Abstract
Purpose
The purpose of this study was to perform a systematic review to assess the utility of accelerometric methods to identify older adults at risk of falls.
Methods
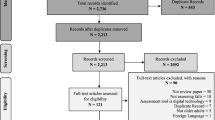
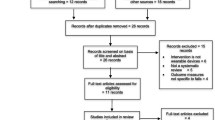
The Preferred Reporting Item for Systematic review and Meta-Analysis (PRISMA) guidelines were followed during all steps of this systematic review. Cross sectional and longitudinal studies assessing gait parameters in older adults using accelerometric devices, and comparing groups based on the risk of falls or fall history were identified from studies published in the MEDLINE, SCOPUS and Cochrane Database of Systematic Reviews databases between January 1996 and January 2017. Study selection and data extraction were performed independently by two reviewers. The quality of the methodology used in the studies included was assessed using the Newcastle–Ottawa Scale.
Results
In total, 354 references were identified through the database search. After selection, ten studies were included in this systematic review. According to the cross sectional studies, people who fall or are at risk of fall are slower, and walk with shorter steps, lower step frequency, worse stride and step regularity in terms of time, position and acceleration profiles. One longitudinal study suggests considering harmonic ratio of upper trunk acceleration in the vertical plane. Two other longitudinal studies highlight the importance of considering more than one gait parameter, and sophisticated statistical tools to discern older adults at risk for future fall(s).
Conclusion
This systematic review essentially highlights the lack of available literature providing strong evidence that gait parameters obtained using acceleration-based methods could be useful to discern older people at risk of fall. Available literature is encouraging, but further high quality studies are needed to highlight the cross-sectional and longitudinal relationships between gait parameters and falls in older adults.

Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- IMF:
-
Intrinsic mode function
- HR:
-
Harmonic ratios
- MLHR:
-
Medio-lateral harmonic ratios
- 8-step MLHR:
-
Medio-lateral harmonic ratios based on the 8-step method
- NOS:
-
Newcastle–Ottawa Scale
- PCA:
-
Principal component analysis
- RMS:
-
Root mean square
- SD:
-
Standard deviation
- SSI:
-
Step Stability Index
References
Rubenstein LZ (2006) Falls in older people: Epidemiology, risk factors and strategies for prevention. Age Ageing 35:ii37–ii41
Thiem U, Klaaßen-Mielke R, Trampisch U, Moschny A, Pientka L, Hinrichs T (2014) Falls and EQ-5D rated quality of life in community-dwelling seniors with concurrent chronic diseases: a cross-sectional study. Health Qual Life Outcomes 12:2
Scheffer AC, Schuurmans MJ, van Dijk N, van der Hooft T, de Rooij SE (2008) Fear of falling: measurement strategy, prevalence, risk factors and consequences among older persons. Age Ageing 37(1):19–24
Delbaere K, Crombez G, Vanderstraeten G, Willems T, Cambier D (2004) Fear-related avoidance of activities, falls and physical frailty. A prospective community-based cohort study. Age Ageing 33(4):368–373
Choi K, Ko Y (2015) Characteristics associated with fear of falling and activity restriction in South Korean Older adults. J Aging Health 27(6):1066–1083
Ambrose AF, Paul G, Hausdorff JM (2013) Risk factors for falls among older adults: a review of the literature. Maturitas 75(1):51–61
Menant JC, Schoene D, Sarofim M, Lord SR (2014) Single and dual task tests of gait speed are equivalent in the prediction of falls in older people: a systematic review and meta-analysis. Ageing Res Rev 16:83–104
MacAulay RK, Allaire TD, Brouillette RM, Foil HC, Bruce-Keller AJ, Han H et al (2015) Longitudinal assessment of neuropsychological and temporal/spatial gait characteristics of elderly fallers: taking it all in stride. Front Aging Neurosci 7:34
Hausdorff JM, Rios DA, Edelberg HK (1050) Gait variability and fall risk in community-living older adults: A 1-year prospective study. Arch Phys Med Rehabil 2001(82):1056
Allali G, Launay CP, Blumen HM, Callisaya ML, De Cock A-M, Kressig RW et al (2017) Falls, Cognitive Impairment, and Gait Performance: results From the GOOD Initiative. J Am Med Dir Assoc 18(4):335–340
Moe-Nilssen R, Helbostad JL (2004) Estimation of gait cycle characteristics by trunk accelerometry. J Biomech 37(1):121–126
Auvinet B, Berrut G, Touzard C, Moutel L, Collet N, Chaleil D et al (2002) Reference data for normal subjects obtained with an accelerometric device. Gait Posture 16(2):124–134
Hartmann A, Luzi S, Murer K, de Bie RA, de Bruin ED (2009) Concurrent validity of a trunk tri-axial accelerometer system for gait analysis in older adults. Gait Posture 29(3):444–448
Hartmann A, Murer K, de Bie RA, de Bruin ED (2009) Reproducibility of spatio-temporal gait parameters under different conditions in older adults using a trunk tri-axial accelerometer system. Gait Posture 30(3):351–355
