Abstract
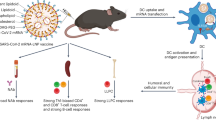
To elicit optimal immune responses, messenger RNA vaccines require intracellular delivery of the mRNA and the careful use of adjuvants. Here we report a multiply adjuvanted mRNA vaccine consisting of lipid nanoparticles encapsulating an mRNA-encoded antigen, optimized for efficient mRNA delivery and for the enhanced activation of innate and adaptive responses. We optimized the vaccine by screening a library of 480 biodegradable ionizable lipids with headgroups adjuvanted with cyclic amines and by adjuvanting the mRNA-encoded antigen by fusing it with a natural adjuvant derived from the C3 complement protein. In mice, intramuscular or intranasal administration of nanoparticles with the lead ionizable lipid and with mRNA encoding for the fusion protein (either the spike protein or the receptor-binding domain of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2)) increased the titres of antibodies against SARS-CoV-2 tenfold with respect to the vaccine encoding for the unadjuvanted antigen. Multiply adjuvanted mRNA vaccines may improve the efficacy, safety and ease of administration of mRNA-based immunization.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 digital issues and online access to articles
$99.00 per year
only $8.25 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
Data availability
The main data supporting the findings of this study are available within this paper and its Supplementary Information. The raw and analysed datasets are too large to readily share publicly yet are available for research purposes from the corresponding author on reasonable request.
References
Corbett, K. S. et al. SARS-CoV-2 mRNA vaccine design enabled by prototype pathogen preparedness. Nature 586, 567–571 (2020).
Polack, F. P. et al. Safety and efficacy of the BNT162b2 mRNA Covid-19 vaccine. N. Engl. J. Med. 383, 2603–2615 (2020).
Baden, L. R. et al. Efficacy and safety of the mRNA-1273 SARS-CoV-2 vaccine. N. Engl. J. Med. 384, 403–416 (2021).
Vogel, A. B. et al. BNT162b vaccines protect rhesus macaques from SARS-CoV-2. Nature 592, 283–289 (2021).
Barbier, A. J., Jiang, A. Y., Zhang, P., Wooster, R. & Anderson, D. G. The clinical progress of mRNA vaccines and immunotherapies. Nat. Biotechnol. 40, 840–854 (2022).
Pardi, N., Hogan, M. J., Porter, F. W. & Weissman, D. mRNA vaccines—a new era in vaccinology. Nat. Rev. Drug Discov. 17, 261–279 (2018).
Buschmann, M. D. et al. Nanomaterial delivery systems for mRNA vaccines. Vaccines 9, 65 (2021).
Kowalski, P. S., Rudra, A., Miao, L. & Anderson, D. G. Delivering the messenger: advances in technologies for therapeutic mRNA delivery. Mol. Ther. 27, 710–728 (2019).
Patel, A. K. et al. Inhaled nanoformulated mRNA polyplexes for protein production in lung epithelium. Adv. Mater. 31, e1805116 (2019).
Zhang, N. N. et al. A thermostable mRNA vaccine against COVID-19. Cell 182, 1271–1283 e1216 (2020).
McKay, P. F. et al. Self-amplifying RNA SARS-CoV-2 lipid nanoparticle vaccine candidate induces high neutralizing antibody titres in mice. Nat. Commun. 11, 3523 (2020).
Pulendran, B., S. Arunachalam, P. & O’Hagan, D. T. Emerging concepts in the science of vaccine adjuvants. Nat. Rev. Drug Discov. 20, 454–475 (2021).
Alameh, M.-G. et al. Lipid nanoparticles enhance the efficacy of mRNA and protein subunit vaccines by inducing robust T follicular helper cell and humoral responses. Immunity 54, 2877–2892.e2877 (2021).
Tahtinen, S. et al. IL-1 and IL-1ra are key regulators of the inflammatory response to RNA vaccines. Nat. Immunol. 23, 532–542 (2022).
Swaminathan, G. et al. A tetravalent sub-unit dengue vaccine formulated with ionizable cationic lipid nanoparticle induces significant immune responses in rodents and non-human primates. Sci. Rep. 6, 34215 (2016).
