Abstract
Globally, carcinomas of the anogenital tract, in particular cervical cancer, remain some of the most common cancers in women, cervical cancer represents the second most frequent gynecological malignancy and the third leading cause of cancer-related death in women worldwide. The causal relationship between human papillomavirus (HPV) infection and anogenital cancer has prompted substantial interest in the development of both preventive and therapeutic vaccines against high-risk HPV types. In the past decade, several groups have shown encouraging results using experimental vaccination systems in animal models and these results have led to several current prophylactic and therapeutic vaccine clinical trials in humans.
Prophylactic vaccination focuses on the induction of high titer neutralizing antibodies that are potentially protective against incident and persistent HPV infection. Two major phase II clinical trials conducted by pharmaceutical companies have demonstrated that their vaccines have 100% efficacy in preventing persistent viral DNA and its associated cellular abnormalities; however, whether they induce long-lasting protective immunity is yet to be determined. At least one US FDA approved prophylactic vaccine targeting the two most common high-risk HPVs is expected to be on the market within the next 2–3 years. Nevertheless, significant reductions in the frequency and onset of cytologic screening and incidences of HPV-related lesions are not expected to become apparent for decades due to the fact that there will be women who are already infected with HPV, the long latency period between infection and development of high-grade lesions, and lesions associated with other high-risk HPV types not being included in the vaccines. Therapeutic vaccines aim to control HPV-associated malignancies by stimulating cellular immune responses that target established HPV infections via viral proteins. Progress in the field of HPV immunotherapy has remained elusive, with clinical trials being limited to small numbers of patients.
Potential treatment of precancerous lesions is unique to HPV-associated infection and cancer because of cytologic monitoring and HPV typing. Unlike more common surgical treatments for cervical lesions, active immunotherapy has the potential to address HPV persistence as the cause of lesion development in addition to leaving the patient with long-term immunity that can be reactivated if and when the patient becomes reinfected.
Similar content being viewed by others
Cervical cancer remains one of the leading causes of cancer-related death among women worldwide, with nearly 500 000 newly diagnosed cases each year resulting in approximately 250 000 deaths.[1–3]The prevalence of combined incident low-grade squamous intraepithelial lesions (SILs), which are an indication of human papillomavirus (HPV) infection, and high-grade SILs, which are the precursor of invasive cervical cancer, is approximately 1–2.5% within screened populations.[4–6]The widespread use of cervical cytological screening based on the Papanicolaou (Pap) smear test has resulted in a 70% decline in mortality from cervical cancer in developed countries with effective Pap-screening programs over the past 50 years.[7]However, in developing countries where screening programs are minimal, cervical cancer remains the second leading cause of cancer-related deaths among women, following breast cancer.[2]
Cancer development is a multi-step process, involving dysregulation of the cell cycle and genomic instability, which can be brought about by genetic mutations and carcinogenic co-factors. However, it is well established that HPV is the etiological agent and persistent HPV infection is a necessary cause for the development of both high-grade cervical lesions and cervical cancer.[8,9]Following infection of basal epithelial cells in the transformation zone of the cervix, the virus genome directs the host cell to produce new infectious virus particles. In a small percentage of cases, the genome of the virus integrates into the host chromosome, ultimately leading to the growth of malignant tumors.
The involvement of HPV in oncogenesis has been extensively studied. The early proteins E6 and E7 are necessary for the development of epithelial cell transformation and the maintenance of the transformed state, as they delay keratinocyte differentiation and stimulate cell cycle progression, in part by binding to and inactivating the tumor suppressor gene products p53 and pRb, respectively.[10,11]E6 and E7 are expressed in low levels in proliferating basal cells, but are expressed at higher levels in transformed cells,[12,13]making them excellent targets for HPV-specific immunotherapy. Importantly, expression of the oncoproteins is required for maintenance of the transformed state[14]and is not likely to be lost as a result of immunological pressures.
Although most HPV infections are benign, persistent infection with high-risk types is associated with the development of cervical and other anogenital cancers. Fifteen HPV types are now classified as high-risk types (HPV16, 18, 31, 33, 35, 39, 45, 51, 52, 56, 58, 59, 68, 73, and 82); three are classified as probable high-risk types (HPV26, 53, and 66); and 12 are classified as low-risk types (HPV6, 11, 40, 42, 43, 44, 54, 61, 70, 72, 81, and CP6108).[15]The low-risk genotypes are commonly detected in benign genital condylomas and low-grade SILs but are almost never found in invasive carcinomas.[16]HPV DNA of high-risk genotypes is detected in virtually all cases of cancer of the cervix, with HPV16 or HPV18 being found in almost 70% of HPV-positive biopsies, regardless of the geographical region in which the patient is residing.[9]Because of their high prevalence in cervical and anogenital lesions, HPV16 and HPV18 are the focus of almost all recent HPV therapeutic vaccine developments. However, the first and foremost strategy for preventing the development of cervical cancer is to prevent HPV infection.
1. Prophylactic Human Papillomavirus (HPV) Vaccines
Generation of Virus-Neutralizing Antibodies
The traditional approach for the prevention of cervical cancer has focused on screening women at risk for the disease using the Pap smear, and treating any precancerous lesions. While this approach has drastically reduced the incidence of cervical cancer in developed countries, underdeveloped countries that are unable to implement comprehensive screening-based programs have not been able to claim similar success. Because HPV is the etiological agent of cervical neoplasia, preventing infection with HPV will also prevent the development of cervical cancer. However, this approach for disease prevention presents greater challenges than prevention of most other sexually transmitted diseases. HPV is easily transmitted and has a high rate of penetrance in the population after the onset of sexual activity.[17,18]Infection often occurs without overt symptoms, and the virus can persist undetected in an individual for years.[17,19]Additionally, HPV virions of the high-risk types cannot be isolated from naturally occurring lesions. The viruses cannot be propagated in large enough quantities in either cell culture or animal systems to enable generation of the traditional heat-inactivated or attenuated virus vaccine. Therefore, development of an HPV-preventive vaccine has mostly focused on immunization of individuals with HPV virus-like particles (VLPs) in order to generate virus-neutralizing antibodies.
VLPs can be obtained by overexpression of the major capsid protein L1 alone, or by co-expression with the minor capsid protein L2.[20,21]HPV VLPs mimic infectious virions in structure and morphology[22,23]and in their ability to induce high titers of virus-neutralizing antisera, even without adjuvant.[20,24]Most neutralizing antibodies induced by intact virions or L1/L2 VLPs recognize type-specific conformational epitopes presented by the L1 molecule,[25–27]although L2 can also present some epitopes that induce the production of neutralizing antibodies.[28–30]Because VLPs do not contain any viral DNA and are non-infectious and non-oncogenic, they are the most attractive candidate for developing a prophylactic vaccine against genital HPV infection.
