Abstract
Background
Disruption of tight junctions (TJs) predisposes to bacterial translocation, intestinal inflammation, and necrotizing enterocolitis (NEC). Previously, studies showed that hyaluronan (HA), a glycosaminoglycan in human milk, maintains intestinal permeability, enhances intestinal immunity, and reduces intestinal infections. In this study, we investigated the effects of HA 35 kDa on a NEC-like murine model.
Methods
Pups were divided into Sham, NEC, NEC+HA 35, and HA 35. Severity of intestinal injury was compared using a modified macroscopic gut scoring and histologic injury grading. The effect of HA 35 on intestinal permeability was determined by measuring FITC dextran and bacterial translocation. RNA and protein expression of TJ proteins (claudin-2, -3, -4, occludin, and ZO-1) were compared between the groups.
Results
Pups in the NEC+HA 35 group had increased survival and lower intestinal injury compared to untreated NEC. In addition, HA 35 reduced intestinal permeability, bacterial translocation, and proinflammatory cytokine release. Ileal expression of claudin-2, -3, -4, occludin, and ZO-1 was upregulated in NEC+HA 35 and HA 35 compared to untreated NEC and shams.
Conclusion
These findings suggest that HA 35 protects against NEC partly by upregulating intestinal TJs and enhancing intestinal barrier function.
Similar content being viewed by others
Introduction
Necrotizing enterocolitis (NEC) is a devastating gastrointestinal disease that primarily affects premature infants of <32 weeks’ gestation. The incidence of NEC is between 7% and 12% and is gradually increasing in frequency, due in part to the increasing number of premature infants surviving each year.1 Although the pathogenesis of NEC is still unclear, evidence suggests that prematurity, altered intestinal microbiome, and intestinal barrier dysfunction are major contributors to the disease. Disruption of intestinal barrier has been shown to be an important factor in the development of intestinal inflammation2,3 and, in combination with an altered intestinal microbiome, can lead to translocation of bacteria and bacterial products, increased inflammation, intestinal necrosis, and in severe cases sepsis and death.4 Thus, identifying strategies or interventions that protect intestinal integrity and modulate inflammation is critical in preventing NEC.
Evidence suggests that exclusive human milk (HM) feeding decreases the risk of NEC in premature infants.5,6 Several protective factors are present in HM including lactoferrin, oligosaccharides, and growth factors.7 HM also contains glycosaminoglycans (GAGs) at 5–10 times the concentration of bovine milk.8 Hyaluronan (HA), a GAG composed of repeating disaccharides of β-d-glucuronic acid and N-acetyl-β-d-glucosamine, is present in HM with the highest concentration during the first months after birth.9 HA is produced at cell surfaces by hyaluronan synthases (HAS1, HAS2, and HAS3) generally as high-molecular-weight HA and can be degraded in response to injury.10 The degraded fragments can either have pro- or anti-inflammatory effects depending on the tissue environment or the size and molecular structure of the HA fragments.11
Recently, HA from HM or purified HA of average molecular weight 35 kDa (HA 35) was shown to prevent intestinal bacterial infection and reduce intestinal inflammation in various mouse models mainly through maintaining the intestinal barrier defenses and function.9,10,11,12,13 Since both factors are involved in the pathogenesis of NEC, we sought to determine the effect of HA 35 on survival, intestinal permeability, and histological injury in a NEC-like model. We then determined the effect of HA 35 on tight junction (TJ) protein expression in ileal tissue. Finally, the effect of HA on proinflammatory cytokine release and bacteremia was compared between the groups.
Materials and methods
All animal experiments (Protocol #04203AR) were approved by the Institutional Animal Care and Use Committee (IACUC) of the University of Oklahoma Health Sciences Center (Protocol #101502-16-024), and performed according to recommendations in the Guide for the Care and Use of Laboratory Animals.14
Experimental design and animal model of NEC
Pups were randomized to one of the following groups: (1) Sham, (2) NEC, (3) NEC+HA, and (4) HA alone. Sodium hyaluronate (Lifecore Biomedical, LLC, Chaska, MN) with a molecular weight of ~35,000 kDa (HA 35) was given to pups in the NEC+HA and HA groups by gavage at a concentration of 15 or 30 mg/kg body weight once daily for 3 days prior to induction of NEC and 1 h prior to bacterial administration (Fig. 1). The doses and intervals were based on previous studies done in large intestinal inflammation models.9,11
HA 35 administration in Dithizone/Klebsiella murine NEC model. Pups were randomized to one of the following groups: Sham; NEC; NEC+HA, and HA alone. HA 35 was given to pups in the NEC+HA and HA group by gavage at a concentration of 15 or 30 mg/kg body weight once daily for 3 days prior to induction of NEC and 1 h prior to bacterial administration. NEC was induced using the Paneth cell disruption and Klebsiella infection NEC-like model. I.P. injection of dithizone (33 mg/kg) was given at P14–16, followed by gavage administration of 1 × 108 CFU Klebsiella pneumoniae/kg. Pups were monitored for 10 h after gavage for clinical illness and survival
NEC was induced using the Paneth cell disruption and Klebsiella infection NEC-like model.15,16 Crl:CD1(ICR) pups (Charles River) at P14–P16 days of age received an intraperitoneal injection of dithizone (33 mg/kg) diluted in ethanol/ammonium hydroxide, followed by gavage administration of 1 × 108 colony-forming units (CFU) Klebsiella pneumoniae/kg (ATCC #10031, Manassas, VA). Pups were monitored for 10 h after gavage for clinical illness and survival.17 At the end of the experiment, surviving pups were euthanized, and blood and tissues were harvested for further analysis.
