Abstract
We hypothesized that nitric oxide (NO) production by the fetal ductus arteriosus is limited because of low fetal PO2, but that at neonatal PO2, NO might be an important regulator of ductus arteriosus tone. We exposed isolated rings of fetal lamb ductus arteriosus to elevated PO2. L-NG-nitro-L-arginine methyl ester (L-NAME), an inhibitor of nitric oxide synthase (NOS), and methylene blue and 6-anilino-5,8-quinolinedione (LY83583), inhibitors of guanylate cyclase, produced constriction of the ductus arteriosus. When ductus arteriosus rings were exposed to low PO2, L-NAME had no effect, and methylene blue and LY83583 had only a small effect on ductus arteriosus tone. Sodium nitroprusside and calcium ionophore A23187 relaxed ductus arteriosus rings more than aortic rings, and relaxed ductus arteriosus rings from immature fetuses more than those from late gestation fetuses. In contrast, ductus arteriosus rings from both early and late gestation were equally sensitive to 8-bromo-cGMP. By both reverse transcriptase-polymerase chain reaction and immunohistochemistry, endothelial cell NOS and inducible calcium-independent NOS, but not nerve cell NOS, were detected in the ductus arteriosus. Inducible NOS was expressed only by endothelial cells lining the ductus arteriosus lumen; in contrast, endothelial cell NOS was expressed by both luminal and vasa vasorum endothelial cells. The role of inducible NOS in the ductus arteriosus is uncertain because the potency of a specific inducible NOS inhibitor in constricting the ductus arteriosus was negligible compared with that of an endothelial cell NOS inhibitor. We speculate that NO may be an important regulator of ductus arteriosus tone at high but not low PO2. The endothelial cell NOS isoform found in vasa vasorum may be an important source of NO because removal of ductus arteriosus luminal endothelium only partially blocks the effects of L-NAME, methylene blue, and LY83583.
Similar content being viewed by others
Main
The endothelium-dependent relaxing factor NO appears to regulate tone in most vascular beds(1). NO relaxes vascular smooth muscle through intracellular processes that are both dependent(2) and independent of cGMP(3). NO is formed from L-arginine by the enzyme NOS. Several isoforms of NOS have been purified and cloned. These include the calcium-dependent isoforms (isolated from nerve and endothelial cells), ncNOS and ecNOS and the inducible calcium-independent isoform (iNOS)(4–7). All three isoforms of NOS can be expressed in large blood vessels(8–11).
The importance of the endothelium and NO in regulating vascular tone is less clear in the ductus arteriosus. Coceani et al.(12) reported that bradykinin (which releases NO in other blood vessels) relaxed the lamb ductus arteriosus in vitro and that this effect depended on the presence of an intact endothelium. They also found that inhibitors of both NOS and cGMP contracted the ductus in vitro; however, the endothelial site for NO production was put into doubt when they found that the presence of an intact endothelium was not required for these effects to be seen(12). In contrast with the in vitro studies, those performed in vivo failed to demonstrate a role for NO in regulation of the fetal ductus arteriosus. Competitive inhibitors of NOS, when infused directly into the fetus, cause systemic and pulmonary hypertension, but have no effect on ductus arteriosus tone(13, 14). On the other hand, despite the lack of effect of NOS inhibitors on the ductus, methylene blue, an inhibitor of soluble guanylate cyclase, has been reported to constrict the fetal ductus in vivo(15).
We hypothesized that although NO might be constitutively produced by the ductus arteriosus under the normoxic conditions of postnatal life, its production might be suppressed by the low oxygen environment of the fetus. We also hypothesized that NO production in the ductus may not be limited to the luminal endothelium, but may depend on other NOS isoforms or other cell sources within the ductus wall. In the following studies, we examined the effects of different conditions of oxygenation and the effects of fetal maturation on ductus responsiveness to NO; we also compared the ductus with the aorta.
METHODS
Fetal lambs (mixed Western breed, between 60 and 139 d of a 145-d term gestation) were delivered by cesarean section. The ewe was anesthetized with a constant i.v. infusion of ketamine-HCl and diazepam throughout the procedure. The fetus was given ketamine-HCl (30 mg/kg intramuscularly) before rapid exsanguination. These procedures were approved by the Committee on Animal Research at the University of California, San Francisco. The ductus arteriosus was dissected free of loose adventitial tissue and divided into 1-mm thick rings that were placed in separate 10-mL organ baths and kept in a dark room, as we have described previously(16). Throughout the experiment, the rings were suspended between two stainless steel hooks at 38°C in a modified Krebs solution (in mM): NaCl, 118; KCl, 4.7; CaCl2, 2.5; MgSO4, 0.9; KH2PO4,1; glucose, 11.1;, NaHCO3, 23) equilibrated with 5% CO2 (pH 7.4), balance 30% O2/65% N2 or balance 95% N2. The bath solution was changed every 20 min. Both the small bath volume and the protocol used for changing the bath solution were designed to maximize the detection of endogenously produced vasodilators. Our intent was to have the vasodilators accumulate in the bath solution rather than to wash them out during a more rapid perfusion. That way their functional presence could be detected by monitoring the contractile effects of their inhibitors. Isometric responses of circumferential tension were measured by Grass FT03C force transducers (Grass Instruments, Quincy, MA). Each of the rings was stretched to an initial length, which results in a maximal contractile response to increases in oxygen tension(17). Initially the rings were stretched during a 15-min interval in medium equilibrated with fetal PO2 20-34 mm Hg, 0.15-0.26 kPa (starting tension). The bath solution then was bubbled with either the same low PO2 gas (26 ± 5 mm Hg, 0.20 ± 0.04 kPa, [horizontal bar over]m ± SD) or with 30% O2/65% N2/5% CO2 (to a PO2 of 175-200 mm Hg, 1.31-1.50 kPa) until the tension reached a new plateau (approximately 90-120 min). Indomethacin 5.6 × 10-6 M then was added to the bath solution, and the rings were allowed to reach a new steady-state tension over the next 60-90 min. We have previously shown that this concentration of indomethacin completely inhibits prostaglandin E2 and I2 production in the ductus(16, 18). Indomethacin was replaced after each change of bathing media for the duration of the experiment. After indomethacin, either an antagonist of NO synthesis [L-NAME(19); L-NIL, a selective inhibitor of iNOS(20); L-NA, a selective inhibitor of the calcium-dependent NOS isoforms(21)] or an inhibitor of soluble guanylate cyclase [methylene blue(22–24) or LY83583(25)] was added to the bath solution. Cumulative dose response curves were performed to determine the effect of the drug on the tissue. An EC50 (the concentration at which 50% of the maximal contractile effect of the drug occurred) was determined from each dose-response curve. In all experiments, we allowed the tension in the rings to reach a new steady state plateau after a drug addition before another experimental agent was added to the bath. After the addition of all contractile drugs, potassium Krebs solution (containing 100 mM KCl substituted for an equimolar amount of NaCl) was used to measure the maximal amount of tension that could be developed by the ductus (maximal contraction).
