Abstract
Background
No direct comparisons of ticagrelor and prasugrel with 1-year clinical follow-up have been reported.
Objectives
Our objective was to compare 1-year clinical outcomes among patients with acute coronary syndrome (ACS) managed with percutaneous coronary intervention (PCI) and treated with either ticagrelor or prasugrel in a real-world setting.
Methods
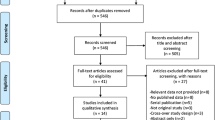
This retrospective study included patients from a payer database who were aged ≥18 years and had ACS managed with PCI with no history of transient ischemic attack (TIA)/stroke. Data were propensity matched for prasugrel use with a 3:1 prasugrel:ticagrelor ratio. Post-discharge net adverse clinical event (NACE) rate at 1 year was evaluated for noninferiority using a pre-defined 20% margin. NACE was a composite of major adverse cardiovascular events (MACE) or rehospitalization for bleeding.
Results
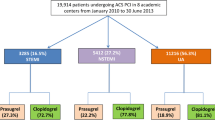
In total, 15,788 ACS-PCI patients were included (prasugrel 12,797; ticagrelor 2991). Prasugrel-treated patients were younger; less likely to be female, have prior myocardial infarction (MI), diabetes, or non-ST-segment elevation MI (NSTEMI); and more likely to have unstable angina (UA) than ticagrelor-treated patients. Prior to matching, NACE and MACE (P < 0.01) were lower, with no difference in bleeding with prasugrel compared with ticagrelor. After matching, there was no significant difference in baseline characteristics. Noninferiority was demonstrated for NACE, MACE, and bleeding between prasugrel and ticagrelor. NACE and MACE were significantly lower with prasugrel use, primarily driven by heart failure, with no significant difference in all-cause death, MI, UA, revascularization, TIA/stroke, or bleeding.
Conclusions
In this retrospective study, physicians preferentially used prasugrel rather than ticagrelor in younger ACS-PCI patients with lower risk of bleeding or comorbidities. After propensity matching, clinical outcomes associated with prasugrel were noninferior to those with ticagrelor.




Similar content being viewed by others
References
Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ACC guideline for the management of patients with non-ST-elevation acute coronary syndromes: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;130:e344–426.
O’Gara PT, Kushner FG, Ascheim DD, et al. ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation. 2013;2013(127):e362–425.
Windecker S, Kolh P, Alfonso F, et al. ESC/EACTS guidelines on myocardial revascularization: the task force on myocardial revascularization of the European Society of Cardiology (ESC) and the European Association for Cardio-Thoracic Surgery (EACTS) Developed with the special contribution of the European Association of Percutaneous Cardiovascular Interventions (EAPCI). Eur Heart J. 2014;35:2541–619.
Levine GN, Bates ER, Bittl JA, et al. ACC/AHA guideline focused update on duration of dual antiplatelet therapy in patients with coronary artery disease: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2016;68(10):1082–115. https://doi.org/10.1016/j.jacc.2016.03.513.
Bagai A, Peterson ED, Honeycutt E, et al. In-hospital switching between adenosine diphosphate receptor inhibitors in patients with acute myocardial infarction treated with percutaneous coronary intervention: Insights into contemporary practice from the TRANSLATE-ACS study. Eur Heart J Acute Cardiovasc Care. 2015;4:499–508.
Wiviott SD, Braunwald E, McCabe CH, et al. Prasugrel versus clopidogrel in patients with acute coronary syndromes. N Engl J Med. 2007;357:2001–15.
Wallentin L, Becker RC, Budaj A, et al. Ticagrelor versus clopidogrel in patients with acute coronary syndromes. New Engl J Med. 2009;361:1045–57.
Steiner S, Moertl D, Chen L, et al. Network meta-analysis of prasugrel, ticagrelor, high- and standard-dose clopidogrel in patients scheduled for percutaneous coronary interventions. Thromb Haemost. 2012;108:318–27.
Chatterjee S, Ghose A, Sharma A, et al. Comparing newer oral anti-platelets prasugrel and ticagrelor in reduction of ischemic events-evidence from a network meta-analysis. J Thromb Thrombolysis. 2013;36:223–32.
Biondi-Zoccai G, Lotrionte M, Agostoni P, et al. Adjusted indirect comparison meta-analysis of prasugrel versus ticagrelor for patients with acute coronary syndromes. Int J Cardiol. 2011;150:325–31.
