Abstract
Objective
Several conspiring factors have resulted in an increase in the level of medical burden in psychiatric patients. Psychiatry residents require increasing levels of medical sophistication. To assess the medical decision-making of psychiatry residents, the authors examined the outcome in subjects initially seen in the emergency psychiatric service and referred to the medical emergency department for medical evaluation and treatment.
Method
Psychiatry residents completed a survey sheet for every patient referred for medical evaluation from the emergency psychiatric service. The survey collected information on demographics, the level of subjective concern, and the anticipated level of medical intervention.
Results
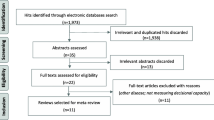
Twenty-seven medical referrals were made in the 6-week study period. Complete data were available for 23 (85.2%) subjects. Psychiatry residents accurately predicted the medical intervention 43.5% of the time. They overestimated the intervention 26.1% of the time and underestimated the intervention 30.4% of the time.
Conclusions
Psychiatry residents’ medical decision-making can be improved. Additional research is required to determine whether additional medical training is needed or whether our findings are a consequence of the variability in how different physicians address medical problems.
Similar content being viewed by others
References
Berren ME, Hill KR, Merikle E, et al: Serious mental illness and mortality rates. Hosp Comm Psychiatry 1994; 45: 604–605
Dembling BP, Chen DT, Vachon L: Life expectancy and causes of death in a population treated for serious mental illness. Psychiatr Serv 1999; 50: 1036–1042
Kilbourne AM, Cornelius JR, Hans X, et al: Burden of general medical conditions among individuals with bipolar disorder. Bipolar Disord 2004; 6: 368–373
Howard PB, Clark JJ, Brown T, et al: Co-morbid medical illness among adult recipients of Medicaid mental health services. Issues Ment Health Nurs 2006 (in press)
Bunce DF 2nd, Jones LR, Badger LW, et al: Medical illness in psychiatric patients: barriers to diagnosis and treatment. South Med J 1982; 75: 941–944
Vieweg V, Levenson J, Pandurangi A, et al: Medical disorders in the schizophrenic patient. Int J Psychiatry Med 1995; 25: 137–172
Goldman LS: Medical illness in patients with schizophrenia. J Clin Psychiatry 1999; 60(suppl) 21: 10–15
El-Mallakh RS, Cowdry RW, Pettigrew IE: Evaluating change: a simple technique for determining statistical significance of proportional criteria. J Healthc Qual 1994; 16: 14–17
Quinn DK, Geppert CM, Maggiore WA: The Emergency Medical Treatment and Active Labor Act of 1985 and the practice of psychiatry. Psychiatr Serv 2002; 53: 1301–1307
Pajonk FG, Grunberg KA, Paschen HR, et al: [Psychiatric emergencies in the physician-based system of a German city.] Fortschs Neurol Psychiatr 2001; 69: 170–174
Qureshi NA, al-Habeeb TA, al-Ghandy YS, et al: Psychiatric co-morbidity in primary care and hospital referrals, Saudi Arabia. East Mediterr Health J 2001; 7: 492–501
Zun LS, Hernandez R, Thompson R, et al: Comparison of EPs’ and psychiatrists’ laboratory assessment of psychiatric patients. Am J Emerg Med 2004; 22: 175–180
Garbrick L, Levitt MA, Barrett M, et al: Agreement between emergency physicians and psychiatrists regarding admission decisions. Acad Emerg Med 1996; 3: 1027–1030
Santucci KA, Sather J, Baker MD: Emergency medicine training programs’ educational requirements in the management of psychiatric emergencies: current perspective. Pediatr Emerg Care 2003; 19: 154–156
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
El-Mallakh, R., Zinner, J., Mackey, A. et al. Medical Decision-Making by Psychiatry Residents. Acad Psychiatry 31, 326–328 (2007). https://doi.org/10.1176/appi.ap.31.4.326
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1176/appi.ap.31.4.326