Abstract
Introduction
Reading disorders caused by homonymous visual field defects (HVFDs) have a significant impact on a patient’s quality of life. However, no review has been conducted to evaluate the available evidence on the effects of rehabilitative interventions on reading disorders caused by HVFDs. Thus, the aim of this study was to systematically evaluate the effects of rehabilitative interventions on reading disorders caused by HVFDs.
Methods
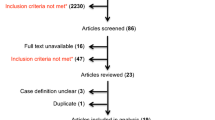
We searched the MEDLINE/PubMed, Cochrane Library, ClinicalTrials.gov, CINAHL, and ScienceDirect databases for relevant articles. Relevant search terms were used to identify reports of randomized controlled trials or randomized crossover trials published between January 1990 and December 2021. Only studies that included reading-speed-related outcomes were analyzed. Risk of bias was assessed using the PEDro scale. Meta-analysis was conducted using a random-effects model, and standardized mean differences (SMD) and 95% confidence intervals (CIs) were calculated. Heterogeneity was assessed using the Ι2 statistic.
Results
Nine studies were included in the meta-analysis. The results showed that rehabilitative interventions significantly improved reading disorders caused by HVFDs (SMD = 0.30; 95% CI 0.08–0.51; P < 0.01; Ι2 = 0.0%). Subgroup analysis showed that reading training significantly improved reading disorders (SMD = 0.35; 95% CI 0.05–0.66; P = 0.02; Ι2 = 0.0%).
Conclusion
Reading disorders caused by HVFDs can be improved through rehabilitation. In addition, reading training for the improvement of eye movement and fixation to compensate for foveal and parafoveal visual field defects may improve reading speed.


Similar content being viewed by others
Data Availability
All data included and analyzed in this study can be confirmed in this article and supplementary materials.
Abbreviations
- 95% CIs:
-
95% Confidence intervals
- FEF:
-
Frontal eye field
- HVFDs:
-
Homonymous visual field defects
- PEF:
-
Parietal eye field
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PROSPERO:
-
Prospective Register of Systematic Reviews
- RCT:
-
Randomized controlled or crossover trial
- rtACS:
-
Repetitive transorbital alternating current stimulation
- SMD:
-
Standardized mean differences
- tDCS:
-
Transcranial direct current stimulation
- VRT:
-
Visual restoration therapy
References
Machner B, Sprenger A, Sander T, Heide W, Kimmig H, Helmchen C, Kömpf D (2009) Visual search disorders in acute and chronic homonymous hemianopia: lesion effects and adaptive strategies. Ann NY Acad Sci 1164(1):419–426. https://doi.org/10.1111/j.1749-6632.2009.03769.x
Zihl J (1995) Visual scanning behavior in patients with homonymous hemianopia. Neuropsychologia 33(3):287–303. https://doi.org/10.1016/0028-3932(94)00119-a
Zihl J (1999) Oculomotor scanning performance in subjects with homonymous visual field disorders. Vis Impair Res 1(1):23–31. https://doi.org/10.1076/vimr.1.1.23.4450
McGwin G Jr, Wood J, Huisingh C, Owsley C (2016) Motor vehicle collision involvement among persons with Hemianopia and Quadrantanopia. Geriatrics 1(3):19. https://doi.org/10.3390/geriatrics1030019
Papageorgiou E, Hardiess G, Ackermann H, Wiethoelter H, Dietz K, Mallot HA, Schiefer U (2012) Collision avoidance in persons with homonymous visual field defects under virtual reality conditions. Vision Res 52(1):20–30. https://doi.org/10.1016/j.visres.2011.10.019
Gall C, Sabel BA (2012) Reading performance after vision rehabilitation of subjects with homonymous visual field defects. PM&R 4(12):928–935. https://doi.org/10.1016/j.pmrj.2012.08.020
Kerkhoff G, Münßinger U, Eberle-strauss G, Stögerer E (1992) Rehabilitation of Hemianopic Alexia in patients with postgeniculate visual field disorders. Neuropsychol Rehabil 2(1):21–42. https://doi.org/10.1080/09602019208401393
Rowe FJ, Wright D, Brand D, Jackson C, Harrison S, Maan T, Scott C, Vogwell L, Peel S, Akerman N, Dodridge C, Howard C, Shipman T, Sperring U, Macdiarmid S, Freeman C (2013) A prospective profile of visual field loss following stroke: Prevalence, type, rehabilitation, and outcome. Biomed Res Int 2013:719096. https://doi.org/10.1155/2013/719096