Macroscopic and microscopic evaluation of intestinal injury
Small intestines of pups were removed and visually inspected for macroscopic signs of NEC. Images were obtained using Amscope MU1803 microscope and digital camera (Irving, CA). Severity of gut injury was graded by a blinded investigator using a modified macroscopic gut scoring17 with a 3-point scoring system based on gut color and dilatation as follows: 0: no discoloration or dilatation; 1: patchy discoloration; 2: extensive discoloration and gut dilatation. For histological injury scoring, the terminal ileum was removed and fixed in 10% formalin buffer, then paraffin-embedded and stained with hematoxylin and eosin (H&E) for microscopic examination. Severity of intestinal injury was assessed based on a five-point scoring system previously developed by Jilling et al.;18 Grade 0: intact; Grade 1: distal epithelial sloughing; Grade 2: mid villus sloughing; Grade 3: complete villus necrosis with preservation of the crypts; and Grade 4: transmural necrosis. Scores were based on the highest score observed on three to five sections in a specimen. A score of ≥2 was defined as NEC.
In vivo intestinal permeability
To assess the effect of HA 35 on intestinal permeability in vivo, fluorescein isothiocyanate (FITC)-labeled dextran (molecular weight 4000) (Sigma-Aldrich Inc. FD4, St. Louis, MO) was used as previously described.19 Mice pups from each group received 44 mg/100 gm body weight FD4, suspended in sterile phosphate-buffered saline by orogastric gavage. Four hours later, pups were euthanized and serum levels of FD4 were measured by spectrophotofluorometry (Tecan, Maennedorf, Switzerland) at an excitation wavelength of 480 nm and emission wavelength of 520 nm after standard concentration curves were established.
Inflammatory cytokine quantification at plasma and intestine
Proinflammatory cytokines/chemokines (interleukin (IL)-1β, tumor necrosis factor (TNF)-α, IL-6, IL-12 p70, interferon (IFN)-γ, C-X-C chemokine motif ligand (CXCL)) and anti-inflammatory (IL-10) cytokines were measured in plasma and intestine using ProcartaPlex Mouse Cytokine & Chemokine Panel (Bioscience, San Diego, CA, USA) based on Luminex technology as per the manufacturer’s instructions. Small intestinal samples were homogenized using a bead beater (Next Advance INC, Troy, NY) in a buffer containing Calbiochem phosphatase and protease inhibitors (524625 and 535140, Millipore, Burlington, MA) and phenylmethanesulfonylfluoride (93482, Sigma-Aldrich, St. Louis, MO). Samples were run on a BioPlex 200 (Bio-Rad, Hercules, CA) and results were calculated based on a seven-point standard curve for each analyte. Final cytokine levels were normalized to total protein concentration (mg/ml) and reported as pg/ml for plasma and pg/mg for tissue levels.
Immunohistochemistry (IHC)
IHC was performed according to the manufacturer’s protocol using Leica Bond-IIITM Polymer Refine Detection system (DS 9800). Polyclonal antibodies claudin-2, -3, -4, and Z0-1 (Catalog #36-4800 and PA5-28858, ThermoFisher, Waltham, MA) and occludin (Catalog #40-4700, Invitrogen, Carlsbad, CA) were used. Formalin-fixed paraffin-embedded tissues were sectioned at desired thickness (4–8 µm) and mounted on positively charged slides. The slides were dried overnight at room temperature and incubated at 60 °C for 45 min followed by deparaffinization and rehydration in an automated multistainer (Leica ST5020). Subsequently, these slides were transferred to the Leica Bond-IIITM and treated for target retrieval at 100 °C for 20 min in a retrieval solution, either at pH 6.0 or pH 9.0. Endogenous peroxidase was blocked using peroxidase-blocking reagent, followed by the selected primary antibody incubation for 60 min diluted at (occludin, 1:200; ZO-1, 1:100; claudins, 1:100). For the secondary antibody, post-primary immunoglobulin G (IgG)-linker and/or Poly-horseradish peroxidase IgG reagents was used. Detection was done using 3, 3′-diaminobenzidine tetra hydrochloride as chromogen and counterstained with hematoxylin. Completed slides were dehydrated (Leica ST5020) and mounted (Leica MM24). Antibody-specific positive control and negative control (omission of primary antibody) were parallel stained. IHC slides stained for the specific TJ protein were read by a blinded pathologist.
