Abstract
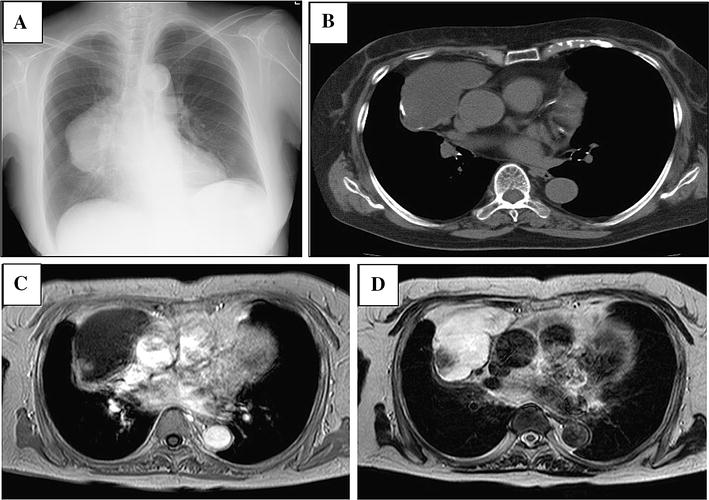
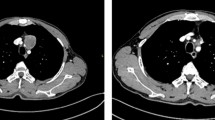
Mucinous adenocarcinoma of the thymus is a particularly rare type among thymic carcinomas. Here, we report a patient who underwent complete surgical resection of the primary mucinous adenocarcinoma of the thymus. She was 74 years old and presented with a 60-mm multilocular cystic tumor in her right anterior mediastinum. We performed extended thymo-thymectomy with partial resection of the right upper lobe and pathologically diagnosed the patient with Masaoka stage II mucinous adenocarcinoma of the thymus. Immunohistochemistry showed the absence of PD-L1, suggesting that immune check point inhibitors targeting PD-1/PD-L1 might not be effective in this case. The increased preoperative serum levels of CA19-9 decreased after the operation. CA19-9 is a biomarker for disease status. Future reports should help elucidate the pathogenesis of this disease.


Similar content being viewed by others
References
Suster S, Moran CA. Thymic carcinoma: spectrum of differentiation and histologic types. Pathology. 1998;30(2):111–22.
Choi WW, Lui YH, Lau WH, Crowley P, Khan A, Chan JK. Adenocarcinoma of the thymus: report of two cases, including a previously undescribed mucinous subtype. Am J Surg Pathol. 2003;27(1):124–30.
Kinoshita F, Shoji F, Takada K, Toyokawa G, Okamoto T, Yano T, et al. Mucinous adenocarcinoma of the thymus: report of a case. Gen Thorac Cardiovasc Surg. 2018;66(2):111–5.
Maeda D, Ota S, Ikeda S, Kawano R, Hata E, Nakajima J, et al. Mucinous adenocarcinoma of the thymus: a distinct variant of thymic carcinoma. Lung Cancer. 2009;64(1):22–7.
Sakanoue I, Hamakawa H, Fujimoto D, Imai Y, Minami K, Tomii K, et al. KRAS mutation-positive mucinous adenocarcinoma originating in the thymus. J Thorac Dis. 2017;9(8):E694–7.
Moser B, Schiefer AI, Janik S, Marx A, Prosch H, Pohl W, et al. Adenocarcinoma of the thymus, enteric type: report of 2 cases, and proposal for a novel subtype of thymic carcinoma. Am J Surg Pathol. 2015;39(4):541–8.
Takahashi F, Tsuta K, Matsuno Y, Takahashi K, Toba M, Sato K, et al. Adenocarcinoma of the thymus: mucinous subtype. Hum Pathol. 2005;36(2):219–23.
Seki E, Aoyama K, Ueda M, Haga T, Nakazato Y, Iijima M, et al. Mucinous adenocarcinoma of the thymus: a case report. J Thorac Oncol. 2008;3(8):935–7.
Kapur P, Rakheja D, Bastasch M, Molberg KH, Sarode VR. Primary mucinous adenocarcinoma of the thymus: a case report and review of the literature. Arch Pathol Lab Med. 2006;130(2):201–4.
Ra SH, Fishbein MC, Baruch-Oren T, Shintaku P, Apple SK, Cameron RB, et al. Mucinous adenocarcinomas of the thymus: report of 2 cases and review of the literature. Am J Surg Pathol. 2007;31(9):1330–6.
Abdul-Ghafar J, Yong SJ, Kwon W, Park IH, Jung SH. Primary thymic mucinous adenocarcinoma: a case report. Korean J Pathol. 2012;46(4):377–81.
Seki Y, Imaizumi M, Shigemitsu K, Yoshioka H, Ueda Y. Mucinous adenocarcinoma of the anterior mediastinum. Kyobu Geka. 2004;57(5):413–6.
Seon HJ, Kim KH, Choi YD, Song SY, Yoon HJ, Kim YH, et al. Angina pectoris caused by the extrinsic compression of coronary artery by primary thymic mucinous adenocarcinoma. Int J Cardiol. 2012;156(1):e13–5.
Maghbool M, Ramzi M, Nagel I, Bejarano P, Siebert R, Saeedzadeh A, et al. Primary adenocarcinoma of the thymus: an immunohistochemical and molecular study with review of the literature. BMC Clin Pathol. 2013;13(1):17.
Hishima T, Fukayama M, Fujisawa M, Hayashi Y, Arai K, Funata N, et al. CD5 expression in thymic carcinoma. Am J Pathol. 1994;145(2):268–75.
Yokoyama S, Miyoshi H. Thymic tumors and immune checkpoint inhibitors. J Thorac Dis. 2018;10(Suppl 13):S1509–15.
Guo M, Tomoshige K, Meister M, Muley T, Fukazawa T, Tsuchiya T, et al. Gene signature driving invasive mucinous adenocarcinoma of the lung. EMBO Mol Med. 2017;9(4):462–81.
Ballehaninna UK, Chamberlain RS. The clinical utility of serum CA 19-9 in the diagnosis, prognosis and management of pancreatic adenocarcinoma: An evidence based appraisal. J Gastrointest Oncol. 2012;3(2):105–19.
Acknowledgements
We thank M. Futakuchi for technical support and discussion.
Availability of Data and Materials
Not applicable
Code Availability
Not applicable
Funding
This work was supported in part by the NIH (grant number R01CA240317), Cincinnati Children’s Hospital Medical Center (GAP funding to Y.M.).
Author information
Authors and Affiliations
Contributions
K.T., Takuro M., and T.N. were involved in the design and conception of the study. Takamune M., R.D., R.M., S.M., and Takuro M. were involved with perioperative care and interpreted the data. K.T., Takuro M., K.M., T.T., Y.M., and T.N. reviewed and revised the manuscript. All the authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
All authors have no conflicts of interest to declare.
Ethics Approval and Consent to Participate
Not applicable. Written informed consent was obtained from the patient. This consent is for all potentially identifiable clinical data and accompanying images and is available for review by the editor of SN Comprehensive Clinical Medicine.
Consent for Publication
Not applicable
Additional information
This manuscript is was prepared in accordance with the CARE guidelines.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Surgery
Rights and permissions
About this article
Cite this article
Tomoshige, K., Tsuchiya, T., Matsumoto, K. et al. Primary Mucinous Adenocarcinoma of the Thymus: a Rare Type of Thymic Carcinoma—Case Report. SN Compr. Clin. Med. 3, 1233–1237 (2021). https://doi.org/10.1007/s42399-021-00839-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42399-021-00839-x