Abstract
Background
Exercise is commonly recommended to prevent and manage osteoporosis. High magnitude strains at rapid rate and short bouts should theoretically elicit an osteogenic response; however, the effects of different levels of impact exercises on several outcomes in people at risk of fracture are still unknown.
Objective
To report the effect of impact exercise on falls, fractures, adverse events, mortality, bone mineral density (BMD), physical functioning, and health-related quality of life (QoL).
Methods
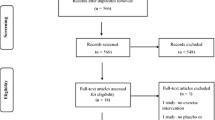
We included randomized controlled trials testing the effect of impact exercise compared with a non-exercise control on outcomes in adults ≥ 50 years with low BMD or fragility fractures. Two reviewers selected studies and extracted data. Where possible, we pooled outcomes using mean difference (MD) with a fixed-effects model and 95% confidence interval (CI). We reported risk of bias using Cochrane and certainty of evidence using GRADE.
Results
We included 29 trials; 19 studies evaluated impact exercise alone, and the remaining trials combined impact with resistance or balance training. Impact exercise alone or combined with resistance training improved Timed Up-and-Go values (MD − 0.95 s, 95% CI − 1.09 to − 0.81, low certainty evidence) and lumbar spine (MD 0.04 g/cm2, 95% CI 0.02–0.06, low certainty evidence) and femoral neck BMD (MD 0.04 g/cm2, 95% CI 0.02–0.07, low certainty evidence). Impact exercise did not improve health-related QoL assessed with QUALEFFO-41 (MD 0.06, 95% CI − 2.18 to 2.30, moderate certainty evidence). The effects of impact exercise on falls, fractures, and mortality are uncertain due to insufficient data. Many trials had a high risk of bias for two or more items.
Conclusions
There is low certainty evidence that impact exercise may improve physical function and BMD in people at risk of fracture. The effect of impact exercises on falls, fractures, and mortality remains unclear. Our findings should be interpreted with caution due to risk of bias and small sample sizes.
Trial Registration
Registered in Prospero (CRD42018115579) on January 30, 2019.



Similar content being viewed by others
References
Giangregorio LM, Papaioannou A, Macintyre NJ, et al. Too fit to fracture: exercise recommendations for individuals with osteoporosis or osteoporotic vertebral fracture. Osteoporos Int. 2014;25:821–35. https://doi.org/10.1007/s00198-013-2523-2.
Sievänen H, Kannus P. Physical activity reduces the risk of fragility fracture. PLoS Med. 2007;4(6):e222. https://doi.org/10.1371/journal.pmed.0040199.
Martyn-St James M, Carroll S. Effects of different impact exercise modalities on bone mineral density in premenopausal women: a meta-analysis. J Bone Min Metab. 2010;28(3):251–67. https://doi.org/10.1007/s00774-009-0139-6.
Welsh L, Rutherford OM. Hip bone mineral density is improved by high-impact aerobic exercise in postmenopausal women and men over 50 years. Eur J Appl Physiol Occup Physiol. 1996;74(6):511–7.
Turner C, Robling A. Exercises for improving bone strength. BR J Sport Med. 2005;39(4):188–9.
Turner C, Robling A. Designing exercise regimens to increase bone strength. Exerc Sport Sci Rev. 2003;31(1):45–50.
Kohrt W, Barry D, Schwartz RS. Muscle forces or gravity: what predominates mechanical loading on bone? Med Sci Sport Exerc. 2011;41(11):2050–5.
Kelley G, Kelley K, Kohrt W. Exercise and bone mineral density in men: a meta-analysis of randomized controlled trials. Bone. 2013;53(1):103–11. https://doi.org/10.1016/j.bone.2012.11.031.
Nikander R, Gagnon C, Dunstan D. Frequent walking, but not total physical activity, is associated with increased fracture incidence: a 5-year follow-up of an Australian population-based prospective study (AusDiab). J Bone Miner Res. 2011;25(7):1638–47.
Morin S, Djekic-Ivankovic M, Funnell L, et al. Patient engagement in clinical guidelines development: input from > 1000 members of the Canadian Osteoporosis Patient Network. Osteoporos Int. 2020;31(5):867–74. https://doi.org/10.1007/s00198-019-05248-4.