Infection with papillomaviruses is strictly species specific; therefore, the use of various animal papillomaviruses has allowed researchers to study and show proof of concept for the protective effects of papillomavirus vaccines. Several animal studies have indicated that humoral immunity is a key factor in preventing experimental infection with animal papillomaviruses.[31] Table I summarizes the data from phase I and phase II clinical trials using preventive HPV vaccines composed of L1 VLPs. Immunization with HPV6 VLPs, HPV11 VLPs, HPV16 VLPs, or HPV18 VLPs indicate that VLP vaccines given intramuscularly to healthy volunteers are well tolerated at various doses and elicit strong humoral immune responses. In four studies reporting responses after median follow-up durations of 17–36 months, vaccination with HPV16 and HPV18 VLPs was shown to prevent persistent HPV16 or HPV18 infection and development of SILs with 90–100% efficacy compared with placebo (table I). Two years after their initial report,[32]Merck & Company Inc. reported that 4 years after the initial vaccination with HPV16 VLPs, the effectiveness of the vaccine was still very high; only 0.9% of patients who received the vaccine developed persistent HPV16 infection compared with 14.8% of patients who received placebo, 1.6% of whom formed precancerous lesions.[33]Based on these data, several larger scale phase II and phase III clinical trials have been initiated to confirm and extend the initial efficacy findings. After reporting their equally promising HPV vaccine efficacy results[34]in May 2004 (table I), GlaxoSmithKline Biologicals in partnership with MedImmune announced the initiation of a phase III clinical trial. Approximately 13 000 young female volunteers will participate in the 4-year study aimed at evaluating the safety and efficacy of the bivalent HPV16 L1/HPV18 L1 VLP vaccine (MEDI-517), which is administered in AS04 adjuvant (aluminum hydroxide and 3-deacylated monophosphoryl lipid A).[35]In addition, Merck has enrolled 17 000 patients into its phase III clinical trial, which is to run until 2008. In this trial, vaccinees will receive a quadrivalent HPV vaccine administered in aluminum hydroxyl phosphate sulfate (alum) adjuvant; the genotypes encompassed in this vaccine are HPV6 and HPV11, the two low-risk types associated with genital warts, and HPV16 and HPV18, the two high-risk HPV types associated with the development of cervical and other anogenital lesions.[36]The quadrivalent vaccine is expected to reduce the risk of HPV infections, which lead to either genital warts in men and women or cervical cancer in women. A recently reported 3-year phase II clinical trial of Merck’s quadrivalent L1 VLP vaccine showed 100% efficacy at preventing clinical disease associated with HPV6, 11, 16, or 18 and 90% efficacy in preventing combined incident and persistent HPV6, 11, 16, or 18 infection.[37]The National Cancer Institute, in collaboration with GlaxoSmithKline, is also planning a large-scale HPV16/HPV18 VLP clinical trial outside of the US.[38]
The true efficacy of HPV L1 vaccines in preventing HPV infection and the clinical disease associated with this will only be realized after many more years of post-vaccination follow-up. While the three clinical trials measuring efficacy were able to demonstrate that their vaccines were 100% effective at preventing persistent HPV infection as measured by the detection of HPV DNA, only one[46]reported no instances of intermittent HPV infection. In the studies by Harper et al.[34]and Koutsky et al.,[32]both reported a lower incidence, but not total prevention, of transient cervical infection in their vaccine groups; the vaccine efficacy for incident infection was approximately 90% in both studies. However, it remains unclear whether the detection of HPV DNA represented true productive infections or a recent encounter with an infected partner. In addition, women that did not complete the vaccination regimen were not as protected as women that received all three doses of the vaccine,[34]suggesting that, if this vaccine is implemented amongst the general public, it will be very important to ensure patient compliance in receiving all vaccine boosters or patients will risk being insufficiently protected.
Another potential hurdle with these vaccines is their limitations for protection against other HPV genotypes. The neutralizing antibodies made against VLPs of a certain genotype are remarkably type specific and do not cross-neutralize one another, except for a limited number of very closely related genotypes.[48]An example of this occurred in one clinical trial in which cases of HPV18 infection were found in patients who had received either an HPV16 or an HPV11 vaccine.[46]Infection with HPV18 was shown to be indifferent to these vaccinations, since there were comparable incidences of HPV18 infection amongst the vaccine and placebo groups. In women who were vaccinated with HPV16 VLPs alone, there were also cases of non-HPV16-associated cervical intraepithelial neoplasia (CIN), which were equally divided between the vaccinated and placebo groups.[32]This indicates that vaccination with VLPs in humans will follow that seen in animal models, in that protection will be type specific, thus creating the need for vaccines that are multivalent (i.e. that contain multiple HPV VLP types). Theoretically, a vaccine containing seven of the most oncogenic HPV types could potentially prevent 87% of cervical cancers with little geographical variation.[49]However, creating one vaccine with many HPV types may be logistically problematic. It is unknown what quantity of one HPV VLP type is required to induce long-term protection, and whether the magnitude of the humoral response will be diminished for each HPV type in the same vaccine if there are too many different dominant immune epitopes given at once, resulting in competition between antigens. Merck’s phase II trial with their quadrivalent vaccine showed that antibody titers to HPV16 were indeed dominant compared with the other three HPV types included in the vaccine.[37]At 36 months, the antibody titers to HPV6, 16, and 18 in vaccinated patients had diminished but were still above those seen in the placebo group. Importantly, the mean antibody titer to HPV11 was not significantly different from that of the placebo group, indicating that booster doses might be needed over time in order to maintain seropositivity.[37]
All of the prophylactic clinical trial results indicate an almost universal induction of very high serum antibody titer levels that are 40–60 times higher than those induced by natural infection and persist over many months to years with only a slight decline in antibody levels.[32,34,39,44]Preliminary data indicate that the HPV VLP vaccines formulated in AS04 adjuvant induce substantially higher and more persistent antibody levels compared with aluminum-only formulations.[50]More promising is the finding that vaccination also induces local mucosal immunity in the cervix of immunized women in the form of IgG and secretory IgA. One study reported that, in a small group of women analyzed who had received the HPV16 VLP vaccine, all participants developed cervical anti-HPV16 antibodies, regardless of their immunization schedule.[51]One caveat was that HPV16 VLP immunization resulted in specific antibody levels in the human genital tract that varied amongst women who had natural ovulatory cycles, with a significant decrease in antibody titer around ovulation, compared with antibody levels that did not vary amongst women taking oral contraceptives.[51]These data indicate that the titer of anti-HPV16 antibodies at the cervix is promising in terms of vaccine efficacy, but it also raises the possibility that a VLP vaccine might be less effective during some phases of the menstrual cycle. In another study, which also investigated anti-HPV antibodies in cervical secretions, detectable anti-HPV11 antibodies could only be found in 24–52% of participants who received an HPV11 vaccine. More importantly, detectable anti-HPV16 antibodies could only be found in 5–10% of participants who received an HPV16 vaccine.[45]Although the observations were disappointing, the authors pointed out that they did not take into account menstrual cycle-associated variations in antibody levels, which could have affected the results, in addition to the large dilution factor as a result of cervicovaginal lavage procedures. Assuming that vaccine-induced antibodies to HPV in cervicovaginal secretions are an important mechanism of the vaccine’s protective effects, antibody levels during ovulation would have to drop below the level required for maintenance of the protective effects of the vaccine to result in a significant decrease in protection from HPV infection. It is unknown what antibody levels are required for prevention of incident or persistent infection and it is unknown which antibodies play a critical role in protective efficacy (i.e. IgA and IgG found in cervical secretions vs basal cell-associated IgG from extravasated blood). Therefore, a larger study with longer follow-up is necessary in order to fully determine the effects of ovulation-suppressing contraceptives on vaccine efficacy, whether the level of HPV-specific antibody persists over decades, and whether booster vaccinations will be needed.[52]
Ideally, vaccination against HPV16 and HPV18 will lead to a significant reduction in the worldwide incidence of cervical cancer. However, there is concern that widespread vaccination with HPV16 and HPV18 may lead to the emergence and spread of some of the less common oncogenic high-risk HPV types. A case for viral variant emergence is exemplified by the epidemic of acute respiratory disease (ARD) in the US military, where sporadic outbreaks of ARD caused by the less prevalent adenovirus types 3 and 21 emerged following vaccination with ADV types 4 and 7 vaccines.[53]At least 30% of cervical cancers are caused by HPV genotypes other than HPV16 and HPV18.[9]These other high-risk oncogenic HPV types are less likely to persist compared with HPV16 and, therefore, are less likely to cause progression of disease.[54]However, they still remain a threat since antibodies against HPV are largely type specific.