Trauzettel-Klosinski S, Brendler K (1998) Eye movements in reading with hemianopic field defects: the significance of clinical parameters. Graefes Arch Clin Exp Ophthalmol 236(2):91–102. https://doi.org/10.1007/s004170050048
Zihl J (1995) Eye movement patterns in hemianopic dyslexia. Brain 118(4):891–912. https://doi.org/10.1093/brain/118.4.891
Warren M (2009) Pilot study on activities of daily living limitations in adults with Hemianopsia. Am J Occup Ther 63(5):626–633. https://doi.org/10.5014/ajot.63.5.626
Papageorgiou E, Hardiess G, Schaeffel F, Wiethoelter H, Karnath HO, Mallot H, Schoenfisch B, Schiefer U (2007) Assessment of vision-related quality of life in patients with homonymous visual field defects. Graefes Arch Clin Exp Ophthalmol 245(12):1749–1758. https://doi.org/10.1007/s00417-007-0644-z
Bolognini N, Rasi F, Coccia M, Làdavas E (2005) Visual search improvement in hemianopic patients after audio-visual stimulation. Brain 128(12):2830–2842. https://doi.org/10.1093/brain/awh656
Mannan SK, Pambakian AL, Kennard C (2010) Compensatory strategies following visual search training in patients with homonymous hemianopia: an eye movement study. J Neurol 257(11):1812–1821. https://doi.org/10.1007/s00415-010-5615-3
Nelles G, Esser J, Eckstein A, Tiede A, Gerhard H, Diener HC (2001) Compensatory visual field training for patients with hemianopia after stroke. Neurosci Lett 306(3):189–192. https://doi.org/10.1016/S0304-3940(01)01907-3
Schuett S, Zihl J (2013) Does age matter? Age and rehabilitation of visual field disorders after brain injury. Cortex 49(4):1001–1012. https://doi.org/10.1016/j.cortex.2012.04.008
Alber R, Moser H, Gall C, Sabel BA (2017) Combined transcranial direct current stimulation and vision restoration training in subacute stroke rehabilitation: a pilot study. PM R 9(8):787–794. https://doi.org/10.1016/j.pmrj.2016.12.003
Kasten E, Wüst S, Behrens-Baumann W, Sabel BA (1998) Computer-based training for the treatment of partial blindness. Nat Med 4(9):1083–1087. https://doi.org/10.1038/2079
Kasten E, Poggel DA, Müller-Oehring E, Gothe J, Schulte T, Sabel BA (1999) Restoration of vision II: residual functions and training-induced visual field enlargement in brain-damaged patients. Restor Neurol Neurosci 15(2):273–287
Olma MC, Dargie RA, Behrens JR, Kraft A, Irlbacher K, Fahle M, Brandt SA (2013) Long-term effects of serial anodal tDCS on motion perception in subjects with occipital stroke measured in the unaffected visual hemifield. Front Hum Neurosci 7:314. https://doi.org/10.3389/fnhum.2013.00314
Moss AM, Harrison AR, Lee MS (2014) Patients with homonymous hemianopia become visually qualified to drive using novel monocular sector prisms. J Neuroophthalmol 34(1):53–56. https://doi.org/10.1097/WNO.0000000000000060
Nogaj S, Dubas K, Michalski A (2021) Efficacy of visual process improvement in patients with homonymous hemianopia. OphthaTherapy 8(1):26–30. https://doi.org/10.24292/01.OT.300321.4
Palomar-Mascaró FJ (2018) Rehabilitation of left homonymous hemianopia with adjacent palomar prism technique and visual therapy on line. J Intellect Disabil Diagn Treat 6(2):31–35. https://doi.org/10.6000/2292-2598.2018.06.02.1
Schuett S (2009) The rehabilitation of hemianopic dyslexia. Nat Rev Neurol 5(8):427–437. https://doi.org/10.1038/nrneurol.2009.97
Maher CG, Sherrington C, Herbert RD, Moseley AM, Elkins M (2003) Reliability of the PEDro scale for rating quality of randomized controlled trials. Phys Ther 83(8):713–721. https://doi.org/10.1093/ptj/83.8.713
Cashin AG, McAuley JH (2020) Clinimetrics: physiotherapy evidence database (PEDro) scale. J Physiother 66(1):59. https://doi.org/10.1016/j.jphys.2019.08.005
Trauzettel-Klosinski S, Brendler K (1998) Eye movements in reading with hemianopic field defects: the significance of clinical parameters. Graefe’s Arch Clin Exp Ophthalmol 236(2):91–102. https://doi.org/10.1007/s004170050048
Kasten E, Bunzenthal U, Sabel BA (2006) Visual field recovery after vision restoration therapy (VRT) is independent of eye movements: an eye tracker study. Behav Brain Res 175(1):18–26. https://doi.org/10.1016/j.bbr.2006.07.024
