Abstract
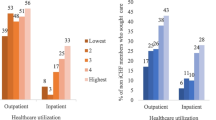
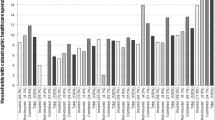
In India, out-of-pocket (OOP) payments as a share of total health expenditures remain disproportionally high across population groups. When combined with poverty, poor access to healthcare and inadequate health insurance coverage, OOP expenses can have catastrophic consequences for rural households. In this context, the present study explored the levels of catastrophic health expenditures (CHE) and their determinants among rural households of a hilly state in India. Primary data were collected from 300 households in Himachal Pradesh. The focus of the study was to provide information on the distribution of CHE. In addition, various characteristics associated with the incidence of CHE were further studied using multiple logistic regression models. The results showed that households across Himachal Pradesh spend a significant proportion of their budget on healthcare. Among the characteristics associated with the likelihood of facing CHE, seeking outpatient care, having a chronic illness and location of the hospital showed significant associations. In conclusion, the financial risks emanating from OOP payments can be significantly reduced by covering outpatient care needs under social health insurance. Furthermore, strengthening rural health infrastructure to screen and treat chronic diseases locally, and minimizing the need to travel to distant places for treatment can also significantly reduce OOP payments.
Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, [Ajay kumar], upon reasonable request.
Abbreviations
- AB-PMJAY:
-
Ayushman Bharat-Pradhan Mantri Jan Arogya Yojna
- CHE:
-
Catastrophic health expenditure
- HC:
-
Head count
- HIMCARE:
-
Mukhya Mantri Himachal Health Care Scheme
- INR:
-
Indian national rupee
- M.E.:
-
Marginal effect
- NSSO:
-
National Sample Survey Office
- OOP:
-
Out-of-pocket
- SE:
-
Standard error
References
Ahmed S, Ahmed MW, Hasan MZ, Mehdi GG, Islam Z, Rehnberg C, Niessen LW, Khan JAM (2022) Assessing the incidence of catastrophic health expenditure and impoverishment from out-of-pocket payments and their determinants in Bangladesh: evidence from the nationwide Household Income and Expenditure Survey 2016. Int Health 14:84–96
Ahmed S, Szabo S, Nilsen K (2018) Catastrophic healthcare expenditure and impoverishment in tropical deltas: evidence from the Mekong Delta region. Int J Equity Health 17:1–13
Akhtar A, Ahmad N, Roy Chowdhury I (2020) Socio-economic inequality in catastrophic health expenditure among households in India: a decomposition analysis. Springer India, New Delhi
Behera DK, Dash U (2020) Is health expenditure effective for achieving healthcare goals? Empirical evidence from South-East Asia Region. Asia-Pac J Reg Sci 4:593–618
Behera DK, Dash U, Sahu SK (2022) Exploring the possible sources of fiscal space for health in India: insights from political regimes. Heal Res Policy Syst 20:32
Berki SE (1986) A look at catastrophic medical expenses and the poor. Health Aff 5:138–145
Berman P, Ahuja R, Bhandari L (2010) The impoverishing effect of healthcare payments in India: new methodology and findings. Econ Polit Wkly 45:65–71
Buigut S, Ettarh R, Amendah DD (2015) Catastrophic health expenditure and its determinants in Kenya slum communities. Int J Equity Health 14:1–12
Chatterjee U, Smith O (2021) Going granular: equity of health financing at the district and facility level in India. Heal Syst Reform 7:1–12
Choi JW, Kim TH, Jang SI, Jang SY, Kim WR, Park EC (2016) Catastrophic health expenditure according to employment status in South Korea: a population-based panel study. BMJ Open 6:1–7
Chokshi M, Patil B, Khanna R, Neogi SB, Sharma J, Paul VK, Zodpey S (2016) Health systems in India. J Perinatol 36:S9–S12
Chuma J, Maina T (2012) Catastrophic health care spending and impoverishment in Kenya. BMC Health Serv Res 12:413
Dalui A, Banerjee S, Roy R (2020) Determinants of out-of-pocket and catastrophic health expenditure in rural population: a community-based study in a block of Purba Barddhaman, West Bengal. Indian J Public Health 64:223
Das MB, Kappor-Mehta S, Tas EO, Zumbyte I (2015) Scaling the heights: social inclusion and sustainable development in Himachal Pradesh. World Bank, Washington, DC. http://hdl.handle.net/10986/21316
Economic and Statistics Department (2022) Economic Survey 2021–2022. Government of Himachal Pradesh. https://himachalservices.nic.in/economics/pdf/economic_survey_2021-22.pdf