To determine the sensitivity of the ductus to relaxing agents, the potassium Krebs solution was washed out of the organ bath, and the ductus was precontracted with solution containing indomethacin and either L-NAME, methylene blue, or LY83583. Cumulative dose response curves were performed to determine the effect of a drug on the tissue. An IC50 (the concentration at which 50% of the maximal relaxant effect of the drug occurred) was determined from each dose-response curve. After the addition of all pro-relaxant drugs, the maximal relaxation of each ductus ring was determined by the response to the combination of SNP (10-3 M) and EGTA (10-2 M).
The difference in tensions between the maximal contraction and the maximal relaxation was considered the net active tension developed by the ring (Fig. 1). The difference in tensions between the steady-state tension achieved in 30% oxygen (or low PO2) and the tension at maximal relaxation was considered the initial tension(Fig. 1). The difference in tensions between the indomethacin-induced tension and the steady-state tension achieved in 30% oxygen (or low PO2) was considered the indomethacin tension(Fig. 1). The difference in tensions between the tension after L-NAME and the indomethacin-induced tension was considered the L-NAME tension. The difference in tensions between the tension after methylene blue and the indomethacin-induced tension was considered the methylene blue tension. The difference in tensions between the tension after LY83583 and the indomethacin-induced tension was considered the LY83583 tension (Fig. 1). Changes in tension for each experimental condition were expressed as a percent of net active tension. The net active tension was always greater than the difference in tension between the maximal contraction and the starting tension by 12 ± 15% (p < 0.05, n = 9). This indicates that the ductus rings were actively contracting even at the time of their initial mounting in the organ bath. After the experiment, the rings were removed from the baths and blotted dry, and their wet weights were determined.
In some experiments, 1.5-mm thick rings of descending aorta were studied and compared with rings of ductus arteriosus from the same fetus. In some experiments, rings of ductus arteriosus or aorta were compared with adjacent rings from the same vessel, the luminal endothelium of which had been removed by rubbing the intimal surface with a rounded wood Q-tip applicator (Sherwood Medical, St. Louis, MO). The completeness of endothelial removal was confirmed at the end of the experiment by sectioning the entire ring and staining it for vWF (see below).
Chemicals. The following compounds were added to the bath solution: L-NAME (Sigma Chemical Co., St. Louis, MO), L-NA (Sigma Chemical Co.), L-NIL (Cayman Chemical Co., Ann Arbor, MI), methylene blue (Sigma Chemical Co.), LY83583 (Biomol, Plymouth Meeting, PA), L-arginine (Sigma Chemical Co.), 8-Br-cGMP (Sigma Chemical Co.), SNP (Sigma Chemical Co.), calcium ionophore A23187 (Sigma Chemical Co.), SNAP (Biomol), EGTA (Sigma Chemical Co.), and ET-1 (Sigma Chemical Co.). Indomethacin was prepared in ethanol (15 mg/mL). A23187 was prepared in DMSO (5 mg/mL). LY83583 was prepared in ethanol (5 mg/mL). The final concentration of ethanol or DMSO did not affect tissue contractility. All other compounds were dissolved directly in Krebs solution. Preparation of methylene blue was performed in the dark to minimize formation of reactive O2 species(26). Except where noted, the maximal concentration of an antagonist (determined in preliminary experiments) was used, e.g. indomethacin 5.6 × 10-6 M, L-NAME 3 × 10-5 M, methylene blue 3 × 10-5 M, and LY83583 3 × 10-5 M.
Statistics. Statistical analysis of unpaired and paired data were performed by the appropriate t test. When more than one comparison was made, Bonferroni correction was used. Nonparametric data were compared with a paired sign test. Values are expressed as mean ± SD. Drug doses refer to their final molar concentration in the bath.
RT-PCR amplification. Total cellular RNA from ductus arteriosus or aorta was prepared using a RNA isolation kit (Purescript, Gentra Systems, Inc., Minneapolis, MN). Fifteen micrograms of purified total RNA were used for cDNA synthesis. The RT reaction was carried out in a 30-μL volume at 42°C using Superscrit II (Bethesda Research Laboratories, Gaithersburg, MD). One-third of the RT reaction was used for PCR. The round one PCR was carried out in a 100-μL mixture containing 20 mM Tris-HCl, pH 8.4, 50 mM KCl, 1.5 mM MgCl2, 0.2 mM each of dATP, dCTP, dGTP, and dTTP, 1 μM of each primer, and 5 U of Taq DNA polymerase (Bethesda Research Laboratories). The primers used for ecNOS(5′-CCTCCGGAGGGGCCCAAGTTCCCTCGC-3′ and 5′-CACGTCGAAGCGGCCGTTTCCGGGGGT-3′)(27), iNOS (5′-TTTCAGCACATCTGCAGACACATATTT-3′ and 5′-CTATGGAGCACAGCCACATTGATCACC-3′)(28), and ncNOS (5′-CTCATCTATGGCGCCAAGCATGCCTGG-3′ and 5′-AGTTGTCACAGTAGTCACGGACGCCCG-3′)(29) were synthesized by The Midland Certified Reagent Co. (Midland, TX). The reaction mixture was heated to 94°C for 5 min; this was followed by 40 amplification cycles consisting of 30 s of denaturation and annealing at 94°C and 75°C, respectively, and a 1-min elongation step at 72°C. A final 10-min extension was carried out at 72°C after completion of the last cycle. All PCRs were carried out in a Perkin-Elmer thermal cycler. The amplified fragments were sequenced using cyclist Exo-Pfu DNA sequencing kit (Stratagene, La Jolla, CA).
Immunohistochemistry. Tissue was fixed for 16 h at 4°C in fresh 4% paraformaldehyde before paraffin embedding. Immunohistochemical methods were similar to those we have previously reported(30). Briefly, 5-μm thick sections were incubated in PBS with 0.2% (vol/vol) Tween 20 for 15 min, followed by incubation with 10% normal goat serum to block nonspecific binding. Two separate antibodies were used to detect ecNOS, a mouse MAb clone 3 (Transduction Laboratory, Lexington, KY), and a rabbit polyclonal antibody(31). Three separate antibodies were used to detect iNOS (two distinct mouse MAb, clone 6 and clone 54 (Transduction Laboratory), and a rabbit polyclonal antibody(32). A rabbit polyclonal antibody was used to detect ncNOS(33). Antibodies were tested by Western analysis and found to be specific for the NOS isoform that they were prepared against and not to cross-react with either of the other two isoforms (data not shown). Control sections were incubated with similar concentrations of either mouse or rabbit IgG (Sigma Chemical Co.). Antibodies were diluted with blocking serum containing bovine serum albumen (1 mg/mL) and applied to the sections overnight at 4°C. The following day the sections were incubated with goat anti-rabbit or anti-mouse secondary antibody (Vector Laboratories, Burlingame, CA) for 60 min. Endogenous peroxidase was quenched by incubation with 0.3%(vol/vol) aqueous hydrogen peroxide. The sections were then exposed to avidin-biotin complex (ABC Elite kit; Vector Laboratories, Burlingame, CA) and reacted with diaminobenzidine. Finally, sections were counterstained with hematoxylin.