Real-time RNA PCR
RNA was isolated from the terminal ileum tissue using the RNeasy Plus Mini Kit (74134, Qiagen, Germantown, MD) per the manufacturer’s instructions and reverse transcribed with a High Capacity cDNA Reverse Transcription Kit (4368814, Applied Biosystems, Foster City, CA). Samples were run in triplicate on ZO-1 (Hs01551861_m1), occludin (Hs00170162_m1), claudin-4 (Hs00976831_s1), claudin-3 (Hs00265816_s1), and claudin-2 (Hs00252666_s1), and values were normalized to ACTB (Hs01060665_g1) using a ΔΔCt analysis of the TaqMan assays and reported as fold change from sham.
Statistics
All data were analyzed and graphs created using the GraphPad Prism software version 6.00 for Windows (LA Jolla, CA, USA, www.graphpad.com). Survival curves to assess mortality were obtained using the Kaplan–Meier survival analysis. Data obtained from each group are presented as mean ± standard error of mean (S.E.M.) and analyzed using either unpaired t test or one-way analysis of variance with Tukey’s multi-comparison test, as appropriate. p value of <0.05 was considered significant.
Results
Oral HA 35 reduces mortality and severity of NEC-like intestinal injury
To determine whether HA 35 protects against experimental NEC, mice pups were given HA 35 (15 or 30 mg/kg), once daily, for 3 days prior to induction of NEC. NEC was induced using the Paneth cell ablation and Klebsiella infection model as described above.15 Pups were then monitored for a total of 10 h for survival and signs of distress. Pups in the NEC+HA 35 had increased survival in a concentration-dependent manner (Fig. 2a) with a survival of 90% in the NEC+HA 35 at 30 mg/kg compared to 70% in the NEC+HA 35 at 15 mg/kg and 50% in untreated NEC with a p value 0.04 and 0.05, respectively.
Kaplan–Meier survival curve a showing increased survival in HA-administered groups. Survival in low-dose HA (15 mg/kg) at 70% and high-dose HA (30 mg/kg) at 90% as compared to untreated NEC at 50% (p = 0.05 & p = 0.04, respectively). b Serum FITC levels were lower in NEC+HA 35 treatment compared to NEC with mean ± S.E.M. of 1554 ± 250 ng/ml in NEC+HA 30 mg/kg, 2456 ± 212 ng/ml in NEC+HA 15 mg/kg, and 5274 ± 389 ng/ml in untreated NEC. ****p < 0.0001. c Scatter plot of bacterial colony counts from blood cultures being significantly lower in NEC+HA 30 mg/kg compared to untreated NEC (mean ± S.E.M of 5426 ± 378 CFU/ml versus 12,722 ± 1519 CFU/ml, respectively. ***p < 0.0001. One-way ANOVA with Tukey’s multi-comparison test
Based on the mortality data, we next assessed the effect of HA 35 at only the 30 mg/kg dose on the incidence and severity of intestinal injury in the NEC model. Compared to the small intestines of pups in the sham group, the NEC group exhibited signs of inflammation, discoloration, and distension (Fig. 3). HA 35 resulted in improved overall gross appearance with reduced signs of dilation and discoloration (Fig. 3a) with a mean + S.E.M. score of 2.125 ± 0.31 compared to 3.25 ± 1 in untreated NEC (p < 0.01) (Fig. 3c). H&E examination of the ileal section in the sham group showed normal, healthy villi and submucosal structure. In contrast, sections from the NEC group showed signs of moderate-to-severe injury with separation of the submucosa and in certain cases transmural necrosis (Fig. 3b). Notably, HA 35 administration in NEC was associated with attenuated histological injury (Fig. 3d) with a mean ± S.E.M. scoring of 1.2 ± 0.25 compared to 2.3 ± 0.15 in the NEC group (p < 0.01).