No animal exists in which the sexual transmission of papillomavirus to the cervix can readily be tested. Therefore, many unresolved issues surrounding the efficacy of parenteral vaccination with HPV VLPs against HPV infection and lesion development cannot be addressed experimentally. It will be difficult to make an estimate of vaccination efficacy against clinical disease based on vaccination efficacy against HPV infection, because HPV-induced clinical disease occurs only in a small percentage of infected individuals. Clinical disease must be shown to be attributable to the specific HPV type present in the vaccine before a conclusion can be drawn about protection, especially since there is already evidence from the HPV trials that protection will be type specific and probably will not have an impact on infection rates by other high-risk HPV types. Elimination of the most prevalent HPV types is expected to affect clinical management of HPV-associated disease over time by reducing the number of women with abnormal Pap tests, thereby reducing the number who must undergo further testing and treatment, such as colposcopy, biopsy, and surgical removal of premalignant lesions.[55,56]This reduction is not likely to occur for 10–25 years, when the intended vaccinees (adolescents) would normally present with abnormal cytology. In addition, mathematical models suggest that a 50% reduction in the rate of cervical cancer incidence is estimated to take 25–55 years, assuming that 75% of females are vaccinated and protected against HPV16 alone.[57]Screening practices in developed countries will not, therefore, change significantly for the present time. Women in countries without vigorous screening programs might benefit the most from vaccination, since 50% of cervical cancers occur in women who do not attend screenings or who are not screened on a regular basis for premalignant lesions.[58]
Prophylactic vaccines might be able to prevent infection with high-risk HPV if delivered to young women before exposure to the virus. Merck plan to seek US FDA approval for their quadrivalent vaccine in 2006; they plan to take the vaccine to market soon thereafter, which would mean a preventive cervical cancer vaccine could be available within 2–3 years.[59]Even after vaccine implementation, assuming that it would be widespread, a reduction in the incidence of cervical cancer is not expected to become apparent for more than a decade, since it generally takes this long or longer for incident HPV infection to progress to cancer.[38]It is estimated that a vaccine that prevents 98% of persistent HPV16/18 will be associated with an approximate equivalent reduction in HPV16/18-associated cancer and a 51% reduction in total cervical cancer.[55]A vaccine that prevents 75% of persistent HPV16/18 infection will be associated with a 70–83% reduction in HPV16/18-associated cancer cases. The effect on total cervical cancer prevalence will likely be attenuated because of cancers associated with other oncogenic non-HPV16 and 18 types. Therefore, a prophylactic vaccine that prevents persistent HPV16/18 infection can be expected to significantly reduce the frequency of HPV16/18-associated low-grade SILs, high-grade SILs, and cervical cancer. However, the impact on overall prevalence of HPV or low-grade SILs may be minimal.[55]Cost analysis modeling has nevertheless shown that vaccination for HPV in combination with delayed screening and screening at less frequent intervals can be more cost effective as an overall health intervention compared with screenings alone.[60]Assuming that prophylactic vaccination were to begin immediately, worldwide there would still be an estimated 10 million women diagnosed with cervical cancer and 5 million cervical cancer deaths over the next 20 years as a consequence of existing HPV infection.[2]There exists, therefore, a compelling case for developing therapeutic vaccines for existing and breakthrough HPV infections, as virus-specific immunotherapy has the potential to have an immediate impact on the incidence of cervical cancer.
2. Therapeutic HPV Vaccines
Activation of the Cellular Immune Response
Cellular immunity, especially activation of antigen-specific CD4+ and CD8+ T lymphocytes, is most likely the critical defense mechanism against HPV-infected cells.[61]Several lines of evidence support the importance of the cellular immune system in the pathogenesis of HPV-associated cervical lesions. More than 60% of HPV-positive SILs are eliminated after local biopsy or resolve spontaneously,[62,63]suggesting that induction of local inflammation and recruitment of white blood cells may be involved with the regression of lesions. Immunodeficiency is associated with an increased prevalence of HPV infection. For example, genetically immunosuppressed individuals, AIDS patients, and immunosuppressed renal transplant patients all have an increased risk of HPV-associated malignancies compared with the general immunocompetent population.[64–67]Immunohistochemical studies on cervical carcinomas have demonstrated high levels of predominantly CD8+ T lymphocytes in cellular infiltrates.[68]Additionally, mononuclear cell infiltrates comprising macrophages, CD4+, and CD8+ T lymphocytes can be found in regressing HPV-associated skin and genital warts in the majority of patients, suggesting that immune responses to HPV may be a component of the regression of the disease.[69–71]In a study of women who had been repeatedly infected with the same HPV type, it was found that all subjects were able to clear the viral DNA rapidly following the second detection of HPV DNA, suggesting the presence of immunological memory.[72]
Various forms of HPV vaccines targeting the E6 and/or E7 proteins of the papillomaviruses have been described in experimental systems using animal models and transplantable HPV-induced tumors.[73,74]These strategies include polynucleotide-based vaccines,[75–77]peptide-based vaccines,[78]protein-based vaccines,[79–81]viral[82,83]and bacterial[84]vector-based vaccines, chimeric VLP-based vaccines,[85,86]and cell-based vaccines.[87–89]Several of these types of immunotherapeutic strategies have been tested in phase I and phase II clinical trials for anogenital cancers and their preceding premalignant lesions (table II). In general, the trials for cervical cancer intervention have been carried out in patients with late-stage disease who have already undergone surgery, radiotherapy, and/or chemotherapy with little to no clinical hope for remission. While immunotherapeutic intervention in end-stage patients has generally not led to any change in clinical outcome, these types of trials can still provide valuable information on the induction of specific immunity to papillomavirus early proteins in cancer-bearing patients. Possible reasons for the lack of clinical improvement in these patients include cancer-associated immunosuppressive mechanisms such as downregulation of or mutations in the MHC and TAP genes[90,91]and other potential immune evasion mechanisms that are attributable to HPV infection itself.[61,92]Recent unpublished reports have indicated that CD4+ T-regulatory cells that have immunosuppressive functions may be involved in local immune suppression in advanced cervical lesions[93]and tumor-draining lymph nodes in patients with cervical cancer.[94]The presence of suppressive T cells in cervical lesions might, therefore, be inhibiting both the CD8+ cytotoxic T lymphocytes and potentially cytotoxic CD4+ T cells, which are induced in patients who have been immunized with the various immunotherapeutic strategies for enhancing anti-HPV cellular immunity. Identification of these potential immune suppressive mechanisms can lead to further immune manipulation strategies to attempt to reverse these inhibitory processes.
