Abstract
Background
This study aimed to systematically evaluate the effect of early oral feeding (EOF) versus late oral feeding (LOF) on postoperative complications and rehabilitation outcomes for patients with esophageal cancer.
Methods
This study searched relevant literature published up to March 2023 by computer retrieval of PubMed, Embase, The Cochrane Library, and Web of Science. A meta-analysis was performed using Review Manager 5.4 software to compare the effects of EOF and LOF on postoperative complications and recovery outcomes of patients with esophageal cancer.
Results
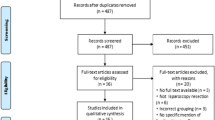
The study included 14 articles, including 9 retrospective studies, 4 randomized controlled trials (RCTs), and 1 prospective study. The 2555 patients included in the study comprised 1321 patients who received EOF and 1234 patients who received LOF. The results of the meta-analysis showed that compared with the LOF group, the EOF group has a shorter time to the first flatus postoperatively (mean difference [MD], − 1.12; 95% confidence interval [CI], (− 1.25 to − 1.00; P < 0.00001), a shorter time to the first defecation postoperatively (MD, − 1.31; 95% CI, − 1.67 to − 0.95;, P < 0.00001], and a shorter hospital stay postoperatively (MD, − 2.87; 95% CI, − 3.84 to − 1.90; P < 0.00001). The two groups did not differ significantly statistically in terms of postoperative anastomotic leakage rate (P = 0.10), postoperative chyle leakage rate (P = 0.10), or postoperative pneumonia rate (P = 0.15).
Conclusion
Early oral feeding after esophageal cancer surgery can shorten the time to the first flatus and the first defecation postoperatively, shorten the hospital stay, and promote the recovery of patients. Moreover, it has no significant effect on the incidence of postoperative complications.









Similar content being viewed by others
References
Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71:209–49.
Weijs TJ, Berkelmans GH, Nieuwenhuijzen GA, et al. Routes for early enteral nutrition after esophagectomy: a systematic review. Clin Nutr. 2015;34:1–6.
Tadano S, Terashima H, Fukuzawa J, Matsuo R, Ikeda O, Ohkohchi N. Early postoperative oral intake accelerates upper gastrointestinal anastomotic healing in the rat model. J Surg Res. 2011;169:202–8.
Soop M, Carlson GL, Hopkinson J, et al. Randomized clinical trial of the effects of immediate enteral nutrition on metabolic responses to major colorectal surgery in an enhanced recovery protocol. Br J Surg. 2004;91:1138–45.
Stang A. Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–5.
Cumpston M, Li T, Page MJ, et al. Updated guidance for trusted systematic reviews: a new edition of the cochrane handbook for systematic reviews of interventions. Cochrane Database Syst Rev. 2019. https://doi.org/10.1002/14651858.ED000142.
Tomaszek SC, Cassivi SD, Allen MS, et al. An alternative postoperative pathway reduces length of hospitalization following oesophagectomy. Eur J Cardiothorac Surg. 2010;37:807–13.
Bolton JS, Conway WC, Abbas AE. Planned delay of oral intake after esophagectomy reduces the cervical anastomotic leak rate and hospital length of stay. J Gastrointest Surg. 2014;18:304–9.
Sun HB, Liu XB, Zhang RX, et al. Early oral feeding following thoracolaparoscopic oesophagectomy for oesophageal cancer. Eur J Cardiothorac Surg. 2015;47:227–33.
Eberhard KE, Achiam MP, Rolff HC, Belmouhand M, Svendsen LB, Thorsteinsson M. Comparison of “nil by mouth” versus early oral intake in three different diet regimens following esophagectomy. World J Surg. 2017;41:1575–83.
Berkelmans GHK, Fransen L, Weijs TJ, et al. The long-term effects of early oral feeding following minimal invasive esophagectomy. Dis Esophagus. 2018;31:1–8.
Speicher JE, Gunn TM, Rossi NP, Iannettoni MD. Delay in oral feeding is associated with a decrease in anastomotic leak following transhiatal esophagectomy. Semin Thorac Cardiovasc Surg. 2018;30:476–84.
Sun HB, Li Y, Liu XB, et al. Early oral feeding following McKeown minimally invasive esophagectomy: an open-label, randomized, controlled, noninferiority trial. Ann Surg. 2018;267:435–42.
Li Y, Liu Z, Liu G, et al. Impact on short-term complications of early oral feeding in patients with esophageal cancer after esophagectomy. Nutr Cancer. 2021;73:609–16.
Berkelmans GHK, Fransen LFC, Dolmans-Zwartjes ACP, et al. Direct oral feeding following minimally invasive esophagectomy (NUTRIENT II trial): an international, multicenter, open-label randomized controlled trial. Ann Surg. 2020;271:41–7.
Liao M, Xia Z, Huang P, et al. Early enteral feeding on esophageal cancer patients after esophageal resection and reconstruction. Ann Palliat Med. 2020;9:816–23.