HA 35 reduces the severity of small intestinal injury in murine NEC. Representative gross (a) and H&E images (b) of the small intestine from the groups. c HA 35 administration was associated with decreased gross appearance of injury with a mean ± S.E.M. macroscopic score of 2.125 ± 0.31 compared 3.25 ± 1 in the NEC group. **p < 0.01. d Histological NEC severity scores of a mean ± S.E.M. of 1.2 ± 0.25 in the NEC+HA 35 group versus 2.3 ± 0.15 in the untreated NEC group. **p < 0.01. Data are in mean ± S.E.M. Results are representative of at least six animals and at least two separate experiments. One-way ANOVA with Dunnet’s multi-comparison test
HA 35 protects intestinal barrier function in NEC model
Disruption of the intestinal epithelial barrier predisposes to bacterial translocation, intestinal inflammation, and NEC.3,20,21 Previous studies have shown that HA 35 maintains intestinal integrity and decreases intestinal permeability in vivo in various murine colitis models.12 To determine the effect of HA 35 on intestinal permeability in NEC, serum levels of FITC–dextran were measured in all surviving pups 4 h after administration of FD4. As expected, pups in the NEC group had elevated serum levels of FITC compared to shams with a mean ± S.E.M 5274 ± 389 versus 1730 ± 250 ng/ml, respectively, p < 0.0001, indicating an impaired barrier function in the NEC group (Fig. 2b). HA 35 treatment in NEC significantly decreased FITC levels in serum in a concentration-dependent manner with a mean ± S.E.M. of 1554 ± 250 ng/ml in the NEC+HA 35 at 30 mg/kg versus 2456 ± 212 ng/ml in the NEC+HA 35 at 15 mg/kg (p < 0.0001). Based on these results, we next determined the effect of HA 35 on bacteremia associated with the NEC model. In a separate experiment, blood culture was collected by intracardiac puncture an hour after oral Klebsiella administration. HA 35 treatment was associated with twofold reduction in bacterial CFU/ml in the blood compared to untreated NEC, with a mean ± S.E.M. of 5426 ± 378 CFU/ml compared to 12,722 ± 1519 CFU/ml in the untreated NEC group (Fig. 2c; p < 0.0001). Live bacteria were undetected by culture methods in the liver and spleens of pups from all groups (data not shown). Altogether, these results indicate that HA 35 administration in NEC leads to reduced intestinal permeability and bacteremia.
HA 35 decreases levels of NEC-induced inflammatory cytokine levels
Cytokine/chemokine dysregulation plays an important role in the pathogenesis of NEC as demonstrated in human and animal models of NEC where increased expression of inflammatory mediators such as TNF, IL-Iβ, IL-6, IL-8, and others were seen in both intestinal tissues and plasma. Studies also suggest that cytokines released in NEC could further damage the epithelial barrier. We therefore determined the effect of HA 35 on pro- and anti-inflammatory cytokine expression in plasma and intestines of all the groups. Pups treated with HA 35 at both doses, 15 and 30 mg/kg, had lower plasma levels of IFN-γ (15 mg/kg, not significant; 30 mg/kg, p = 0.0149), TNF-α (p = 0.0483, p = 0.0018), Gro-α (p = 0.0003, p < 0.0001), IL-12ρ70 (p = 0.0003), and IL-6, (p < 0.0001) as compared to pups in the untreated NEC group, respectively (Fig. 4). Cytokine expression in the intestine for TNF-α, IFN-γ, IL-6, CXCL, and IL-1β showed a lower trend for the HA-treated groups but did not achieve statistical significance. No significant differences in anti-inflammatory cytokine expression (IL-10) was noted between HA-treated NEC and untreated NEC both in the plasma and intestines.
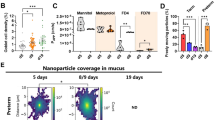
HA 35 administration decreases the systemic (plasma) pro-inflammatory cytokine release in NEC-like model. Pro-inflammatory cytokine levels of a TNF-α (*p = 0.0483, **p = 0.0018), b Gro-α (***p = 0.0003, ****p < 0.0001), c IL-12ρ70 (***p = 0.0003), and d IL-6 (****p < 0.0001) were decreased in NEC+HA 35 compared to untreated NEC. Data are in mean ± S.E.M. Results are representative of more than six animals and at least two separate experiments. One-way ANOVA with Tukey’s multi-comparison test
HA 35 increases TJ expression in NEC
Intestinal epithelial integrity is maintained by TJs, which play a major role in regulating intestinal permeability. Alterations in the expression or localization of TJ proteins occurs in intestinal inflammation models, such as inflammatory bowel diseases and NEC.3,22 Importantly, HA 35 administration maintained intestinal permeability and increased ZO-1 expression in both healthy and dextran sodium sulfate (DSS)-treated wild-type mice.12 We therefore sought to determine the effect of HA 35 on localization, intensity, and expression of claudins -2, -3, -4, occludin, and ZO-1. We found that in shams claudin-2 and ZO-1 (Fig. 5) staining was mainly located in the cytoplasm and apical region, while occludin, claudin-3, and -4 were localized in the cytoplasm and lateral walls (Fig. 5). Similar to other studies, staining intensity of occludin was noted to be decreased in the NEC group compared to shams, while claudin-2 staining, a pore-forming TJ, was increased in NEC. Intensity staining and localization of ZO-1 was not affected in NEC compared to sham. Importantly, HA 35-treated pups had increased staining intensity for all TJ proteins in the healthy and NEC-challenged pups. Moreover, occludin and claudin-3 localization in the HA-treated groups were similar to shams, concentrated mainly in the cytoplasm and lateral cytoplasmic membrane at basal crypt regions. Claudin-4 staining was also increased in the HA-treated pups and localized mainly at the tips of the villi in the lateral cytoplasmic membranous region. RNA expression by quantitative PCR showed significantly upregulated expression of all the TJs in the HA 35-treated healthy and NEC+HA 35 groups compared to untreated NEC and shams. On the other hand, the expression of claudin-2 and 3 was downregulated in the NEC group.
