Abstract
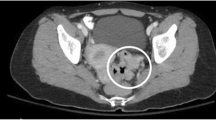
Ovarian cancer is the most lethal of all gynecologic cancers.1 Primary debulking surgery (PDS) with achievement of no residual tumor (RT, 0) still is the recommended treatment, and the one with the greatest prognostic impact.2,3 Given the usual disease spread, several surgical procedures often are needed, and one of the most frequent is rectosigmoid resection.4 Anastomotic leak is the most feared complication. Other common complications are persistent urinary, defecatory, and sexual dysfunction due to autonomic nervous system injuries during surgery.5 Even if mesorectal resection is not deemed part of the treatment paradigm for advanced ovarian cancer (AOC), total mesorectal excision (TME) is the most common surgical technique used. However, for selected cases, with detection of no lymphadenopathies at the origin of the of the inferior mesenteric artery and a favorable ratio between the length of the left colon and the extent of the bowel carcinomatosis, a mesorectal-sparing resection with the preservation of the superior rectal artery and the mesorectal tissue should be pursued. This report presents the case of a 54-year-old woman with a diagnosis of FIGO stage 3C AOC who underwent PDS. The video (video 1) provides a step-by-step description of the surgical technique adopted for colorectal resection with mesorectal-sparing technique. Rectosigmoid mesorectal-sparing resection is feasible and could be a viable option for selected cases of AOC, maximizing the blood supply to colorectal anastomosis while minimizing the risk of both anastomotic leak and pelvic autonomic nervous system dysfunction.6
Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2020. CA Cancer J Clin. 2020;70:7–30. https://doi.org/10.3322/caac.21590 (Epub 8 January 2020 PMID: 31912902).
Du Bois A, Reuss A, Pujade-Lauraine E, Harter P, Ray-Coquard I, Pfisterer J. Role of surgical outcome as prognostic factor in advanced epithelial ovarian cancer: a combined exploratory analysis of 3 prospectively randomized phase 3 multicenter trials: by the Arbeitsgemeinschaft Gynaekologische Onkologie Studiengruppe Ovarialkarzinom (AGO-OVAR) and the Groupe d’Investigateurs Nationaux Pour les Etudes des Cancers de l’Ovaire (GINECO). Cancer. 2009;115:1234–44. https://doi.org/10.1002/cncr.24149 (PMID: 19189349).
Ghirardi V, Moruzzi MC, Bizzarri N, et al. Minimal residual disease at primary debulking surgery versus complete tumor resection at interval debulking surgery in advanced epithelial ovarian cancer: a survival analysis. Gynecol Oncol. 2020;157:209–13. https://doi.org/10.1016/j.ygyno.2020.01.010 (Epub 15 Jaunary 2020 PMID: 31952843).
Grimm C, Harter P, Alesina PF, et al. The impact of type and number of bowel resections on anastomotic leakage risk in advanced ovarian cancer surgery. Gynecol Oncol. 2017;146:498–503. https://doi.org/10.1016/j.ygyno.2017.06.007 (Epub 10 January 2017 PMID: 28610745).
Kverneng Hultberg D, Svensson J, Jutesten H, et al. The impact of anastomotic leakage on long-term function after anterior resection for rectal cancer. Dis Colon Rectum. 2020;63:619–28. https://doi.org/10.1097/DCR.0000000000001613 (PMID: 32032197).
Nally DM, Kavanagh DO, Winter DC. Close rectal dissection in benign diseases of the rectum: a review. Surgeon. 2019;17:119–26. https://doi.org/10.1016/j.surge.2018.06.002 (Epub 18 July 2018 PMID: 30031668).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
DISCLOSURE
The authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Supplementary material 1 (MP4 270690 kb)
Rights and permissions
About this article
Cite this article
Rosati, A., Vargiu, V., Santullo, F. et al. Rectosigmoid Mesorectal-Sparing Resection in Advanced Ovarian Cancer Surgery. Ann Surg Oncol 28, 6721–6722 (2021). https://doi.org/10.1245/s10434-021-09651-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-09651-2