Abstract
Objective
Radiotherapy (RT) effectively palliates symptomatic spinal metastases; however, both radiation myelopathy (RM) and disease progression are concerns following re-irradiation (re-RT). Limited published data suggest a low RM risk if the total biologically effective dose (BED) is ≤135.5 Gy, re-treatment interval is ≥6 months, and each course’s BED is ≤98 Gy. RM risk groups have been proposed; however, few data inform disease and RM outcomes after re-RT respecting these criteria. This study investigates these outcomes following re-RT for spinal metastases after publication of the aforementioned RM criteria.
Methods
Patients followed at a single institution after palliative spinal re-RT (C1-L2) from January 2008 to November 2013 were identified. Chart review assessed RM criteria, risk groups, and disease progression. BEDs were calculated using the linear quadratic model.
Results
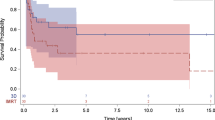
Fifty-three patients underwent re-RT to a median cumulative BED of 126.8 Gy (range 48.0–157.8) with a median re-treatment interval of 19.3 months (range 1.0–197.6). No courses had a BED ≥98 Gy. After a median follow-up of 4.1 months (range 0.2–124.9) for all (n = 53) and 11.5 months (range 1.6–29.4) for surviving (n = 12) patients, no RM was observed. The median survival following re-RT was 5.5 months (range 0.5–125.3). Fourteen patients progressed locally (14/53; 26.4 %); all developed varying degrees of irreversible neurologic injury.
Conclusion
Patients undergoing re-RT for spinal metastases have a poor prognosis. No RM was observed after re-RT largely respecting published low-risk criteria. Neurologic injury from progression was common. Further study of exceeding the low-risk criteria, particularly among poor prognosis patients, may be warranted.

Similar content being viewed by others
References
Kaloostian PE, Yurter A, Zadnik PL, Sciubba DM, Gokaslan ZL (2014) Current paradigms for metastatic spinal disease: an evidence-based review. Ann Surg Oncol 21(1):248–262. doi:10.1245/s10434-013-3324-8
Howell DD, James JL, Hartsell WF, Suntharalingam M, Machtay M, Suh JH, Demas WF, Sandler HM, Kachnic LA, Berk LB (2013) Single-fraction radiotherapy versus multifraction radiotherapy for palliation of painful vertebral bone metastases-equivalent efficacy, less toxicity, more convenient: a subset analysis of Radiation Therapy Oncology Group trial 97–14. Cancer 119(4):888–896. doi:10.1002/cncr.27616
Rades D, Stalpers LJ, Veninga T, Schulte R, Hoskin PJ, Obralic N, Bajrovic A, Rudat V, Schwarz R, Hulshof MC, Poortmans P, Schild SE (2005) Evaluation of five radiation schedules and prognostic factors for metastatic spinal cord compression. J Clin Oncol 23(15):3366–3375. doi:10.1200/JCO.2005.04.754
Chow E, Zeng L, Salvo N, Dennis K, Tsao M, Lutz S (2012) Update on the systematic review of palliative radiotherapy trials for bone metastases. Clin Oncol 24(2):112–124. doi:10.1016/j.clon.2011.11.004
Wong CS, Van Dyke J, Milosevic M, Laperriere NJ (1994) Radiation myelopathy following single courses of radiotherapy and retreatment. Int J Radiat Oncol Biol Phys 30(3):575–581
Fairchild A, Barnes E, Ghosh S, Ben-Josef E, Roos D, Hartsell W, Holt T, Wu J, Janjan N, Chow E (2009) International patterns of practice in palliative radiotherapy for painful bone metastases: evidence-based practice? Int J Radiat Oncol Biol Phys 75(5):1501–1510. doi:10.1016/j.ijrobp.2008.12.084
Chia SK, Speers CH, D'Yachkova Y, Kang A, Malfair-Taylor S, Barnett J, Coldman A, Gelmon KA, O'Reilly SE, Olivotto IA (2007) The impact of new chemotherapeutic and hormone agents on survival in a population-based cohort of women with metastatic breast cancer. Cancer 110(5):973–979. doi:10.1002/cncr.22867
Johnson DH, Schiller JH, Bunn PA Jr (2014) Recent clinical advances in lung cancer management. J Clin Oncol. doi:10.1200/JCO.2013.53.1228
Antonarakis ES, Eisenberger MA (2011) Expanding treatment options for metastatic prostate cancer. N Engl J Med 364(21):2055–2058. doi:10.1056/NEJMe1102758
Schultheiss TR, Stephens LC (1992) Permanent radiation myelopathy. Br J Radiol 65:737–753
Nieder C, Grosu AL, Andratschke NH, Molls M (2005) Proposal of human spinal cord reirradiation dose based on collection of data from 40 patients. Int J Radiat Oncol Biol Phys 61(3):851–855. doi:10.1016/j.ijrobp.2004.06.016
Nieder C, Grosu AL, Andratschke NH, Molls M (2006) Update of human spinal cord reirradiation tolerance based on additional data from 38 patients. Int J Radiat Oncol Biol Phys 66(5):1446–1449. doi:10.1016/j.ijrobp.2006.07.1383
Rades D, Stalpers LJ, Veninga T, Hoskin PJ (2005) Spinal reirradiation after short-course RT for metastatic spinal cord compression. Int J Radiat Oncol Biol Phys 63(3):872–875. doi:10.1016/j.ijrobp.2005.03.034
