Abstract
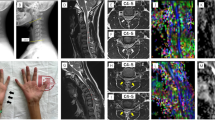
Limb-kinetic apraxia (LKA) is defined as an execution disorder of movements, resulting from injury of the corticofugal tract (CFT) from the secondary motor area. Diagnosis of LKA is difficult because it is made by clinical observation of movements. In this study, using diffusion tensor tractography (DTT), we attempted to investigate injury of the CFT from the secondary motor area in patients with corona radiata infarct. Twenty patients with corona radiata infarct were recruited. A probabilistic tractography method was used in fiber tracking for reconstruction of the corticospinal tract (CST) and CFT. Fractional anisotropy (FA), mean diffusivity, and tract volume of the CSTs and CFTs from the dorsal premotor cortex (dPMC) and supplementary motor area (SMA) were measured. In the affected hemisphere, FA values of the CST from the precentral hand knob and the CFT from the dPMC were significantly decreased compared with those of the unaffected hemisphere (p < 0.05). The tract volumes of the CST from the precentral hand knob and the CFTs from the dPMC and SMA in the affected hemisphere were also significantly decreased compared with those of the unaffected hemisphere (p < 0.05). We demonstrated concurrent injury of the CFTs from the secondary motor area along with injury of the CST in patients with corona radiata infarct, using DTT. Our results suggest that LKA ascribed to injury of the CFTs from the secondary motor area could be accompanied by injury of the CST ascribed to the corona radiata infarct.

Similar content being viewed by others
References
Leiguarda RC, Marsden CD (2000) Limb apraxias: higher-order disorders of sensorimotor integration. Brain 123(Pt 5):860–879
Ochipa C, Gonzalez Rothi LJ (2000) Limb apraxia. Semin Neurol 20(4):471–478. doi:10.1055/s-2000-13180
Heilman KM, Valenstein E (2003) Clinical neuropsychology, 4th edn. Oxford University Press, Oxford
Gross RG, Grossman M (2008) Update on apraxia. Curr Neurol Neurosci Rep 8(6):490–496
Heilman KM (2010) Apraxia. Continuum (Minneap Minn) 16(4 Behavioral Neurology):86–98. doi:10.1212/01.CON.0000368262.53662.08
Larner AJ (2001) A dictionary of neurological signs: clinical neurosemiology. Kluwer, Boston
Hong JH, Lee J, Cho YW, Byun WM, Cho HK, Son SM, Jang SH (2012) Limb apraxia in a patient with cerebral infarct: diffusion tensor tractography study. NeuroRehabilitation 30(4):255–259. doi:10.3233/NRE-2012-0753
Jang SH (2013) Motor recovery by improvement of limb-kinetic apraxia in a chronic stroke patient. NeuroRehabilitation 33(2):195–200. doi:10.3233/NRE-130945
Lee KC, Finley R, Miller B (2004) Apraxia of lid opening: dose-dependent response to carbidopa–levodopa. Pharmacotherapy 24(3):401–403
Yamada S, Matsuo K, Hirayama M, Sobue G (2004) The effects of levodopa on apraxia of lid opening: a case report. Neurology 62(5):830–831
Mori S, Crain BJ, Chacko VP, van Zijl PC (1999) Three-dimensional tracking of axonal projections in the brain by magnetic resonance imaging. Ann Neurol 45(2):265–269
Kunimatsu A, Aoki S, Masutani Y, Abe O, Hayashi N, Mori H, Masumoto T, Ohtomo K (2004) The optimal trackability threshold of fractional anisotropy for diffusion tensor tractography of the corticospinal tract. Magn Reson Med Sci 3(1):11–17
Newton JM, Ward NS, Parker GJ, Deichmann R, Alexander DC, Friston KJ, Frackowiak RS (2006) Non-invasive mapping of corticofugal fibres from multiple motor areas—relevance to stroke recovery. Brain 129(Pt 7):1844–1858. doi:10.1093/brain/awl106
Seo JP, Jang SH (2013) Different characteristics of the corticospinal tract according to the cerebral origin: DTI study. AJNR Am J Neuroradiol 34(7):1359–1363. doi:10.3174/ajnr.A3389
Jang SH (2014) The corticospinal tract from the viewpoint of brain rehabilitation. J Rehabil Med 46(3):193–199. doi:10.2340/16501977-1782
Jang SH, Kim K, Kim SH, Son SM, Jang WH, Kwon HG (2014) The relation between motor function of stroke patients and diffusion tensor imaging findings for the corticospinal tract. Neurosci Lett 572C:1–6. doi:10.1016/j.neulet.2014.04.044
