Abstract
Background: Comprehension of risks, benefits and alternative treatment options is poor among patients referred for cardiac surgery interventions. We sought to explore the impact of a formalized shared decision-making (SDM) process on patient comprehension and decisional quality among older patients referred for cardiac surgery.
Methods: We developed and evaluated a paper-based decision aid for cardiac surgery within the context of a prospective SDM design. Surgeons were trained in SDM through a Web-based program. We acted as decisional coaches, going through the decision aids with the patients and their families, and remaining available for consultation. Patients (aged ≥ 65 yr) undergoing isolated valve, coronary artery bypass graft (CABG) or CABG and valve surgery were eligible. Participants in the non-SDM phase followed standard care. Participants in the SDM group received a decision aid following cardiac catheterization, populated with individualized risk assessment, personal profile and comorbidity status. Both groups were assessed before surgery on comprehension, decisional conflict, decisional quality, anxiety and depression.
Results: We included 98 patients in the SDM group and 97 in the non-SDM group. Patients who received decision aids through a formalized SDM approach scored higher in comprehension (median 15.0, interquartile range [IQR] 12.0–18.0) than those who did not (median 9.0, IQR 7.0–12.0, p < 0.001). Decisional quality was greater in the SDM group (median 82.0, IQR 73.0–91.0) than in the non-SDM group (median 76.0, IQR 62.0–82.0, p < 0.05). Decisional conflict scores were lower in the SDM group (mean 1.76, standard deviation [SD] 1.14) than in the non-SDM group (mean 5.26, SD 1.02, p < 0.05). Anxiety and depression scores showed no significant difference between groups.
Conclusion: Institution of a formalized SDM process including individualized decision aids improved comprehension of risks, benefits and alternatives to cardiac surgery, as well as decisional quality, and did not result in increased levels of anxiety.
Despite consensus on the importance of patient-centred care, including elicitation of patient preference in arriving at a treatment plan, effective implementation of shared decision-making (SDM) in surgery has been sparse.1 More than 20 years ago, the Institute of Medicine called for patient-centred care in their landmark document, “Crossing the Quality Chasm.”2 It included an explicit requirement for the effective elicitation of patient preferences, a requirement that has yet to be realized.2 The legal requirement to effectively communicate the risks, benefits and alternatives to surgical treatment date back to 1914.3
Current approaches to informed consent in surgery, specifically in cardiac surgery, result in very poor comprehension of the risks, benefit and alternatives, failing to achieve even the rudimentary requirements for legal consent, let alone heeding the call for effective patient-centred care.4–7 The lack of comprehension resulting from current informed consent processes is compounded among older, high-risk patients undergoing cardiac surgery, where the decision of whether to have an operation has to be weighed against the increased likelihood of long-term adverse outcomes. We have previously shown that patients referred for cardiac surgery are older, have higher prevalence of frailty and are facing more complex, combined cardiac surgery procedures.8 Further, we showed that frail patients undergoing cardiac surgery are at considerably higher risk of death and, perhaps more importantly, prolonged institutional care.9 Thus, there is an unprecedented degree of equipoise for frail, older patients referred for cardiac surgery.
Shared decision-making is a process that involves the patient and the provider making collaborative decisions on the treatment plan, accounting for both clinical evidence and patient preferences. The efficacy of SDM has been reported in several studies, and SDM has been shown to be optimally effective when combined with decision aids, documents that communicate information about potential outcomes associated with given treatment choices.10–12
Previously, we embarked on a qualitative study using focus groups of patients and providers to determine the best approaches to establishing SDM among patients being considered for cardiac surgery.13 We determined that both groups supported the use of individualized decision aids, populated with predictions calculated for each individual for the outcomes identified as most relevant (i.e., death, stroke, dialysis, prolonged institutional care and 2-yr survival).13 They were also supportive of earlier intervention and the use of a decisional coach (i.e., a health care professional who reviews the decision aid with the patients and their families and facilitates information flow).
With these findings in mind, we sought to determine the impact of a formalized SDM process on decisional quality among patients referred for cardiac surgery.