Erlangga D, Suhrcke M, Ali S, Bloor K (2019) Correction: The impact of public health insurance on health care utilisation, financial protection and health status in low: The middle-income countries: a systematic review (PLoS ONE (2019) 14:8 (e0219731) DOI: 10.1371/journal.pone.0219731). PLoS ONE 14:1–20
Flores G, O’Donnell O (2016) Catastrophic medical expenditure risk. J Health Econ 46:1–15
Garg CC, Karan AK (2009) Reducing out-of-pocket expenditures to reduce poverty: a disaggregated analysis at rural-urban and state level in India. Health Policy Plan 24:116–128
Ghosh S (2011) Catastrophic payments and impoverishment due to out-of-pocket health spending. Econ Polit Wkly 46:63–70
Gupt A, Kaur P, Kamraj P, Murthy BN (2016) Out of pocket expenditure for hospitalization among below poverty line households in district Solan, Himachal Pradesh, India, 2013. PLoS ONE 11:1–11
Jia Y, Hu M, Fu H, Yip W (2022) Provincial variations in catastrophic health expenditure and medical impoverishment in China: a nationwide population-based study. Lancet Reg Heal West Pac 31:100633
Karan A, Yip W, Mahal A (2017) Extending health insurance to the poor in India: an impact evaluation of Rashtriya Swasthya Bima Yojana on out of pocket spending for healthcare. Soc Sci Med 181:83–92
Kumar S, Anil Kumar K (2021) Out-of-pocket expenditure and catastrophic health spending on maternity care for hospital based delivery care in empowered action group (EAG) States of India. Glob Soc Welf 8:231–241
Kumar S, Sarjolta D (2019) An evaluation of healthcare expenditure in Himachal Pradesh. Manpow J LIII:1–16
Li X, Shen JJ, Lu J, Wang Y, Sun M, Li C, Chang F, Hao M (2013) Household catastrophic medical expenses in eastern China: determinants and policy implications. BMC Health Serv Res 13:506
Li Y, Wu Q, Xu L, Legge D, Hao Y, Gao L, Wan G (2012) Factors affecting catastrophic health expenditure and impoverishment from medical expenses in China: policy implications of universal health insurance. Bull World Heal Organ 90:664–671
Luo Y, Shi Z, Guo D, He P (2023) Toward universal health coverage: regional inequalities and potential solutions for alleviating catastrophic health expenditure in the post-poverty elimination era of China. Int J Heal Policy Manag 12:7332
Misra S, Awasthi S, Singh JV, Agarwal M, Kumar V (2015) Assessing the magnitude, distribution and determinants of catastrophic health expenditure in urban Lucknow, North India. Clin Epidemiol Glob Heal 3:10–16
Mohanty SK, Kim R, Khan PK, Subramanian SV (2018) Geographic variation in household and catastrophic health spending in India: assessing the relative importance of villages, districts, and states, 2011–2012. Milbank Q 96:167–206
MOHFW (2021) National health accounts estimates for India 2017–18, pp 1–88
MOHFW (2022) National health accounts estimates for India 2018–2019, pp 1–102
Mondal S, Kanjilal B, Peters DH, Lucas H (2010) Catastrophic out-of-pocket payment for health care and its impact on households: experience from West Bengal, India. In: Future health systems, innovations for equity, p 1–20. https://www.academia.edu/download/39670202/Catastrophic_out-of-pocket_payment_for_h20151104-24817-gql6e7.pdf
Mondal S, Lucas H, Peters D, Kanjilal B (2014) Catastrophic out-of-pocket payment for healthcare and implications for household coping strategies: evidence from West Bengal, India. Econ Bull 34:1303–1316
MOSPI (2019) Key indicators of social consumption in India: health, p 127
Nagulapalli S (2014) Burden of out-of-pocket health payments in Andhra Pradesh. Econ Polit Wkly 49:64–72
National Sample Survey Organisation (2001) Concepts and definitions used in NSS, pp 1–144
Njagi P, Arsenijevic J, Groot W (2018) Understanding variations in catastrophic health expenditure, its underlying determinants and impoverishment in Sub-Saharan African countries: a scoping review. Syst Rev 7:136
NSS (2015) Key indicators of social consumption in India: health, pp 1–99
Pal R (2012) Measuring incidence of catastrophic out-of-pocket health expenditure: with application to India. Int J Health Care Financ Econ 12:63–85
Pandey A, Kumar GA, Dandona R, Dandona L (2018a) Variations in catastrophic health expenditure across the states of India: 2004 to 2014. PLoS ONE 13:e0205510
Pandey A, Ploubidis GB, Dandona L (2018b) Trends in catastrophic health expenditure in India: 1993 to 2014. Bull World Health Organ 96:18–28