Kavanagh JJ, Menz HB (2008) Accelerometry: a technique for quantifying movement patterns during walking. Gait Posture 28(1):1–15
Moe-Nilssen R, Helbostad JL (2005) Interstride trunk acceleration variability but not step width variability can differentiate between fit and frail older adults. Gait Posture 21(2):164–170
Moe-Nilssen R (1998) A new method for evaluating motor control in gait under real-life environmental conditions. Part 1: the instrument. Clin Biomech 13(4):320–327
Moher D, Liberati A, Tetzlaff J, Altman DG (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8(5):336–341
(2018) The modified Newcastle Ottawa scale for cross sectional studies. http://journals.plos.org/plosone/article/file?type=supplementary&id=info:doi/10.1371/journal.pone.0136065.s004
Newcastle (2017) Ottawa quality assessment scale cohort studies [cited 2017 07-10]. http://www.ohri.ca/programs/clinical_epidemiology/nosgen.pdf
Cho CY, Kamen G (1998) Detecting balance deficits in frequent fallers using clinical and quantitative evaluation tools. J Am Geriatr Soc 46(4):426–430
Auvinet B, Berrut G, Touzard C, Moutel L, Collet N, Chaleil D et al (2003) Gait abnormalities in elderly fallers. J Aging Phys Act 11(1):40–52
Menz HB, Lord SR, Fitzpatrick RC (2003) Acceleration patterns of the head and pelvis when walking are associated with risk of falling in community-dwelling older people. J Gerontol Ser A Biol Sci Med Sci 58(5):M446–M452
Bautmans I, Jansen B, Van Keymolen B, Mets T (2011) Reliability and clinical correlates of 3D-accelerometry based gait analysis outcomes according to age and fall-risk. Gait Posture 33(3):366–372
Senden R, Savelberg HH, Grimm B, Heyligers IC, Meijer K (2012) Accelerometry-based gait analysis, an additional objective approach to screen subjects at risk for falling. Gait Posture 36(2):296–300
Cui X, Peng CK, Costa MD, Weiss A, Goldberger AL, Hausdorff JM (2014) Development of a new approach to quantifying stepping stability using ensemble empirical mode decomposition. Gait Posture 39(1):495–500
Brodie MAD, Menz HB, Smith ST, Delbaere K, Lord SR (2015) Good lateral harmonic stability combined with adequate gait speed is required for low fall risk in older people. Gerontology 61(1):69–78
Marschollek M, Rehwald A, Wolf KH, Gietzelt M, Nemitz G, Zu Schwabedissen HM et al (2011) Sensor-based Fall risk assessment – an expert ‘to go’. Methods Inf Med 50(5):420–426
Doi T, Hirata S, Ono R, Tsutsumimoto K, Misu S, Ando H (2013) The harmonic ratio of trunk acceleration predicts falling among older people: results of a 1-year prospective study. J Neuroeng Rehabil 10:7
Mignardot JB, Deschamps T, Barrey E, Auvinet B, Berrut G, Cornu C et al (2014) Gait disturbances as specific predictive markers of the first fall onset in elderly people: a two-year prospective observational study. Front Aging Neurosci 6:22
Senden R, Grimm B, Heyligers IC, Savelberg HHCM, Meijer K (2009) Acceleration-based gait test for healthy subjects: reliability and reference data. Gait Posture 30(2):192–196
Menz HB, Lord SR, Fitzpatrick RC (2003) Acceleration patterns of the head and pelvis when walking on level and irregular surfaces. Gait Posture 18(1):35–46
Thaler-Kall K, Peters A, Thorand B, Grill E, Autenrieth CS, Horsch A et al (2015) Description of spatio-temporal gait parameters in elderly people and their association with history of falls: results of the population-based cross-sectional KORA-Age study. BMC Geriatr 15:32
Mortaza NAON (2014) Mehdikhani N Are gait parameters capable of distinguishing a faller than a non-faller elderly? Eur J Phys Rehabil Med 50(6):677–691
Herman T, Mirelman A, Giladi N, Schweiger A, Hausdorff JM (2010) Executive control deficits as a prodrome to falls in healthy older adults: a prospective study linking thinking, walking, and falling. J Gerontol Ser A Biol Sci Med Sci 65A(10):1086–1092
Foucher KC, Thorp LE, Orozco D, Hildebrand M, Wimmer MA (2010) Differences in preferred walking speeds in a gait laboratory compared with the real world after total hip replacement. Arch Phys Med Rehabil 91(9):1390–1395
Sedgwick P, Greenwood N (2015) Understanding the Hawthorne effect. BMJ 351:h4672. https://doi.org/10.1136/bmj.h4672
Rispens SM, Van Dieën JH, Van Schooten KS, Cofré Lizama LE, Daffertshofer A, Beek PJ et al (2016) Fall-related gait characteristics on the treadmill and in daily life. J Neuroeng Rehabil 13:12
Acknowledgements
S.G. is supported by a fellowship from the FNRS (Fonds National de la Recherche Scientifique de Belgique—FRS-FNRS—www.frsfnrs.be). The authors would like to thank Mrs. Françoise Pasleau for advice on search strategies.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declared that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Gillain, S., Boutaayamou, M., Beaudart, C. et al. Assessing gait parameters with accelerometer-based methods to identify older adults at risk of falls: a systematic review. Eur Geriatr Med 9, 435–448 (2018). https://doi.org/10.1007/s41999-018-0061-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41999-018-0061-3