Immunohistochemical staining images (×10 and ×40 inserts) for TJ proteins and the corresponding qPCR RNA analysis. HA 35-treated pups showed increased intensity of staining in healthy and NEC-challenged pups for all TJ proteins. Insert ×40 images showing increased cryptal intensity of staining in HA 35-treated healthy and NEC-challenged pups for TJ occludin (a) and claudin-3 (c). Claudin-4 (b) staining was increased in the lateral cytoplasmic membranes of the tips of villi. Insert ×40 images showing cytoplasmic staining for ZO-1 (d) in tips of villi in all groups and increased cytoplasmic cryptal staining for claudin-2 (e) noted in the NEC group. RNA PCR results showed upregulated expression of occludin, claudin-4, claudin-3, ZO-1, and claudin-2 in HA 35 and NEC+HA 35 groups compared to untreated NEC (f–j). Claudin-3 RNA expression was downregulated in the NEC group compared to sham (h), while RNA expression for ZO-1 and claudin-2 was upregulated in the HA 35 and NEC+HA 35 group compared to untreated NEC (i, j). Data represent mean + S.E.M. Analysis was done by two-way ANOVA with Tukey’s multi-comparison test
Discussion
Altogether, our study shows that oral HA 35 increases survival and reduces incidence and severity of intestinal injury in Paneth cell ablation and Klebsiella infection NEC model. HA 35 also reduced intestinal permeability, bacteremia, and systemic inflammatory response in the NEC model. While the pathogenesis of NEC remains unclear, altered intestinal microbiome, immature intestinal defenses and barrier, and exaggerated inflammatory response play major roles in the disease.20 Though increased intestinal permeability is a predisposing factor for developing NEC, intestinal inflammation itself can lead to increased gut permeability, resulting in a positive feedback loop. The net effect is increased inflammatory cytokine release, leukocyte infiltration, epithelial necrosis, and bacterial translocation across the lumen.4,7,23
Research efforts have been ongoing to develop nutritional or pharmacological strategies that promote intestinal integrity and modulate intestinal inflammation in preterm infants. HM has been proven to be safe and protective in human studies.5 Compared to formula, HM decreases intestinal permeability and enhances the underdeveloped physical barrier, likely due to its bioactive components, such as lactoferrin, immunoglobulin, and oligosaccharides. HM is also rich in GAGs (HA, chondroitin sulfate, heparin, heparan sulfate) early in lactation suggesting an important role of this component in the neonatal period.24 We previously showed that chondroitin sulfate in HM protects against intestinal bacterial infection through a reduction in both invasion and translocation.25 In addition, GAGs have been shown to play an important role in innate intestinal immunity as an antioxidant and by promoting microbial colonization of the intestine.26 Specifically, HA is synthesized by one of the HASs and has either pro- or anti-inflammatory properties depending on the size and tissue environment. Mice pretreated intraperitoneally with HA < 500 kDa are resistant to lipopolysaccharide-induced sepsis.27 HA isolated from HM or commercially available HA 35 enhances intestinal innate immunity, decreases intestinal permeability in colitis models, and attenuates ethanol-induced gut and liver injury partly through maintaining intestinal barrier function.12,24,28 Notably, of all the specific sized HA (HA 4.7, 16, 28, 74 kDa), HA 35 was the most potent inducer of TJ proteins and antimicrobial peptide expression in colonic epithelium in vitro. Importantly, large molecular weight (HA 2000 kDa) had no effect on TJ protein expression, suggesting that this effect is highly size specific.29 Similarly, we found that prophylactic HA 35 was protective in NEC model and was associated with twofold reduction in intestinal permeability as assessed by serum FITC level and levels of bacteremia and systemic proinflammatory response.
Several mechanisms could lead to the protective effect of HA in the NEC model we used in our study, including direct or indirect effects on bacteria such as competitive and direct binding of HA to bacteria or inhibiting bacterial growth. In a clinical trial, the use of HA and chondroitin sulfate as a combination was superior to standard of care in preventing recurrence of urinary tract infection.30 In vitro, high-molecular-weight HA (<750 kDa) was shown to act as a bacteriostatic agent, with no bactericidal effects, mainly against Gram-positive bacteria.31,32 Though not addressed in our study, HA 35 could be protective by acting as a bacteriostatic agent and dampening the effect of the Klebsiella challenge in the model, thereby reducing the levels of bacteremia, systemic inflammation, and mortality. It is also possible that the protective effects of HA 35 on NEC- induced increased permeability and bacteremia is indirectly through reducing intestinal histological injury, specifically cell necrosis and apoptosis.