There are many strengths and weaknesses surrounding the strategies being developed to treat cervical cancer. Among the highly immunogenic strategies are viral- and bacterial-based vectors and dendritic cell-based vaccines. However, there are many regulatory safety issues surrounding the vector-based vaccines, as well as the potential inability of subjects to mount a sufficient immune response to these vaccines because of pre-existing immunity to the virus or bacterial vector or an inability to boost the response after one vaccination. Dendritic cell vaccination requires custom-made, patient-specific, time-consuming, and costly procedures. It is particularly unlikely that dendritic cell-based therapies would be implemented either for women in developing countries who have no access to adequate screening programs or for women in developed countries who have access to more cost-effective standard surgical procedures. Peptide and protein-based vaccines are relatively easy to produce and there are generally no safety concerns because there is no genetic material included. The drawbacks are that peptide vaccines must match to the patient’s HLA type and are not as immunogenic as some of the other strategies, and that protein-based vaccines elicit better antibody than CTL responses. DNA-based vaccines are easy to produce, are very versatile in their ability to carry multiple targeting and costimulatory genes, and can be used in multiple immunizations. However, there are the major concerns of DNA integration and cell transformation, not to mention the introduction of potential oncogenes such as E6 and E7. Reasonable approaches to ensure that patients are not exposed to potentially oncogenic DNA and proteins when using gene-based vaccines include multiple-point mutations engineered into the oncogene sequences[116]or reorganization of blocks of sequences[117]that render the proteins nonfunctional. As patient safety is always the first priority, these issues must be adequately addressed before therapeutic vaccines can make a significant impact on cancer burden.
Trials of immunotherapy in patients with HPV-associated premalignant disease, where it has been presumed that induction of HPV-specific T cells after vaccination has resulted in some of the clinical regression of lesions observed, have been more informative (table II). Randomized controlled therapeutic trials are particularly difficult to implement because of the safety issue of leaving lesions untreated when a patient can be treated easily with a standard loop electrosurgical excision procedure (LEEP) or cryotherapy. Furthermore, therapeutic clinical trial results have not yet been able to provide, or even suggest, reasons why some patients have an immunological, but not a clinical, response to vaccination, and why other patients have a clinical response but no significant increases in HPV-specific T-cell immunity. Whereas the mechanism of action for the prevention of HPV infection is rather straightforward, the mechanisms that lead to the successful elimination of HPV-induced lesions are not defined and are far more complex than eliciting neutralizing antibodies. It is for this reason that the field of cancer immunotherapy is still lagging significantly behind that of prevention of virus infection. Immunotherapy of cancer outside of the field of HPV (e.g. melanoma, breast cancer, prostate cancer, lymphoma) has encountered similar problems, where promising preclinical model studies have not been able to predict which approaches will generate the most efficient and robust immune responses in cancer patients.[118]Future trials in HPV will likely include combining heterologous vaccination vehicles in the form of prime/boost strategies, which have shown great promise in preclinical murine models[119–121]and also in the limited clinical trials that have been performed[114,115](table II).
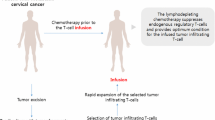
HPV immunotherapy strategies that may prove promising but are not yet available in the clinic include adoptive transfer of antigen-specific T cells[122,123]and viral vectors derived from RNA-based viruses such as the Venezuelan equine encephalitis virus[83,116]or Semliki Forest virus.[124]T-cell receptor (TCR) transfer technology, which encompasses retroviral transfer of genes encoding antigen-specific TCR into peripheral blood T cells of patients, has the potential to generate a bank of TCR genes with specificity to various viral tumor antigens that may be selected for in any patient with tumor cells expressing the appropriate antigen.[125,126]
The development of therapeutic vaccines for the clinical management of HPV-associated disease is not intended for late-stage cervical cancer but for patients who have precancerous lesions and who still have a chance that the disease will respond positively to immunotherapy. The majority of phase II clinical trials are now conducted in patients with earlier stage lesions such as CIN I/II/III or vulval intraepithelial neoplasia I/II/III. The ability to treat precancerous lesions is unique to HPV infection and associated cancers because of the histological changes and HPV status, which are monitored with Pap smears and associated HPV DNA typing. While current surgical treatments are generally effective and well tolerated, they do not address the cause of the problem; specifically HPV infection and viral persistence. Half of all patients that undergo LEEP surgery return to the clinic with either recurrent or new lesions.[127]The advantage of therapeutic vaccines over surgery is that active immunotherapy targets HPV proteins directly through the patient’s own immune system, leaving the patient with long-term immunity that can be reactivated if and when the patient becomes re-infected.
3. Conclusion
Advances in vaccine development for the prevention and treatment of cervical cancer have produced encouraging results in clinical trials over the past 5 years. The next 5–10 years will be particularly exciting because we should gain a clearer understanding of the protective effects of HPV VLP-based vaccines and to what extent the vaccines provide long-lasting protection, presuming that women vaccinated in the early trials will be monitored in follow-up studies. Prophylactic vaccines that target neutralizing epitopes in both L1 and L2, as well as combined prophylactic/therapeutic vaccines, are currently being developed, as are more effective therapeutic vaccines. The results from clinical HPV therapeutic vaccine trials provide an opportunity to identify the characteristics of the immune responses that best correlate with regression of HPV-associated lesions and provide data leading to the rational development of more effective vaccines. Understanding of the mechanisms that work against successful treatment, such as immune evasion or suppressive T cells, will allow for the design of vaccines that reverse these mechanisms. A direct comparison of these different types of vaccines will help identify the most potent therapeutic vaccine for a particular type of malignancy.
Although not without substantial issues that still need to be addressed, the current prophylactic clinical trials with HPV VLPs have generated widespread optimism that at least one US FDA-approved vaccine will be made available to the public in the next 2–3 years. Several important and complex implementation issues will need to be addressed before these vaccines can make a substantial public health contribution.[38]These issues include, but are not limited to, defining the population of people that should be vaccinated with a prophylactic vaccine; how cervical cancer screening programs should or should not be adjusted; how to implement effective vaccination and screening programs in developing countries; and generating enthusiasm and initiative for developing second-generation vaccines that may be more effective at accomplishing the ultimate goal of cancer burden reduction once the current vaccines are on the market.
The current target population for prophylactic vaccination is adolescent girls and boys. Parental acceptance of a vaccine that targets a sexually transmitted disease will likely vary depending upon their personal life experiences and attitudes.[128]Education about HPV, its transmission rate, its ubiquitousness, and its association with genital warts and cancer will also be important for increasing vaccine acceptability, in addition to strong recommendations from physicians and health agencies.[128,129]Because non-vaccinated or already infected girls and women in the population will still be at risk of HPV infection and/or development of lesions, clinical screening practices in developed countries should not and will not change significantly for decades. There is still a need for regular cytologic examination and triage based on high-risk HPV status for the current non-vaccinated population and this will continue until prophylactic vaccination is sufficiently widespread.[60,130]Even then, screening should never be totally eliminated because there is the risk of lesion development from other high-risk HPV types that are not included in the current vaccines.