Methods
Study setting and recruitment
We conducted a prospective interventional study in the Nova Scotia Health Authority (NSHA) Department of Cardiac Surgery between June 2014 and June 2017. The NSHA Department of Cardiac Surgery is the sole provider of cardiac surgical care for the province of Nova Scotia, as well as a portion of the province of Prince Edward Island. We recruited patients from the cardiovascular clinic, and the same-day admission and inpatient units at the Halifax Infirmary.
Inclusion criteria
We included patients aged 65 years or older who were referred for cardiac surgery, including isolated valves, isolated coronary artery bypass grafts (CABGs) or both CABG and valves. We excluded patients undergoing urgent or emergent procedures.
Data collection
Patients in the non-SDM group had no change to their consent process or standard of care to act as a baseline for the SDM group. Before surgery, participants completed questionnaires. We contacted patients again 6–9 months after discharge for phone follow-up and administration of a quality-of-life questionnaire (EQ-5D-3L).
Patients in the SDM group consented to additional information supports, including contact with the decisional coach and provision of a decision aid populated with an individualized risk assessment, personal profile and comorbidity status. Specifically, we created a unique decision aid populated with risks of adverse outcomes, previously determined through focus groups to be of primary concern to patients undergoing cardiac surgery. The decisional coach was the cardiac surgery patient navigator, a registered nurse with experience in cardiac surgery, who normally provides support to patients awaiting cardiac surgery. After SDM training and familiarization with the decision aid material, the patient navigator, acting as decision coach, went through the decision aid with the patient and, per the patient’s direction, family members. The coach answered questions or brought them to the assigned cardiac surgeon for resolution as needed. After providing informed consent was completed but before surgery, participants completed questionnaires. Patients were contacted again 6–9 months after discharge for phone follow-up and administration of a quality-of-life questionnaire (EQ-5D-3L).
Questionnaires
Both the non-SDM and SDM groups completed the same set of questionnaires.
The Maritime Heart Centre Comprehension Scale (MHCCS) is based on a validated cardiac comprehension scale by Mishra and colleagues.14 It measures how informed patients are when giving consent for elective CABG, scoring patients based on their responses to the consent discussion.14 The MHCCS is a 10-item questionnaire, modified to reflect our study population (Appendix 1A, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004922/tab-related-content), with responses scored on a scale of 0–3 (with 3 indicating the most accurate and complete response) or 0–2 (for risk recall). Scores for the entire scale range from 0 to 24, with higher scores indicating greater comprehension of issues pertaining to the consent discussion.
The Decisional Conflict Scale (DCS) is a validated instrument used to measure patient perceptions of uncertainty in choosing options and modifiable factors contributing to uncertainty (Appendix 1B). We chose the 10-item, 3-response format to accommodate those with limited reading or response skills. Each response category is scored from 0 to 4, with total scores ranging from 0 to 40, where higher scores indicate greater decisional conflict.15
The SDM 9-Item Questionnaire (SDM-Q-9) was developed in a theory-driven manner and measures the extent to which patients are involved in the process of decision-making from the perspective of the patient. It has been found to be acceptable and reliable, and to have factorial validity (Appendix 1C). The SDM-Q-9 is a 9-item Likert scale, with scores ranging from 0 to 5 (with 5 indicating a high level of patient agreement) and a total score ranging from 0 to 45, which is then converted to a score out of 100.16
The Hospital Anxiety and Depression Scale (HADS) is a validated self-assessment scale to detect states of depression, anxiety and emotional distress among patients being treated for a variety of clinical problems (Appendix 1D). The scale has a total of 14 items, with responses scored on a scale of 0–3 (with 3 indicating higher symptom frequencies. Scores for each subscale (anxiety and depression) range from 0 to 21 with scores categorized as normal (0–7), mild (8–10), moderate (11–14) and severe (15–21). Scores for the entire scale (emotional distress) range from 0 to 42, with higher scores indicating more distress.17
The EQ-5D-3L is a validated instrument for use as a measure of health outcome (Appendix 1E).18 It includes a descriptive system and a visual analogue scale (VAS). The descriptive system includes the following 5 dimensions: mobility, self-care, usual activities, pain or discomfort and anxiety or depression. Each dimension has 3 categorical levels (no problems, some problems, extreme problems). The EQ VAS records the respondent’s self-rated health on a vertical, visual scale where the endpoints are labelled “best imaginable health state” and “worst imaginable health state.”
