Abstract
Objective
To examine the impact of COVID-19 pandemic on early intervention (EI) services in VLBW infants.
Study design
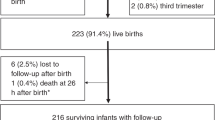
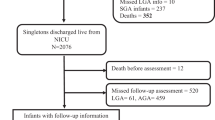
208 VLBW infants seen in NICU follow-up (FU) pre-COVID-19 were compared to 132 infants seen during COVID-19 at 4, 8 and 20 months corrected age (CA) in terms of enrollment in Child and Family Connections (CFC; intake agency for EI), EI therapies, need for CFC referral and Bayley scores.
Results
Infants seen during COVID-19 at 4, 8 and 20 months CA were 3.4 (OR, 95% CI 1.64, 6.98), 4.0 (1.77, 8.95) and 4.8 (2.10, 11.08) times more likely to need CFC referral at FU based on severity of developmental delay. Infants followed during COVID-19 had significantly lower mean Bayley cognitive and language scores at 20 months CA.
Conclusions
VLBW infants seen during COVID-19 had significantly higher odds of needing EI and significantly lower cognitive and language scores at 20 months CA.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Organization WH. Third round of the global pulse survey on continuity of essential health services during the COVID-19 pandemic. Interim report. Health Services Performance Assessment WHH; 2022. Report No.: WHO Reference Number: WHO/2019-nCoV/EHS_continuity/survey/2022.1.
Lipner HS, Huron RF. Developmental and Interprofessional Care of the Preterm Infant: Neonatal Intensive Care Unit Through High-Risk Infant Follow-up. Pediatr Clin North Am. 2018;65:135–41.
Spittle A, Orton J, Anderson PJ, Boyd R, Doyle LW. Early developmental intervention programmes provided post hospital discharge to prevent motor and cognitive impairment in preterm infants. Cochrane Database Syst Rev. 2015;2015:CD005495.
Bayley N. Bayley Scales of Infant and Toddler Development. 3rd edn. San Antonio, TX: Harcourt Assessment Inc.; 2006.
Fenton TR. A new growth chart for preterm babies: Babson and Benda’s chart updated with recent data and a new format. BMC Pediatr. 2003;3:13.
Bell MJ, Ternberg JL, Feigin RD, Keating JP, Marshall R, Barton L, et al. Neonatal necrotizing enterocolitis. Therapeutic decisions based upon clinical staging. Ann Surg. 1978;187:1–7.
Miller K, Berentson G, Roberts H, McMorris C, Needelman H. Examining early intervention referral patterns in neonatal intensive care unit follow up clinics using telemedicine during COVID-19. Early Hum Dev. 2022;172:105631.
Roberts MY, Thornhill L, Lee J, Zellner MA, Sudec L, Grauzer J, et al. The Impact of COVID-19 on Illinois Early Intervention Services. Am J Speech Lang Pathol. 2022;31:974–81.
Jeste S, Hyde C, Distefano C, Halladay A, Ray S, Porath M, et al. Changes in access to educational and healthcare services for individuals with intellectual and developmental disabilities during COVID-19 restrictions. J Intellect Disabil Res. 2020;64:825–833.
Kowanda M, Cartner L, Kentros C, Geltzeiler AR, Singer KE, Weaver WC, et al. Availability of Services and Caregiver Burden: Supporting Individuals With Neurogenetic Conditions During the COVID-19 Pandemic. J Child Neurol. 2021;36:760–7.
Levin-Decanini T, Henderson C, Mistry S, Dwarakanath N, Ray K, Miller E, et al. Decreased access to therapeutic services for children with disabilities during COVID-19 stay-at-home orders in Western Pennsylvania. J Pediatr Rehabil Med. 2022;15:517–21.