It will take time and the continued efforts of both researchers and clinicians to realize the goal of delivering safe and effective preventive HPV vaccines to those who need it most and to be able to effectively treat those women who already have HPV infections and HPV-related disease. The consequences for clinical management in the case of prophylactic vaccines may include a significant reduction in the frequency and onset of cytologic screening and in the occurrence of high-grade intraepithelial lesions and related cancer; these consequences will likely become apparent in the next few decades assuming widespread vaccination is adopted. There will also hopefully be therapeutic vaccines that are just as effective as current treatment options, that are less invasive, and that target the cause of the problem, namely HPV persistence once infected. Global effective implementation of both prophylactic and therapeutic vaccine regimens could result in a significant reduction in both healthcare costs and worldwide cervical cancer incidence due to HPV infection.
References
Pisani P, Bray F, Parkin DM. Estimates of the world-wide prevalence of cancer for 25 sites in the adult population. Int J Cancer 2002; 97: 72–81
Parkin DM, Bray F, Ferlay J, et al. Global cancer statistics, 2002. CA Cancer J Clin 2005; 55: 74–108
Jemal A, Murray T, Samuels A, et al. Cancer statistics, 2003. CA Cancer J Clin 2003; 53: 5–26
Manos MM, Kinney WK, Hurley LB, et al. Identifying women with cervical neoplasia: using human papillomavirus DNA testing for equivocal papanicolaou results. JAMA 1999; 281: 1605–10
Chhieng DC, Elgert PA, Cangiarella JF, et al. Clinical significance of atypical glandular cells of undetermined significance: a follow-up study from an academic medical center. Acta Cytol 2000; 44: 557–66
Stoler MH. Advances in cervical screening technology. Mod Pathol 2000; 13: 275–84
Kurman RJ, Henson DE, Herbst AL, et al. Interim guidelines for management of abnormal cervical cytology. The 1992 National Cancer Institute Workshop. JAMA 1994; 271: 1866–9
Bosch FX, Lorincz A, Munoz N, et al. The causal relation between human papillomavirus and cervical cancer. J Clin Pathol 2002; 55: 244–65
Munoz N. Human papillomavirus and cancer: the epidemiological evidence. J Clin Virol 2000; 19: 1–5
Werness BA, Levine AJ, Howley PM. Association of human papillomavirus types 16 and 18 E6 proteins with p53. Science 1990; 248: 76–9
Dyson N, Howley PM, Munger K, et al. The human papilloma virus-16 E7 oncoprotein is able to bind to the retinoblastoma gene product. Science 1989; 243: 934–7
Durst M, Glitz D, Schneider A, et al. Human papillomavirus type 16 (HPV 16) gene expression and DNA replication in cervical neoplasia: analysis by in situ hybridization. Virology 1992; 189: 132–40
Crish JF, Bone F, Balasubramanian S, et al. Suprabasal expression of the human papillomavirus type 16 oncoproteins in mouse epidermis alters expression of cell cycle regulatory proteins. Carcinogenesis 2000; 21: 1031–7
vonKnebel DM, Rittmuller C, Aengeneyndt F, et al. Reversible repression of papillomavirus oncogene expression in cervical carcinoma cells: consequences for the phenotype and E6-p53 and E7-pRB interactions. J Virol 1994; 68: 2811–21
Munoz N, Bosch FX, deSanjose S, et al. Epidemiologic classification of human papillomavirus types associated with cervical cancer. N Engl J Med 2003; 348: 518–27
Stone KM. Human papillomavirus infection and genital warts: update on epidemiology and treatment. Clin Infect Dis 1995; 20Suppl. 1: S91–7
Ho GY, Bierman R, Beardsley L, et al. Natural history of cervicovaginal papillomavirus infection in young women. N Engl J Med 1998; 338: 423–8
Winer RL, Lee SK, Hughes JP, et al. Genital human papillomavirus infection: incidence and risk factors in a cohort of female university students. Am J Epidemiol 2003; 157: 218–26
Castle PE, Schiffman M, Herrero R, et al. A prospective study of age trends in cervical human papillomavirus acquisition and persistence in Guanacaste, Costa Rica. J Infect Dis 2005; 191: 1808–16
Kirnbauer R, Booy F, Cheng N, et al. Papillomavirus L1 major capsid protein self-assembles into virus-like particles that are highly immunogenic. Proc Natl Acad Sci U S A 1992; 89: 12180–4
Kirnbauer R, Taub J, Greenstone H, et al. Efficient self-assembly of human papillomavirus type 16 L1 and L1-L2 into virus-like particles. J Virol 1993; 67: 6929–36
Hagensee ME, Olson NH, Baker TS, et al. Three-dimensional structure of vaccinia virus-produced human papillomavirus type 1 capsids. J Virol 1994; 68: 4503–5
Chen XS, Garcea RL, Goldberg I, et al. Structure of small virus-like particles assembled from the L1 protein of human papillomavirus 16. Mol Cell 2000; 5: 557–67
Christensen ND, Hopfl R, DiAngelo SL, et al. Assembled baculovirus-expressed human papillomavirus type 11 L1 capsid protein virus-like particles are recognized by neutralizing monoclonal antibodies and induce high titres of neutralizing antibodies. J Gen Virol 1994; 75: 2271–6
Christensen ND, Kreider JW. Antibody-mediated neutralization in vivo of infectious papillomaviruses. J Virol 1990; 64: 3151–6
Roden RB, Greenstone HL, Kirnbauer R, et al. In vitro generation and type-specific neutralization of a human papillomavirus type 16 virion pseudotype. J Virol 1996; 70: 5875–83
White WI, Wilson SD, Bonnez W, et al. In vitro infection and type-restricted antibody-mediated neutralization of authentic human papillomavirus type 16. J Virol 1998; 72: 959–64
Roden RB, Weissinger EM, Henderson DW, et al. Neutralization of bovine papillomavirus by antibodies to L1 and L2 capsid proteins. J Virol 1994; 68: 7570–4
Kawana K, Matsumoto K, Yoshikawa H, et al. A surface immunodeterminant of human papillomavirus type 16 minor capsid protein L2. Virology 1998; 245: 353–9
Kawana Y, Kawana K, Yoshikawa H, et al. Human papillomavirus type 16 minor capsid protein 12 N-terminal region containing a common neutralization epitope binds to the cell surface and enters the cytoplasm. J Virol 2001; 75: 2331–6
Fausch SC, DaSilva DM, Eiben GL, et al. HPV protein/peptide vaccines: from animal models to clinical trials. Front Biosci 2003; 8: 81–91
Koutsky LA, Ault KA, Wheeler CM, et al. A controlled trial of a human papillomavirus type 16 vaccine. N Engl J Med 2002; 347: 1645–51
Maugh II, Thomas H. Vaccine blocks cervical cancer: study finds that most women treated were protected for four years from a virus strain that can cause the disease. Los Angeles Times 2004 Nov 2; Section: A10