Miao, L. et al. Delivery of mRNA vaccines with heterocyclic lipids increases anti-tumor efficacy by STING-mediated immune cell activation. Nat. Biotechnol. 37, 1174–1185 (2019).
Ahn, J. & Barber, G. N. STING signaling and host defense against microbial infection. Exp. Mol. Med. 51, 1–10 (2019).
Hassett, K. J. et al. Optimization of lipid nanoparticles for intramuscular administration of mRNA vaccines. Mol. Ther. Nucleic Acids 15, 1–11 (2019).
Sabnis, S. et al. A novel amino lipid series for mRNA delivery: improved endosomal escape and sustained pharmacology and safety in non-human primates. Mol. Ther. 26, 1509–1519 (2018).
Maier, M. A. et al. Biodegradable lipids enabling rapidly eliminated lipid nanoparticles for systemic delivery of RNAi therapeutics. Mol. Ther. 21, 1570–1578 (2013).
Toapanta, F. R. & Ross, T. M. Complement-mediated activation of the adaptive immune responses: role of C3d in linking the innate and adaptive immunity. Immunol. Res. 36, 197–210 (2006).
Bower, J. F. & Ross, T. M. in Current Topics in Complement 249–264 (Springer, 2006).
Rickert, R. C. Regulation of B lymphocyte activation by complement C3 and the B cell coreceptor complex. Curr. Opin. Immunol. 17, 237–243 (2005).
Phua, K. K. L., Staats, H. F., Leong, K. W. & Nair, S. K. Intranasal mRNA nanoparticle vaccination induces prophylactic and therapeutic anti-tumor immunity. Sci. Rep. 4, 5128 (2014).
Mai, Y. et al. Intranasal delivery of cationic liposome–protamine complex mRNA vaccine elicits effective anti-tumor immunity. Cell. Immunol. 354, 104143 (2020).
Tarke, A. et al. Impact of SARS-CoV-2 variants on the total CD4(+) and CD8(+) T cell reactivity in infected or vaccinated individuals. Cell Rep. Med. 2, 100355 (2021).
Schulien, I. et al. Characterization of pre-existing and induced SARS-CoV-2-specific CD8(+) T cells. Nat. Med. 27, 78–85 (2021).
Le Bert, N. et al. SARS-CoV-2-specific T cell immunity in cases of COVID-19 and SARS, and uninfected controls. Nature 584, 457–462 (2020).
Grifoni, A. et al. Targets of T cell responses to SARS-CoV-2 coronavirus in humans with COVID-19 disease and unexposed individuals. Cell 181, 1489–1501 e1415 (2020).
Peng, Y. et al. Broad and strong memory CD4(+) and CD8(+) T cells induced by SARS-CoV-2 in UK convalescent individuals following COVID-19. Nat. Immunol. 21, 1336–1345 (2020).
Oberhardt, V. et al. Rapid and stable mobilization of CD8+ T cells by SARS-CoV-2 mRNA vaccine. Nature 597, 268–273 (2021).
Reinscheid, M. et al. COVID-19 mRNA booster vaccine induces transient CD8+ T effector cell responses while conserving the memory pool for subsequent reactivation. Nat. Commun. 13, 4631 (2022).
Liu, J. et al. CD8 T cells contribute to vaccine protection against SARS-CoV-2 in macaques. Sci. Immunol. 7, eabq7647 (2022).
Tarke, A. et al. SARS-CoV-2 vaccination induces immunological T cell memory able to cross-recognize variants from alpha to omicron. Cell 185, 847–859 e811 (2022).
Mise-Omata, S. et al. Memory B cells and memory T cells induced by SARS-CoV-2 booster vaccination or infection show different dynamics and responsiveness to the omicron variant. J. Immunol. 209, 2104–2113 (2022).
Dhawan, M. et al. Updated insights into the T cell-mediated immune response against SARS-CoV-2: a step towards efficient and reliable vaccines. Vaccines 11, 101 (2023).
Moss, P. The T cell immune response against SARS-CoV-2. Nat. Immunol. 23, 186–193 (2022).
Richardson, S. J., Bai, A., Kulkarni, A. A. & Moghaddam, M. F. Efficiency in drug discovery: liver S9 fraction assay as a screen for metabolic stability. Drug Metab. Lett. 10, 83–90 (2016).