For identification of vWF, a similar protocol to the one described above was used. In addition, sections were treated with trypsin [GIBCO BRL, Grand Island, NY; 0.025% (weight/100 mL)] in PBS for 10 min before the addition of rabbit polyclonal antibody to vWF (Dako, Carpenteria, CA). Assays for any given antibody were reproduced on three separate occasions.
RESULTS
In the presence of 30% oxygen (PO2 175-200 mm Hg, 1.31-1.50 kPa), rings of ductus arteriosus contracted spontaneously to a tension that was 34± 10% of the rings' net active tension (Fig. 2). Indomethacin caused an additional increase in tension (23 ± 15% net active tension). When L-arginine, the immediate precursor of NO, was added to the oxygen- plus indomethacin-contracted ductus rings, there was no change in tension (0 ± 0% net active tension). In contrast, when L-NAME, an antagonist of NO synthesis, was added to the oxygen- plus indomethacin-contracted rings, there was a concentration-dependent increase in tension (Fig. 3). L-Arginine completely reversed the L-NAME-induced contraction. The magnitude of the maximal indomethacin-induced contraction was not significantly different from that of the maximal L-NAME-induced contraction. Both L-NA (the selective inhibitor of the calcium-dependent NOS isoforms) and L-NIL (the selective inhibitor of iNOS) also contracted the ductus; however, L-NA was 50 times more potent than L-NIL (Fig. 3).
Inhibitors of prostaglandin and NO production contract the fetal ductus only at elevated PO2. All tensions expressed as a percentage of net active tension; [horizontal bar over]m ± SD,n = 9, gestation = 121 ± 19 d. *p < 0.05,**p < 0.01; value in 30% oxygen vs low oxygen value. Starting tension (30% O2) = 4.9 ± 2.6 g. Starting tension (low PO2) = 4.3 ± 2.1 g.
Response of ductus arteriosus rings to three inhibitors of NOS: L-NA, L-NAME, and L-NIL. Rings of ductus arteriosus from eight fetuses(129 ± 3 d gestation) were precontracted with 30% oxygen and indomethacin before performing a dose response with either L-NA, L-NAME, or L-NIL. All tensions are expressed as a percentage of net active tension([horizontal bar over]m ± SD). EC50 is the concentration at which 50% of the maximal contractile effect of the drug occurred. *p< 0.01 EC50 (L-NIL) vs EC50 (L-NA or L-NAME). Abscissa = log of molar concentrations. L-NA dose response: starting tension = 6.2 ± 0.5 g; net active tension = 25.5 ± 2.7 g; L-NAME dose response: starting tension = 6.0 ± 1.0 g, net active tension = 21.3± 3.0 g; L-NIL dose response: starting tension = 7.4 ± 1.8 g, net active tension = 24.4 ± 3.0 g.
The responses of the ductus to indomethacin and L-NAME were quite different when the rings were incubated with medium equilibrated in low PO2 (26± 5 mm Hg, 0.20 ± 0.04 kPa, n = 9). We have shown previously that, during equilibration with low PO2, prostaglandin production by the ductus arteriosus is inhibited(18). As the prostaglandin concentration in the bath solution decreases, ductus tension increases(18, 34). In the current experiments, rings of ductus incubated in low PO2 contracted to a tension that was greater than that achieved when the rings were incubated in 30% oxygen (Fig. 2). As we have shown previously(18), indomethacin had no contractile effect on ductus rings incubated in low PO2. Both L-NAME and L-arginine also had no effect on the contractile tone of ductus rings that were incubated in low PO2. The lack of effect of L-NAME at low PO2 was not due to a loss of sensitivity of the tissue to NO because the NO donor SNP had the same relaxant effect on L-NAME plus indomethacin-exposed rings, whether they were incubated in low or 30% oxygen-equilibrated media (IC50 (SNP) low PO2 = 3 ± 3 × 10-8 M versus IC50(SNP) 30% O2 = 2 ± 2 × 10-8 M). The final tension achieved by rings that were exposed to both indomethacin and L-NAME, in the presence of low PO2, was significantly less (60 ± 16% net active tension) than that achieved in rings exposed to the same two inhibitors, in the presence of 30% O2 (71 ± 15%, p < 0.05).
Inhibitors of soluble guanylate cyclase [methylene blue(22–24) and LY83583(25)], contracted the 30% oxygen-exposed ductus in a dose-dependent manner (methylene blue, EC50 = 2.8 ± 1.6 × 10-6 M, n = 4; LY83583, EC50 = 6.7 ± 3.3× 10-7 M, n = 6) (Table 1). Methylene blue and LY83583 contracted the ductus to the same extent as L-NAME and indomethacin (Table 1). Both the NOS inhibitor, L-NAME, and the guanylate cyclase inhibitors, methylene blue and LY83583, appeared to affect the same pathway in the ductus, because both methylene blue(n = 4) and LY83583 (n = 6) completely blocked any further contraction of the ductus by L-NAME; conversely, L-NAME completely blocked any further contraction of the ductus by methylene blue (n = 4) or LY83583 (n = 6) (data not shown). On the other hand, the contractile responses of L-NAME, methylene blue, and LY83583 on the ductus were not affected by the presence or absence of indomethacin (n = 3) (data not shown).
Although the NOS inhibitor, L-NAME, and the soluble guanylate cyclase inhibitors, methylene blue and LY83583, seem to work through the same pathway in ductus exposed to 30% oxygen, their actions diverged when ductus rings were incubated in low PO2. Low PO2 completely blocked the effects of L-NAME on ductus tone (Fig. 2); in contrast, the effects of methylene blue and LY83583 were only partially inhibited by low PO2(Table 1). Low PO2 had no effect on the sensitivity of the ductus to 8-Br-cGMP (IC50 (8-Br-cGMP) low PO2= 1.2 ± 0.3 × 10-5 M versus IC50(8-Br-cGMP) 30% O2 = 1.2 ± 0.5 × 10-5 M).
Removal of the luminal endothelium did not alter the effects of indomethacin on the ductus arteriosus (Table 2). This has been reported previously(12). Similarly, removal of the luminal endothelium did not alter the sensitivity of the rings to SNP(IC50 (SNP), intact = 3 ± 3 × 10-8 M versus denuded = 3 ± 2 × 10-8 M) or to 8-Br-cGMP(IC50 (8-Br-cGMP), intact = 1.4 ± 0.3 × 10-5 M versus denuded = 1.2 ± 0.3 × 10-5 M). However, removal of the luminal endothelium of the ductus arteriosus did decrease the contractile effects of L-NAME, methylene blue, and LY83583, but by only 27-37%(Table 2).