Harper DM, Franco EL, Wheeler C, et al. Efficacy of a bivalent L1 virus-like particle vaccine in prevention of infection with human papillomavirus types 16 and 18 in young women: a randomised controlled trial. Lancet 2004; 364: 1757–65
GlaxoSmithKline News. Developing and launching novel medicines and vaccines [online]. Available from URL: http://www.worldwidevaccines.com/news/news_view_article.asp?.from=2&newsld=3071 [Accessed 2004 May 19]
Merck & Company Corporate News. PATRICIA: Trial launched of new vaccine aimed at preventing cervical cancer [online]. Available from URL: http://www.merck.com/newsroom/press_releases/corporate/2003_1209_print.html [Accessed 2004 May 19]
Villa LL, Costa RL, Petta CA, et al. Prophylactic quadrivalent human papillomavirus (types 6, 11, 16, and 18) L1 virus-like particle vaccine in young women: a randomised double-blind placebo-controlled multicentre phase II efficacy trial. Lancet Oncol 2005; 6: 271–8
Schiller JT, Davies P. Delivering on the promise: HPV vaccines and cervical cancer. Nat Rev Microbiol 2004; 2: 343–7
Harro CD, Pang YY, Roden RB, et al. Safety and immunogenicity trial in adult volunteers of a human papillomavirus 16 L1 virus-like particle vaccine. J Natl Cancer Inst 2001; 93: 284–92
Evans TG, Bonnez W, Rose RC, et al. A Phase 1 study of a recombinant viruslike particle vaccine against human papillomavirus type 11 in healthy adult volunteers. J Infect Dis 2001; 183: 1485–93
Emeny RT, Wheeler CM, Jansen KU, et al. Priming of human papillomavirus type 11-specific humoral and cellular immune responses in college-aged women with a virus-like particle vaccine. J Virol 2002; 76: 7832–42
Kawana K, Yasugi T, Kanda T, et al. Safety and immunogenicity of a peptide containing the cross-neutralization epitope of HPV16 L2 administered nasally in healthy volunteers. Vaccine 2003; 21: 4256–60
Pinto LA, Edwards J, Castle PE, et al. Cellular immune responses to human papillomavirus (HPV)-16 L1 in healthy volunteers immunized with recombinant HPV-16 L1 virus-like particles. J Infect Dis 2003; 188: 327–38
Ault KA, Giuliano AR, Edwards RP, et al. A phase I study to evaluate a human papillomavirus (HPV) type 18 L1 VLP vaccine. Vaccine 2004; 22: 3004–7
Fife KH, Wheeler CM, Koutsky LA, et al. Dose-ranging studies of the safety and immunogenicity of human papillomavirus type 11 and type 16 virus-like particle candidate vaccines in young healthy women. Vaccine 2004; 22: 2943–52
Brown DR, Fife KH, Wheeler CM, et al. Early assessment of the efficacy of a human papillomavirus type 16 L1 virus-like particle vaccine. Vaccine 2004; 22: 2936–42
Poland GA, Jacobson RM, Koutsky LA, et al. Immunogenicity and reactogenicity of a novel vaccine for human papillomavirus 16: a 2-year randomized controlled clinical trial. Mayo Clin Proc 2005; 80: 601–10
Roden RB, Hubbert NL, Kirnbauer R, et al. Assessment of the serological relatedness of genital human papillomaviruses by hemagglutination inhibition. J Virol 1996; 70: 3298–301
Munoz N, Bosch FX, Castellsague X, et al. Against which human papillomavirus types shall we vaccinate and screen? The international perspective. Int J Cancer 2004; 111: 278–85
Giannini S, Fourneau M, Colau B, et al. Evaluation of the immune response induced by vaccination with HPV 16/18 L1 VLP formulated with either AS04 or aluminum adjuvant [abstract no. P-173]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 230
Nardelli-Haefliger D, Wirthner D, Schiller JT, et al. Specific antibody levels at the cervix during the menstrual cycle of women vaccinated with human papillomavirus 16 virus-like particles. J Natl Cancer Inst 2003; 95: 1128–37
Barr E, Koutsky LA. Re: specific antibody levels at the cervix during the menstrual cycle of women vaccinated with human papillomavirus 16 virus-like particles. J Natl Cancer Inst 2004; 96: 412–3
Gaydos CA, Gaydos JC. Adenovirus vaccine. In: Plotkin SA, Orenstein WA, editors. Vaccine. Philadelphia (PA): WB Saunders, 1999: 609–28
Schiffman M, Herrero R, Desalle R, et al. The carcinogenicity of human papillomavirus types reflects viral evolution. Virology 2005; 337: 76–84
Goldie SJ, Grima D, Kohli M, et al. A comprehensive natural history model of HPV infection and cervical cancer to estimate the clinical impact of a prophylactic HPV-16/18 vaccine. Int J Cancer 2003; 106: 896–904
Goldie SJ, Kohli M, Grima D, et al. Projected clinical benefits and cost-effectiveness of a human papillomavirus 16/18 vaccine. J Natl Cancer Inst 2004; 96: 604–15
Barnabas R, Garnett G. Assessing the effect of HPV16 transmission and HPV16 progression rates on the potential impact of HPV vaccines [abstract no. F-07]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 34
Sasieni PD, Cuzick J, Lynch-Farmery E. Estimating the efficacy of screening by auditing smear histories of women with and without cervical cancer. The National Co-ordinating Network for Cervical Screening Working Group. Br J Cancer 1996; 73: 1001–5
Koutsky L. HPV Vaccines [abstract no. F-01]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 31
Kulasingam SL, Myers ER. Potential health and economic impact of adding a human papillomavirus vaccine to screening programs. JAMA 2003; 290: 781–9
Eiben GL, Velders MP, Kast WM. The cell-mediated immune response to human papillomavirus-induced cervical cancer: implications for immunotherapy. Adv Cancer Res 2002; 86: 113–48
Kataja V, Syrjanen K, Mantyjarvi R, et al. Prospective follow-up of cervical HPV infections: life table analysis of histopathological, cytological and colposcopic data. Eur J Epidemiol 1989; 5: 1–7
Nasiell K, Roger V, Nasiell M. Behavior of mild cervical dysplasia during long-term follow-up. Obstet Gynecol 1986; 67: 665–9
Benton C, Shyahidullah H, Hunter JAM. Human papillomavirus in the immunocompromised. Papillomavirus Rep 1999; 3: 23–6
Maiman M, Fruchter RG, Serur E, et al. Human immunodeficiency virus infection and cervical neoplasia. Gynecol Oncol 1990; 38: 377–82
Laga M, Icenogle JP, Marsella R, et al. Genital papillomavirus infection and cervical dysplasia: opportunistic complications of HIV infection. Int J Cancer 1992; 50: 45–8
Rudlinger R, Smith IW, Bunney MH, et al. Human papillomavirus infections in a group of renal transplant recipients. Br J Dermatol 1986; 115: 681–92
Hilders CG, Ras L, vanEendenburg JD, et al. Isolation and characterization of tumor-infiltrating lymphocytes from cervical carcinoma. Int J Cancer 1994; 57: 805–13
