Abstract
Background
In primary aldosteronism (PA), lateralized aldosterone excess can be treated with aldosterone antagonists or surgery, which raises the question as to whether surgery or medications should be the preferred management. A difference in required patient follow-up/clinic resource utilization might provide a surrogate estimate of the comparative outcome efficacy of medical versus surgical therapy.
Methods
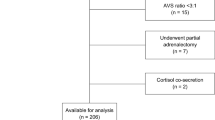
From a retrospective review of our adrenal vein sampling (AVS) database June 2005 to August 2011, we chose all patients with PA who were surgical candidates and investigated with AVS. There were 77 subjects; 38 (with aldosteronoma) had unilateral adrenalectomy, and 39 (7 aldosteronoma and 32 hyperplasia) were treated with primary medical therapy. After AVS, patients with nonsurgical disease immediately started mineralocorticoid antagonists and follow-up measured from the AVS date. Surgical patients were seen in the clinic immediately after hospital discharge and follow-up measured from the operative date. Target BP was <140/90 before discharge to the community.
Results
Total follow-up ranged from 1 to 55 months, and 4 subjects were lost to follow-up. Mean follow-up in the medical and surgical groups was 13.4 versus 6.5 months (p < 0.004). There was a trend toward more clinic visits for the medical group (7.0 vs 5.2, p = 0.17).
Conclusions
Most PA patients can be managed by medical or surgical approaches. Medically treated patients require much longer-term follow-up to manage their condition, whereas most surgical patients can be successfully discharged shortly after surgery. When possible, surgical management may represent a more expeditious means of treating PA.
Similar content being viewed by others
References
Rossi GP, Bernini G, Caliumi C, Desideri G, Fabris B, Ferri C, et al. A prospective study of the prevalence of primary aldosteronism in 1,125 hypertensive patients. J Am Coll Cardiol. 2006;48:2293–3000.
Nishikawa T, Saito J, Omura M. Prevalence of primary aldosteronism: should we screen for primary aldosteronism before treating hypertensive patients with medication? Endocrine J. 2007;54:487–95.
Alvarez-Madrazo S, Padmanabhan S, Mavosi BM, Watkins H, Avery P, Wallace AM, et al. Familial and phenotypic associations of the aldosterone–renin ratio. J Clin Endocrinol Metab. 2009;94:4324–33.
Padfield, PL. Prevalence and role of a raised aldosterone to renin ratio in the diagnosis of primary aldosteronism: a debate on the scientific logic of the use of the ratio in practice. Clin Endocrinol (Oxf). 2003;59:422–6.
Mahmud A, Mahgoub M, Hall M, Feely J. Does aldosterone to renin ratio predict the antihypertensive effect of the aldosterone antagonist spironolactone? Am J Hypertens. 2005;18:1631–35.
Sartori M, Calo LA, Mascagna V, Realdi A, Macchini L, Ciccariello L, et al. Aldosterone and refractory hypertension: a prospective cohort study. Am J Hypertens. 2006;19:373–9.
Zarnegar R, Young WF, Lee J, Sweet MP, Kebebew E, Farley DR, et al. The aldosteronoma resolution score: predicting complete resolution of hypertension after adrenalectomy for aldosteronoma. Ann Surg. 2008;247:511–8.
Jeunemaitre X, Chatellier G, Kreft-Jais C, Charru A, DeVries C, Plouin PF, et al. Efficacy and tolerance of spironolactone in essential hypertension. Am J Cardiol. 1987;60:820–5.
Karagiannis A, Tziomalos K, Papageorgiou A, Kakafika AI, Pagourelias ED, Anagnostis P, et al. Spironolactone versus eplerenone for the treatment of idiopathic hyperaldosteronism. Expert Opin Pharmacother. 2008;9:509–15.
Catena C, Colussi GL, Lapenna R, Nadalini E, Chiuch A, Gianfagna P, et al. Long term cardiac effects of adrenalectomy or mineralocorticoid antagonists in patients with primary aldosteronism. Hypertension. 2007;50:911–8.
Ahmed AH, Gordon RD, Sukor N, Pimenta E, Stowasser M. Quality of life in patients with bilateral primary aldosteronism before and during treatment with spironolactone and/or amiloride, including a comparison with our previously published results in those with unilateral disease treated surgically. J Clin Endocrinol Metab. 2011;96:2904–11.
Kline GA, Harvey A, Jones C, Hill MH, So B, Scott-Douglas N, et al. Adrenal vein sampling in primary aldosteronism: final diagnosis depends upon which interpretation rule is used. Int Urol Nephrol. 2008;40:1035–43.
Favia G, Lumachi F, Scarpa V, D’Amico DF. Adrenalectomy in primary aldosteronism: a long term follow up study in 52 patients. World J Surg. 1992;16:680–4.
Siren J, Valimaki M, Huikuri K, Sivula A, Voutilainen P, Haapiainen R. Adrenalectomy for primary aldosteronism: long term follow up study in 29 patients. World J Surg. 1998;22:418–22.
Meyer A, Brabant G, Behrend M. Long term follow up after adrenalectomy for primary aldosteronism. World J Surg. 2005;29:155–9.
Catena C, Colussi GL, Nadalini E, Chiuch A, Baroselli S, Lapenna R, et al. Cardiovascular outcomes in patients with primary aldosteronism after treatment. Arch Int Med. 2008;168:80–5.
Radley DC, Schoen C. Geographic variation in access to care: the relationship with quality. N Engl J Med. 2012;367:3–6.
Sywak M, Pasieka JL. Long term follow up and cost benefit of adrenalectomy in patients with primary hyperaldosteronism. Br J Surg. 2002;89:1587–93.
CONFLICT OF INTEREST
The authors have nothing to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kline, G.A., Pasieka, J.L., Harvey, A. et al. Medical or Surgical Therapy for Primary Aldosteronism: Post-treatment Follow-up as a Surrogate Measure of Comparative Outcomes. Ann Surg Oncol 20, 2274–2278 (2013). https://doi.org/10.1245/s10434-013-2871-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-013-2871-3