Another potential protective mechanism of HA in NEC could be through its effect on TJ expression and localization. Claudins, occludin, and ZO-1 are complex transmembrane proteins located at the apical and lateral ends of the cells and play a role in regulating selective intestinal permeability.22 Increased endocytosis or decreased exocytosis of these proteins from cytoplasm to cytoplasmic membrane or decreased expression can occur during intestinal inflammation resulting in disassembly of the junction and translocation of antigens and bacteria.33 Studies from humans and animal models of NEC confirm the importance of optimal localization and/or expression of these TJs in maintaining intestinal epithelial integrity and prevention of NEC.34 Similar to others, we showed decreased intensity staining and altered localization of the barrier forming claudin-3, claudin-4, and occludin in the NEC group. Notably, HA 35 therapy was associated with increased staining intensity expression for most of the TJs studied in both healthy pups and pups challenged with NEC. These data support findings by other studies where HA 35 administration enhanced TJ expression in colonic epithelium of healthy and Citrobacter-infected mice.12 Similar to studies from human patients with NEC, staining intensity for claudin-2, a pore-forming TJ, was higher and more localized within crypts in the NEC group compared to sham.2 HA 35 prevented the increased localization of claudin-2 in the NEC animals; however, in contrast to the IHC staining data, gene expression for claudin-2 was higher in the HA-treated groups. However, this gene expression increase was not associated with increased intestinal permeability in vivo.
Our study has several limitations. First, the effect of HA on the intestinal microbiome was not evaluated. Similar to other glycans, HA is non-digestible and has been shown to prevent bacterial adhesion and inhibit bacterial growth.26,35,36,37,38 Moreover, HA 35 administration was protective in a bacterial infection model by increasing β-defensin expression in intestinal epithelium in vivo and in vitro.10 These data raise an intriguing possibility that HA could act as a prebiotic and could potentially alter the intestinal microbial composition of neonatal pups, thereby preventing the development of NEC. Second, our study did not address the mechanism by which HA 35 affects TJ expression in the NEC model. It is well known that HA exerts its effect by interacting with the signaling pathway receptors Toll-like receptors 4 and 2 (TLR4 and TLR2) and CD44.9 In an ethanol-induced liver injury model, HA 35 given orally restored Toll-interacting protein (Tollip) and decreased TNF-α expression. Tollip is an ubiquitously expressed protein that forms a complex with the IL-1 receptor-associated kinase 1 and impairs the activation of nuclear factor-κB. Tollip also decreases TLR4- and TLR2-mediated inflammation by direct interaction with the receptors.28 Interestingly, NEC is characterized by an imbalance between TLR4 activation and its negative regulators. Specifically, TOLLIP expression is lower in both immature enterocytes23 and NEC models leading to the exaggerated inflammatory response in immature intestines as compared to term infants and adult. Third, only specific size HA 35 was used in our study based on the previous studies.9,11,24 Data on lower-molecular- or higher-molecular-weight HA in the NEC model is currently unknown. Moreover, only 15 and 30 mg/kg dosing was used in the study based on prior studies in larger intestinal models.9,11,24 Further studies are needed to determine whether higher doses are more beneficial or detrimental in NEC. Lastly, the Paneth cell disruption and Klebsiella infection model used in this study has some limitations. Similar to other murine NEC models, it does not encompass all the risk factors that contribute to NEC. However, it offers the advantage of challenging pups at P14 with the intestinal developmental age similar to that of infants at highest risk of developing NEC.39 In addition, it results in an end point of impaired barrier function, intestinal inflammation, bacterial dysbiosis, and histological injury similar to that seen in the classical hypoxia/hypothermia model and that of human infants with NEC.15,40
In conclusion, we have demonstrated that HA 35 administration prevents mortality and reduces intestinal permeability in a NEC-like intestinal injury model. This protective effect of HA 35 in the model was at least in part due to enhanced intestinal barrier function and preservation of the TJ expression and localization. These data support the concept that oral HA may be effective as a prophylactic treatment that promotes intestinal barrier function in premature infants and prevents the development of NEC. Further studies are needed to elucidate the mechanism of action and determine its effects in other NEC models and on the intestinal microbiome.
References
Rees, C. M., Eaton, S. & Pierro, A. Trends in infant mortality from necrotising enterocolitis in England and Wales and the USA. Arch. Dis. Child. Fetal Neonatal Ed. 93, F395–F396 (2008).
