Abstract
Purpose
Topical negative pressure (TNP) has become a common treatment of infected wounds. A systematic review and meta-analysis was performed to investigate TNP efficacy compared to conventional therapy in the treatment of deep surgical site infections (SSIs), particularly post-sternotomy infections.
Methods
MEDLINE, EMBASE, and Cochrane Central Register of Controlled Trials were searched for randomized clinical trials (RCTs) and observational studies comparing TNP to conventional treatment in deep SSIs published up to February 2012. Study quality was evaluated through the GRADE system and bias risk through the Newcastle–Ottawa scale (NOS). Primary outcome was infection cure/wound resolution rate. Secondary outcomes were adverse events, length of stay, mortality, and costs. The results are presented with 95 % confidence intervals (95 % CIs) and report estimates as odds ratios (ORs). Heterogeneity was determined through the I 2 test, with >50 % being considered significant.
Results
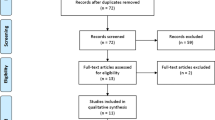
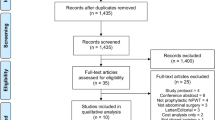
Among 83 studies retrieved, 12 cohort studies including 873 patients were considered. All the studies were of low quality, 11/12 had a medium risk of bias, and none were RCTs. Wound resolution was obtained more frequently in TNP-treated patients as compared with continuous and closed drainage (OR 6.45, 95 % CI 3.46–12.00). TNP use was associated with significant reduction of length of stay compared with standard of care (mean difference: 8.21, 95 % CI −12.19, −4.23). High heterogeneity was detected between studies, explained by the TNP comparator type.
Conclusions
The systematic review and meta-analysis suggest that TNP might be more effective than standard therapy in the cure of deep SSIs. However, multicenter RCTs are needed to confirm the potential value of this treatment.


Similar content being viewed by others
References
Edwards JR, Peterson KD, Mu Y, et al. National Healthcare Safety Network (NHSN) report: data summary for 2006 through 2008, issued December 2009. Am J Infect Control. 2009;37:783–805.
Marchi M, Grilli E, Mongardi M, Bedosti C, Nobilio L, Moro ML. Prevalence of infections in long-term care facilities: how to read it? Infection. 2012;40:493–500.
Johnson KE, Kiyatkin DE, An AT, Riedel S, Melendez J, Zenilman JM. PCR offers no advantage over culture for microbiologic diagnosis in cellulitis. Infection. 2012;40:537–41.
Tacconelli E. Antimicrobial use: risk driver of multidrug resistant microorganisms in healthcare settings. Curr Opin Infect Dis. 2009;22:352–8.
Singer AJ, Dagum AB. Current management of acute cutaneous wounds. N Engl J Med. 2008;359:1037–46.
Bradley M, Cullum N, Nelson EA, Petticrew M, Sheldon T, Torgerson D. Systematic reviews of wound care management: (2). Dressings and topical agents used in the healing of chronic wounds. Health Technol Assess. 1999;3:1–35.
Argenta LC, Morykwas MJ. Vacuum-assisted closure: a new method for wound control and treatment: clinical experience. Ann Plast Surg. 1997;38:563–76.
Pan A, Cauda R, Concia E, et al.; GISIG (Gruppo Italiano di Studio sulle Infezioni Gravi) Working Group on Complicated Skin and Skin-Structure Infections. Consensus document on controversial issues in the treatment of complicated skin and skin-structure infections. Int J Infect Dis. 2010;14(Suppl 4):S39–53.
Damiani G, Pinnarelli L, Sommella L, et al. Vacuum-assisted closure therapy for patients with infected sternal wounds: a meta-analysis of current evidence. J Plast Reconstr Aesthet Surg. 2011;64:1119–23.
Mangram AJ, Horan TC, Pearson ML, et al. Guideline for prevention of surgical site infection, 1999. Hospital Infection Control Practices Advisory Committee. Infect Control Hosp Epidemiol. 1999;20:250–78.
Wells GA, Shea B, O’Connell D, et al. The Newcastle–Ottawa Scale (NOS) for assessing the quality of nonrandomised studies in meta-analyses. http://www.ohri.ca/programs/clinical_epidemiology/oxford.asp. Accessed 17 May 2011.
Atkins D, Best D, Briss PA, et al.; GRADE Working Group. Grading quality of evidence and strength of recommendations. BMJ. 2004;328:1490.
Higgins JP, Thompson SG. Quantifying heterogeneity in a meta-analysis. Stat Med. 2002;21:1539–58.