Rodrigues IB, Ashe M, Bartley J. How exercise professionals support people with acute vertebral fractures? [abstract]. In: Proceedings of the 2019 American society of bone mineral research. 2019.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLOS Med. 2009;8(5):336–41.
Higgins J, Altman D, Gotzsche P, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928.
Rodrigues I, Ponzano M, Butt D, et al. The effects of walking or Nordic walking in adults 50 years and older at risk of fractures: a systematic review and meta-analysis. JAPA. 2020 (in press).
Ponzano M, Rodrigues I, Hosseini Z, et al. Progressive resistance training for improving health-related outcomes in people at risk of fracture: a systematic review and meta-analysis. Phys Ther. 2020 (in press).
Weeks B, Beck B. The BPAQ: a bone-specific physical activity assessment instrument. Osteoporos In. 2008;19(11):1567–77. https://doi.org/10.1007/s00198-008-0606-2.
Marotti G. Map of bone formation rate values recorded throughout the skeleton of the dog. Bone Morphometry, University of Ottawa Press, Ottawa, Ontario. 1975. p. 202–07.
Kimmel B. A quantitative histologic study of bone turnover in young adult beagles. Anat Rec. 1982;45:31–45.
O’Neil J, Tabish H, Welch V, et al. Applying an equity lens to interventions: using PROGRESS ensures consideration of socially stratifying factors to illuminate inequities in health. J Clin Epidemiol. 2014;67(1):56–64. https://doi.org/10.1016/j.jclinepi.2013.08.005.
Lips P, Cooper C, Agnusdei D, et al. Quality of life in patients with vertebral fractures: validation of the Quality of Life Questionnaire of the European Foundation for Osteoporosis (QUALEFFO). Working Party for Quality of Life of the European Foundation for Osteoporosis. Osteoporos Int. 1999;10(2):150–60.
Atkins D, Best D, Briss P, et al. Grading quality of evidence and strength of recommendations. BMJ. 2004;328(7454):1490. https://doi.org/10.1136/bmj.328.7454.1490.
Alayat M, Abdel-Kafy E, Thabet A, et al. Long-term effect of pulsed Nd-YAG laser combined with exercise on bone mineral density in men with osteopenia or osteoporosis: 1 year of follow-up. Photomed Laser Surg. 2018;36(2):105–11.
Basat H, Esmaeilzadeh S, Eskiyurt N. The effects of strengthening and high-impact exercises on bone metabolism and quality of life in postmenopausal women: a randomized controlled trial. J Back Musculoskelet Rehabil. 2013;26(4):427–35.
Bergland A, Thorsen H, Karesen R. Effect of exercise on mobility, balance, and health-related quality of life in osteoporotic women with a history of vertebral fracture: a randomized, controlled trial. Osteoporos Int. 2011;22(6):1863–71.
Bolton K, Egerton T, Wark J. Effects of exercise on bone density and falls risk factors in post-menopausal women with osteopenia: a randomised controlled trial. J Sci Med Sport. 2012;15(2):102–9. https://doi.org/10.1016/j.jsams.2011.08.007.
Borba-Pinheiro C, Dantas E, Drigo A, et al. Adapted combat sports on bone related variables and functional independence of postmenopausal women in pharmacological treatment: a clinical trial study. Arch Budo. 2016;12(1):187–99.
Bravo G, Gauthier P, Roy PM, et al. Impact of a 12-month exercise program on the physical and psychological health of osteopenic women. J Am Geriatr Soc. 1996;44(7):756–62. https://doi.org/10.1111/j.1532-5415.1996.tb03730.x.
Chao M, Hazelton M, Cholowski K. The effect of an exercise program on physical fitness and quality of life in adults with osteopenia in Taiwan: a randomized controlled trial. Thai J Nurs Res. 2005;9(3):170–92.
Cheng J, Haibing H, Chen Y. Effect of aerobic exercise and raloxifene combination therapy on senile osteoporosis. J Phys Ther Sci. 2016;28(6):1791–4.
Chien M, Wu Y, Hsu A, et al. Efficacy of a 24-week aerobic exercise program for osteopenic postmenopausal women. Calcif Tissue Int. 2000;67(6):443–8.
Fleisher L, Trudelle-Jackson M, Thompson E, et al. Effects of weight-bearing and resistance exercises on lower extremity strength, postural stability, and quality of life in postmenopausal women with low bone mass. J Womens Health Phys. 2011;35(3):114–27.