Rogozinski TT, Jablonska S, Jarzabek-Chorzelska M. Role of cell-mediated immunity in spontaneous regression of plane warts. Int J Dermatol 1988; 27: 322–6
Coleman N, Birley HD, Renton AM, et al. Immunological events in regressing genital warts. Am J Clin Pathol 1994; 102: 768–74
Hong K, Greer CE, Ketter N, et al. Isolation and characterization of human papillomavirus type 6-specific T cells infiltrating genital warts. J Virol 1997; 71: 6427–32
Nakagawa M, Viscidi R, Deshmukh I, et al. Time course of humoral and cell-mediated immune responses to human papillomavirus type 16 in infected women. Clin Diagn Lab Immunol 2002; 9: 877–82
Roden RB, Ling M, Wu TC. Vaccination to prevent and treat cervical cancer. Hum Pathol 2004; 35: 971–82
DaSilva DM, Eiben GL, Fausch SC, et al. Cervical cancer vaccines: emerging concepts and developments. J Cell Physiol 2001; 186: 169–82
Velders MP, Weijzen S, Eiben GL, et al. Defined flanking spacers and enhanced proteolysis is essential for eradication of established tumors by an epitope string DNA vaccine. J Immunol 2001; 166: 5366–73
Han R, Cladel NM, Reed CA, et al. DNA vaccination prevents and/or delays carcinoma development of papillomavirus-induced skin papillomas on rabbits. J Virol 2000; 74: 9712–6
Chen CH, Ji H, Suh KW, et al. Gene gun-mediated DNA vaccination induces antitumor immunity against human papillomavirus type 16 E7-expressing murine tumor metastases in the liver and lungs. Gene Ther 1999; 6: 1972–81
Zwaveling S, Ferreira Mota SC, Nouta J, et al. Established human papillomavirus type 16-expressing tumors are effectively eradicated following vaccination with long peptides. J Immunol 2002; 169: 350–8
Gerard CM, Baudson N, Kraemer K, et al. Therapeutic potential of protein and adjuvant vaccinations on tumour growth. Vaccine 2001; 19: 2583–9
Chu NR, Wu HB, Wu T, et al. Immuno therapy of a human papillomavirus (HPV) type 16 E7-expressing tumour by administration of fusion protein comprising Mycobacterium bovis bacille Calmette-Guerin (BCG) hsp65 and HPV16 E7. Clin Exp Immunol 2000; 121: 216–25
Welters MJ, Filippov DV, van denEeden SJ, et al. Chemically synthesized protein as tumour-specific vaccine: immunogenicity and efficacy of synthetic HPV16 E7 in the TC-1 mouse tumour model. Vaccine 2004; 23: 305–11
Lamikanra A, Pan ZK, Isaacs SN, et al. Regression of established human papillomavirus type 16 (HPV-16) immortalized tumors in vivo by vaccinia viruses expressing different forms of HPV-16 E7 correlates with enhanced CD8(+) T-cell responses that home to the tumor site. J Virol 2001; 75: 9654–64
Velders MP, McElhiney S, Cassetti MC, et al. Eradication of established tumors by vaccination with Venezuelan equine encephalitis virus replicon particles delivering human papillomavirus 16 E7 RNA. Cancer Res 2001; 61: 7861–7
Gunn GR, Zubair A, Peters C, et al. Two Listeria monocytogenes vaccine vectors that express different molecular forms of human papilloma virus-16 (HPV-16) E7 induce qualitatively different T cell immunity that correlates with their ability to induce regression of established tumors immortalized by HPV-16. J Immunol 2001; 167: 6471–9
Greenstone HL, Nieland JD, deVisser KE, et al. Chimeric papillomavirus virus-like particles elicit antitumor immunity against the E7 oncoprotein in an HPV16 tumor model. Proc Natl Acad Sci U S A 1998; 95: 1800–5
Schafer K, Muller M, Faath S, et al. Immune response to human papillomavirus 16 L1E7 chimeric virus-like particles: induction of cytotoxic T cells and specific tumor protection. Int J Cancer 1999; 81: 881–8
Mayordomo JI, Zorina T, Storkus WJ, et al. Bone marrow-derived dendritic cells pulsed with synthetic tumour peptides elicit protective and therapeutic anti tumour immunity. Nat Med 1995; 1: 1297–302
Ossevoort MA, Feltkamp MC, vanVeen KJ, et al. Dendritic cells as carriers for a cytotoxic T-lymphocyte epitope-based peptide vaccine in protection against a human papillomavirus type 16-induced tumor. J Immunother Emphasis Tumor Immunol 1995; 18: 86–94
Chang EY, Chen CH, Ji H, et al. Antigen-specific cancer immunotherapy using a GM-CSF secreting allogeneic tumor cell-based vaccine. Int J Cancer 2000; 86: 725–30
Connor ME, Stern PL. Loss of MHC class-I expression in cervical carcinomas. Int J Cancer 1990; 46: 1029–34
Fowler NL, Frazer IH. Mutations in TAP genes are common in cervical carcinomas. Gynecol Oncol 2004; 92: 914–21
Tindle RW. Immune evasion in human papillomavirus-associated cervical cancer. Nat Rev Cancer 2002; 2: 59–65
Kobayashi A. Regulatory cells are involved in local immunosuppression in cervical cancer [abstract no. H-03]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 44
van der Burg SH, de Jong AM, van der Hulst AM, et al. HPV-specific CD4+ T cells in cervical tumor-draining lymph nodes dominantly produce IL-10 and are capable of suppressing the antigenic response of naive T cells [abstract no. H-05]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 45
Steller MA, Gurski KJ, Murakami M, et al. Cell-mediated immunological responses in cervical and vaginal cancer patients immunized with a lipidated epitope of human papillomavirus type 16 E7. Clin Cancer Res 1998; 4: 2103–9
vanDriel WJ, Ressing ME, Kenter GG, et al. Vaccination with HPV16 peptides of patients with advanced cervical carcinoma: clinical evaluation of a phase I-II trial. Eur J Cancer 1999; 35: 946–52
Muderspach L, Wilczynski S, Roman L, et al. A phase I trial of a human papillomavirus (HPV) peptide vaccine for women with high-grade cervical and vulvar intraepithelial neoplasia who are HPV 16 positive. Clin Cancer Res 2000; 6: 3406–16
Goldstone SE, Palefsky JM, Winnett MT, et al. Activity of HspE7, a novel immunotherapy, in patients with anogenital warts. Dis Colon Rectum 2002; 45: 502–7
Hallez S, Simon P, Maudoux F, et al. Phase I/II trial of immunogenicity of a human papillomavirus (HPV) type 16 E7 protein-based vaccine in women with oncogenic HPV-positive cervical intraepithelial neoplasia. Cancer Immunol Immunother 2004; 53: 642–50
Frazer IH, Quinn M, Nicklin JL, et al. Phase 1 study of HPV16-specific immunotherapy with E6E7 fusion protein and ISCOMATRIX adjuvant in women with cervical intraepithelial neoplasia. Vaccine 2004; 23: 172–81
Zhang LF, Zhou J, Chen S, et al. HPV6b virus like particles are potent immunogens without adjuvant in man. Vaccine 2000; 18: 1051–8
Klencke B, Matijevic M, Urban RG, et al. Encapsulated plasmid DNA treatment for human papillomavirus 16-associated anal dysplasia: a Phase I study of ZYC101. Clin Cancer Res 2002; 8: 1028–37
