depression and anxiety: Results of the Netherlands study of depression and anxiety. Psychological Medicine, 40, 1101–1111. doi:10.1017/S0033291709991371
Greenberg, A. S., Esterman, M., Wilson, D., Serences, J. T., & Yantis, S. (2010). Control of spatial and feature-based attention in frontoparietal cortex. Journal of Neuroscience, 30, 14330–14339. doi:10.1523/JNEUROSCI.4248-09.2010
Groenewold, N. A., Opmeer, E. M., de Jonge, P., Aleman, A., & Costafreda, S. G. (2013). Emotional valence modulates brain functional abnormalities in depression: Evidence from a meta-analysis of fMRI studies. Neuroscience & Biobehavioral Reviews, 37, 152–163. doi:10.1016/j.neubiorev.2012.11.015
Hamani, C., Mayberg, H., Stone, S., Laxton, A., Haber, S., & Lozano, A. M. (2011). The subcallosal cingulate gyrus in the context of major depression. Biological Psychiatry, 69, 301–308. doi:10.1016/j.biopsych.2010.09.034
Hammen, C. (2005). Stress and depression. Annual Review of Clinical Psychology, 1, 293–319. doi:10.1146/annurev.clinpsy.1.102803.143938
Harmer, C. J., Goodwin, G. M., & Cowen, P. J. (2009). Why do antidepressants take so long to work? A cognitive neuropsychological model of antidepressant drug action. British Journal of Psychiatry, 195, 102–108. doi:10.1192/bjp.bp.108.051193
Kerestes, R., Ladouceur, C. D., Meda, S., Nathan, P. J., Blumberg, H. P., Maloney, K., & Phillips, M. L. (2012). Abnormal prefrontal activity subserving attentional control of emotion in remitted depressed patients during a working memory task with emotional distracters. Psychological Medicine, 42, 29–40. doi:10.1017/S0033291711001097
Kessler, R. C., & Ustun, T. B. (2004). The world mental health (WMH) survey initiative version of the world health organization (WHO) composite international diagnostic interview (CIDI). International Journal of Methods in Psychiatric Research, 13, 93–121.
Kircanski, K., Joormann, J., & Gotlib, I. H. (2012). Cognitive aspects of depression. Wiley Interdisciplinary Reviews: Cognitive Science, 3, 301–313. doi:10.1002/wcs.1177
Kriegeskorte, N., Lindquist, M. A., Nichols, T. E., Poldrack, R. A., & Vul, E. (2010). Everything you never wanted to know about circular analysis, but were afraid to ask. Journal of Cerebral Blood Flow & Metabolism, 30, 1551–1557. doi:10.1038/jcbfm.2010.86
Kriegeskorte, N., Simmons, W. K., Bellgowan, P. S. F., & Baker, C. I. (2009). Circular analysis in systems neuroscience: the dangers of double dipping. Nature Neuroscience, 12(5), 535-540. doi:10.1038/nn.2303
Lau, M., Segal, Z., & Williams, J. (2004). Teasdale’s differential activation hypothesis: Implications for mechanisms of depressive relapse and suicidal behaviour. Behaviour Research and Therapy, 42, 1001–1017. doi:10.1016/j.brat.2004.03.003
Lindquist, K. A., Wager, T. D., Kober, H., Bliss-Moreau, E., & Barrett, L. F. (2012). The brain basis of emotion: A meta-analytic review. Behavioral and Brain Sciences, 35, 121–143. doi:10.1017/S0140525X11000446
Lisiecka, D. M., Carballedo, A., Fagan, A. J., Ferguson, Y., Meaney, J., & Frodl, T. (2013). Recruitment of the left hemispheric emotional attention neural network in risk for and protection from depression. Journal of Psychiatry and Neuroscience, 38, 117–128. doi:10.1503/jpn.110188
Lundqvist, D., Flykt, A., & Ohmann, A. (1998). The Karolinska Directed Emotional Faces (KDEF) [Database]. Stockholm, Sweden: Karolinska Institute.
Mannie, Z. N., Taylor, M. J., Harmer, C. J., Cowen, P. J., & Norbury, R. (2011). Frontolimbic responses to emotional faces in young people at familial risk of depression. Journal of Affective Disorders, 130, 127–132. doi:10.1016/j.jad.2010.09.030
Matthews, S., Simmons, A., Strigo, I., Gianaros, P., Yang, T., & Paulus, M. (2009). Inhibition-related activity in subgenual cingulate is associated with symptom severity in major depression. Psychiatry Research: Neuroimaging, 172, 1–6. doi:10.1016/j.pscychresns.2008.08.006
Monroe, S., & Simons, A. (1991). Diathesis stress theories in the context of life stress research—Implications for the depressive-disorders. Psychological Bulletin, 110, 406–425. doi:10.1037/0033-2909.110.3.406
Norbury, R., Selvaraj, S., Taylor, M. J., Harmer, C., & Cowen, P. J. (2010). Increased neural response to fear in patients recovered from depression: A 3T functional magnetic resonance imaging study. Psychological Medicine, 40, 425–432. doi:10.1017/S0033291709990596
Pearlin, L., & Schooler, C. (1978). Structure of coping. Journal of Health and Social Behavior, 19, 2–21. doi:10.2307/2136319
Penninx, B. W., Beekman, A. T., Smit, J. H., Zitman, F. G., Nolen, W. A., Spinhoven, P., . . . NESDA Research Consortium. (2008). The Netherlands Study of Depression and Anxiety (NESDA): Rationale, objectives and methods. International Journal of Methods in Psychiatric Research, 17, 121–140. doi:10.1002/mpr.256
Phillips, M. L., Ladouceur, C. D., & Drevets, W. C. (2008). A neural model of voluntary and automatic emotion regulation: Implications for understanding the pathophysiology and neurodevelopment of bipolar disorder. Molecular Psychiatry, 13, 833–857. doi:10.1038/mp.2008.65
Ray, R. D., Ochsner, K. N., Cooper, J. C., Robertson, E. R., Gabrieli, J. D. E., & Gross, J. J. (2005). Individual differences in trait rumination and the neural systems supporting cognitive reappraisal. Cognitive, Affective, & Behavioral Neuroscience, 5, 156–168. doi:10.3758/CABN.5.2.156
Rive, M. M., van Rooijen, G., Veltman, D. J., Phillips, M. L., Schene, A. H., & Ruhe, H. G. (2013). Neural correlates of dysfunctional emotion regulation in major depressive disorder: A systematic review of neuroimaging studies. Neuroscience & Biobehavioral Reviews, 37, 2529–2553. doi:10.1016/j.neubiorev.2013.07.018
Roiser, J. P., Elliott, R., & Sahakian, B. J. (2012). Cognitive mechanisms of treatment in depression. Neuropsychopharmacology, 37, 117–136. doi:10.1038/npp.2011.183
Rush, A. J., Gullion, C. M., Basco, M. R., Jarrett, R. B., & Trivedi, M. H. (1996). The Inventory of Depressive Symptomatology (IDS): Psychometric properties. Psychological Medicine, 26, 477–486.