Jiang Z, Luo J, Xu M, et al. Safety analysis of early oral feeding after esophagectomy in patients complicated with diabetes. J Cardiothorac Surg. 2021;16:56.
Chen X, Wang P, Leng C, et al. Early oral feeding after esophagectomy accelerated gut function recovery by regulating brain-gut peptide secretion. Surgery. 2022;172:919–25.
Fransen LFC, Janssen THJB, Aarnoudse M, Nieuwenhuijzen GAP, Luyer MDP. Direct oral feeding after a minimally invasive esophagectomy: a single-center prospective cohort study. Ann Surg. 2022;275:919–23.
Hao W, Gao K, Li K, et al. The feasibility of early oral feeding after neoadjuvant chemotherapy combined with “non-tube no fasting”-enhanced recovery. Ann Surg Oncol. 2023;30:1564–71.
Fujita T, Daiko H, Nishimura M. Early enteral nutrition reduces the rate of life-threatening complications after thoracic esophagectomy in patients with esophageal cancer. Eur Surg Res. 2012;48:79–84.
Li X, Yan S, Ma Y, et al. Impact of early oral feeding on anastomotic leakage rate after esophagectomy: a systematic review and meta-analysis. World J Surg. 2020;44:2709–18.
Shanmugasundaram R, Hopkins R, Neeman T, Beenen E, Fergusson J, Gananadha S. Minimally invasive McKeown’s vs open oesophagectomy for cancer: a meta-analysis. Eur J Surg Oncol. 2019;45:941–9.
Mboumi IW, Reddy S, Lidor AO. Complications after esophagectomy. Surg Clin North Am. 2019;99:501–10.
Miao L, Zhang Y, Hu H, et al. Incidence and management of chylothorax after esophagectomy. Thorac Cancer. 2015;6:354–8.
Shah RD, Luketich JD, Schuchert MJ, et al. Postesophagectomy chylothorax: incidence, risk factors, and outcomes. Ann Thorac Surg. 2012;93:897–904.
Zhang SS, Yang H, Luo KJ, et al. The impact of body mass index on complication and survival in resected oesophageal cancer: a clinical-based cohort and meta-analysis. Br J Cancer. 2013;109:2894–903.
Lassen K, Kjaeve J, Fetveit T, et al. Allowing normal food at will after major upper gastrointestinal surgery does not increase morbidity: a randomized multicenter trial. Ann Surg. 2008;247:721–9.
Zhu Z, Li Y, Zheng Y, et al. Chewing 50 times per bite could help to resume oral feeding on the first postoperative day following minimally invasive oesophagectomy. Eur J Cardiothorac Surg. 2018;53:325–30.
Preston SR, Markar SR, Baker CR, Soon Y, Singh S, Low DE. Impact of a multidisciplinary standardized clinical pathway on perioperative outcomes in patients with oesophageal cancer. Br J Surg. 2013;100:105–12.
Van den Heijkant TC, Costes LM, van der Lee DG, et al. Randomized clinical trial of the effect of gum chewing on postoperative ileus and inflammation in colorectal surgery. Br J Surg. 2015;102:202–11.
Zheng R, Devin CL, Pucci MJ, Berger AC, Rosato EL, Palazzo F. Optimal timing and route of nutritional support after esophagectomy: a review of the literature. World J Gastroenterol. 2019;25:4427–36.
Klevebro F, Johar A, Lagergren J, Lagergren P. Outcomes of nutritional jejunostomy in the curative treatment of esophageal cancer. Dis Esophagus. 2019. https://doi.org/10.1093/dote/doy113.
Acknowledgment
This research was supported by the Gansu Province Key R&D Project (22YF7FA095).
Declarations
Funding
Gansu Province Key R&D Project, (22YF7FA095).
Author information
Authors and Affiliations
Contributions
Ziqiang Hong: Conceptualization, Methodology, Formal analysis, Investigation, Writing‒Original Draft, and Visualization. Yunjiu Gou and Jing Zhao: Conceptualization, Methodology, Formal analysis, Investigation, Writing‒Review & Editing, Visualization, and Supervision. Xiangdou Bai and Hongchao Li: Conceptualization, Methodology, Investigation, and Writing‒Review & Editing. Tao Cheng, Yingjie Lu and Yannan Sheng: Conceptualization, Methodology, Writing‒Review & Editing, and Supervision. Baiqiang Cui, Xusheng Wu and Dacheng Jin: Conceptualization, Methodology, Writing‒Review & Editing, and Supervision.
Corresponding author
Ethics declarations
Disclosure
There are no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hong, Z., Lu, Y., Li, H. et al. Effect of Early Versus Late Oral Feeding on Postoperative Complications and Recovery Outcomes for Patients with Esophageal Cancer: A Systematic Evaluation and Meta-Analysis. Ann Surg Oncol 30, 8251–8260 (2023). https://doi.org/10.1245/s10434-023-14139-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-14139-2