Kariko, K. et al. Incorporation of pseudouridine into mRNA yields superior nonimmunogenic vector with increased translational capacity and biological stability. Mol. Ther. 16, 1833–1840 (2008).
Li, B., Luo, X. & Dong, Y. Effects of chemically modified messenger RNA on protein expression. Bioconjug. Chem. 27, 849–853 (2016).
Kauffman, K. J. et al. Optimization of lipid nanoparticle formulations for mRNA delivery in vivo with fractional factorial and definitive screening designs. Nano Lett. 15, 7300–7306 (2015).
Miao, L. et al. Synergistic lipid compositions for albumin receptor mediated delivery of mRNA to the liver. Nat. Commun. 11, 2424 (2020).
vander Straeten, A. et al. A microneedle vaccine printer for thermostable COVID-19 mRNA vaccines. Nat. Biotechnol. https://doi.org/10.1038/s41587-023-01774-z (2023).
Oberli, M. A. et al. Lipid nanoparticle assisted mRNA delivery for potent cancer immunotherapy. Nano Lett. 17, 1326–1335 (2017).
Alu, A. et al. Intranasal COVID-19 vaccines: from bench to bed. eBioMedicine 76, 103841 (2022).
Li, B. et al. Combinatorial design of nanoparticles for pulmonary mRNA delivery and genome editing. Nat. Biotechnol. https://doi.org/10.1038/s41587-023-01679-x (2023).
Ndeupen, S. et al. The mRNA–LNP platform’s lipid nanoparticle component used in preclinical vaccine studies is highly inflammatory. iScience 24, 103479 (2021).
Lu, L. L., Suscovich, T. J., Fortune, S. M. & Alter, G. Beyond binding: antibody effector functions in infectious diseases. Nat. Rev. Immunol. 18, 46–61 (2017).
Zohar, T. et al. Compromised humoral functional evolution tracks with SARS-CoV-2 mortality. Cell 183, 1508–1519.e1512 (2020).
Kaplonek, P. et al. Early cross-coronavirus reactive signatures of humoral immunity against COVID-19. Sci. Immunol. 6, eabj2901 (2021).
Kaplonek, P. et al. mRNA-1273 vaccine-induced antibodies maintain Fc effector functions across SARS-CoV-2 variants of concern. Immunity 55, 355–365.e354 (2022).
Harrod, K. et al. The Fc-mediated effector functions of a potent SARS-CoV-2 neutralizing antibody, SC31, isolated from an early convalescent COVID-19 patient, are essential for the optimal therapeutic efficacy of the antibody. PLoS ONE 16, e0253487 (2021).
Rosenblum, H. G. et al. Safety of mRNA vaccines administered during the initial 6 months of the US COVID-19 vaccination programme: an observational study of reports to the Vaccine Adverse Event Reporting System and v-safe. Lancet Infect. Dis. (2022).
Bastard, P., Zhang, Q., Zhang, S. Y., Jouanguy, E. & Casanova, J. L. Type I interferons and SARS-CoV-2: from cells to organisms. Curr. Opin. Immunol. 74, 172–182 (2022).
Hervas-Stubbs, S. et al. Effects of IFN-alpha as a signal-3 cytokine on human naive and antigen-experienced CD8(+) T cells. Eur. J. Immunol. 40, 3389–3402 (2010).
Richner, J. M. et al. Modified mRNA vaccines protect against Zika virus infection. Cell 169, 176 (2017).
Xia, S. et al. Safety and immunogenicity of an inactivated SARS-CoV-2 vaccine, BBIBP-CorV: a randomised, double-blind, placebo-controlled, phase 1/2 trial. Lancet Infect. Dis. 21, 39–51 (2021).
Dempsey, P. W., Allison, M. E. D., Akkaraju, S., Goodnow, C. C. & Fearon, D. T. C3d of complement as a molecular adjuvant: bridging innate and acquired immunity. Science 271, 348–350 (1996).
Ross, T. M., Xu, Y., Bright, R. A. & Robinson, H. L. C3d enhancement of antibodies to hemagglutinin accelerates protection against influenza virus challenge. Nat. Immunol. 1, 127–131 (2000).