Shared decision-making training
After recruitment of participants in the non-SDM group, research staff and the principal investigator underwent extensive training through formalized SDM education sessions. These courses were prepared and moderated by the Informed Medical Decisions Foundation in Boston, Massachusetts. The course framework was then condensed to a 90-minute presentation with teach-back and testing for all cardiac surgeons and the patient navigator via 1-on-1 training sessions with research moderators. Training included an online training course covering medical experiences amenable to SDM, evaluation of patient–provider interaction, addressing patients’ goals and concerns, and SDM practice. Follow-up phone calls were scheduled once all research staff completed training to review course material and cover any additional questions regarding the use of SDM in clinical settings.
Decisional support material
We developed risk calculators to provide individualized risk as part of the decisional support materials for patients in the SDM group. Risk prediction was based on either our own published models or validated external models. Using our validated risk prediction models (which include frailty as a predictor) allowed us to provide patient-specific risks for in-hospital death, major morbidity and prolonged institutional care, as well as longer-term (2-yr) freedom from death. For death and discharge to institution (defined as nursing facility or home hospital), we used a previously published in-house model to assess the risk of frailty on postoperative outcomes. For risk of stroke, we used the Society of Thoracic Surgeons’ 2008 stroke models for isolated CABG, isolated valve, and both CABG and valve.19–21 We generated risk of acute renal failure using variable weights from models by Thakar and colleagues.22
For predicted 2-year risk of death with medical treatment, we convened a Delphi panel with staff cardiac surgeons and SDM cardiologists to arrive at consensus for risks from 2-year survival rates among medically treated patients. After review of literature on ischemic heart disease and aortic stenosis, the Delphi panel agreed on ranged estimates of 3%–28% for ischemic heart disease and 30%–60% for aortic stenosis.
Based on qualitative work illustrating the need for and barriers to SDM, including identification of the outcomes important to patients,13 we generated decision aids for patients in the SDM group. These aids included information about a patient’s particular heart condition, relevant aspects of the anatomy and function of the heart, treatment options and the individualized risk assessments. The information from our risk calculators allowed us to populate decision aids with individualized information for each patient, displayed in 10 × 10 dot plots, with red dots indicating the risk percentage for adverse outcomes from the risk calculator (Appendix 2, available at www.canjsurg.ca/lookup/doi/10.1503/cjs.004922/tab-related-content). Armstrong and colleagues23 stated that the general public can interpret survival at a point in time relatively well, and that understanding could be improved with a single curve practice exercise. However, in their study, only 74 % of participants could interpret a survival curve well enough to determine the number of survivors at various time points, and only 55 % could calculate the difference in survival between 2 time points.23 Given our interest in communicating the risk of surviving the procedure and survivability rates at 2 years, coupled with the age difference between our population of interest (age ≥ 65 yr) and those in the Armstrong study (mean age 39.8 yr), we felt that dot plot graphics were the best medium to communicate this information. Ancker and colleagues24 described these plots as part-to-whole icon arrays with sequential arrangements, where proportions are easy to judge because the part-to-whole information is available visually.24 We selected the adverse outcomes modelled in each individualized decision aid that were important to patients based on our previously published qualitative work with patients aged 65 years and older who were referred for cardiac surgery.13
Data analysis
We managed and analyzed data with SAS 9.3 for Windows. We used descriptive statistics to summarize demographic characteristics. We compared questionnaire scores in the non-SDM and SDM groups using the Mann–Whitney U test for 2 independent samples and reporting the median and interquartile range (IQR) as scores were not normally distributed. We determined changes in EQ-5D-3L scores from initial and follow-up assessments using paired t tests. Significance was set at p less than 0.05.