Passaro D, Fadda V, Maratea D, et al. Anti-platelet treatments in acute coronary syndrome: simplified network meta-analysis. Int J Cardiol. 2011;150:364–7.
Simeone JC, Molife C, Marrett E, et al. One-year post-discharge resource utilization and treatment patterns of patients with acute coronary syndrome managed with percutaneous coronary intervention and treated with ticagrelor or prasugrel. Am J Cardiovasc Drugs. 2015;15:337–50.
AstraZeneca. Brilinta [package insert] 2017 https://www.azpicentral.com/brilinta/brilinta.pdf#page=1. Accessed July 05 2017.
Eli Lilly and Company. Effient [package insert]. 2017. http://pi.lilly.com/us/effient.pdf. Accessed July 05 2017.
Rosenbaum PR, Rubin DB. Reducing bias in observational studies using subclassification on the propensity score. J Am Stat Assoc. 1984;79:516–24.
Rubin DB. The design versus the analysis of observational studies for causal effects: parallels with the design of randomized trials. Stat Med. 2007;26:20–36.
Austin PC. Primer on statistical interpretation or methods report card on propensity-score matching in the cardiology literature from 2004 to 2006: a systematic review. Circ Cardiovasc Qual Outcomes. 2008;1:62–7.
Cohen M. Predictors of bleeding risk and long-term mortality in patients with acute coronary syndromes. Curr Med Res Opin. 2005;21:439–45. https://doi.org/10.1185/030079905X30725.
Mehran R, Baber U, Steg PG, et al. Cessation of dual antiplatelet treatment and cardiac events after percutaneous coronary intervention (PARIS): 2 year results from a prospective observational study. Lancet. 2013;382:1714–22.
Moscucci M, Fox KA, Cannon CP, et al. Predictors of major bleeding in acute coronary syndromes: the Global Registry of Acute Coronary Events (GRACE). Eur Heart J. 2003;24:1815–23.
Austin PC, Mamdani MM. A comparison of propensity score methods: a case-study estimating the effectiveness of post-AMI statin use. Stat Med. 2006;25:2084–106. https://doi.org/10.1002/sim.2328.
Schneeweiss S. Sensitivity analysis and external adjustment for unmeasured confounders in epidemiologic database studies of therapeutics. Pharmacoepidemiol Drug Saf. 2006;15(5):291–303.
Bae JP, Faries DE, Ernst FR, et al. Real-world observations with prasugrel compared to clopidogrel in acute coronary syndrome patients treated with percutaneous coronary intervention in the United States. Curr Med Res Opin. 2014;30:2207–16.
Wang TY, Zettler M, Effron MB, et al. Comparative effectiveness of prasugrel vs. clopidogrel among acute myocardial infarction patients treated with percutaneous coronary intervention: 30-day outcomes from the TRANSLATE-ACS observational study. J Am Coll Cardiol. 2013;62(18_S1):B1. https://doi.org/10.1016/j.jacc.2013.08.729.
Baber U, Sartori S, Aquino M, et al. 90-Day Effectiveness and Safety of Prasugrel vs. Clopidogrel as Used in Clinical Practice in Patients With ACS Undergoing PCI: Initial Findings from the PROMETHEUS Study. Society for Cardiovascular Angiography and Interventions—38th Annual Scientific Sessions. 2015.
Larmore C, Effron MB, Molife C, et al. ”Real-World” comparison of prasugrel with ticagrelor in patients with acute coronary syndrome treated with percutaneous coronary intervention in the United States. Catheter Cardiovasc Interv. 2016;88(4):535–44. https://doi.org/10.1002/ccd.26279.
Becker RC, Bassand JP, Budaj A, et al. Bleeding complications with the P2Y12 receptor antagonists clopidogrel and ticagrelorin the PLATelet inhibition and patient Outcomes (PLATO) trial. Eur Heart J. 2011;32:2933–44.
Alexopoulos D, Galati A, Xanthopoulou I, et al. Ticagrelor versus prasugrel in acute coronary syndrome patients with high on-clopidogrel platelet reactivity following percutaneous coronary intervention. J Am Coll Cardiol. 2012;60:193–9.