Bower, J., Sanders, K. & Ross, T. C3d enhances immune responses using low doses of DNA expressing the HIV-1 envelope from codon-optimized gene sequences. Curr. HIV Res. 3, 191–198 (2005).
Green, T. D. et al. C3d enhancement of neutralizing antibodies to measles hemagglutinin. Vaccine 20, 242–248 (2001).
He, Y. G. et al. A novel C3d-containing oligomeric vaccine provides insight into the viability of testing human C3d-based vaccines in mice. Immunobiology 223, 125–134 (2018).
Zhang, D. et al. Construction and immunogenicity of DNA vaccines encoding fusion protein of murine complement C3d-p28 and GP5 gene of porcine reproductive and respiratory syndrome virus. Vaccine 29, 629–635 (2011).
Green, T. D., Montefiori, D. C. & Ross, T. M. Enhancement of antibodies to the human immunodeficiency virus type 1 envelope by using the molecular adjuvant C3d. J. Virol. 77, 2046–2055 (2003).
Watanabe, I. et al. Protection against influenza virus infection by intranasal administration of C3d-fused hemagglutinin. Vaccine 21, 4532–4538 (2003).
Yang, S. et al. Fusion of C3d molecule with neutralization epitope(s) of hepatitis E virus enhances antibody avidity maturation and neutralizing activity following DNA immunization. Virus Res. 151, 162–169 (2010).
Wang, L., Sunyer, J. O. & Bello, L. J. Fusion to C3d enhances the immunogenicity of the E2 glycoprotein of type 2 bovine viral diarrhea virus. J. Virol. 78, 1616–1622 (2004).
Zhang, Z. et al. Fusion to chicken C3d enhances the immunogenicity of the M2 protein of avian influenza virus. Virol. J. 7, 89 (2010).
Chen, G. et al. Clinical and immunological features of severe and moderate coronavirus disease 2019. J. Clin. Invest. 130, 2620–2629 (2020).
Wang, Z. et al. Enhanced SARS-CoV-2 neutralization by dimeric IgA. Sci. Transl. Med. 13, eabf1555 (2021).
Sterlin, D. et al. IgA dominates the early neutralizing antibody response to SARS-CoV-2. Sci. Transl. Med. 13, eabd2223 (2021).
Boyaka, P. N. Inducing mucosal IgA: a challenge for vaccine adjuvants and delivery systems. J. Immunol. 199, 9–16 (2017).
Allie, S. R. et al. The establishment of resident memory B cells in the lung requires local antigen encounter. Nat. Immunol. 20, 97–108 (2018).
Morabito, K. M. et al. Memory inflation drives tissue-resident memory CD8+ T cell maintenance in the lung after intranasal vaccination with murine cytomegalovirus. Front. Immunol. 9, 1861 (2018).
Levin, E. G. et al. Waning immune humoral response to BNT162b2 Covid-19 vaccine over 6 months. N. Engl. J. Med. 385, e84 (2021).
Goldberg, Y. et al. Waning immunity after the BNT162b2 vaccine in Israel. N. Engl. J. Med. 385, e85 (2021).
Künzli, M. et al. Route of self-amplifying mRNA vaccination modulates the establishment of pulmonary resident memory CD8 and CD4 T cells. Sci. Immunol. 7, eadd3075 (2022).
Vaca, G. B. et al. Intranasal mRNA–LNP vaccination protects hamsters from SARS-CoV-2 infection. Preprint at bioRxiv (2023).
Boudreau, C. M. & Alter, G. Extra-neutralizing FcR-mediated antibody functions for a universal influenza vaccine. Front. Immunol. 10, 440 (2019).
Meyer, M. et al. Ebola vaccine-induced protection in nonhuman primates correlates with antibody specificity and Fc-mediated effects. Sci. Transl. Med. 13, eabg6128 (2021).
Neidich, S. D. et al. Antibody Fc effector functions and IgG3 associate with decreased HIV-1 risk. J. Clin. Invest. 129, 4838–4849 (2019).
Zohar, T. et al. Upper and lower respiratory tract correlates of protection against respiratory syncytial virus following vaccination of nonhuman primates. Cell Host Microbe 30, 41–52.e45 (2022).