Ductus rings from immature fetuses were about six times more sensitive to the vasodilating effects of NO donors, like SNP and SNAP, than rings from late gestation fetuses (Fig. 4). The increased sensitivity early in gestation was not due to an increased sensitivity to cGMP, because the IC50 for 8-Br-cGMP was the same at both gestational ages (Fig. 4). However, in spite of the increased sensitivity of the immature ductus to NO donors, the contraction produced by inhibiting NO production with L-NAME was not greater in the immature ductus (15 ± 6% of net active tension, n = 15) when compared with the more mature ductus (24 ± 8% of net active tension, n = 16).
The immature ductus is more sensitive than the mature ductus to NO relaxation but equally sensitive to 8-Br-cGMP relaxation. Ductus arteriosus rings from 15 fetuses <105 d (93 ± 12 d) and 26 fetuses>125 d (133 ± 5 d) were precontracted with either 30% oxygen + indomethacin + L-NAME (to inhibit endogenous NO production for SNP and SNAP experiments) or 30% oxygen + indomethacin + LY83583 (to inhibit endogenous cGMP production for 8-Br-cGMP experiment). Net induced tension is the difference between the tension after precontraction and the minimal tension produced in the ring (after SNP (10-3 M) plus EGTA (10-2 M)).*p < 0.01 values from fetuses >125 d vs those<105 d gestation. Starting tensions: <105 d = 4.5 ± 1.4,n = 23 rings; >125 d = 5.8 ± 1.4, n = 32 rings. Relaxation is expressed as a negative (-) change in tension. Abscissa = log of molar concentrations.
When we compared the ductus with the aorta (Fig. 5), we found that the ductus was both more sensitive to, and more completely relaxed by, the NO donor, SNP (Fig. 5). In these experiments, the aortic rings were precontracted with either 25 × 10-3 M potassium Krebs solution or ET-1 (10-7 M), because they had no spontaneous tension, nor did they contract when exposed to indomethacin or LY83583. To compare the ductus responses with aortic responses, the ductus rings were also precontracted with potassium Krebs solution or ET-1. Rings contracted by excess K+ were more resistant to NO-induced relaxation than those contracted by ET-1 (Fig. 5). This has been noted previously in other vessels(35). Although K+-contracted rings were less sensitive to SNP than were ET-1-contracted rings, the increased sensitivity of the ductus, compared with the aorta, remained the same, whichever agent was used to contract the tissues. In contrast, rings of ductus arteriosus were as sensitive to the dilating effects of 8-Br-cGMP as were aortic rings (Fig. 5).
The ductus arteriosus is more sensitive than the aorta to NO relaxation but equally sensitive to 8-Br-cGMP relaxation. Ductus and aorta rings were precontracted with either oxygen + indomethacin + ET-1 or oxygen + indomethacin + K+ (see “Results”). For the SNP dose-response curves, L-NAME was added to inhibit endogenous NO production. For the 8-Br-cGMP dose-response curve, LY83583 was added to inhibit endogenous cGMP production. Net induced tension is the difference between the tension developed after K+ or ET-1 and the minimal tension produced in the ring. For the ductus, the minimal tension was that after SNP, because the ring always relaxed below the starting tension; for the aorta, the minimal tension was the starting tension, because SNP did not relax the ring back to the starting tension. SNP dose-response in ET-1: starting tensions, ductus = 6.6± 1.0 g; aorta = 6.8 ± 0.9 g. SNP dose-response in K+, starting tensions, ductus = 5.7 ± 1.1 g; aorta = 5.7 ± 2.1 g. 8-Br-cGMP dose-response in K+, starting tensions, ductus = 6.3 ± 1.4 g; aorta = 5.7 ± 1.2 g. *p < 0.05, ductus vs aorta. Relaxation is expressed as a negative (-) change in tension. Abscissa = log of molar concentrations.
We used the calcium ionophore, A23187, to evaluate calcium-dependent generation of NO by the endothelium of both the ductus and the aorta(Table 3). A23187 relaxed both the ductus and the aorta. However, the ductus was relaxed more by A23187 than was the aorta(Table 3). L-NAME inhibited the A23187-induced relaxation of both tissues. L-NAME, by itself, had no effect on the aorta unless it had been precontracted with ET-1. When the aorta was precontracted with ET-1, L-NAME (3 × 10-5 M) produced a contraction that was only 6± 1% of the net active tension. In contrast, L-NAME produced a contraction of the ductus that was 15-25% of the net active tension, whether or not the ductus was precontracted with ET-1. Removal of the luminal endothelium inhibited the A23187-induced relaxation of the aorta by 80± 5%; in contrast, A23187-induced relaxation of the ductus was inhibited by only 42 ± 17% (p < 0.05) when the luminal endothelium was removed (Table 3A).
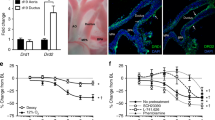
To identify which of the known NOS isoforms were present in the fetal ductus arteriosus and aorta, we used ductus and aorta from two fetal lambs(120 and 128 d of gestation) that were frozen in liquid N2 immediately after dissection. Total cellular RNA was examined by RT-PCR for the expression of ecNOS, iNOS, and ncNOS. In both the ductus and the aorta, the ecNOS and iNOS primers yielded products of the expected size; their identity was confirmed subsequently by sequencing (Fig. 6). The ncNOS primers also amplified a fragment of about 600 bp (data not shown) that was found to be nonspecific upon sequencing.
RT-PCR for ecNOS and iNOS in fetal lamb ductus arteriosus and aorta. RNA samples from tissues were processed for 40 cycles of PCR using primers directed to the cDNA sequence of ecNOS and iNOS, as described in “Methods.” PCR of the primers alone, without template, resulted in no product (data not shown).
We used an antibody against vWF to localize endothelial cells within the fetal ductus arteriosus (Fig. 7). As anticipated, a single layer of endothelial cells lined the ductus lumen. In addition, an extensive network of vasa vasorum both surrounded the muscle (in the adjacent adventitia) and penetrated deep into the muscle media. The density and degree of penetration of the vasa vasorum increased with advancing gestation. In the immature ductus (<105 d of gestation), vasa vasorum mostly were restricted to the outer 25% of the muscle media. In contrast, in the near-term ductus(>135 d of gestation), vasa vasorum arborized throughout 75% of the muscle media (Table 4). In the aorta, vasa vasorum rarely penetrated the muscle media even as the animal approached term.
Vasa vasorum are more prominent in the near-term ductus arteriosus. Endothelial cells are stained brown with vWF antibody.(a) Single endothelial cell layer lines the lumen (L) of a 136-d gestation fetal ductus. Vasa vasorum in the muscle media(arrows). (b) After luminal endothelial cell removal, endothelial cells persist in the vasa vasorum (arrows) of the muscle wall (135-d gestation fetal ductus). Both 136-d gestation aorta (c) and 100-d gestation ductus (d) have a paucity of vasa vasorum(arrows) in the muscle media. Small arrows point to vasa vasorum in the adventitia of the ductus. (Horizontal bar represents μm.)