Iwamoto J, Takeda T, Otani T, et al. Effect of increased physical activity on bone mineral density in postmenopausal osteoporotic women. Keio J Med. 1998;47(3):157–61.
Iwamoto J, Takeda T, Ichimura S. Effects of exercise training and detraining on BMD in post-menopausal women with osteoprosis. J Ortho Sci. 2001;6(2):128–32. https://doi.org/10.1007/s007760100059.
Jones G, Jakobi J, Taylor A. Community exercise program for older adults recovering from hip fracture: a pilot study. J Aging Phys Act. 2006;14(4):439–55.
Korpelainen R, Keinänen-Kiukaanniemi J, Heikkinen S, et al. Effect of exercise on extraskeletal risk factors for hip fractures in elderly women with low BMD: a population-based randomized controlled trial. J Bone Miner Res. 2006;21(5):772–9.
Korpelainen R, Keinänen-Kiukaanniemi J, Heikkinen S, et al. Effect of impact exercise on bone mineral density in elderly women with low BMD: a population-based randomized controlled 30-month intervention. Osteoporos Int. 2006;17(1):109–18.
Liu-Ambrose T, Khan K, Eng J, et al. Resistance and agility training reduce fall risk in women aged 75 to 85 with low bone mass: a 6-month randomized, controlled trial. J Am Geriatr Soc. 2004;52(5):657–65.
Liu-Ambrose T, Khan K, Eng J, et al. Both resistance and agility training increase cortical bone density in 75- to 85-year-old women with low bone mass: a 6-month randomized controlled trial. J Clin Densitom. 2004;7(4):390–8.
Liu-Ambrose T, Khan K, Eng J, et al. Balance confidence improves with resistance or agility training. Increase is not correlated with objective changes in fall risk and physical abilities. Gerontology. 2004;50(6):373–82.
Liu-Ambrose T, Khan K, Eng J, et al. Both resistance and agility training reduce back pain and improve health-related quality of life in older women with low bone mass. Osteoporos Int. 2005;16(11):1321–9.
Marchese DI, D’Andrea M, Ventura V, et al. Effects of a weight-bearing exercise training on bone mineral density and neuromuscular function of osteopenic women. Eur J Inflamm. 2012;10(3):427–35.
Olsen C, Bergland A. The effect of exercise and education on fear of falling in elderly women with osteoporosis and a history of vertebral fracture: results of a randomized controlled trial. Osteoporos Int. 2014;25(8):2017–25.
Papaioannou A, Adachi JD, Winegard K, et al. Efficacy of home-based exercise for improving quality of life among elderly women with symptomatic osteoporosis-related vertebral fractures. Osteoporos Int. 2003;14(8):677–82.
Pernambuco C, Borba-Pinheiro C, Vale DS, et al. Functional autonomy, bone mineral density ( BMD ) and serum osteocalcin levels in older female participants of an aquatic exercise program (AAG). Arch Gerontol Geriatr. 2013;56(3):466–71. https://doi.org/10.1016/j.archger.2012.12.012.
Resnick B, Orwig D, Yu-Yahiro J, et al. Testing the effectiveness of the exercise plus program in older women post-hip fracture. Ann Behav Med. 2007;34(1):67–76. https://doi.org/10.1007/BF02879922.
Sherrington C, Lord SR. Home exercise to improve strength and walking velocity after hip fracture : a randomized controlled trial. Arch Phys Med Rehabil. 1997;78(2):208–12. https://doi.org/10.1016/s0003-9993(97)90265-3.
Smulders E, Weerdesteyn V, Groen BE, et al. Efficacy of a short multidisciplinary falls prevention program for elderly persons with osteoporosis and a fall history: a randomized controlled trial. Arch Phys Med Rehabil. 2010;91(11):1705–11. https://doi.org/10.1016/j.apmr.2010.08.004.
Watson SL, Weeks BK, Weis LJ, et al. High-intensity resistance and impact training improves bone mineral density and physical function osteoporosis: the LIFTMOR randomized controlled trial. J Bone Miner Res. 2018;33(2):211–20. https://doi.org/10.1002/jbmr.3284.