Burton R, Smith ND, Crabb DP (2014) Eye movements and reading in glaucoma: observations on patients with advanced visual field loss. Graefes Arch Clin Exp Ophthalmol 252(10):1621–1630. https://doi.org/10.1007/s00417-014-2752-x
Yu D, Cheung SH, Legge GE, Chung ST (2007) Effect of letter spacing on visual span and reading speed. J Vis 7(2):1–10. https://doi.org/10.1167/7.2.2
Luo D, Wan X, Liu J, Tong T (2016) Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat Methods Med Res 27(6):1785–1805. https://doi.org/10.1177/0962280216669183
Wan X, Wang W, Liu J, Tong T (2014) Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med Res Methodol 14:1–13. https://doi.org/10.1186/1471-2288-14-135
Bjelakovic G, Nikolova D, Gluud LL, Simonetti RG, Gluud C (2008) Mortality in randomized trials of antioxidant supplements for primary and secondary prevention: systematic review and meta-analysis. JAMA 297(8):842. https://doi.org/10.1001/jama.297.8.842
Martins D, Paduraru M, Paloyelis Y (2022) Heterogeneity in response to repeated intranasal oxytocin in schizophrenia and autism spectrum disorders: a meta-analysis of variance. Br J Pharmacol 179(8):1525–1543. https://doi.org/10.1111/bph.15451
Nelson HD, Vesco KK, Haney E, Fu R, Nedrow A, Miller J, Nicolaidis C, Walker M, Humphrey L (2006) Nonhormonal therapies for menopausal hot flashes: systematic review and meta-analysis. JAMA 295(17):2057. https://doi.org/10.1001/jama.295.17.2057
Higgins JPT, Green S, Cochrane Collaboration (2011) Table 7.7. a: Formulae for combining groups. Cochrane Handbook for Systematic Reviews of Interventions. Version, 5(0). https://handbook-5-1.cochrane.org/chapter_7/table_7_7_a_formulae_for_combining_groups.htm
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Kanda Y (2012) Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transplant 48(3):452–458. https://doi.org/10.1038/bmt.2012.244
Spitzyna GA, Wise RJ, McDonald SA, Plant GT, Kidd D, Crewes H, Leff AP (2007) Optokinetic therapy improves text reading in patients with hemianopic alexia: a controlled trial. Neurology 68(22):1922–1930. https://doi.org/10.1212/01.wnl.0000264002.30134.2a
Crotty M, van den Berg M, Hayes A, Chen C, Lange K, George S (2018) Hemianopia after stroke: a randomized controlled trial of the effectiveness of a standardised versus an individualized rehabilitation program, on scanning ability whilst walking1. NeuroRehabilitation 43(2):201–209. https://doi.org/10.3233/NRE-172377
Keller I, Lefin-Rank G (2010) Improvement of visual search after audiovisual exploration training in hemianopic patients. Neurorehabil Neural Repair 24(7):666–673. https://doi.org/10.1177/1545968310372774
Aimola L, Lane AR, Smith DT, Kerkhoff G, Ford GA, Schenk T (2014) Efficacy and feasibility of home-based training for individuals with homonymous visual field defects. Neurorehabil Neural Repair 28(3):207–218. https://doi.org/10.1177/1545968313503219
Schuett S, Heywood CA, Kentridge RW, Zihl J (2008) Rehabilitation of hemianopic dyslexia: are words necessary for re-learning oculomotor control? Brain 131(12):3156–3168. https://doi.org/10.1093/brain/awn285
Schuett S, Heywood CA, Kentridge RW, Dauner R, Zihl J (2012) Rehabilitation of reading and visual exploration in visual field disorders: transfer or specificity? Brain 135(3):912–921. https://doi.org/10.1093/brain/awr356
Zihl J, Kentridge RW, Pargent F, Heywood CA (2021) Aging and the rehabilitation of homonymous hemianopia: The efficacy of compensatory eye-movement training techniques and a five-year follow up. Aging Brain 1:100012. https://doi.org/10.1016/j.nbas.2021.100012
Kuester-Gruber S, Kabisch P, Cordey A, Karnath HO, Trauzettel-Klosinski S (2021) Training of vertical versus horizontal reading in patients with hemianopia - a randomized and controlled study. Graefes Arch Clin Exp Ophthalmol 259(3):745–757. https://doi.org/10.1007/s00417-020-04952-w
de Haan GA, Melis-Dankers BJ, Brouwer WH, Tucha O, Heutink J (2015) The effects of compensatory scanning training on mobility in patients with homonymous visual field defects: a randomized controlled trial. PLoS One. https://doi.org/10.1371/journal.pone.0134459
