Abstract
Background
Potentially inappropriate prescriptions (PIPs) can lead to adverse drug reactions and should be avoided whenever possible.
Objective
Our objective was to assess the PIP resumption rate 6 months after discharge from our geriatric unit and to compare it with data in the literature.
Methods
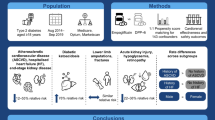
This single-center observational study included patients aged ≥ 70 years with at least one PIP that had been stopped during hospitalization (according to Screening Tool for Older Persons Prescriptions [STOPP] and Screening Tool to Alert doctors to Right Treatment [START] criteria, version 2) between May 2018 and October 2018. We collected sociodemographic data, medication reconciliation data, and descriptive data during a comprehensive geriatric assessment. Each patient’s medication history after discharge was determined in collaboration with their usual community pharmacist.
Results
A total of 125 patients (females 70%, mean age 87.1 years) were included. Data for the admission and discharge medication reconciliations were available for 44 patients (35%). On admission, 121 of the 125 patients (97%) were taking cardiovascular medication. Of the 336 treatments withdrawn, 61 (18.2%) had been re-prescribed at 6 months post-discharge—including half within the first month. The most frequent STOPP criterion was lack of indication (32%), and the overall PIP resumption rate was 22%. According to the anatomical therapeutic chemical (ATC) classification, the main organ system affected by PIPs was the cardiovascular system (47%, with a resumption rate of 17%).
Conclusion
Our results highlighted a low PIP resumption rate at 6 months and showed that a collaborative medication review is associated with persistent medium-term medication changes.




Similar content being viewed by others
References
Projections de population à l’horizon 2060—Insee Première—1320. 2015.
EU statistics on income and living conditions (EU-SILC) methodology—Statistics Explained. 2016.
Les dépenses de santé en 2017—Résultats des comptes de la santé—Édition 2018—Ministère des Solidarités et de la Santé. 2017.
Gonthier R, Blanc P, Stierlam F. Should we treat all the diseases of the elderly? Therapie. 2004;59(2):227–32.
Herr M, Sirven N, Grondin H, et al. Frailty, polypharmacy, and potentially inappropriate medications in old people: findings in a representative sample of the French population. Eur J Clin Pharmacol. 2017;73(9):1165–72.
Pérez T, Moriarty F, Wallace E, et al. Prevalence of potentially inappropriate prescribing in older people in primary care and its association with hospital admission: longitudinal study. BMJ. 2018;363:k4524.
Gurwitz JH, Field TS, Harrold LR, Rothschild J, Debellis K, Seger AC, et al. Incidence and preventability of adverse drug events among older persons in the ambulatory setting. JAMA. 2003;289:1107–16.
Tulner LR, Kuper IMJA, Frankfort SV, et al. Discrepancies in reported drug use in geriatric outpatients: relevance to adverse events and drug interactions. Am J Geriatr Pharmacother. 2009;7(2):93–104.
Joachim C, Trenque T, Novella JL, et al. Prévalence de la iatropathogénie chez des sujets âgés hospitalisés en unité spécialisée dans les pathologies démentielles. Revue d’Épidémiologie et de Santé Publique. 2011;59:96.
Onder G, Landi F, Cesari M, et al. Inappropriate medication use among hospitalized older adults in Italy: results from the Italian Group of Pharmacoepidemiology in the Elderly. Eur J Clin Pharmacol. 2003;59(2):157–62.
Helas E, Seux V, Pauly V, et al. Drugs modifications for inpatients hospitalized in acute care for elders unit. Revue Médicale Interne. 2010;32:15–22.
Pandraud-Riguet I, Bonnet-Zamponi D, Bourcier E, et al. Monitoring of potentially inappropriate prescriptions in older inpatients: a french multicenter study. J Am Geriatr Soc. 2017;65(12):2713–9.
Blix HS, Viktil KK, Reikvam A, et al. The majority of hospitalized patients have drug-related problems: results from a prospective study in general hospitals. Eur J Clin Pharmacol. 2004;60(9):651–8.
Bemt PMLA, Loos EM, Linden C, et al. Effect of medication reconciliation on unintentional medication discrepancies in acute hospital admissions of elderly adults: a multicenter study. J Am Geriatr Soc. 2013;61(8):1262–8.
Nice CRC. SFPC Mémo Conciliation des traitements médicamenteux.:18.
Ravn-Nielsen LV, Duckert ML, Lund ML, et al. Effect of an In-hospital multifaceted clinical pharmacist intervention on the risk of readmission: a randomized clinical trial. JAMA Internal Med. 2018;178(3):375–82.
Piau A, Huet Y, Gallini A, et al. Optimization of drug therapy in elderly individuals admitted to a geriatric unit. Clin Interv Aging. 2017;12:1691–6.
Frély A, Chazard E, Pansu A, et al. Impact of acute geriatric care in elderly patients according to the Screening Tool of Older Persons’ Prescriptions/Screening Tool to Alert doctors to Right Treatment criteria in northern France. Geriatr Gerontol Int. 2016;16(2):272–8.
Haute Autorité de Santé—Avis n◦2017.0082/AC/SA3P du 4 octobre 2017 du collège de la Haute Autorité de santé relatif aux supports d’accompagnement des patients âgés polymédiqués par les pharmaciens d’officine—le bilan de médication, convention entre l’UNCAM et les syndicats d’officinaux.
