Abstract
Objective: Clinical experience suggests important differences in prescriptions from general practitioners and specialists. This study investigated these differences and their determinants for antidepressant drug prescribing intentions by general practitioners and psychiatrists in France.
Study Participants: In May 1995, a mail questionnaire was sent to a representative panel of 300 general practitioners and 100 psychiatrists from the Midi-Pyrenees area (South West France). Two types of questions were asked: the first concerned the type of antidepressants prescribed according to the characteristics of depression (‘severe’, with insomnia, anxiety, etc.) and the second, the factors influencing prescriptions (personal experience, adverse effects, clinical trials, cost, etc.).
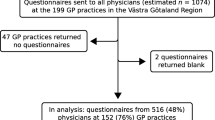
Results: 151 general practitioners (51%) and 63 psychiatrists (63%) answered the questionnaire. The analysis showed large differences between the two groups of physicians. Serotoninergic antidepressants were reported to be the most common first-line drugs of choice in both groups of practitioners. General practitioners claimed to prescribe serotoninergic antidepressants more frequently than psychiatrists (74 vs 59%, p < 0.05). Psychiatrists were reported to prescribe higher dosages of antidepressants than general practitioners in ‘severe’ depression (109.7 vs 85.6mg daily, p < 0.001). General practitioners were reported to prescribe anxiolytic agents more frequently than psychiatrists (73 vs 54%, p < 0.05), and neuroleptic agents less frequently (1 vs 11%, p < 0.001). The factors reported to influence antidepressant prescription differed in the two groups of physicians. Postuniversity teaching, hospital specialist information and registered indication were considered more important by general practitioners than psychiatrists, who reported to be more influenced by patients’ and colleagues’ opinions.
Conclusion: These results demonstrated that the differences in intention in prescribing between psychiatrists and general practitioners can be explained by a different approach to prescription since psychiatrists place more importance on human and clinical factors (patients’ and colleagues’ opinions) than general practitioners, who referred more to ‘official’ data (university, hospital and registered indications).
Similar content being viewed by others
References
Montastruc JL, Llau ME, Schmitt L, et al. Ordonnance du psychiatre, ordonnance du généraliste: approche pharmaco-épidémiologique. Psychol Médicale 1995; 27 Special 2: 118–21
Nau JY. Consumption of psychotropics in France. Lancet 1994; 343: 1152
Gerard PE, Dagens V, Deslandes A. 1960–2000:40 ans d'utilisation des antidépresseurs. Sem Hôp Paris 1995; 71: 727–34
Cialdella PH, Figon G, Boissel JP. Information thérapeutique et intention de prescription: une étude auprès de 117 médecins généralistes français de la région rhône-alpes. In: Fondation Marcel Nériuex, editor. Pharmacoépidémiologie, prescription et utilisation des médicaments. 1992 Cinquiémes entretiens du Centre Jacques Cartier. Montréal
Isacsson G, Redfars I, Wasserman D, et al. Choice of antide-pressants: questionnaire survey of psychiatrists and general practitioners in two areas of Sweden. BMJ 1994; 309: 1546–9
Song F, Freemantle N, Sheldon TA, et al. Selective serotonin reuptake inhibitors: meta-analysis of efficacy and acceptability. BMJ 1993; 306: 683–7
Owens D. Benefits of new drugs are exaggerated. BMJ 1994; 309: 1281–2
Anderson IM, Tomenson BM. The efficacy of selective serotonin reuptake inhibitors in depression: a meta-analysis of studies against tricyclic antidepressants. J Psychopharmacol 1994; 8: 238–49
Anderson IM, Tomenson BM. Treatment discontinuation with selective serotonin reuptake inhibitors compared with tricyclic antidepressants: a meta-analysis. BMJ 1995; 310: 1433–8
Montgomery SA, Kasper S. Comparison of compliance between serotonin reuptake inhibitors and tricyclic antidepressants: a meta-analysis. Int Clin Psychopharmacol 1995; 9: 33–40
Henry JA, Alexander CA, Sener EK. Relative mortality from overdose of antidepressants. BMJ 1995; 310: 221–4
Mackay FJ, Dunn NR, Wilton LV, et al. A comparison of fluvoxamine, fluoxetine, sertraline and paroxetine examined by observational cohort studies. Pharmacoepidemiol Drug Saf 1997; 6: 235–46
Sporer KA. The serotonin syndrome: implicated drugs, patho-physiology and management. Drug Saf 1995; 13: 94–105
Oolfson M, Klerman GL. Trends in the prescription of antide-pressants by office-based psychiatrist. Am J Psychiatry 1993; 150: 571–7
Rouillon F, Blachier C, Dreyfus JP, et al. Etude pharmaco-épidémiologique de la consommation des antidépresseurs en population générale. Encéphale 1996; 22: S39–S48
Anonyme. Benzodiazepines-antidépresseurs: un couple difficile. Med Hyg 1994; 52: 1496
Medawar C. The antidepressant web. Marketing depression and waking medicines work. Int JRiskSaf Med 1997; 10: 75–125
Paykel ES, Priest RG. Recognition and management of depression in general practice: consensus statement. BMJ 1992; 305: 1198–202
Kerr MP. Antidepressant prescribing: a comparison between general practitioners and psychiatrits. Br J Gen Pract 1994; 44: 275–6
Matthews K, Eagles JM, Matthews CA. The use of antidepressant drugs in general practice. A questionnaire survey. Eur J Clin Pharmacol 1993; 45: 205–10
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Lapeyre-Mestre, M., Desboeuf, K., Aptel, I. et al. A Comparative Survey of Antidepressant Drug Prescribing Habits of General Practitioners and Psychiatrists. Clin. Drug Investig. 16, 53–61 (1998). https://doi.org/10.2165/00044011-199816010-00007
Published:
Issue Date:
DOI: https://doi.org/10.2165/00044011-199816010-00007