Sheets EE, Urban RG, Crum CP, et al. Immunotherapy of human cervical high-grade cervical intraepithelial neoplasia with microparticle-delivered human papillomavirus 16 E7 plasmid DNA. Am J Obstet Gynecol 2003; 188: 916–26
Garcia F, Petry KU, Muderspach L, et al. ZYC101a for treatment of high-grade cervical intraepithelial neoplasia: a randomized controlled trial. Obstet Gynecol 2004; 103: 317–26
Ferrara A, Nonn M, Sehr P, et al. Dendritic cell-based tumor vaccine for cervical cancer II: results of a clinical pilot study in 15 individual patients. J Cancer Res Clin Oncol 2003; 129: 521–30
Corona Gutierrez CM, Tinoco A, Navarro T, et al. Therapeutic vaccination with MVA E2 can eliminate precancerous lesions (CIN 1, CIN 2, and CIN 3) associated with infection by oncogenic human papillomavirus. Hum Gene Ther 2004; 15: 421–31
Thompson HS, Davies ML, Holding FP, et al. Phase I safety and antigenicity of TA-GW: a recombinant HPV6 L2E7 vaccine for the treatment of genital warts. Vaccine 1999; 17: 40–9
Lacey CJ, Thompson HS, Monteiro EF, et al. Phase IIa safety and immunogenicity of a therapeutic vaccine, TA-GW, in persons with genital warts. J Infect Dis 1999; 179: 612–8
Borysiewicz LK, Fiander A, Nimako M, et al. A recombinant vaccinia virus encoding human papillomavirus types 16 and 18, E6 and E7 proteins as immunotherapy for cervical cancer. Lancet 1996; 347: 1523–7
Kaufmann AM, Stern PL, Rankin EM, et al. Safety and immunogenicity of TA-HPV, a recombinant vaccinia virus expressing modified human papillomavirus (HPV)-16 and HPV-18 E6 and E7 genes, in women with progressive cervical cancer. Clin Cancer Res 2002; 8: 3676–85
deJong A, O’Neill T, Khan AY, et al. Enhancement of human papillomavirus (HPV) type 16 E6 and E7-specific T-cell immunity in healthy volunteers through vaccination with TA-CIN, an HPV16 L2E7E6 fusion protein vaccine. Vaccine 2002; 20: 3456–64
Baldwin PJ, van derBurg SH, Boswell CM, et al. Vaccinia-expressed human papillomavirus 16 and 18 E6 and E7 as a therapeutic vaccination for vulval and vaginal intraepithelial neoplasia. Clin Cancer Res 2003; 9: 5205–13
Davidson EJ, Boswell CM, Sehr P, et al. Immunological and clinical responses in women with vulval intraepithelial neoplasia vaccinated with a vaccinia virus encoding human papillomavirus 16/18 oncoproteins. Cancer Res 2003; 63: 6032–41
Smyth LJ, VanPoelgeest MI, Davidson EJ, et al. Immunological responses in women with human papillomavirus type 16 (HPV-16)-associated anogenital intraepithelial neoplasia induced by heterologous prime-boost HPV-16 oncogene vaccination. Clin Cancer Res 2004; 10: 2954–61
Davidson EJ, Faulkner RL, Sehr P, et al. Effect of TA-CIN (HPV 16 L2E6E7) booster immunisation in vulval intraepithelial neoplasia patients previously vaccinated with TA-HPV (vaccinia virus encoding HPV 16/18 E6E7). Vaccine 2004; 22: 2722–9
Cassetti MC, McElhiney SP, Shahabi V, et al. Antitumor efficacy of Venezuelan equine encephalitis virus replicon particles encoding mutated HPV16 E6 and E7 genes. Vaccine 2004; 22: 520–7
Osen W, Peiler T, Ohlschlager P, et al. A DNA vaccine based on a shuffled E7 oncogene of the human papillomavirus type 16 (HPV 16) induces E7-specific cytotoxic T cells but lacks transforming activity. Vaccine 2001; 19: 4276–86
Ganss R, Arnold B, Hammerling GJ. Mini-review: overcoming tumor-intrinsic resistance to immune effector function. Eur J Immunol 2004; 34: 2635–41
Chen CH, Wang TL, Hung CF, et al. Boosting with recombinant vaccinia increases HPV-16 E7-specific T cell precursor frequencies of HPV-16 E7-expressing DNA vaccines. Vaccine 2000; 18: 2015–22
van derBurg SH, Kwappenberg KM, O’Neill T, et al. Pre-clinical safety and efficacy of TA-CIN, a recombinant HPV16 L2E6E7 fusion protein vaccine, in homologous and heterologous prime-boost regimens. Vaccine 2001; 19: 3652–60
DaSilva DM, Schiller JT, Kast WM. Heterologous boosting increases immu-nogenicity of chimeric papillomavirus virus-like particle vaccines. Vaccine 2003; 21: 3219–27
Feltkamp MC, Vreugdenhil GR, Vierboom MP, et al. Cytotoxic T lymphocytes raised against a subdominant epitope offered as a synthetic peptide eradicate human papillomavirus type 16-induced tumors. Eur J Immunol 1995; 25: 2638–42
Rosenberg SA, Yannelli JR, Yang JC, et al. Treatment of patients with metastatic melanoma with autologous tumor-infiltrating lymphocytes and interleukin 2. J Natl Cancer Inst 1994; 86: 1159–66
Daemen T, Riezebos-Brilman A, Bungener L, et al. Eradication of established HPV16-transformed tumours after immunisation with recombinant Semliki Forest virus expressing a fusion protein of E6 and E7. Vaccine 2003; 21: 1082–8
Xue S, Gillmore R, Downs A, et al. Exploiting T cell receptor genes for cancer immunotherapy. Clin Exp Immunol 2005; 139: 167–72
Scholten KB, Schreurs MW, Ruizendaal JJ, et al. Preservation and redirection of HPV16E7-specific T cell receptors for immunotherapy of cervical cancer. Clin Immunol 2005; 114: 119–29
Brinkman JA, Caffrey AS, Muderspach LI, et al. The impact of anti HPV vaccination on cervical cancer incidence and HPV induced cervical lesions: consequences for clinical management. Eur J Gynaecol Oncol 2005; 26: 129–42
Dempsey A, Zimet G, Koutsky L. Parental acceptance of HPV vaccines [abstract no. P-163]. 22nd International Papillomavirus Conference; 2005 May–6; Vancouver, 225
Brabin L. A study of parents’ views on adolescent HPV vaccination [abstract no. P-506]. 22nd International Papillomavirus Conference; 2005 May 1–6; Vancouver, 393
Hughes JP, Garnett GP, Koutsky L. The theoretical population-level impact of a prophylactic human papilloma virus vaccine. Epidemiology 2002; 13: 631–9
Acknowledgments
Parts of the studies mentioned in this article were supported through grants from the National Institutes of Health (NIH) [NIH R01 CA74397 and NIH P01 CA97296], the V Foundation, and the Whittier Foundation (to Dr Kast). Dr Da Silva is supported in part by a postdoctoral research training fellowship NCI T32 CA009320. Dr Kast holds the Walter A. Richter Cancer Research Chair.
The authors claim no financial conflicts of interest that are directly relevant to the contents and opinions expressed in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Da Silva, D.M., Kast, W.M. Vaccination against cervical cancer. Am J Cancer 4, 207–219 (2005). https://doi.org/10.2165/00024669-200504040-00001
Published:
Issue Date:
DOI: https://doi.org/10.2165/00024669-200504040-00001