In the near-term ductus arteriosus, endothelial cells lining both the lumen and the vasa vasorum expressed ecNOS (Fig. 8). After the luminal endothelium was removed, ecNOS expression was limited to the vasa vasorum arborizing through the vessel's muscle media (Fig. 8). The immature ductus and the aorta have a decreased number of vasa vasorum entering their muscle media. As a result, the ecNOS in the immature ductus and aorta appears to be concentrated mostly in the luminal endothelium (Fig. 8).
The near-term ductus arteriosus has ecNOS in its vasa vasorum. The immunostaining results of the two separate antibodies against ecNOS were identical. To conserve space, we present only the results of the mouse MAb (brown staining). Both the luminal endothelial cells(a) and the vasa vasorum (b) (arrows) contain ecNOS [(a) and (b) = fetal ductus, 136-d gestation]. After removal of the luminal endothelial cells (c), ecNOS persists in the endothelial cells of the vasa vasorum [(c) = fetal ductus, 136-d gestation, after tissue bath-contraction study; note the pattern of staining was identical whether the tissue was fixed before or after the contraction experiment]. Both 136-d gestation aorta (d) and 100-d gestation ductus (e) have a paucity of ecNOS-containing vasa vasorum in their muscle media. Small arrows point to vasa vasorum in the adventitia of the 100-d gestation ductus (e). (Horizontal bar representsμm.) L, lumen.
In both the fetal ductus and aorta, endothelial cells lining the vessel's lumen also expressed iNOS (Fig. 9). No other cells of the ductus or aorta (including vasa vasorum endothelial cells) expressed the iNOS isoform (Fig. 9). This pattern of expression was the same whether the tissue was studied immediately after removal from the fetus or after the 8-h in vitro contraction study. The ncNOS isoform was not found in any of the cellular elements of the ductus or aorta (Fig. 9).
Fetal vessels express iNOS but not ncNOS. iNOS: (a-e) The immunostaining results of the three separate antibodies against iNOS were identical. To conserve space, we present only the results of the mouse MAb (clone 54) (brown stain). Luminal endothelial cells of the 136-d gestation fetal ductus (a) and aorta(c) express iNOS. Vasa vasorum (b) (arrows) of the ductus do not express iNOS. After luminal endothelial cell removal(d), there is no iNOS expression in the ductus arteriosus(arrow = vasa vasorum in the muscle media). Ductus from 100-d fetal ductus (e). Small arrows point to the nonstained vasa vasorum in the ductus adventitia (e). (f-h) ncNOS: neither the luminal endothelial cells (f), nor the vasa vasorum(g) (long arrows) or nerves (g) (broad arrows) in the ductus wall, express ncNOS. Adult sheep cerebellum(h) with ncNOS-containing neurons (brown stain)(arrow) is a positive control for ncNOS staining.
DISCUSSION
Our observations clarify some of the apparent discrepancies found among prior studies that examined the role of an endothelium-dependent source of NO in regulating the ductus arteriosus. Prior studies failed to demonstrate a cholinergic-induced release of NO from the ductus arteriosus(36–41). It is possible that earlier studies may have worked with vessel preparations containing a damaged endothelium. On the other hand, some endothelia lack receptors for acetylcholine(35, 42). In preliminary experiments (not presented here), we also observed that cholinergic agents failed to relax the ductus. Therefore, we used the calcium ionophore A23187, which stimulates endothelial-dependent NO production through a nonreceptor-mediated pathway(43). A23187 relaxed both the oxygen-exposed ductus and the aorta. NO increases the release of prostaglandin E2 by increasing both cyclooxygenase and prostaglandin E2 isomerase activities(44–46); however, the action of NO in our study cannot be explained by this mechanism, because all rings were incubated in concentrations of indomethacin that inhibit prostaglandin production(16, 18).
The relaxant effect of A23187 on the ductus was more efficacious than on the aorta (Table 3). This might be due to the increased sensitivity of the ductus to NO (Fig. 5) or to an increased accumulation of NO in the ductus tissue after A23187. It is unlikely that the difference between the two tissues is due to differences in downstream intracellular signaling events because 8-Br-cGMP had a similar effect on both the ductus and the aorta (Fig. 5).
In the presence of elevated PO2, inhibitors of NO (L-NAME, L-NA, and L-NIL) and soluble guanylate cyclase (methylene blue, LY83583) contracted the ductus arteriosus. This occurred even under basal conditions, without the presence of exogenous stimulators of NO production. The contractile effects of these inhibitors were comparable to those of indomethacin. Although methylene blue has other actions (such as generating oxygen free radicals(26, 47) and stimulating α-adrenergic nerves), these appear to be unlikely causes for its effect on the ductus; we have previously shown that free radicals dilate the ductus rather than constrict it(16). Furthermore, no difference in the effect of methylene blue on the ductus was found when the ductus was pretreated with dibenzyline, an α-adrenoreceptor blocker(12).
Using RT-PCR and immunohistochemistry, we demonstrated the presence of two of the NOS isoforms (ecNOS and iNOS) in the ductus wall. Both isoforms were found only in endothelial cells. Although iNOS is present in the tissue, its role in the regulation of ductus tone may not be that significant. The ecNOS inhibitor (L-NA) had a much more potent effect on ductus contractility than did the iNOS inhibitor (L-NIL) (Fig. 3). In addition, although there was no evidence of iNOS in the ductus after denudation of the luminal endothelium (Fig. 9), we still found evidence for significant NO production in the denuded tissue(Tables 2 and 3A). This latter observation can be explained by the persistence of the ecNOS isoform in the denuded ductus wall. In addition to its presence in the luminal endothelium, ecNOS isoform is also expressed by endothelial cells of the vasa vasorum (Fig. 8). The ductus arteriosus is almost completely encircled by vasa vasorum in its adventitia. However, it is unclear what role these vessels play in regulation of ductus tone because NO has poor penetration of the muscle media from the adventitial compartment(48). However, with advancing gestation, there is extensive penetration and arborization of ecNOS-containing vasa vasorum throughout three-quarters of the ductus muscle media (Table 4). The density of vasa vasorum investing a vessel's wall depends on both the thickness of the vessel wall and its oxygen requirements(49). We hypothesize that, in addition to supplying the nutritional needs of blood vessels, the ecNOS-containing vasa vasorum may play an important role in regulating vessel tone.
Both iNOS and ecNOS also were expressed by endothelial cells of the fetal aorta. However, the density of vasa vasorum in the muscle media of the aorta was reduced compared with the ductus. As one might anticipate, the aorta's ability to respond to A23187 was much more dependent on the presence of an intact luminal endothelial layer; removal of luminal endothelial cells from the aorta was associated with a much more pronounced loss of NOS activity than in the ductus (Table 3A).
