Abstract
Objective
Health outcomes of patients with chronic disease might be influenced by assistance from others in performing daily activities. We examined whether perceived adequacy of such tangible support was associated with prognosis in a cohort of patients with coronary artery disease.
Design
Longitudinal cohort study.
Setting/Participants
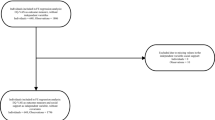
In spring 1993, a cohort of 1,468 patients with chronic artery disease was identified using claims data. The cohort consisted of all surviving residents of Manitoba. Canada, who had been hospitalized for acute myocardial infarction from 1991 to 1992: 820 patients completed the initial survey, and 734 completed a follow-up survey approximately 1 year later.
Measurements and Main Results
Adequacy of tangible support was assessed by asking if respondents needed help at home because of health problems, and whether these needs were met. We examined the association between perceived adequacy of tangible support and health outcomes at 1 year (mortality, physical function). Of 820 participants, 74% perceived no need for help, 13% has sufficient help, 9% needed more help, and 5% needed much more help; 31 patients died during follow-up. After adjustment for age and initial health status, odds ratios (95% confidence interval) for death were: sufficient help 1.8 (0.61, 5.8); need more help 3.2 (1.1, 9.4); and need much more help 6.5 (2.0, 21.6) compared with respondents with no perceived need. Decline in physical function was also linearly related to perceiving less-adequate tangible support. Sensitivity analyses indicated it is highly improbable that results were due to selection bias.
Conclusions
Perceived lack of needed assistance was related to mortality and to decline in physical functioning. Adequacy of tangible support was an important prognostic factor for these patients with coronary artery disease and may be a determinant of health outcomes.
Similar content being viewed by others
References
Case R, Moss A, Case N, McDermott M, Eberly S. Living alone after myocardial infarction. Impact on prognosis. JAMA, 1992:267:515–9.
Eriksen W. The role of social support in the pathogenesis of coronary heart disease. A literature review. Fam Pract. 1994;11:201–9.
Bucher H. Lack of social support reduces survival after first myocardial infarction. J Gen Intern Med. 1994;9:409–17.
Berkman L. The relationship of social networks and social support to morbidity and mortality. In: Cohen S, Syme SL, eds. Social Support and Health. Orlando, Fla: Academic Press: 1985.
Cohen S, Syme L. The study and application of social support. In: Cohen S, Syme L, eds. Social Support and Health. Orlando, Fla: Academic Press: 1985.
Orth-Gomer K, Rosengren A, Wilhelmsen L. Lack of social support and incidence of coronary heart disease in middle-aged Swedish men. Psychosom Med. 1993;55:37–43.
Berkman L, Leo-Summers L, Horwitz R. Emotional support and survival after myocardial infarction. A prospective, population-based study of the elderly. Ann Intern Med. 1992;117:1003–9.
Jenkinson CM, Madeley RJ, Mitchell RA, Turner ID. The influence of psychosocial factors on survival after myocardial infarction. Public Health. 1993;107:305–17.
Medalie JH, Goldbourt U. Angina pectoris among 10,000 men. Am J Med. 1976;60:910–21.
Seeman TE, Syme SL. Social networks and coronary artery disease: a comparison of the structure and function of social relations as predictors of disease. Psychosom Med. 1987;49:341–54.
Vogt T, Mullooly J, Ernst D, Pope C, Hollis J. Social networks as predictors of ischemic heart disease, cancer, stroke and hypertension: incidence, survival and mortality. J Clin Epidemiol. 1992;45:659–66.
Williams R, Barefoot J, Califf R, et al. Prognostic importance of social and economic resources among medically treated patients with anglographically documented coronary artery disease. JAMA. 1992;267:520–4.
Ruberman W, Weinblatt E, Goldberg J, Chaudhary B. Psychosocial influences on mortality after myocardial infarction. N Engl J Med. 1984;311:552–9.