Murphy A, Pinkerton LM, Bruckner E, Risser HJ. The impact of the novel coronavirus disease 2019 on therapy service delivery for children with disabilities. J Pediatr. 2021;231:168–77.e1
Neece C, McIntyre LL, Fenning R. Examining the impact of COVID-19 in ethnically diverse families with young children with intellectual and developmental disabilities. J Intellect Disabil Res. 2020;64:739–49.
Cole B, Pickard K, Stredler-Brown A. Report on the use of telehealth in early intervention in Colorado: Strengths and challenges with telehealth as a service delivery method. Int J Telerehabil. 2019;11:33–40.
Ferrari E, Palandri L, Lucaccioni L, Talucci G, Passini E, Trevisani V. et al. The Kids Are Alright (?). Infants’ Development and COVID-19 Pandemic: A Cross-Sectional Study. Int J Public Health. 2022;67:1604804.
Huang P, Zhou F, Guo Y, Yuan S, Lin S, Lu J, et al. Association Between the COVID-19 Pandemic and Infant Neurodevelopment: A Comparison Before and During COVID-19. Front Pediatrics. 2021;9:1–11.
Shuffrey LC, Firestein MR, Kyle MH, Fields A, Alcantara C, Amso D, et al. Association of Birth During the COVID-19 Pandemic With Neurodevelopmental Status at 6 Months in Infants With and Without In Utero Exposure to Maternal SARS-CoV-2 Infection. JAMA Pediatr. 2022;176:e215563.
Giesbrecht GL, Catherine; Dennis, Cindy-Lee; Tough, Suzanne; McDonald, Sheila; Tomfohr-Madsen, Lianne. Increased risk for developmental delay among babies born during the pandemic. PsyArXiv. 2022; Preprinted posted online.
Imboden A, Sobczak BK, Griffin V. The impact of the COVID-19 pandemic on infant and toddler development. J Am Assoc Nurse Pract. 2021.
Hessami K, Norooznezhad AH, Monteiro S, Barrozo ER, Abdolmaleki AS, Arian SE, et al. COVID-19 Pandemic and Infant Neurodevelopmental Impairment: A Systematic Review and Meta-analysis. JAMA Netw Open. 2022;5:e2238941.
Costa P, Cruz AC, Alves A, Rodrigues MC, Ferguson R. The impact of the COVID-19 pandemic on young children and their caregivers. Child Care Health Dev. 2022;48:1001–7.
Lemmon ME, Chapman I, Malcolm W, Kelley K, Shaw RJ, Milazzo A, et al. Beyond the First Wave: Consequences of COVID-19 on High-Risk Infants and Families. Am J Perinatol. 2020;37:1283–8.
Ehrler M, Werninger I, Schnider B, Eichelberger DA, Naef N, Disselhoff V, et al. Impact of the COVID-19 pandemic on children with and without risk for neurodevelopmental impairments. Acta Paediatr. 2021;110:1281–8.
De Leon IC, Philipps J, Yoegel M, Byrnes J, Kase JS. Comparison of Goal Achievement When Transitioning from In-Person Therapy to Teletherapy in Westchester County Early Intervention Program Due to the COVID-19 Pandemic. Int J Telerehabil. 2022;14:e6450.
Kronberg J, Tierney E, Wallisch A, Little LM. Early Intervention Service Delivery via Telehealth During COVID-19: A Research-Practice Partnership. Int J Telerehabil. 2021;13:e6363.
Author information
Authors and Affiliations
Contributions
JD compiled the data, drafted and revised the manuscript; CW compiled the data, revised the manuscript; MK compiled the data, revised the manuscript; TJ designed the study, analyzed the data, drafted and revised the manuscript; MG designed the study, revised the manuscript; EL revised the manuscript; KP designed the study, drafted and revised the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
David, J., Wambach, C.G., Kraemer, M. et al. Impact of the COVID-19 pandemic on early intervention utilization and need for referral after NICU discharge in VLBW infants. J Perinatol 44, 40–45 (2024). https://doi.org/10.1038/s41372-023-01711-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01711-7