Abstract
Objective
Because there is no current information on medical student suicides, the authors surveyed US medical schools about deaths by suicide of medical students from June 2006 to July 2011.
Methods
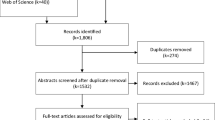
In spring through summer of 2012, the authors sent electronic surveys to the 133 accredited US allopathic medical schools at the time, excluding Puerto Rican schools. The 15-item survey included questions about deaths by suicide and deaths by means other than suicide. In the case of a reported suicide, the survey obtained information regarding demographic characteristics and method of suicide.
Results
The 90 responding schools (response rate 69 %) reported a total of six suicides (four males, two females; five Caucasians, one Asian) from July 2006 to June 2011. Two deaths by suicide occurred in first year, two in second year, and two in third year. Two of the suicides occurred by gunshot, two by hanging, one by overdose, and for one, the cause of death was unknown. Three of the six students left a suicide note.
Conclusion
Although the number and rate of suicides among medical students may be lower than a prior survey that was conducted more than 15 years ago, these data affirm the importance of suicide prevention programs for medical students.
Similar content being viewed by others
References
Murphy SL, Xu J, Kochanek KD: Deaths: preliminary data for 2010. National Vital Statistics Reports 2012; 60
Centers for Disease Control and Prevention, National Center for Health Statistics: Underlying cause of death 1999–2010 on CDC WONDER online database, 2012; available at http://wonder.cdc.gov/ucd-icd10.html. accessed January 9, 2013
Compton MT, Carrera J, Frank E. Stress and depressive symptoms/dysphoria among US medical students: results from a large, nationally representative survey. J Nerv Ment Dis. 2008;196:891–7.
Dyrbye LN, Harper W, Durning SJ, et al. Patterns of distress in US medical students. Med Teach. 2011;33:834–9.
Dyrbye LN, Thomas MR, Massie FS, et al. Burnout and suicidal ideation among U.S. medical students. Ann Intern Med. 2008;149:334–41.
Goebert D, Thompson D, Takeshita J, et al. Depressive symptoms in medical students and residents: a multischool study. Acad Med. 2009;84:236.
Schwenk TL, Davis L, Wimsatt LA. Depression, stigma, and suicidal ideation in medical students. JAMA. 2010;304:1181–90.
Alexandrino-Silva C, Pereira ML, Bustamante C, et al. Suicidal ideation among students enrolled in healthcare training programs: a cross-sectional study. Rev Bras Psiquiatr. 2009;31:338–44.
Curran TA, Gawley E, Casey P, Gill M, Crumlish N. Depression, suicidality and alcohol abuse among medical and business students. Ir Med J. 2009;102:249–52.
Eskin M, Voracek M, Stieger S, Altinyazar V. A cross-cultural investigation of suicidal behavior and attitudes in Austrian and Turkish medical students. Soc Psychiatry Psychiatr Epidemiol. 2011;46:813–23.
Tyssen R, Vaglum P, Gronvold NT, Ekeberg O. Suicidal ideation among medical students and young physicians: a nationwide and prospective study of prevalence and predictors. J Affect Disord. 2001;64:69–79.
Dyrbye LN, Thomas MR, Shanafelt TD. Systematic review of depression, anxiety, and other indicators of psychological distress among US and Canadian medical students. Acad Med. 2006;81:354–73.
Baca-Garcia E, Perez-Rodriguez MM, Oquendo MA, et al. Estimating risk for suicide attempt: are we asking the right questions? Passive suicidal ideation as a marker for suicidal behavior. J Affect Disord. 2011;134:327–32.
Beck AT, Brown GK, Steer RA, Dahlsgaard KK, Grisham JR. Suicide ideation at its worst point: a predictor of eventual suicide in psychiatric outpatients. Suicide and Life-Threatening Behav. 1999;29:1–9.
Blair-West GW, Cantor CH, Mellsop GW, Eyeson-Annan ML. Lifetime suicide risk in major depression: sex and age determinants. J Affect Disord. 1999;55:171–8.
Bulik CM, Carpenter LL, Kupfer DJ, Frank E. Features associated with suicide attempts in recurrent major depression. J Affect Disord. 1990;18:29–37.