We have previously shown that the ductus arteriosus of the immature fetus is much more sensitive to the vasodilating effects of the prostaglandins E2 and I2 than is the near-term ductus(50). In the current studies, we found that the immature ductus is also much more sensitive to the vasodilating effects of NO (Fig. 4). In spite of this, L-NAME, the inhibitor of endogenous NO production, has the same contractile effect on the immature as on the near-term ductus. This suggests that there may be less NO produced in the immature ductus in vitro. This would correspond with our observation that the immature ductus has a diminished number of ecNOS-containing vasa vasorum penetrating its muscle media (Fig. 8). Other investigators have observed a similar phenomenon during maturation of the pulmonary vessels (i.e., decreased NO release by fetal vessels compared with newborn vessels)(51). We hypothesize that these observations may also be explained by the increase in ecNOS-containing vasa vasorum that occurs with maturation of the pulmonary artery. This hypothesis does not preclude the possibility that the activity of NOS also changes during gestation, because our studies were designed to examine just the presence of NOS, and not its activity.
Prior studies have shown that prostaglandin production by the ductus is inhibited at low PO2(18, 34). It is therefore not surprising that in the presence of low PO2, indomethacin has no contractile effect on the isolated ductus arteriosus (Fig. 2). The importance of NO in ductus regulation also appears to depend on the surrounding oxygen tension. Under oxygen tensions mimicking those found in the fetus, the ductus is capable of responding to exogenous NO, but is unable to produce NO in vitro(Fig. 2). It is unlikely that, in our experiments, the inability of the ductus rings to produce prostaglandins or NO is due to tissue deterioration during prolonged exposure to low PO2; there is no difference in either the maximal contractile response to K+ or the maximal relaxant response to SNP when ductus rings are examined after either 1 or 8 h of incubation in Low PO2 (our unpublished observations). Similarly, there is no difference in the net active tensions achieved between ductus rings that are incubated in low PO2 or in 30% O2 for 6 h (Fig. 2,Table 1), and finally, although ductus rings incubated in low PO2 do not produce prostaglandins or contract when exposed to indomethacin, they will produce significant amounts of prostaglandins and will develop a significant indomethacin-induced contraction if they are subsequently incubated in high PO2(18).
Our in vitro findings may seem at odds with the observation that indomethacin causes constriction of the fetal ductus in vivo. Our in vitro studies examined the prostaglandins that were produced locally by the ductus. In addition to locally produced prostaglandins, the fetus has high circulating concentrations of prostaglandin E2(52). Prior studies have shown a good correlation between changes in circulating prostaglandin E2 and alterations in ductus patency in the fetus(53). Recent findings strongly support the concept that circulating prostaglandins, rather than those made within the ductus wall, are primarily responsible for maintaining ductus patency in the fetus (S. Chemtob and R. Clyman, unpublished observations).
The studies reported above suggest that, in addition to locally produced prostaglandin E2, NO also may play an insignificant role in maintaining fetal ductus patency in vivo. This hypothesis is consistent with the in vivo findings of Cornfield et al.(13) and Abman et al.(14). Other investigators similarly have found that low oxygen tension suppresses vascular NO production(54–56). However, this has not been uniformly observed(57–59).
Although inhibitors of NO production no longer affect the ductus under conditions of low oxygen tension, inhibitors of cGMP production still contract the ductus in vitro (Table 1). A similar observation has been made in vivo(15). We hypothesize that under conditions of low oxygen tension, other activators of guanylate cyclase (e.g. carbon monoxide produced by heme oxygenase)(60) may play a role in regulating ductus tone. However, once the ductus is exposed to the elevated oxygen tension of postnatal life, there appears to be an increase in NO production, which, in turn, increases smooth muscle cGMP, as we have observed in other transitional fetal vessels(61). After birth, NO probably becomes the dominant pathway for activating cGMP in the ductus, because inhibitors of cGMP production no longer affect the ductus that has been exposed to L-NAME.
The existing evidence from in vitro and in vivo studies leads to the following conclusions and speculations about the role of NO in ductus arteriosus regulation. NO can be synthesized by endothelial cells of both the vasa vasorum and vessel lumen. However, at oxygen tensions found in the fetus, little NO is produced by the ductus arteriosus. Once exposed to the elevated neonatal PO2, NO is produced within the ductus wall. Because the immature ductus is more sensitive to NO-induced vasodilation than the mature ductus, it may have more potent effects in the premature newborn. The left-to-right shunt of oxygenated blood (with its increased shear forces) through the premature patent ductus arteriosus may shift the balance of vasodilators within the wall from one primarily controlled by prostaglandins to one that is strongly influenced by NO; these findings may help to explain why indomethacin becomes less effective in closing the patent ductus arteriosus in the extremely immature infant during the first 10 d after birth(62).
Abbreviations
- NO:
-
nitric oxide
- NOS:
-
nitric oxide synthase
- ecNOS, ncNOS, iNOS:
-
endothelial cell, nerve cell, and inducible calcium-independent isoforms of NOS
- L-NAME:
-
NG-nitro-L-arginine methyl ester
- L-NIL:
-
L-N6-(1-iminoethyl)lysine
- L-NA:
-
L-NG[-nitro-L-arginine]
- LY83583:
-
6-anilino-5,8-quinolinedione
- SNP:
-
sodium nitroprusside
- vWF:
-
von Willebrand factor
- 8-Br-cGMP:
-
8-Bromo-guanosine 3′,5′-cyclic monophosphate
- RT:
-
reverse transcriptase
- PCR:
-
polymerase chain reaction
- SNAP:
-
S-nitroso-N-acetylpenicillamine
- ET-1:
-
endothelin-1
References
Ignarro LJ 1989 Endothelium-derived nitric oxide: actions and properties. FASEB J 3: 31–36.
Moncada S 1992 The 1991 Ulf von Euler Lecture. The L-arginine: nitric oxide pathway. Acta Physiol Scand 145: 201–227.
Bolotina VM, Najibi S, Palacino JJ, Pagano PJ, Cohen RA 1994 Nitric oxide directly activates calcium-dependent potassium channels in vascular smooth muscle. Nature 368: 850–853.
Gross SS, Jaffe EA, Levi R, Kilbourn RG 1991 Cytokine-activated endothelial cells express an isotype of nitric oxide synthase which is tetrahydrobiopterin-dependent, calmodulin-independent and inhibited by arginine analogs with a rank-order of potency characteristic of activated macrophages. Biochem Biophys Res Commun 178: 823–829.
Radomski MW, Palmer RM, Moncada S 1990 Glucocorticoids inhibit the expression of an inducible, but not the constitutive, nitric oxide synthase in vascular endothelial cells. Proc Natl Acad Sci USA 87: 10043–10047.
Schini VB, Busse R, Vanhoutte PM 1994 Inducible nitric oxide synthase in vascular smooth muscle. Arzneim Forsch 44: 432–435.