Spiegel D, Kraemer HC, Bloom JR, Gottheil E. Effect of psychosocial treatment on survival of patients with metastatic breast cancer. Lancet. 1989;2:888–91.
Schaefer C, Coyne JC, Lazarus RS. The health-related functions of social support. J Behav Med. 1981;4:381–406.
Oxman TE, Berkman LF, Kasl S, Freeman DH, Barrett J. Social support and depressive symptoms in the elderly. Am J Epidemiol. 1992;135:356–68.
Fleming R, Baum A, Singer JE. Social support and community mental health. In: Cohen S, Syme SL, eds. Social Support and Health. Orlando, Fla: Academic Press: 1985.
Kulik J, Mahler H. Social support and recovery from surgery. Health Psychol. 1989;8(2):221–38.
Norbeck J, Tilden V. Life stress, social support and emotional equilibrium in complications of pregnancy: a prospective multivariate study. J Health Soc Behav. 1983;24:30–46.
Weinberger M, Tierney WM, Booher P, Hiner SL. Social support, stress and functional status in patients with osteoarthritis. Soc Sci Med. 1990;30:503–8.
House JS, Robbins C, Metzner HM, et al. The association of social relationships and activities with mortality: prospective evidence from the Tecumseh Community Health Study. Am J Epidemiol. 1982; 116:123–40.
Berkman LF, Syme L. Social networks, host resistance and mortality: a nine-year follow-up study of Alameda County residents. Am J Epidemiol. 1979;109:186–204.
House JS, Kahn RL. Measures and concepts of social support. In: Cohen S, Syme SL, eds. Social Support and Health. Orlando, Fla: Academic Press; 1985.
Chappell NL, Badger M. Social isolation and well-being. J Gerontol. 1989;44:S169–76.
Ware J, Kosinski M, Keller S. SF-36 Physical and Mental Health Summary Scales: A User’s Manual. 2nd ed. Boston, Mass: The Health Institute, New England Medical Center; 1994.
Roos N. From research to policy: what have we learned from designing the population health information system? Med Care. 1995;33(suppl):DS132–45.
Ware J, Snow K, Kosinski M, Gandek B. SF-36 Health Survey: Manual and Interpretation Guide. Boston, Mass: The Health Institute, New England Medical Center: 1993.
Ware J, Bayliss M, Rogers W, Kosinski M, Tarlov A. Differences in 4-year health outcomes for elderly and poor, chronically ill patients treated in HMO and fee-for-service systems. Results from the Medical Outcomes Study. JAMA. 1996;276:1039–47.
Ware J, Kosinski M, Bayliss M, McHorney C, Roger W, Raczek A. Comparison of methods for the scoring and statistical analysis of SF-36 health profile and summary measures: summary of results from the Medical Outcomes Study. Med Care. 1995;33:264–79.
Campeau L. Grading of angina pectoris. Circulation. 1976;54:522–3. Letter.
Rose G. Cardiovascular Survey Methods. 2nd ed. Geneva, Switzerland: World Health Organization; 1982. World Health Organization monograph series.
Diehr P, Patrick D, Hedrick S, et al. Including deaths when measuring health status over time. Med Care. 1995;33(suppl):AS164–72.
Friedman MM. Social support sources and psychological well-being in older women with heart disease. Res Nurs Health. 1993;16:405–13.
Hennekens CH, Buring JE. Epidemiology in Medicine. Boston, Mass: Little, Brown, Inc.; 1987.
Author information
Authors and Affiliations
Additional information
Drs. Woloshin and Schwartz are supported by a Veterans Affairs Fellowship in Ambulatory Care.
Rights and permissions
About this article
Cite this article
Woloshin, S., Schwartz, L.M., Tosteson, A.N.A. et al. Perceived adequacy of tangible social support and health outcomes in patients with coronary artery disease. J GEN INTERN MED 12, 613–618 (1997). https://doi.org/10.1046/j.1525-1497.1997.07121.x
Issue Date:
DOI: https://doi.org/10.1046/j.1525-1497.1997.07121.x