Alexopoulos D, Xanthopoulou I, Mavronasiou E, et al. Randomized assessment of ticagrelor versus prasugrel antiplatelet effects in patients with diabetes. Diabetes Care. 2013;36:2211–6.
Vilahur G, Gutiérrez M, Casani L, et al. Protective effects of ticagrelor on myocardial injury after infarctionclinical perspective. Circulation. 2016;134:1708–19.
Jeong HS, Hong SJ, Cho SA, et al. Comparison of ticagrelor versus prasugrel for inflammation, vascular function, and circulating endothelial progenitor cells in diabetic patients with non–ST-segment elevation acute coronary syndrome requiring coronary stenting: a prospective, randomized, crossover trial. JACC Cardiovasc Interv. 2017;10:1646–58.
Motovska Z, Hlinomaz O, Miklik R, et al. Prasugrel versus ticagrelor in patients with acute myocardial infarction treated with primary percutaneous coronary intervention: multicenter randomized Prague-18 study. Circulation. 2016;134:1603–12.
Minicucci MF, Azevedo PS, Polegato BF, et al. Heart failure after myocardial infarction: clinical implications and treatment. Clin Cardiol. 2011;34:410–4.
Alexopoulos D, Xanthopoulou I, Gkizas V, et al. Randomized assessment of ticagrelor versus prasugrel antiplatelet effects in patients with ST-segment-elevation myocardial infarction. Circ Cardiovasc Interv. 2012;5:797–804.
Parodi G, Valenti R, Bellandi B, et al. Comparison of prasugrel and ticagrelor loading doses in ST-segment elevation myocardial infarction patients: RAPID (Rapid Activity of Platelet Inhibitor Drugs) primary PCI study. J Am Coll Cardiol. 2013;61:1601–6.
Bonello L, Laine M, Kipson N, et al. Ticagrelor increases adenosine plasma concentration in patients with an acute coronary syndrome. J Am Coll Cardiol. 2014;63:872–7.
Nanhwan MK, Ling S, Kodakandla M, et al. Chronic treatment with ticagrelor limits myocardial infarct size: an adenosine and cyclooxygenase-2-dependent effect. Arterioscler Thromb Vasc Biol. 2014;34:2078–85.
Stone GW, Witzenbichler B, Weisz G, et al. Platelet reactivity and clinical outcomes after coronary artery implantation of drug-eluting stents (ADAPT-DES): a prospective multicentre registry study. Lancet. 2013;382:614–23.
Kohli P, Udell JA, Murphy SA, et al. Discharge aspirin dose and clinical outcomes in patients with acute coronary syndromes treated with prasugrel versus clopidogrel: an analysis from the TRITON-TIMI 38 study (trial to assess improvement in therapeutic outcomes by optimizing platelet inhibition with prasugrel-thrombolysis in myocardial infarction 38). J Am Coll Cardiol. 2014;63:225–32.
Acknowledgements
The authors thank Doug Faries, PhD, Hsiao Lieu, MD, Molly Tomlin, MS, Nayan Acharya, MD (deceased), and Vladimir Kryzhanovski, MD, at Eli Lilly and Company; Feride Frech-Tamas, PhD, Elizabeth Marrett, MPH, and Qiaoyi Zhang, PhD, at Daiichi Sankyo Inc.; and Teresa Bennett and Jaime Lucove at Symphony Health Solutions, for valuable contributions to this study and manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by Daiichi Sankyo Inc., Parsippany, NJ, USA, and Eli Lilly and Company, Indianapolis, IN, USA.
Conflict of interest
MBE is a shareholder of, receives a pension from, and—at the time of the study—was an employee of Eli Lilly and Company. CM, SK, YZ, and PLM are shareholders and employees of Eli Lilly and Company. GV is an unpaid consultant to Daiichi Sankyo and Eli Lilly. KVN and RLP II are paid consultants to Daiichi Sankyo and Eli Lilly. JCS, BLN, and BM are employed by Evidera, which received funding from Eli Lilly and Company and Daiichi Sankyo Inc. to conduct this research.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Effron, M.B., Nair, K.V., Molife, C. et al. One-Year Clinical Effectiveness Comparison of Prasugrel with Ticagrelor: Results from a Retrospective Observational Study using an Integrated Claims Database. Am J Cardiovasc Drugs 18, 129–141 (2018). https://doi.org/10.1007/s40256-017-0255-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40256-017-0255-y