Roth T, Sokolov AN, Messias A, Roth P, Weller M, Trauzettel-Klosinski S (2009) Comparing explorative saccade and flicker training in hemianopia: a randomized controlled study. Neurology 72(4):324–331. https://doi.org/10.1212/01.wnl.0000341276.65721.f2
Elshout JA, van Asten F, Hoyng CB, Bergsma DP, van den Berg AV (2016) Visual rehabilitation in chronic cerebral blindness: a randomized controlled crossover study. Front Neurol 7:92. https://doi.org/10.3389/fneur.2016.00092
Mödden C, Behrens M, Damke I, Eilers N, Kastrup A, Hildebrandt H (2012) A randomized controlled trial comparing 2 interventions for visual field loss with standard occupational therapy during inpatient stroke rehabilitation. Neurorehabil Neural Repair 26(5):463–469. https://doi.org/10.1177/1545968311425927
Plow EB, Obretenova SN, Jackson ML, Merabet LB (2012) Temporal profile of functional visual rehabilitative outcomes modulated by transcranial direct current stimulation. Neuromodulation 15(4):367–373. https://doi.org/10.1111/j.1525-1403.2012.00440.x
Räty S, Borrmann C, Granata G, Cárdenas-Morales L, Schoenfeld A, Sailer M, Silvennoinen K, Holopainen J, De Rossi F, Antal A, Rossini PM, Tatlisumak T, Sabel BA (2021) Non-invasive electrical brain stimulation for vision restoration after stroke: an exploratory randomized trial (REVIS). Restor Neurol Neurosci 39(3):221–235. https://doi.org/10.3233/RNN-211198
Rowe FJ, Conroy EJ, Bedson E, Cwiklinski E, Drummond A, García-Fiñana M, Howard C, Pollock A, Shipman T, Dodridge C, MacIntosh C, Johnson S, Noonan C, Barton G, Sackley C (2017) A pilot randomized controlled trial comparing effectiveness of prism glasses, visual search training and standard care in hemianopia. Acta Neurol Scand 136(4):310–321. https://doi.org/10.1111/ane.12725
Choi W, Desai RH, Henderson JM (2014) The neural substrates of natural reading: a comparison of normal and nonword text using eyetracking and fMRI. Front Hum Neurosci 8:1024. https://doi.org/10.3389/fnhum.2014.01024
Kerkhoff G, Münßinger U, Haaf E, Eberle-Strauss G, Stögerer E (1992) Rehabilitation of homonymous scotomata in patients with postgeniculate damage of the visual system: saccadic compensation training. Restor Neurol Neurosci 4(4):245–254. https://doi.org/10.3233/RNN-1992-4402
Lane AR, Smith DT, Ellison A, Schenk T (2010) Visual exploration training is no better than attention training for treating hemianopia. Brain 133(6):1717–1728. https://doi.org/10.1093/brain/awq088
Pambakian AL, Mannan SK, Hodgson TL, Kennard C (2004) Saccadic visual search training: a treatment for patients with homonymous hemianopia. J Neurol Neurosurg Psychiatry 75(10):1443–1448. https://doi.org/10.1136/jnnp.2003.025957
McConkie GW, Rayner K (1975) The span of the effective stimulus during a fixation in reading. Percept psychophys 17(6):578–586. https://doi.org/10.3758/BF03203972
Higgins JPT, Green S (2011) 12.6. 2 re-expressing SMDs using rules of thumb for effect sizes. Cochrane Handbook for Systematic Reviews of Interventions. https://handbook-5-1.cochrane.org/chapter_12/12_6_2_re_expressing_smds_using_rules_of_thumb_for_effect_sizes.htm
Acknowledgements
The first author sincerely thanks Assistant Professor Hiroki Okada and Professor Shinya Sakai for their kind and detailed supervision from the research planning to the submission of the article, and Michiyo Kawamura and Moe Nemoto, Hokkaido University Library, for their help in creating search strategies. In addition, we thank Professor Alexander Leff for the kind answers to data requests.
Funding
The authors did not receive any financial support for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest relevant to this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Maeyama, T., Okada, H. & Sakai, S. The effects of rehabilitative interventions on reading disorders caused by homonymous visual field defects: a meta-analysis focusing on improvement in reading speed. Acta Neurol Belg 124, 123–140 (2024). https://doi.org/10.1007/s13760-023-02327-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-023-02327-6