Yamin, R. et al. Fc-engineered antibody therapeutics with improved anti-SARS-CoV-2 efficacy. Nature 599, 465–470 (2021).
Puntel, M. et al. Identification and visualization of CD8+ T cell mediated IFN-gamma signaling in target cells during an antiviral immune response in the brain. PLoS ONE 6, e23523 (2011).
Kim, P. S. & Ahmed, R. Features of responding T cells in cancer and chronic infection. Curr. Opin. Immunol. 22, 223–230 (2010).
Blattman, J. N. & Greenberg, P. D. Cancer immunotherapy: a treatment for the masses. Science 305, 200–205 (2004).
Hoft, D. F. et al. Live and inactivated influenza vaccines induce similar humoral responses, but only live vaccines induce diverse T-cell responses in young children. J. Infect. Dis. 204, 845–853 (2011).
Heyes, J., Palmer, L., Bremner, K. & MacLachlan, I. Cationic lipid saturation influences intracellular delivery of encapsulated nucleic acids. J. Control. Release 107, 276–287 (2005).
Shobaki, N., Sato, Y. & Harashima, H. Mixing lipids to manipulate the ionization status of lipid nanoparticles for specific tissue targeting. Int. J. Nanomed. 13, 8395–8410 (2018).
Chen, X., Gentili, M., Hacohen, N. & Regev, A. A cell-free nanobody engineering platform rapidly generates SARS-CoV-2 neutralizing nanobodies. Nat. Commun. 12, 5506 (2021).
Acknowledgements
This work was supported by the National Institutes of Health (NIH) (R61AI161805) and Translate Bio. B.L. was also supported by the Leslie Dan Faculty of Pharmacy startup fund, the Princess Margaret Cancer Centre operating fund, the Connaught Fund (514681), the J. P. Bickell Foundation (515159), the Canada Research Chairs Program (CRC-2022-00575), Canadian Institutes of Health Research (PJH-185722), Natural Sciences and Engineering Research Council of Canada (RGPIN-2023-05124) and the Canada Foundation for Innovation—John R. Evans Leaders Fund (43711). A.Y.J. was also supported by the NIH (UG3HL147367 and UH3HL147367). The Systems Serology Laboratory is supported by the generous gifts of M. and L. Schwartz, T. and S. Ragon and the Samana Kay Research Scholars award. The Systems Serology Lab also receives funding from the Massachusetts Consortium on Pathogen Readiness (MassCPR), the Gates Global Health Vaccine Accelerator Platform and the NIH (1P01AI165072-01, 3R37AI080289-11S1, U19AI42790-01, U19AI135995-02 and U19AI42790-01). T.S. was supported by the Marble Centre for Cancer Nanomedicine. S.B. is a Howard Hughes Medical Institute investigator. J.W. was supported by the Cystic Fibrosis Foundation (WITTEN19XX0) and the NIH (R01 HL162564-02). Y.X. was supported by a Postdoc Fellowship from the PRiME-UHN Clinical Catalyst Program at the University of Toronto. We thank the Koch Institute Swanson Biotechnology Centre for technical support, specifically the Animal Imaging and Preclinical Testing, Flow Cytometry, High Throughput Sciences, Histology and Nanotechnology Materials Core Facilities. We also thank R. Bronson and E. Calle for assistance with the histology, and M. Gentili and N. Hacohen for providing the reagents for the pseudotype neutralization assay. Figures 2a and 4e were created with Biorender.com.
Author information
Authors and Affiliations
Contributions
B.L. and A.Y.J. conceived the project and wrote the paper, with input from all authors. B.L. and I.R. designed the combinatorial lipid library. B.L., A.Y.J., I.R., C.A, T.M.R., A.G.R.G, L.H.R., T.S., C.M., J.W., H.M., T.M.C., Y.X. and R.P.M. performed experiments and analysed data. B.L., A.Y.J., R.L. and D.G.A. discussed the results and edited the paper. B.L., S.B., G.A., R.L. and D.G.A. acquired funding and supervised the project.