Pradhan J, Behera S (2020) Does choice of health care facility matter? Assessing out-of-pocket expenditure and catastrophic spending on emergency obstetric care in India. J Biosoc Sci 53:481
Prinja S, Chauhan AS, Karan A, Kaur G, Kumar R (2017) Impact of publicly financed health insurance schemes on healthcare utilization and financial risk protection in India: a systematic review. PLoS ONE 12:e0170996
Quintussi M, Van de Poel E, Panda P, Rutten F (2015) Economic consequences of ill-health for households in northern rural India. BMC Health Serv Res 15:179
Raban MZ, Dandona R, Dandona L (2013) Variations in catastrophic health expenditure estimates from household surveys in India. Bull World Health Organ 91:726–735
RBI (2020) Handbook of statistics on Indian economy 2019–20
Sangar S, Dutt V, Thakur R (2018) Economic burden, impoverishment and coping mechanisms associated with out-of-pocket health expenditure: analysis of rural-urban differentials in India. J Public Health 26:485–494
Sangar S, Dutt V, Thakur R (2019a) Economic burden, impoverishment, and coping mechanisms associated with out-of-pocket health expenditure in India: a disaggregated analysis at the state level. Int J Health Plann Manage 34:4–7
Sangar S, Dutt V, Thakur R (2019b) Burden of out-of-pocket health expenditure and its impoverishment impact in India: evidence from National Sample Survey. J Asian Public Policy 15:60–77
Sangar S, Dutt V, Thakur R (2019c) Rural–urban differentials in out-of-pocket health expenditure and resultant impoverishment in India: evidence from NSSO 71st Round. Asia-Pac J Reg Sci 3:273–291
Shi W, Chongsuvivatwong V, Geater A, Zhang J, Zhang H, Brombal D (2011) Effect of household and village characteristics on financial catastrophe and impoverishment due to health care spending in Western and Central Rural China: A multilevel analysis. Heal Res Policy Syst 9:16
Su TT, Kouyaté B, Flessa S (2006) Catastrophic household expenditure for health care in a low-income society: a study from Nouna District, Burkina Faso. Bull World Health Organ 84:21–27
Thu Thuong NT, Van Den Berg Y, Huy TQ, Tai DA, Anh BNH (2021) Determinants of catastrophic health expenditure in Vietnam. Int J Health Plann Manage 36:316–333
UIDAI (2020) Total population (projected 2020), pp 1–3
Van Minh H, Kim Phuong NT, Saksena P, James CD, Xu K (2013) Financial burden of household out-of pocket health expenditure in Viet Nam: findings from the National Living Standard Survey 2002–2010. Soc Sci Med 96:258–263
Wagstaff A, van Doorslaer E (2003) Catastrophe and impoverishment in paying for health care: with applications to Vietnam 1993–1998. Health Econ 12:921–933
WHO, WB (2019) Global monitoring report on financial protection in Health 2019: advance copy, pp 1–60
WHO, WB (2021) Global monitoring report on financial protection in Health 2021
Xu K, Evans DB, Kawabata K, Zeramdini R, Klavus J, Murray CJL (2003) Household catastrophic health expenditure: a multicountry analysis. Lancet 362:111–117
Xu X, Wang Q, Li C (2022) The impact of dependency burden on urban household health expenditure and its regional heterogeneity in china: based on quantile regression method. Front Public Heal 10:1–13
Xu Y, Gao J, Zhou Z, Xue Q, Yang J, Luo H, Li Y, Lai S, Chen G (2015) Measurement and explanation of socioeconomic inequality in catastrophic health care expenditure: evidence from the rural areas of Shaanxi Province. BMC Health Serv Res 15:1–10
Yadav J, Allarakha S, Menon GR, John D, Nair S (2021) Socioeconomic impact of hospitalization expenditure for treatment of noncommunicable diseases in India: a repeated cross-sectional analysis of national sample survey data, 2004 to 2018. Value Heal Reg Issues 24:199–213
Zhen X, Zhang H, Hu X, Gu S, Li Y, Gu Y, Huang M (2018) A comparative study of catastrophic health expenditure in Zhejiang and Qinghai province, China. BMC Health Serv Res 9:1–8
Funding
No funding was received for conducting this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare that are related to the content of this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kumar, A., Sharma, H.R. & Gupta, S. Extent and determinants of catastrophic health expenditure in rural areas of Himachal Pradesh, India. Asia-Pac J Reg Sci 7, 1289–1305 (2023). https://doi.org/10.1007/s41685-023-00307-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41685-023-00307-5