Ethics approval
All participating patients consented to taking part in answering questionnaires and follow-up phone calls at 6–9 months. We obtained written informed consent from all patients. The study had full approval of the NSHA Research Ethics Board (CDHA-RS/2014-237).
Results
Of the 195 patients who participated in the study, 98 (50.3%) participated in the non-SDM group and 97 (49.7%) participated in the SDM group. Non-SDM participants were recruited between June 2014 and September 2015, and SDM group participants were recruited between January 2016 and June 2017. None of the preoperative characteristics of study participants were significantly associated with the patients’ province of residence. The baseline preoperative characteristics are presented in Table 1. Six patients in the non-SDM group and 7 patients in the SDM group were referred for surgery but ultimately received percutaneous cardiac intervention or medical therapy. The median age was 70.3 years, females made up 25.6% of participants, 60.5% underwent isolated CABG, most participants were discharged home after surgery and slightly more participants in the SDM group were in-house patients. Overall, the non-SDM and SDM groups were comparable in risk factors, patient demographics and procedures performed.
Preoperative characteristics of patients referred for cardiac surgery at the Halifax Infirmary from June 2014 to June 2017
Comprehension
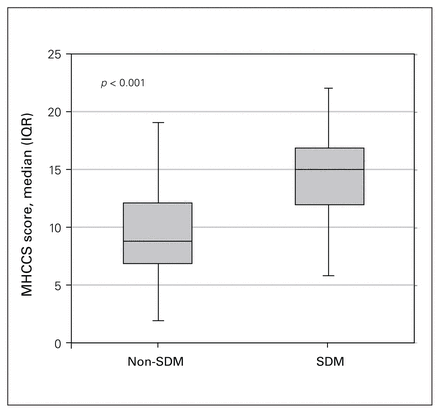
Comprehension, as measured by the MHCCS, was significantly higher in the SDM group, with a median score of 15 (IQR 12.0–18.0), compared with a median score of 9 (IQR 7.0–12.0) in the non-SDM group (p < 0.001) (Figure 1).
Patient comprehension in the shared decision-making (SDM) and non-SDM groups, as measured by the Maritime Heart Centre Comprehension Scale (MHCCS). IQR = interquartile range.
Decisional quality
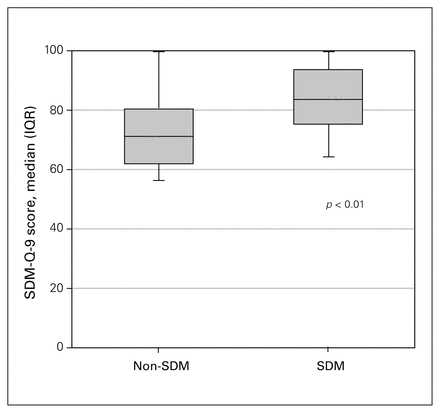
Decision quality, as measured by the SDM-Q-9, was higher in the SDM group, with a median score of 82 (IQR 73.0–91.0), compared with a median score of 76 (IQR 62.0–82.0) in the non-SDM group (p < 0. 01) (Figure 2).
Decisional quality in the shared decision-making (SDM) and non-SDM groups, as measured with the Shared Decision-Making 9-Item Questionnaire (SDM-Q-9). IQR = interquartile range.
Decisional conflict
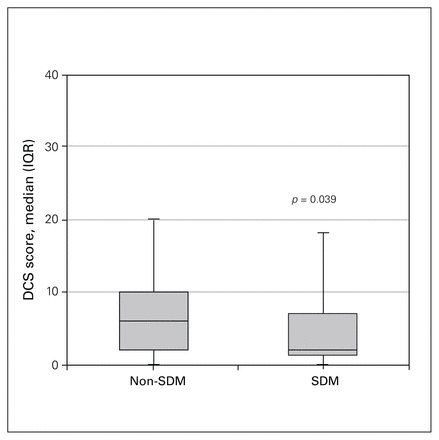
Decisional conflict, as measured by the DCS, was lower in the SDM group, with a mean of 1.76 (standard deviation [SD] 1.14), compared with a mean of 5.26 (SD 1.02) in the non-SDM group (p = 0.039), where lower scores indicate less decisional conflict (Figure 3).