Corresponding author
Ethics declarations
Competing interests
B.L., A.Y.J. and D.G.A. have filed a patent for the use of C3d in mRNA vaccines. D.G.A receives research funding from Sanofi/Translate Bio and is a co-founder of Orna Therapeutics. R.L. co-founded Moderna and serves on its board. He has been an advisor for Hopewell Therapeutics and Combined Therapeutics. For a list of entities with which R.L. is or has been recently involved, compensated or uncompensated, refer to the ‘Competing Interests’ section of the supplementary information (accurate as of July 2023). The other authors declare no competing interests.
Peer review
Peer review information
Nature Biomedical Engineering thanks Michael Mitchell and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Extended data
Extended Data Fig. 1 Comparison of LNP formulations containing MC3, Lipid 331, ALC-0315 or A18-Iso5-2DC18.
a, Transfection of mFFL LNPs in THP-1 cells (50 ng mRNA per well, n = 3). b, Transfection of mFFL LNPs containing either MC3, Lipid 331, ALC-0315, or A18-Iso5-2DC18 (A18) at the i.m. injection site in mice (0.2 mg/kg mRNA, n = 3 biologically independent mice per group). c. Representative IVIS imaging results from IM injection. d. The abundance of residual ionizable lipids at the injection site three days post-injection (n = 5 mice per group). Statistical significance was analysed using a one-way ANOVA with Dunnett’s correction (a) or one-way ANOVA with post-hoc Tukey test (b) or a two-tailed Student’s t-test (d). Data are presented as mean ± SD.
Extended Data Fig. 2 Characterization of anti-RBDDelta IgG1, IgG2b and IgG2c following the vaccination of RBDDelta, mRNA or RBDDelta/C3d mRNA mixture, or RBDDelta-C3d fusion mRNA.
a, MFIs of IgG subclasses obtained from Luminex assay measuring serological antibody binding against the RBD antigen from the Delta variant of SARS-CoV-2. Data related to Fig. 3i. b, Ratio of IgG2c to IgG1 levels as a surrogate of Th1-Th2 bias. Ratios were calculated as log10(MFIIgG2c)/log10(MFIIgG1). n = 5, statistical significance was analysed using a one-way ANOVA with post-hoc Tukey test. Data are presented as mean ± SD.
Extended Data Fig. 3 Pseudovirus neutralization titers following IM or IN vaccination with MC3 or Lipid 331 LNPs encapsulating either mRBDDelta or mRBDDelta-C3d.
NT50 of sera collected from vaccinated C57BL/6J mice two weeks post (a) IM or (b) IN boost vaccination. Mice were vaccinated with either mRBDDelta in MC3 or Lipid 331 LNPs (MC3 and 331, respectively), mRBDDelta-C3d in MC3 or Lipid 331 LNPs (MC3 + C3d and 331 + C3d, respectively), or PBS. A pseudovirus neutralization assay was used to determine NT50 values. Statistical significance was determined using a Kruskal-Wallis one-way ANOVA. Data are presented as geometric mean titre± geometric SD.
Extended Data Fig. 5 Characterization of anti-RBDDelta antibody subclasses and Fc receptor binding following IM or IN vaccination with MC3 or Lipid 331 LNPs encapsulating either mRBDDelta or mRBDDelta-C3d.
a, MFIs of antibody features obtained from Luminex assay measuring serological antibody binding against the RBD antigen from the Delta variant of SARS-CoV-2. Serum was collected from mice vaccinated with either mRBDDelta in MC3 or Lipid 331 LNPs (MC3 and 331, respectively), mRBDDelta-C3d in MC3 or Lipid 331 LNPs (MC3 + C3d and 331 + C3d, respectively), or PBS. Data related to vaccination study in Fig. 4. b, Ratio of IgG2c to IgG1 levels as a surrogate of Th1-Th2 bias. Ratios were calculated as log10(MFIIgG2c)/log10(MFIIgG1). n = 5, statistical significance was analysed using a one-way ANOVA with post-hoc Tukey test. Data are presented as mean ± SD.
Supplementary information
Supplementary Information
Supplementary methods and figures, and detailed competing interests for R.L.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li, B., Jiang, A.Y., Raji, I. et al. Enhancing the immunogenicity of lipid-nanoparticle mRNA vaccines by adjuvanting the ionizable lipid and the mRNA. Nat. Biomed. Eng (2023). https://doi.org/10.1038/s41551-023-01082-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41551-023-01082-6