Watson SL, Weeks BK, Weis LJ, et al. High-intensity exercise did not cause vertebral fractures and improves thoracic kyphosis in postmenopausal women with low to very low bone mass: the LIFTMOR trial. Osteoporos Int. 2019;30(5):957–64. https://doi.org/10.1007/s00198-018-04829-z.
Wen H, Huang Y, Li T, et al. Effects of short-term step aerobics exercise on bone metabolism and functional fitness in postmenopausal women with low bone mass. Osteoporos Int. 2017;28(2):539–47.
Howe T, Shea B, Dawson L, et al. Exercise for preventing and treating osteoporosis in postmenopausal women. Cochrane Database Syst Rev. 2011;7.
Kelley G, Kelley K, Kohrt W. Effects of ground and joint reaction force exercise on lumbar spine and femoral neck bone mineral density in postmenopausal women: a meta-analysis of randomized controlled trials. BMC Musculoskelet Disord. 2012;20(13):177.
Zehnacker CH, Bemis-Dougherty A. Effect of weighted exercises on bone mineral density in post menopausal women a systematic review. J Geriatr Phys Ther. 2007;30(2):79–88.
Kemmler W, Von Stengel S. High-intensity exercise to prevent fractures—risk or gain? Nat Rev Endocrinol. 2018;14(1):6–8.
Kemmler W, Bebenek M, Kohl M, et al. Exercise and fractures in postmenopausal women. Final results of the controlled Erlangen Fitness and Osteoporosis Prevention Study (EFOPS). Osteoporos Int. 2015;26(10):2491–9.
Vainionpää A, Korpelainen R, Vihriälä E, et al. Intensity of exercise is associated with bone density change in premenopausal women. Osteoporos Int. 2006;17(3):455–63.
Sherrington C, Fairhall N, Wallbank G, et al. Exercise for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2019;1.
Gibbs J, MacIntyre N, Ponzano M, et al. Exercise for improving outcomes after osteoporotic vertebral fracture. Cochrane Database Syst Rev. 2019;7.
Brown J, Josee R. The Scientific Advisory Council of the Osteoporosis Society of Canada. 2002 clinical practice guidelines for the diagnosis and management of osteoporosis in Canada. CMAJ. 2002;167(10):S1–34.
Cauley JA, Thompson DE, Ensrud KC, et al. Risk of mortality following clinical fractures. Osteoporos Int. 2000;11:556–61.
Robinovitch S, Feldman F, Yang Y, et al. Video capture of the circumstances of falls in elderly people residing in long-term care: an observational study. Lancet. 2013;381(9860):47–54. https://doi.org/10.1016/S0140-6736(12)61263-X.
Stel V, Smit J, Pluijm M, et al. Consequences of falling in older men and women and risk factors for health service use and functional decline. Age Ageing. 2004;33(1):58–65.
Acknowledgements
The authors would like to acknowledge the assistance of Jeff Templeton, Sydney Mannell, Vivetha Ramesh, and Nora Thorpe in the screening and the data extraction phases of this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Authorship Contributions
IBR screened, analyzed, interpreted, and wrote the first draft of the manuscript. LG and LT assisted with statistical methods and analyses. PC, DB, MA, and LG reviewed the final analysis and revised the original manuscript. JS conducted the literature search. MP and ZH assisted in screening and revising the final manuscript. All authors read and approved the final manuscript.
Funding
Funding for this project was received from Osteoporosis Canada, the Canadian.
Availability of data and materials
Available upon request for research purposes. Institutes of Health Research, the Federation of Portuguese Canadian Business & Professionals, the University of Waterloo, and the Saskatchewan Health Research Foundation.
Conflict of interest
Isabel Rodrigues, Matteo Ponzano, Zeinab Hosseini, Lehana Thabane, Phil Chilibeck, Debra Butt, Maureen Ashe, Jackie Stapleton, John Wark and Lora Giangregorio declare that they have no conflicts of interest relevant to the content of this review.
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Role of sponsor
Funding sponsors did not provide a role, other than financial support, in developing this review.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rodrigues, I.B., Ponzano, M., Hosseini, Z. et al. The Effect of Impact Exercise (Alone or Multicomponent Intervention) on Health-Related Outcomes in Individuals at Risk of Fractures: A Systematic Review and Meta-Analysis of Randomized Controlled Trials. Sports Med 51, 1273–1292 (2021). https://doi.org/10.1007/s40279-021-01432-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-021-01432-x