Decisional conflict in the shared decision-making (SDM) and non-SDM groups, as measured with the Decisional Conflict Scale (DSC). IQR = interquartile range.
Anxiety and depression
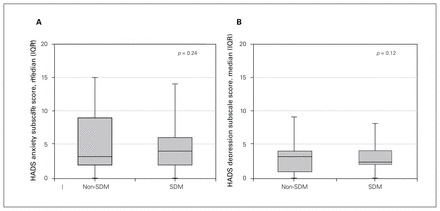
There was no significant difference in HADS scores by group for either anxiety (p = 0.24) or depression (p = 0.12), suggesting that more effective communication of risk was not associated with these measures (Figure 4). The median total score was 9 (IQR 4-0–12.0) in the non-SDM group and 7 (IQR 5.0–11.0) in the SDM group.
(A) Anxiety and (B) depression in the shared decision-making (SDM) and non-SDM groups, as measured with the Hospital Anxiety and Depression Scale (HADS). IQR = interquartile range.
Quality of life
The EQ-5D-3L questionnaires were presented to patients before surgery and 6–9 months after surgery during the follow-up phone call. We used listwise deletion for missing data for patients who did not complete both baseline and follow-up assessments of the EQ-5D-3L. We deleted 10 cases in the non-SDM group, and 14 cases in the SDM group because of loss to follow-up. Although patients in both groups had an increase in quality of life at 6 months compared with their preoperative baseline, there were no significant differences between the non-SDM and SDM groups in the degree of improvement seen (Table 2). Scores on the EQ-VAS were not significantly different between groups or from baseline to follow-up (Table 3).
Quality-of-life (EQ-5D-3L) outcomes for patients referred for cardiac surgery at the Halifax Infirmary from June 2014 to June 2017
Quality-of-life visual analogue scale (EQ-VAS) scores for patients referred for cardiac surgery at the Halifax Infirmary from June 2014 to June 2017
Discussion
We found that the addition of individualized decisional supports for older patients referred for cardiac surgery increased patient comprehension and decisional quality, while reducing decisional regret and not significantly changing clinical assessments of anxiety or depression. It has been well documented in the literature that although current informed consent practices meet legal requirements, these are not sufficient to provide truly informed consent. Shared decision-making has been consistently shown to effectively improve decisional quality in multiple disciplines, emphasizing the role of the patient through a patient-centred approach, engaging and empowering patients to become equal partners in the decision-making process. In this study, we initiated a formalized, SDM process for older patients referred for cardiac surgery that is effective in increasing decisional quality in terms of comprehension, as well as degree of SDM and decisional conflict. This finding is in support of previous qualitative work we had done among our patients and providers.13
Our results are in agreement with published literature regarding the value of SDM in positively affecting both decisional quality and intervention. Although recognized as a worthwhile initiative in surgical interventions, actual SDM efforts in surgical decision-making are at a very early stage. Politi and colleagues25 employed an interactive decision aid in a randomized controlled trial (RCT) to help patients undergoing mastectomy (n = 120) make choices around breast reconstruction. They found a 45% increase in comprehension scores, comparable to our effect size (66% improvement), but they observed no effect on decisional conflict or SDM scores. This may reflect the fact that their decision aid, while individualized through interactive patient responses, was not linked directly to the surgical consult or informed consent discussion. Furthermore, surgeons did not undergo any form of SDM training, and no coach was employed.25 Lam and colleagues26 demonstrated that a generic decision aid regarding surgical therapy for breast cancer, again without coach or surgeon training, modestly improved patients’ perceived difficulty in making a decision (8% reduction in scores for therapeutic decision-making difficulty); decisional conflict was reduced by 20%. No measure of comprehension was included. A recent systematic review identified 20 pre–post or RCT studies in urology, orthopedic surgery and breast surgery.27 These studies were small and heterogeneous in terms of both design and outcomes measured; however, some signals appeared fairly coherent. For instance, evidence for the effectiveness of SDM training for clinicians could not be demonstrated, multimedia decision aids (video and print) of an individualized nature were most effective, and impact on actual decisions taken for surgery was rarely demonstrable, likely because of small sample sizes. Most studies were in urologic and breast or endocrine surgery, with no studies identified in cardiac surgery.27 Our study showed improvement in all aspects of decisional quality with effect sizes comparable or superior to those of published studies. The literature supports the individualized decision aids that we employed. We cannot comment on whether SDM training for surgeons or provision of a decisional coach contributed to the positive findings that we achieved.