Kwon HG, Yang JH, Park JB, Kim MH, Choi SH, Yang DS (2014) Anatomical location and somatotopic organization of the corticospinal tract in the corona radiata of the normal human brain: a diffusion tensor tractography study. NeuroReport 25(9):710–714. doi:10.1097/WNR.0000000000000170
Jang SH, Cho SH, Kim YH, You SH, Kim SH, Kim O, Yang DS, Son S (2005) Motor recovery mechanism of diffuse axonal injury: a combined study of transcranial magnetic stimulation and functional MRI. Restor Neurol Neurosci 23(1):51–56
Behrens TE, Johansen-Berg H, Woolrich MW, Smith SM, Wheeler-Kingshott CA, Boulby PA, Barker GJ, Sillery EL, Sheehan K, Ciccarelli O, Thompson AJ, Brady JM, Matthews PM (2003) Non-invasive mapping of connections between human thalamus and cortex using diffusion imaging. Nat Neurosci 6(7):750–757. doi:10.1038/nn1075
Smith SM, Jenkinson M, Woolrich MW, Beckmann CF, Behrens TE, Johansen-Berg H, Bannister PR, De Luca M, Drobnjak I, Flitney DE, Niazy RK, Saunders J, Vickers J, Zhang Y, De Stefano N, Brady JM, Matthews PM (2004) Advances in functional and structural MR image analysis and implementation as FSL. Neuroimage 23(Suppl 1):S208–S219. doi:10.1016/j.neuroimage.2004.07.051
Behrens TE, Berg HJ, Jbabdi S, Rushworth MF, Woolrich MW (2007) Probabilistic diffusion tractography with multiple fibre orientations: What can we gain? Neuroimage 34(1):144–155. doi:10.1016/j.neuroimage.2006.09.018
Jang SH (2011) Somatotopic arrangement and location of the corticospinal tract in the brainstem of the human brain. Yonsei Med J 52(4):553–557. doi:10.3349/ymj.2011.52.4.553
Hansen JT, Koeppen BM, Netter FH, Craig JA, Perkins J (2002) Atlas of Neuroanatomy and Neurophysiology: selections from the Netter Collection of Medical Illustrations. Icon Custom Communication. p 98
Mayka MA, Corcos DM, Leurgans SE, Vaillancourt DE (2006) Three-dimensional locations and boundaries of motor and premotor cortices as defined by functional brain imaging: a meta-analysis. Neuroimage 31(4):1453–1474. doi:10.1016/j.neuroimage.2006.02.004
Assaf Y, Pasternak O (2008) Diffusion tensor imaging (DTI)-based white matter mapping in brain research: a review. J Mol Neurosci 34(1):51–61. doi:10.1007/s12031-007-0029-0
Neil JJ (2008) Diffusion imaging concepts for clinicians. J Magn Reson Imaging 27(1):1–7. doi:10.1002/jmri.21087
Liepmann H (1920) Apraxie. Ergebn ges Med 1:516–543
Denes G, Mantovan MC, Gallana A, Cappelletti JY (1998) Limb-kinetic apraxia. Mov Disord 13(3):468–476. doi:10.1002/mds.870130316
Kwon H, Jang SH (2012) Delayed recovery of gait function in a patient with intracerebral haemorrhage. J Rehabil Med 44(4):378–380. doi:10.2340/16501977-0962
Borroni B, Garibotto V, Agosti C, Brambati SM, Bellelli G, Gasparotti R, Padovani A, Perani D (2008) White matter changes in corticobasal degeneration syndrome and correlation with limb apraxia. Arch Neurol 65(6):796–801. doi:10.1001/archneur.65.6.796
Wedeen VJ, Wang RP, Schmahmann JD, Benner T, Tseng WY, Dai G, Pandya DN, Hagmann P, D’Arceuil H, de Crespigny AJ (2008) Diffusion spectrum magnetic resonance imaging (DSI) tractography of crossing fibers. Neuroimage 41(4):1267–1277. doi:10.1016/j.neuroimage.2008.03.036
Yamada K, Sakai K, Akazawa K, Yuen S, Nishimura T (2009) MR tractography: a review of its clinical applications. Magn Reson Med Sci 8(4):165–174
Acknowledgments
This work was supported by the Medical Research Center Program (2015R1A5A2009124) through the National Research Foundation of Korea (NRF) funded by the Ministry of Science, ICT and Future Planning.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Standard
The authors declare that they acted in accordance with ethical standards laid down in the 1964 Declaration of Helsinki.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Jang, S.H., Seo, J.P. Limb-kinetic apraxia due to injury of corticofugal tracts from secondary motor area in patients with corona radiata infarct. Acta Neurol Belg 116, 467–472 (2016). https://doi.org/10.1007/s13760-016-0600-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13760-016-0600-y