Busse R, Mulsch A 1990 Calcium-dependent nitric oxide synthesis in endothelial cytosol is mediated by calmodulin. FEBS Lett 265: 133–136.
Bredt DS, Hwang PM, Snyder SH 1990 Localization of nitric oxide synthase indicating a neural role for nitric oxide. Nature 347: 768–770.
Nozaki K, Moskowitz MA, Maynard KI, Koketsu N, Dawson TM, Bredt DS, Snyder SH 1993 Possible origins and distribution of immunoreactive nitric oxide synthase-containing nerve fibers in cerebral arteries. J Cereb Blood Flow Metab 13: 70–79.
Beasley D 1990 Interleukin 1 and endotoxin activate soluble guanylate cyclase in vascular smooth muscle. Am J Physiol 259:R38–R44.
Wood KS, Buga GM, Byrns RE, Ignarro LJ 1990 Vascular smooth muscle-derived relaxing factor (MDRF) and its close similarity to nitric oxide. Biochem Biophys Res Commun 170: 80–88.
Coceani F, Kelsey L, Seidlitz E 1994 Occurrence of endothelium-derived relaxing factor-nitric oxide in the lamb ductus arteriosus. Can J Physiol Pharmacol 72: 82–88.
Cornfield DN, Chatfield BA, McQueston JA, McMurtry IF, Abman SH 1992 Effects of birth-related stimuli on L-arginine-dependent pulmonary vasodilation in ovine fetus. Am J Physiol 262:H1474–H1481.
Abman SH, Chatfield BA, Hall SL, McMurtry IF 1990 Role of endothelium-derived relaxing factor during transition of pulmonary circulation at birth. Am J Physiol 259:H1921–H1927.
Fox JJ, Ziegler JW, Dunbar DI, Halbower AC, Kinsella JP, Abman SH 1996 Role of nitric oxide and cGMP system in regulation of ductus arteriosus tone in ovine fetus. Am J Physiol 271:H2638–H2645.
Clyman RI, Saugstad OD, Mauray F 1989 Reactive oxygen metabolites relax the lamb ductus arteriosus by stimulating prostaglandin production. Circ Res 64: 1–8.
Clyman RI, Mauray F, Wong L, Heymann MA, Rudolph AM 1978 The developmental response of the ductus arteriosus to oxygen. Biol Neonate 34: 177–181.
Clyman RI, Mauray F, Demers LM, Rudolph AM, Roman C 1980 Does oxygen regulate prostaglandin-induced relaxation in the lamb ductus arteriosus?. Prostaglandins 19: 489–498.
Rees DD, Palmer RM, Schulz R, Hodson HF, Moncada S 1990 Characterization of three inhibitors of endothelial nitric oxide synthase in vitro and in vivo. Br J Pharmacol 101: 746–752.
Moore WM, Webber RK, Jerome GM, Tjoeng FS, Misko TP, Currie MG 1994 L-N6-(l-Iminoethyl)lysine: a selective inhibitor of inducible nitric oxide synthase. J Med Chem 37: 3886–3888.
Furfine ES, Harmon MF, Paith JE, Garvey EP 1993 Selective inhibition of constitutive nitric oxide synthase by L-NG-nitroarginine. Biochemistry 32: 8512–8517.
Gruetter CA, Gruetter DY, Lyon JE, Kadowitz PJ, Ignarro LJ 1981 Relationship between cyclic guanosine 3′,5′-monophosphate formation and relaxation of coronary arterial smooth muscle by glyceryl trinitrate, nitroprusside, nitrite and nitric oxide: effects of methylene blue and methemoglobin. J Pharmacol Exp Ther 219: 181–186.
Martin W, Villani GM, Jothianandan D, Furchgott RF 1985 Selective blockade of endothelium-dependent and glyceryl trinitrate-induced relaxation by hemoglobin and by methylene blue in the rabbit aorta. J Pharmacol Exp Ther 232: 708–716.
Katsuki S, Arnold W, Mittal C, Murad F 1977 Stimulation of guanylate cyclase by sodium nitroprusside, nitroglycerin and nitric oxide in various tissue preparations and comparison to the effects of sodium azide and hydroxylamine. J Cyclic Nucleotide Res 3: 23–35.
Mülsch A, Luckhoff A, Pohl U, Busse R, Bassenge E 1989 LY 83583 (6-anilino-5:8-quinolinedione) blocks nitrovasodilator-induced cyclic GMP increases and inhibition of platelet activation. Naunyn-Schmiedebergs Arch Pharmacol 340: 119–125.
Marshall JJ, Wei EP, Kontos HA 1988 Independent blockade of cerebral vasodilation from acetylcholine and nitric oxide. Am J Physiol 255:H847–H854.
Nishida K, Harrison DG, Navas JP, Fisher AA, Dockery SP, Uematsu M, Nerem RM, Alexander RW, Murphy TJ 1992 Molecular cloning and characterization of the constitutive bovine aortic endothelial cell nitric oxide synthase. J Clin Invest 90: 2092–2096.
Lowenstein CJ, Glatt CS, Bredt DS, Snyder SH 1992 Cloned and expressed macrophage nitric oxide synthase contrasts with the brain enzyme. Proc Natl Acad Sci USA 89: 6711–6715.
Bredt DS, Hwang PM, Glatt CE, Lowenstein C, Reed RR, Snyder SH 1991 Cloned and expressed nitric oxide synthase structurally resembles cytochrome P-450 reductase. Nature 351: 714–718.
Tannenbaum JE, Waleh NS, Mauray F, Gold L, Perkett EA, Clyman RI 1996 Transforming growth factor-β protein and Messenger RNA expression is increased in the closing ductus arteriosus. Pediatr Res 39: 427–434.
Ferriero DM, Holtzman DM, Black SM, Sheldon RA 1996 Neonatal mice lacking neuronal nitric oxide synthase are less vulnerable to hypoxic ischemic injury. Neurobiol Dis 3: 64–71.
Riemer RK, Buscher C, Bansal RK, Black SM, He Y, Natuzzi ES 1997 Increased expression of nitric oxide synthase in the myometrium of the pregnant rat uterus. Am J Physiol 35:E1008–E1015.
Black SM, Bedolli MA, Martinez S, Bristow JD, Ferriero DM, Soifer SJ 1995 Expression of neuronal nitric oxide synthase corresponds to regions of selective vulnerability to hypoxia-ischemia in the developing rat central nervous system. Neurobiol Dis 2: 145–155.
Coceani F, Huhtanen D, Hamiltorr NC, Bishai I, Olley PM 1986 Involvement of intramural prostaglandin E2 in prenatal patency of the lamb ductus arteriosus. Can J Physiol Pharmacol 64: 737–744.
Ignarro LJ, Byrns RE, Wood KS 1987 Endothelium-dependent modulation of cGMP levels and intrinsic smooth muscle tone in isolated bovine intrapulmonary artery and vein. Circ Res 60: 82–92.