Of note, there was no demonstrable effect on the decisions made for either surgery versus percutaneous coronary intervention or medical therapy. This is consistent with the literature. Although our study was not powered for this outcome, it is important to note our previous qualitative work called for earlier intervention in the decisional process. In the current effort, our SDM approach occurred close to the time of surgery, at the point of informed consent, primarily because this is the step in the system that cardiac surgeons control. Optimal timing would be closer to the point of cardiac catheterization, although, as the only centre serving an entire province, there is a great deal of time pressure that makes meaningful interaction with members of the cardiac surgery team difficult at this time point. Current efforts to create an SDM intervention at the point of cardiac catheterization is underway at the NSHA Department of Cardiac Surgery.
In addition, health-related quality of life measures (EQ-5D-3L and EQ-VAS) improved between baseline and 6-month follow-up for both the non-SDM and SDM groups; there were no significant differences between the groups in this regard. The positive impact of SDM on ultimate health-related quality of life may be through better matching expectations with outcomes, but there is very limited literature, in the area of early treatment of breast cancer, to support this idea.28 Further work will be required as SDM matures in surgical decision-making to sort this issue out more fully.
Limitations
A relatively small number of patients recruited from a single centre in Canada may have limited generalizability. in addition, the calculation of risk in the formalized SDM intervention to populate decision aids was based on a locally generated model with good statistical performance but potentially limited generalizability. A recent study showed that low health literacy, linked to low socioeconomic status, resulted in increased decisional conflict and challenges in implementing effective SDM.29 The prospective interventional design of our study was adopted to avoid carry-over effects of SDM training for surgeons that would be inevitable in an RCT design, but creates the potential confounder of a change in practice. Patient characteristics were stable between the groups, but other aspects of clinical processes may have been affected.
Conclusion
We have shown that a formalized SDM approach with personalized decision aids improved comprehension, decisional quality and decisional conflict, without increasing anxiety or depression. Clinicians and patients benefit from tools that estimate and effectively communicate the potential benefits and risks of treatment options. The philosophy of evidence-based medicine requires that clinicians incorporate not only the best available evidence but also the patient’s values, preferences and circumstances in the decision-making process. Thus, tailoring of care, not only to the patient’s risk but to the patient’s circumstances and preferences, through careful shared deliberation represents the ideal realization in practice of the philosophy of evidence-based medicine. Our efforts in SDM include shifting the culture of medical decision-making in our centre toward a patient- and family-centric process based on accurate and relevant outcomes for this patient population. These developments will allow us to provide the right intervention for the right patient. Continued efforts in SDM in cardiac surgery will focus on scaling these initiatives to other cardiac surgery providers across Canada and North America, as well as to surgical providers across other NSHA surgical disciplines.
Acknowledgements
The authors thank the surgeons of the Division of Cardiac Surgery, Dalhousie/Nova Scotia Health for their cooperation as well as the patient navigator for her invaluable efforts at helping patients with decision aids.
Footnotes
Competing interests: Ryan Gainer and Gregory Hirsch report funding from the Nova Scotia Health Catalyst Grant. No other competing interests were declared.
Contributors: All of the authors contributed to the conception and design of the work, and to data acquisition, analysis and interpretation; all of the authors drafted the manuscript, revised it critically for important intellectual content, gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This study was funded by a Canadian Institutes of Health Research Open Operating Grant to Gregory Hirsch.
- Accepted October 12, 2022.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/