Rades D, Stalpers LJ, Veninga T, Schulte R, Hoskin PJ, Alberti W (2005) Effectiveness and toxicity of reirradiation (Re-RT) for metastatic spinal cord compression (MSCC). Strahlenther Onkol 181(9):595–600. doi:10.1007/s00066-005-1406-7
Oken MM, Creech RH, Tormey DC, Horton J, Davis TE, McFadden ET, Carbone PP (1982) Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol 5(6):649–655
Fowler JF (1989) The linear-quadratic formula and progress in fractionated radiotherapy. Br J Radiol 62(740):679–694
Singh R, Al-Hallaq H, Pelizzari CA, Zagaja GP, Chen A, Jani AB (2003) Dosimetric quality endpoints for low-dose-rate prostate brachytherapy using biological effective dose (BED) vs. conventional dose. Med Dosim 28(4):255–259. doi:10.1016/j.meddos.2003.04.001
Kaplan E, Meier P (1958) Nonparametric estimation from incomplete observations. J Am Stat Assoc 53:457–481
R Development Core Team (2013) R: a language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing, 2013. http://www.R-project.org/
Siegel R, Ma J, Zou Z, Jemal A (2014) Cancer statistics, 2014. CA Cancer J Clin 64(1):9–29. doi:10.3322/caac.21208
Chow E, Abdolell M, Panzarella T, Harris K, Bezjak A, Warde P, Tannock I (2008) Predictive model for survival in patients with advanced cancer. J Clin Oncol 26(36):5863–5869. doi:10.1200/JCO.2008.17.1363
Chow E, Davis L, Panzarella T, Hayter C, Szumacher E, Loblaw A, Wong R, Danjoux C (2005) Accuracy of survival prediction by palliative radiation oncologists. Int J Radiat Oncol Biol Phys 61(3):870–873. doi:10.1016/j.ijrobp.2004.07.697
Gripp S, Moeller S, Bolke E, Schmitt G, Matuschek C, Asgari S, Asgharzadeh F, Roth S, Budach W, Franz M, Willers R (2007) Survival prediction in terminally ill cancer patients by clinical estimates, laboratory tests, and self-rated anxiety and depression. J Clin Oncol 25(22):3313–3320. doi:10.1200/JCO.2006.10.5411
Krishnan MS, Epstein-Peterson Z, Chen YH, Tseng YD, Wright AA, Temel JS, Catalano P, Balboni TA (2014) Predicting life expectancy in patients with metastatic cancer receiving palliative radiotherapy: the TEACHH model. Cancer 120(1):134–141. doi:10.1002/cncr.28408
Tseng YD, Krishnan MS, Sullivan AJ, Jones JA, Chow E, Balboni TA (2013) How radiation oncologists evaluate and incorporate life expectancy estimates into the treatment of palliative cancer patients: a survey-based study. Int J Radiat Oncol Biol Phys 87(3):471–478. doi:10.1016/j.ijrobp.2013.06.2046
Garg AK, Wang XS, Shiu AS, Allen P, Yang J, McAleer MF, Azeem S, Rhines LD, Chang EL (2011) Prospective evaluation of spinal reirradiation by using stereotactic body radiation therapy: the University of Texas MD Anderson Cancer Center experience. Cancer 117(15):3509–3516. doi:10.1002/cncr.25918
Mahadevan A, Floyd S, Wong E, Jeyapalan S, Groff M, Kasper E (2011) Stereotactic body radiotherapy reirradiation for recurrent epidural spinal metastases. Int J Radiat Oncol Biol Phys 81(5):1500–1505. doi:10.1016/j.ijrobp.2010.08.012
Sahgal A, Ma L, Weinberg V, Gibbs IC, Chao S, Chang UK, Werner-Wasik M, Angelov L, Chang EL, Sohn MJ, Soltys SG, Letourneau D, Ryu S, Gerszten PC, Fowler J, Wong CS, Larson DA (2012) Reirradiation human spinal cord tolerance for stereotactic body radiotherapy. Int J Radiat Oncol Biol Phys 82(1):107–116. doi:10.1016/j.ijrobp.2010.08.021
Haley ML, Gerszten PC, Heron DE, Chang YF, Atteberry DS, Burton SA (2011) Efficacy and cost-effectiveness analysis of external beam and stereotactic body radiation therapy in the treatment of spine metastases: a matched-pair analysis. J Neurosurg Spine 14(4):537–542. doi:10.3171/2010.12.SPINE10233
Chow E, van der Linden YM, Roos D, Hartsell WF, Hoskin P, Wu JSY, Brundage MD, Nabid A, Tissing-Tan CJA, Oei B, Babington S, Demas WF, Wilson CF, Meyer RM, Chen BE, Wong RKS (2014) Single versus multiple fractions of repeat radiation for painful bone metastases: a randomised, controlled, non-inferiority trial. Lancet Oncol 15(2):164–171. doi:10.1016/s1470-2045(13)70556-4
Acknowledgments
This study received the following financial support for the research, authorship, and/or publication of this article: American Society of Clinical Oncology Conquer Cancer Foundation Career Development Award (T.A.B...).
Conflict of interest
Matthew D. Cheney, M.D., Ph.D., Tai-Chung Lam, M.D., Hajime Uno, Ph.D., Barbara A. Jaehn, B.S., Antonio L. Damato, Ph.D., Monica Krishnan, M.D., and Tracy A. Balboni, M.D., M.P.H., confirm that they have no conflicts of interest.
Ethical standards
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Declaration of 1975 as revised in 2008. Informed consent was obtained from all patients included in the study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cheney, M.D., Lam, TC., Uno, H. et al. Outcomes after palliative re-irradiation of spinal metastases. J Radiat Oncol 4, 157–162 (2015). https://doi.org/10.1007/s13566-015-0192-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13566-015-0192-9