Abstract
Background
Guidelines recommend surgical excision of atypical ductal hyperplasia (ADH) due to the concern of undersampling a potential malignancy on core needle biopsy (CNB). The purpose of this study was to determine clinical, radiological and pathological variables associated with ADH upstaging to cancer and to develop a predictive risk calculator capable of identifying women who have a low oncological risk of upstaging.
Methods
A prospectively collected database from a tertiary breast referral center was analyzed for women diagnosed with ADH on CNB between January 2013 to December 2017 who underwent surgical excision. CNB and surgical pathology reports were examined to determine rate of upstaging. The association between clinical, radiological and pathological variables were evaluated using regression analysis to determine predictors of ADH upstaging to cancer. Significant variables (p ≤ 0.05) identified on univariate analysis were assigned a score of “1” and were included in the ADH upstaging risk calculator.
Results
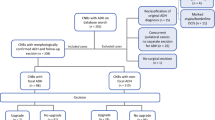
A total of 1986 patients underwent surgery for a high-risk lesion. We identified 318 (16.0%) patients who had ADH identified on their CNB who underwent surgery—of which 290 were included in our study. The upstage rate was 24.8%. Five variables were associated with upstaging and included in our calculator: (1) lesion > 5 mm on ultrasound; (2) lesion > 5 mm on mammogram; (3) one or more “high-risk” lesion(s) on CNB; (4) pathological suspicion for cancer and; (5) incomplete removal of calcifications on CNB. Patients with a score of 0 had a 2% risk of being upstaged to cancer and were deemed low risk with 17.2% of patients falling within this category.
Conclusions
Patients with ADH on CNB can be stratified into a low oncological cohort who have a 2% risk of being upstaged to carcinoma. In the future, these select patients may be counselled and potentially offered observation as an alternative to surgery.



Similar content being viewed by others
References
Hartmann LC, Radisky DC, Frost MH, et al. Understanding the premalignant potential of atypical hyperplasia through its natural history: a longitudinal cohort study. Cancer Prev Res (Phila) 2014;7:211–217.
Deshaies I, Provencher, L., Jacob S, et al. Factors associated with upgrading to malignancy at surgery of atypical ductal hyperplasia diagnosed on core biopsy. Breast. 2011;20:50–55.
Salagean ED, Slodkowska E, Nofech-Mozes S, et al. Atypical ductal hyperplasia on core needle biopsy: Development of a predictive model stratifying carcinoma upgrade risk on excision. Breast J. 2019;25(1):56-61.
Mooney KL, Bassett LW, Apple SK. Upgrade rates of high-risk breast lesions diagnosed on core needle biopsy: a single-institution experience and literature review. Mod Pathol. 2016;29(12):1471–1484.
John M. Eisenberg Center for Clinical Decisions and Communications Science: Core Needle Biopsy for Breast Abnormalities. Rockville (MD): Agency for Healthcare Research and Quality (US); 2007-. AHRQ Comparative Effectiveness Reviews. 2016 May 26.
Khoury T, Chen X, Wang D, et al. Nomogram to predict the likelihood of upgrade of atypical ductal hyperplasia diagnosed on a core needle biopsy in mammographically detected lesions. Histopathology. 2015;67:106–120.
Peña A, Shah SS, Fazzio RT, et al. Multivariate model to identify women at low risk of cancer upgrade after a core needle biopsy diagnosis of atypical ductal hyperplasia. Breast Cancer Res Treat. 2017; 164:295–304.
Nguyen CV, Albarracin CT, Whitman GJ, et al. Atypical ductal hyperplasia in directional vacuum-assisted biopsy of breast microcalcifications: Considerations for surgical excision. Ann Surg Oncol. 2011;18(3):752–761.
Menen RS, Ganesan N, Bevers T, et al. Long-Term safety of observation in selected women following core biopsy diagnosis of atypical ductal hyperplasia. Ann Surg Oncol. 2017;24(1):70–76.
Allison KH, Eby PR, Kohr J, et al. Atypical ductal hyperplasia on vacuum-assisted breast biopsy: suspicion for ductal carcinoma in situ can stratify patients at high risk for upgrade. Hum. Pathol. 2010;42; 41–50.
Uzan, C., Mazouni, C., Ferchiou, M. et al, A model to predict the risk of upgrade to malignancy at surgery in atypical breast lesions discovered on percutaneous biopsy specimens. Ann Surg Oncol. 2013;20:2850–2857.
Adrales G, Turk P, Wallace T, et al. Is surgical excision necessary for atypical ductal hyperplasia of the breast diagnosed by Mammotome? Am J Surg. 2000;180:313–5.
Ko E, Han W, Lee JW, et al. Scoring system for predicting malignancy in patients diagnosed with atypical ductal hyperplasia at ultrasound-guided core needle biopsy. Breast Cancer Res Treat. 2008;112:189–195.
D’Orsi CJ, Sickles EA, Mendelson EB, et al. ACR BI-RADS® Atlas, Breast Imaging Reporting and Data System. Reston, VA, American College of Radiology; 2013.
Bendifallah S, Defert S, Chabbert-Buffet N, et al: Scoring to predict the possibility of upgrades to malignancy in atypical ductal hyperplasia diagnosed by an 11-gauge vacuum-assisted biopsy device: An external validation study. Eur J Cancer. 2012;48:30-36.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures and Sources of Financial Support
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lustig, D.B., Guo, M., Liu, C. et al. Development and Prospective Validation of a Risk Calculator That Predicts a Low Risk Cohort for Atypical Ductal Hyperplasia Upstaging to Malignancy: Evidence for a Watch and Wait Strategy of a High-Risk Lesion. Ann Surg Oncol 27, 4622–4627 (2020). https://doi.org/10.1245/s10434-020-08881-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-020-08881-0