Bergmann, K. R. et al. Bifidobacteria stabilize claudins at tight junctions and prevent intestinal barrier dysfunction in mouse necrotizing enterocolitis. Am. J. Pathol. 182, 1595–1606 (2013).
Moore, S. A. et al. Intestinal barrier dysfunction in human necrotizing enterocolitis. J. Pediatr. Surg. 51, 1907–1913 (2016).
Tanner, S. M. et al. Pathogenesis of necrotizing enterocolitis: modeling the innate immune response. Am. J. Pathol. 185, 4–16 (2015).
Sullivan, S. et al. An exclusively human milk-based diet is associated with a lower rate of necrotizing enterocolitis than a diet of human milk and bovine milk-based products. J. Pediatr. 156, 562–567.e1 (2010).
Maffei, D. & Schanler, R. J. Human milk is the feeding strategy to prevent necrotizing enterocolitis! Semin. Perinatol. 41, 36–40 (2017).
Denning, T. L., Bhatia, A. M., Kane, A. F., Patel, R. M. & Denning, P. W. Pathogenesis of NEC: role of the innate and adaptive immune response. Semin. Perinatol. 41, 15–28 (2017).
Coppa, G. V. et al. Human milk glycosaminoglycans: the state of the art and future perspectives. Ital. J. Pediatr. 39, 2 (2013).
Hill, D. R. et al. Human milk hyaluronan enhances innate defense of the intestinal epithelium. J. Biol. Chem. 288, 29090–29104 (2013).
Kessler, S. P., Obery, D. R. & de la Motte, C. Hyaluronan synthase 3 null mice exhibit decreased intestinal inflammation and tissue damage in the DSS-induced colitis model. Int. J. Cell Biol. 2015, 745237 (2015).
Hill, D. R., Kessler, S. P., Rho, H. K., Cowman, M. K. & de la Motte, C. A. Specific-sized hyaluronan fragments promote expression of human beta-defensin 2 in intestinal epithelium. J. Biol. Chem. 287, 30610–30624 (2012).
Kim, Y. et al. Hyaluronan 35kDa treatment protects mice from Citrobacter rodentium infection and induces epithelial tight junction protein ZO-1 in vivo. Matrix Biol. 62(Supplement C), 28–39 (2017).
Kessler, S. P. et al. Multifunctional role of 35 kilodalton hyaluronan in promoting defense of the intestinal epithelium. J. Histochem. Cytochem. 66, 273–287 (2018).
National Research Council (US) Committee for the Update of the Guide for the Care and Use of Laboratory Animals. Guide for the Care and Use of Laboratory Animals (National Academies, 1985).
Zhang, C. et al. Paneth cell ablation in the presence of Klebsiella pneumoniae induces necrotizing enterocolitis (NEC)-like injury in the small intestine of immature mice. Dis. Model. Mech. 5, 522–532 (2012).
Eckert, J., Scott, B., Lawrence, S. M., Ihnat, M. & Chaaban, H. FLLL32, a curcumin analog, ameliorates intestinal injury in necrotizing enterocolitis. J. Inflamm. Res. 10, 75–81 (2017).
Zani, A. et al. Assessment of a neonatal rat model of necrotizing enterocolitis. Eur. J. Pediatr. Surg. 18, 423–426 (2008).
Jilling, T., Lu, J., Jackson, M. & Caplan, M. S. Intestinal epithelial apoptosis initiates gross bowel necrosis in an experimental rat model of neonatal necrotizing enterocolitis. Pediatr. Res. 55, 622–629 (2004).
Gupta, J. & Nebrada, A. R. Analysis of intestinal permeability in mice. Bio-Protoc. 4, e1289 (2014).
Anand, R. J., Leaphart, C. L., Mollen, K. P. & Hackam, D. J. The role of the intestinal barrier in the pathogenesis of necrotizing enterocolitis. Shock 27, 124–133 (2007).
Hackam, D. J., Upperman, J. S., Grishin, A. & Ford, H. R. Disordered enterocyte signaling and intestinal barrier dysfunction in the pathogenesis of necrotizing enterocolitis. Semin. Pediatr. Surg. 14, 49–57 (2005).
Suzuki, T. Regulation of intestinal epithelial permeability by tight junctions. Cell. Mol. Life Sci. 70, 631–659 (2013).
Nanthakumar, N. et al. The mechanism of excessive intestinal inflammation in necrotizing enterocolitis: an immature innate immune response. PLoS ONE 6, e17776 (2011).
Motte, C. Adl Hyaluronan in intestinal homeostasis and inflammation: implications for fibrosis. Am. J. Physiol. Gastrointest. Liver Physiol. 301, G945–G949 (2011).
Burge, K. Y., Hannah, L., Eckert, J. V., Gunasekaran, A. & Chaaban, H. The protective influence of chondroitin sulfate, a component of human milk, on intestinal bacterial invasion and translocation. J. Hum. Lact. 35, 538–549 (2019).