Begg CB, Mazumdar M. Operating characteristics of a rank correlation test for publication bias. Biometrics. 1994;50:1088–101.
Berg HF, Brands WG, van Geldorp TR, et al. Comparison between closed drainage techniques for the treatment of postoperative mediastinitis. Ann Thorac Surg. 2000;70:924–9.
Fleck TM, Koller R, Giovanoli P, et al. Primary or delayed closure for the treatment of poststernotomy wound infections? Ann Plast Surg. 2004;52:310–4.
Fuchs U, Zittermann A, Stuettgen B, Groening A, Minami K, Koerfer R. Clinical outcome of patients with deep sternal wound infection managed by vacuum-assisted closure compared to conventional therapy with open packing: a retrospective analysis. Ann Thorac Surg. 2005;79:526–31.
Scholl L, Chang E, Reitz B, Chang J. Sternal osteomyelitis: use of vacuum-assisted closure device as an adjunct to definitive closure with sternectomy and muscle flap reconstruction. J Card Surg. 2004;19:453–61.
Simek M, Hajek R, Zalesak B, et al. Topical negative pressure versus conventional treatment of deep sternal wound infection in cardiac surgery. Eur Wound Manag Assoc J. 2008;8:17–20.
Catarino PA, Chamberlain MH, Wright NC, et al. High-pressure suction drainage via a polyurethane foam in the management of poststernotomy mediastinitis. Ann Thorac Surg. 2000;70:1891–5.
Segers P, De Jong AP, Kloek JJ, de Mol BA. Poststernotomy mediastinitis: comparison of two treatment modalities. Interact Cardiovasc Thorac Surg. 2005;4:555–60.
Sjögren J, Gustafsson R, Nilsson J, Malmsjö M, Ingemansson R. Clinical outcome after poststernotomy mediastinitis: vacuum-assisted closure versus conventional treatment. Ann Thorac Surg. 2005;79:2049–55.
Song DH, Wu LC, Lohman RF, Gottlieb LJ, Franczyk M. Vacuum assisted closure for the treatment of sternal wounds: the bridge between debridement and definitive closure. Plast Reconstr Surg. 2003;111:92–7.
Colwell AS, Donaldson MC, Belkin M, Orgill DP. Management of early groin vascular bypass graft infections with sartorius and rectus femoris flaps. Ann Plast Surg. 2004;52:49–53.
De Feo M, Vicchio M, Nappi G, Cotrufo M. Role of vacuum in methicillin-resistant deep sternal wound infection. Asian Cardiovasc Thorac Ann. 2010;18:360–3.
Assmann A, Boeken U, Feindt P, Schurr P, Akhyari P, Lichtenberg A. Vacuum-assisted wound closure is superior to primary rewiring in patients with deep sternal wound infection. Thorac Cardiovasc Surg. 2011;59:25–9.
Gregor S, Maegele M, Sauerland S, Krahn JF, Peinemann F, Lange S. Negative pressure wound therapy: a vacuum of evidence? Arch Surg. 2008;143:189–96.
Conflict of interest
No author has any conflict nor funding to declare.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below are the links to the electronic supplementary material.
15010_2013_536_MOESM1_ESM.png
Supplementary material 1 (PNG 63 kb) Fig. E1 Time to healing, expressed in days, in patients with SSIs treated with TNP or standard of care. Legend: Mean and standard deviation (SD) of time to healing among the TNP group and controls
15010_2013_536_MOESM2_ESM.eps
Supplementary material 2 (EPS 596 kb) Fig. E2. Crude mortality in patients with SSIs treated with TNP or standard of care. E2a: overall mortality at the last follow-up visit reported in the study. E2b: short-term mortality (in-hospital to 3 months). E2c: long-term mortality (6 to 12 months) Legend: The labels Events and Total refer to number of patients deceased and total included cases, respectively, among the TNP group and controls
15010_2013_536_MOESM4_ESM.pdf
Supplementary material 4 (PDF 14 kb) Fig. E3. Funnel plot of studies assessing the primary outcome. SE, standard error; log, logarithm; OR, odds ratio
Rights and permissions
About this article
Cite this article
Pan, A., De Angelis, G., Nicastri, E. et al. Topical negative pressure to treat surgical site infections, with a focus on post-sternotomy infections: a systematic review and meta-analysis. Infection 41, 1129–1135 (2013). https://doi.org/10.1007/s15010-013-0536-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-013-0536-6