Bodach E, Coceani F, Dumbrille A, Okpako DT, Olley PM 1980 The response of the isolated ductus arteriosus to transmural stimulation and drugs. Br J Pharmacol 71: 419–427.
McMurphy DM, Boreus LO 1971 Studies on the pharmacology of the perfused human fetal ductus arteriosus. Am J Obstet Gynecol 109: 937–942.
McMurphy DM, Heymann MA, Rudolph AM, Melmon KL 1972 Developmental changes in constriction of the ductus arteriosus: responses to oxygen and vasoactive agents in the isolated ductus arteriosus of the fetal lamb. Pediatr Res 6: 231–238.
Oberhansli-Weiss I, Heymann MA, Rudolph AM, Melmon KL 1972 The pattern and mechanisms of response to oxygen by the ductus arteriosus and umbilical artery. Pediatr Res 6: 693–700.
Kovalcik V 1963 Response of the isolated ductus arteriosus to oxygen and anoxia. J Physiol 169: 185–197.
Knight DH, Patterson DF, Melbin J 1973 Constriction of the fetal ductus arteriosus induced by oxygen, acetylcholine, and norepinephrine in normal dogs and those genetically predisposed to persistent patency. Circulation 47: 127–132.
Van de Voorde J, Vanderstichele H, Leusen I 1987 Release of endothelium-derived relaxing factor from human umbilical vessels. Circ Res 60: 517–522.
Rubanyi GM, Desiderio D, Luisi A, Johns A, Sybertz EJ 1989 Phorbol dibutyrate inhibits release and action of endothelium-derived relaxing factor(s) in canine blood vessels. J Pharmacol Exp Ther 249: 858–863.
Kelner MJ, Uglik SF 1994 Mechanism of prostaglandin E2 release and increase in PGH2/PGE2 isomerase activity by PDGF: involvement of nitric oxide. Arch Biochem Biophys 312: 240–243.
Dong YL, Yallampalli C 1996 Interaction between nitric oxide and prostaglandin E2 pathways in pregnant rat uteri. Am J Physiol 270:E471–E476.
Sautebin L, Ialenti A, Ianaro A, Di Rosa M 1995 Modulation by nitric oxide of prostaglandin biosynthesis in the rat. Br J Pharmacol 114: 323–328.
Marczin N, Ryan US, Catravas JD 1992 Methylene blue inhibits nitrovasodilator- and endothelium-derived relaxing factor-induced cyclic GMP accumulation in cultured pulmonary arterial smooth muscle cells via generation of superoxide anion. J Pharmacol Exp Ther 263: 170–179.
Steinhorn RH, Morin FC, Russell JA 1994 The adventitia may be a barrier specific to nitric oxide in rabbit pulmonary artery. J Clin Invest 94: 1883–1888.
Heistad DD, Armstrong ML, Amundsen S 1986 Blood flow through vasa vasorum in arteries and veins: effects of luminal PO2 . Am J Physiol 250:H434–H442.
Clyman RI, Mauray F, Rudolph AM, Heymann MA 1980 Age-dependent sensitivity of the lamb ductus arteriosus to indomethacin and prostaglandins. J Pediatr 96: 94–98.
Abman SH, Chatfield BA, Rodman DM, Hall SL, McMurtry IF 1991 Maturational changes in endothelium-derived relaxing factor activity of ovine pulmonary arteries in vitro. Am J Physiol 260:L280–L285.
Challis JR, Dilley SR, Robinson JS, Thorburn GD 1976 Prostaglandins in the circulation of the fetal lamb. Prostaglandins 11: 1041–1052.
Friedman WF, Malony DA, Kirkpatrick SE 1978 Prostaglandins: physiological and clinical correlations. Adv Pediatr 25: 151–204.
Furchgott RF, Zawadzki JV 1980 The obligatory role of endothelial cells in the relaxation of arterial smooth muscle by acetylcholine. Nature 288: 373–376.
Shaul PW, Wells LB 1994 Oxygen modulates nitric oxide production selectively in fetal pulmonary endothelial cells. Am J Respir Cell Mol Biol 11: 432–438.
Johns RA, Linden JM, Peach MJ 1989 Endothelium-dependent relaxation and cyclic GMP accumulation in rabbit pulmonary artery are selectively impaired by moderate hypoxia. Circ Res 65: 1508–1515.
Park KH, Rubin LE, Gross SS, Levi R 1992 Nitric oxide is a mediator of hypoxic coronary vasodilation. Relation to adenosine and cyclooxygenase-derived metabolites. Circ Res 71: 992–1001.
Sun MK, Reis DJ 1992 Evidence nitric oxide mediates the vasodepressor response to hypoxia in sino-denervated rats. Life Sci 50: 555–565.
Pohl U, Busse R 1989 Hypoxia stimulates release of endothelium-derived relaxant factor. Am J Physiol 256:H1595–H1600.
Verma A, Hirsch DJ, Glatt CE, Ronnett GV, Snyder SH 1993 Carbon monoxide: a putative neural messenger. Science 259: 381–384.
Clyman RI, Blacksin AS, Manganiello VC, Vaughan M 1975 Oxygen and cyclic nucleotides in human umbilical artery. Proc Natl Acad Sci USA 72: 3883–3887.
Clyman RI 1996 Commentary: recommendations for the postnatal use of indomethacin. An analysis of four separate treatment strategies. J Pediatr 128: 601–607.
Acknowledgements
The authors thank Paul Sagan for his expert editorial assistance. We also thank Christine Roman and Mario Trujillo for their help in obtaining tissue specimens.
Author information
Authors and Affiliations
Additional information
Supported in part by U.S. Public Health Service, National Heart, Lung, Blood Institute Grants HL 46691 and HL 56061 and a gift from the Perinatal Associates Research Foundation.
Rights and permissions
About this article
Cite this article
Clyman, R., Waleh, N., Black, S. et al. Regulation of Ductus Arteriosus Patency by Nitric Oxide in Fetal Lambs: The Role of Gestation, Oxygen Tension, and Vasa Vasorum. Pediatr Res 43, 633–644 (1998). https://doi.org/10.1203/00006450-199805000-00012
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199805000-00012
This article is cited by
-
Understanding the pathobiology in patent ductus arteriosus in prematurity—beyond prostaglandins and oxygen
Pediatric Research (2019)
-
Patent ductus arteriosus in preterm infants: is early transcatheter closure a paradigm shift?
Journal of Perinatology (2019)
-
Prenatal closure of the ductus arteriosus and maternal ingestion of anthocyanins
Journal of Perinatology (2010)
-
Maturation of the contractile response of the Emu ductus arteriosus
Journal of Comparative Physiology B (2008)
-
Interactions between NO, CO and an endothelium‐derived hyperpolarizing factor (EDHF) in maintaining patency of the ductus arteriosus in the mouse
British Journal of Pharmacology (2007)