Coutellier M, Mouly S, Delcey V, et al. What happens to therapeutic changes decided during hospitalization in an internal medicine ward? A two-month single-centre prospective study in France. La Revue de medecine interne. 2014;35(8):498–502.
Martin P, Tamblyn R, Benedetti A, et al. Effect of a pharmacist-led educational intervention on inappropriate medication prescriptions in older adults: the D-PRESCRIBE randomized clinical trial. JAMA. 2018;320(18):1889–98.
Gallagher P, Ryan C, Byrne S, et al. STOPP (Screening Tool of Older Person’s Prescriptions) and START (Screening Tool to Alert doctors to Right Treatment). Consensus validation. Int J Clin Pharmacol Ther. 2008;46(2):72–83.
O’Mahony D, Gallagher P, Ryan C, et al. STOPP & START criteria: A new approach to detecting potentially inappropriate prescribing in old age./data/revues/18787649/v1i1/S1878764910000112/. 2010.
Lang PO, Dramé M, Guignard B, et al. Les critères STOPP/START.v2: adaptation en langue française. NPG. 2015;15(90):323–36.
Metthodology., W.H.O.C.C.f.D.S International language for drug utilisation research.
Charlson ME, Pompei P, Ales KL, et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis. 1987;40(5):373–83.
Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”: a practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189–98.
Mosnier-Thoumas S, Videau MN, Lafargue A, et al. Benefit of the geriatric mobile unit’s intercession on the quality of medical prescriptions for the elderly: past year assessment. Ann Pharm Fr. 2019;77(2):136–45.
Lachamp M, Pauly V, Sambuc R, et al. Cost-effectiveness of drugs modifications for inpatients hospitalized in acute care geriatric units. La Revue de Medecine Interne. 2012;33(9):482–90.
Tuetey C, Karcher P, Groc YL, et al. Les déterminants de la prolongation des séjours en SSRG et les indicateurs du devenir des patients après leur sortie: Étude rétrospective au CHRU de Strasbourg. NPG. 2015;15(90):337–45.
Farbos F. Optimisation thérapeutique dans un service de post-urgence gériatrique: suivi des recommandations hospitalières par le médecin généraliste. Sciences pharmaceutiques. 2014. ffdumas01107392f.
Lajus J. Unité d’évaluation gériatrique pluriprofessionnelle dans la ville de Bordeaux: suivi des propositions d’optimisation thérapeutique par les médecins généralistes. Médecine humaine et pathologie. 2018. ffdumas-02025473.
Riordan DO, Aubert CE, Walsh KA, et al. Prevalence of potentially inappropriate prescribing in a subpopulation of older European clinical trial participants: a cross-sectional study. BMJ Open. 2018;8(3):e019003.
Zermansky AG, Alldred DP, Petty DR, et al. Clinical medication review by a pharmacist of elderly people living in care homes-randomised controlled trial. Age Ageing. 2006;35(6):586–91.
Mekonnen AB, Abebe TB, McLachlan AJ, et al. Impact of electronic medication reconciliation interventions on medication discrepancies at hospital transitions: a systematic review and meta-analysis. BMC Med Inform Decis Mak. 2016;16:112.
Bosma LBE, Hunfeld NGM, Quax RAM, et al. The effect of a medication reconciliation program in two intensive care units in the Netherlands: a prospective intervention study with a before and after design. Ann Intensive Care. 2018;8(1):19.
Pourrat X, Roux C, Bouzige B, et al. Impact of drug reconciliation at discharge and communication between hospital and community pharmacists on drug-related problems: study protocol for a randomized controlled trial. Trials. 2014;15:260.
Borione CMA. La conciliation médicamenteuse de sortie: intérêt pour réduire la iatrogénie chez la personne âgée et tisser des liens ville-hôpital. Médecine humaine et pathologie. 2015. dumas-01263157.
Gasperini G, Molinier S, Marimoutou C, et al. Quel est l’impact d’une hospitalisation sur les traitements au long cours chez les patients de plus de 65 ans. Gériatrie et Psychologie Neuropsychiatrie du Vieillissement. 2016;14(4):389–97.
Kreckman J, Wasey W, Wise S, et al. Improving medication reconciliation at hospital admission, discharge and ambulatory care through a transition of care team. BMJ Open Qual. 2018;7(2):e000281.
Johansen JS, Havnes K, Halvorsen KH, et al. Interdisciplinary collaboration across secondary and primary care to improve medication safety in the elderly (IMMENSE study): study protocol for a randomised controlled trial. BMJ Open. 2018;8(1):e020106.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was used for this work.
Conflicts of Interest
Camille Debacq, Julie Bourgueil, Amal Aidoud, Joëlle Bleuet, Marc Mennecart, Veronique Dardaine-Giraud, Bertrand Fougère have no conflicts of interest that are directly relevant to the content of this article.
Availability of data and material
Not applicable.
Ethics approval
This study was performed in line with the principles of the Declaration of Helsinki. Approval was granted by the Ethics Committee of University of medicine of Tours.
Consent
Informed consent of each patient was collected by sending an information letter accompanied by an objection form.
Rights and permissions
About this article
Cite this article
Debacq, C., Bourgueil, J., Aidoud, A. et al. Persistence of Effect of Medication Review on Potentially Inappropriate Prescriptions in Older Patients Following Hospital Discharge. Drugs Aging 38, 243–252 (2021). https://doi.org/10.1007/s40266-020-00830-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-020-00830-6