Gould MS, King R, Greenwald S, et al. Psychopathology associated with suicidal ideation and attempts among children and adolescents. J Am Acad Child Adolesc Psychiatry. 1998;37:915–23.
Malone KM, Haas GL, Sweeney JA, Mann JJ. Major depression and the risk of attempted suicide. J Affect Disord. 1995;34:173–85.
Simon HJ. Mortality among medical students, 1947–1967. J Med Educ. 1968;43:1175–82.
Everson RB, Fraumeni Jr JF. Mortality among medical students and young physicians. J Med Educ. 1975;50:809–11.
Pepitone-Arreola-Rockwell F, Rockwell D, Core N. Fifty-two medical student suicides. Am J Psychiatry. 1981;138:198–201.
Hays LR, Cheever T, Patel P. Medical student suicide, 1989–1994. Am J Psychiatry. 1996;153:553–5.
Austenfeld JL, Paolo AM, Stanton AL. Effects of writing about emotions versus goals on psychological and physical health among third-year medical students. J Pers. 2006;74:267–86.
Bloodgood RA, Short JG, Jackson JM, Martindale JR. A change to pass/fail grading in the first two years at one medical school results in improved psychological well-being. Acad Med. 2009;84:655–62.
Dare AJ, Petrie KJ, Bagg W. Prepared for practice? Medical students’ perceptions of a shortened final year medical programme. N Z Med J. 2009;122:32–43.
Finkelstein C, Brownstein A, Scott C, Lan YL. Anxiety and stress reduction in medical education: an intervention. Med Educ. 2007;41:258–64.
Guthrie E, Black D, Shaw C, Hamilton J, Creed F, Tomenson B. Psychological stress in medical students: a comparison of two very different university courses. Stress Med. 1998;13:179–84.
Kiessling C, Schubert B, Scheffner D, Burger W. First year medical students’ perceptions of stress and support: a comparison between reformed and traditional track curricula. Med Educ. 2004;38:504–9.
Reed DA, Shanafelt TD, Satele DW, et al. Relationship of pass/fail grading and curriculum structure with well-being among preclinical medical students: a multi-institutional study. Acad Med. 2011;86:1367–73.
Rohe DE, Barrier PA, Clark MM, Cook DA, Vickers KS, Decker PA. The benefits of pass-fail grading on stress, mood, and group cohesion in medical students. Mayo Clin Proc. 2006;81:1443–8.
Rosenzweig S, Reibel DK, Greeson JM, Brainard GC, Hojat M. Mindfulness-based stress reduction lowers psychological distress in medical students. Teach Learn Med. 2003;15:88–92.
Shapiro SL, Schwartz GE, Bonner G. Effects of mindfulness-based stress reduction on medical and premedical students. J Behav Med. 1998;21:581–99.
Warnecke E, Quinn S, Ogden K, Towle N, Nelson MR. A randomised controlled trial of the effects of mindfulness practice on medical student stress levels. Med Educ. 2011;45:381–8.
Whitehouse WG, Dinges DF, Orne EC, et al. Psychosocial and immune effects of self-hypnosis training for stress management throughout the first semester of medical school. Psychosom Med. 1996;58:249–63.
Shiralkar M, Harris TB, Eddins-Folensbee FF, Coverdale JH: A systematic review of stress-management programs for medical students. Acad Psychiatry. [In Press].
Centers for Disease Control and Prevention: Suicide and self-inflicted injury, 2012; available at http://www.cdc.gov/nchs/fastats/suicide.htm. accessed January 17, 2013.
Association of American Medical Colleges. AAMC FACTS: total enrollment by U.S. medical school and sex, 2012; available at https://www.aamc.org/data/facts/enrollmentgraduate/158808/total-enrollment-by-medical-school-by-sex.html. accessed January 7, 2013.
Acknowledgments
The authors wish to thank Nancy Searle, Ed.D., who assisted in the early stages of this project.
Disclosure
On behalf of all the authors, the corresponding author states that there are no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheng, J., Kumar, S., Nelson, E. et al. A National Survey of Medical Student Suicides. Acad Psychiatry 38, 542–546 (2014). https://doi.org/10.1007/s40596-014-0075-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40596-014-0075-1