Newburg, D. S. & Morelli, L. Human milk and infant intestinal mucosal glycans guide succession of the neonatal intestinal microbiota. Pediatr. Res. 77, 115–120 (2015).
Muto, J., Yamasaki, K., Taylor, K. R. & Gallo, R. L. Engagement of CD44 by hyaluronan suppresses TLR4 signaling and the septic response to LPS. Mol. Immunol. 47, 449–456 (2009).
Saikia, P. et al. Hyaluronic acid 35 normalizes TLR4 signaling in Kupffer cells from ethanol-fed rats via regulation of microRNA291b and its target Tollip. Sci. Rep. 7, 15671 (2017).
Kim, Y. et al. Layilin is critical for mediating hyaluronan 35kDa-induced intestinal epithelial tight junction protein ZO-1 in vitro and in vivo. Matrix Biol. 66, 93–109 (2018).
Ciani, O. et al. Intravesical administration of combined hyaluronic acid (HA) and chondroitin sulfate (CS) for the treatment of female recurrent urinary tract infections: a European multicentre nested case-control study. BMJ Open 6, e009669 (2016).
Carlson, G. A. et al. Bacteriostatic properties of biomatrices against common orthopaedic pathogens. Biochem. Biophys. Res. Commun. 321, 472–478 (2004).
Pirnazar, P. et al. Bacteriostatic effects of hyaluronic acid. J. Periodontol. 70, 370–374 (1999).
Lechuga, S. & Ivanov, A. I. Disruption of the epithelial barrier during intestinal inflammation: Quest for new molecules and mechanisms. Biochim. Biophys. Acta 1864, 1183–1194 (2017).
Halpern, M. D. & Denning, P. W. The role of intestinal epithelial barrier function in the development of NEC. Tissue Barriers 3, e1000707 (2015).
Newburg, D. S., Ruiz-Palacios, G. M. & Morrow, A. L. Human milk glycans protect infants against enteric pathogens. Annu. Rev. Nutr. 25, 37–58 (2005).
Coppa, G. V. et al. Human milk glycosaminoglycans inhibit in vitro the adhesion of Escherichia coli and Salmonella fyris to human intestinal cells. Pediatr. Res. 79, 603–607 (2016).
Drago, L. et al. Antiadhesive and antibiofilm activity of hyaluronic acid against bacteria responsible for respiratory tract infections. APMIS 122, 1013–1019 (2014).
Romanò, C. L., De Vecchi, E., Bortolin, M., Morelli, I. & Drago, L. Hyaluronic acid and its composites as a local antimicrobial/antiadhesive barrier. J. Bone Jt. Infect. 2, 63–72 (2017).
Stanford, A. H. et al. A direct comparison of mouse and human intestinal development using epithelial gene expression patterns. Pediatr Res. https://doi.org/10.1038/s41390-019-0472-y (2019).
Lueschow, S. R. et al. Loss of murine Paneth cell function alters the immature intestinal microbiome and mimics changes seen in neonatal necrotizing enterocolitis. PLoS ONE 13, e0204967 (2018).
Acknowledgements
We thank the Stephenson Cancer Center at the University of Oklahoma, Oklahoma City, OK and an Institutional Development Award (IDeA) from the National Institute of General Medical Sciences of the National Institutes of Health under grant number P20 GM103639 for the use of Histology and Immunohistochemistry Core, which provided processing and embedding/tissue staining/immunohistochemistry services. A.G. received funding from The Children Hospital Foundation, Oklahoma City; H.C. received funding from NIGMS K08GM127308 and Presbyterian Health Foundation.
Author information
Authors and Affiliations
Contributions
A.G. contributed to the conception and design, animal experiments, and drafting the article. J.E. contributed to the experimental design, animal experiments, and data analysis. K.B. contributed to the animal experiments, data analysis, and critically reviewing the article. Z.Y. contributed to the data analysis and interpretation and revising the article. S.K. contributed to the conception and design. C.d.l.M. contributed to the conception and design and revising the article. H.C. contributed to the conception and design, animal experiments, data analysis, and revising and final approval of the version to be published.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gunasekaran, A., Eckert, J., Burge, K. et al. Hyaluronan 35 kDa enhances epithelial barrier function and protects against the development of murine necrotizing enterocolitis. Pediatr Res 87, 1177–1184 (2020). https://doi.org/10.1038/s41390-019-0563-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-019-0563-9
This article is cited by
-
Review of claudin proteins as potential biomarkers for necrotizing enterocolitis
Irish Journal of Medical Science (1971 -) (2021)
-
Insights Image for “Hyaluronan 35 kDa enhances epithelial barrier function and protects against the development of murine necrotizing enterocolitis”
Pediatric Research (2020)