Scher, C., Ingram, R., & Segal, Z. (2005). Cognitive reactivity and vulnerability: Empirical evaluation of construct activation and cognitive diatheses in unipolar depression. Clinical Psychology Review, 25, 487–510. doi:10.1016/j.cpr.2005.01.005
Schulz, K. P., Clerkin, S. M., Halperin, J. M., Newcorn, J. H., Tang, C. Y., & Fan, J. (2009). Dissociable neural effects of stimulus valence and preceding context during the inhibition of responses to emotional faces. Human Brain Mapping, 30, 2821–2833. doi:10.1002/hbm.20706
Struijs, S. Y., Groenewold, N. A., Oude Voshaar, R. C., & de Jonge, P. (2013). Cognitive vulnerability differentially predicts symptom dimensions of depression. Journal of Affective Disorders, 151, 92–99. doi:10.1016/j.jad.2013.05.057
Stuhrmann, A., Suslow, T., & Dannlowski, U. (2011). Facial emotion processing in major depression: A systematic review of neuroimaging findings. Biology of Mood & Anxiety Disorders, 1, 10. doi:10.1186/2045-5380-1-10
Thomas, E. J., Elliott, R., McKie, S., Arnone, D., Downey, D., Juhasz, G., & Anderson, I. M. (2011). Interaction between a history of depression and rumination on neural response to emotional faces. Psychological Medicine, 41, 1845–1855. doi:10.1017/S0033291711000043
Van der Does, W. (2002). Cognitive reactivity to sad mood: Structure and validity of a new measure. Behaviour Research and Therapy, 40, 105–120. doi:10.1016/S0005-7967(00)00111-X
Van der Does, A. J. W., & Williams, J. M. G. (2003). Leiden Index of Depression Sensitivity–Revised (LEIDS-R) [Database]. Leiden, The Netherlands: Leiden University.
Vanderhasselt, M., Kuehn, S., & De Raedt, R. (2011). Healthy brooders employ more attentional resources when disengaging from the negative: An event-related fMRI study. Cognitive, Affective, & Behavioral Neuroscience, 11, 207–216. doi:10.3758/s13415-011-0022-5
Wolfensberger, S. P. A., Veltman, D. J., Hoogendijk, W. J. G., Boomsma, D. I., & de Geus, E. J. C. (2008). Amygdala responses to emotional faces in twins discordant or concordant for the risk for anxiety and depression. NeuroImage, 41, 544–552. doi:10.1016/j.neuroimage.2008.01.053
Zhong, M., Wang, X., Xiao, J., Yi, J., Zhu, X., Liao, J., & Yao, S. (2011). Amygdala hyperactivation and prefrontal hypoactivation in subjects with cognitive vulnerability to depression. Biological Psychology, 88, 233–242. doi:10.1016/j.biopsycho.2011.08.007
Author note
We are very grateful for the contributions of all the participants and the staffs of the participating institutions. The infrastructure for the NESDA study (available at www.nesda.nl) is funded, in part, by the Geestkracht program of the Netherlands Organization for Health Research and Development (ZonMw, Grant 10-000-1002) and is supported, in part, by the participating universities and mental health care organizations: VU University Medical Center, GGZ inGeest, Arkin, Leiden University Medical Center, GGZ Rivierduinen, University Medical Center Groningen, Lentis, GGZ Friesland, GGZ Drenthe, the Scientific Institute for Quality of Health Care (IQ Healthcare), the Netherlands Institute for Health Services Research (NIVEL), and the Netherlands Institute of Mental Health and Addiction (Trimbos). N.A.G. was partly supported by a personal grant from the Gratama Stichting. The authors do not have any potential conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplement 1
(DOC 37 kb)
Rights and permissions
About this article
Cite this article
Groenewold, N.A., Roest, A.M., Renken, R.J. et al. Cognitive vulnerability and implicit emotional processing: imbalance in frontolimbic brain areas?. Cogn Affect Behav Neurosci 15, 69–79 (2015). https://doi.org/10.3758/s13415-014-0316-5
Published:
Issue Date:
DOI: https://doi.org/10.3758/s13415-014-0316-5