Abstract
Purpose
Metastasis of lung adenocarcinoma (LADC) is a crucial factor determining patient survival. Repurposing of the antipsychotic agent penfluridol has been found to be effective in the inhibition of growth of various cancers. As yet, however, the anti-metastatic effect of penfluridol on LADC has rarely been investigated. Herein, we addressed the therapeutic potential of penfluridol on the invasion/metastasis of LADC cells harboring different epidermal growth factor receptor (EGFR) mutation statuses.
Methods
MTS viability, transwell migration and invasion, and tumor endothelium adhesion assays were employed to determine cytotoxic and anti-metastatic effects of penfluridol on LADC cells. Protease array, Western blot, immunohistochemistry (IHC), immunofluorescence (IF) staining, and expression knockdown by shRNA or exogenous overexpression by DNA plasmid transfection were performed to explore the underlying mechanisms, both in vitro and in vivo.
Results
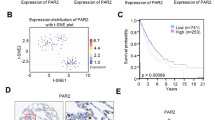
We found that nontoxic concentrations of penfluridol reduced the migration, invasion and adhesion of LADC cells. Protease array screening identified matrix metalloproteinase-12 (MMP-12) as a potential target of penfluridol to modulate the motility and adhesion of LADC cells. In addition, we found that MMP-12 exhibited the most significantly adverse prognostic effect in LADC among 39 cancer types. Mechanistic investigations revealed that penfluridol inhibited the urokinase plasminogen activator (uPA)/uPA receptor/transforming growth factor-β/Akt axis to downregulate MMP-12 expression and, subsequently, reverse MMP-12-induced epithelial–mesenchymal transition (EMT). Subsequent analysis of clinical LADC samples revealed a positive correlation between MMP12 and mesenchymal-related gene expression levels. A lower survival rate was found in LADC patients with a SNAl1high/MMP12high profile compared to those with a SNAl1low/MMP12low profile.
Conclusions
Our results indicate that MMP-12 may serve as a useful biomarker for predicting LADC progression and as a promising penfluridol target for treating metastatic LADC.






Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this article and its supplemental files.
Abbreviations
- BM:
-
basement membrane
- ECM:
-
extracellular matrix
- EMT:
-
epithelial–mesenchymal transition
- GEO:
-
Gene Expression Omnibus
- KM plotter:
-
Kaplan–Meier plotter
- LADC:
-
lung adenocarcinoma
- MMP:
-
matrix metalloproteinase
- NSCLC:
-
non-small cell lung cancer
- SCC:
-
squamous cell carcinoma
- TCGA:
-
The Cancer Genome Atlas
- TGF-β:
-
transforming growth factor-β
- uPA:
-
urokinase plasminogen activator
- uPAR:
-
uPA receptor
- WT:
-
wild-type
References
B.Y. Wang, J.Y. Huang, C.Y. Cheng, C.H. Lin, J. Ko, Y.P. Liaw, Lung cancer and prognosis in taiwan: a population-based cancer registry. J. Thorac. Oncol. 8, 1128–1135 (2013)
D.M. Jackman, Y. Zhang, C. Dalby, T. Nguyen, J. Nagle, C.A. Lydon, M.S. Rabin, K.K. McNiff, B. Fraile, J.O. Jacobson, Cost and survival analysis before and after implementation of Dana-Farber clinical pathways for patients with stage IV non-small-cell lung cancer. J. Oncol. Pract. 13, e346–e352 (2017)
L. Qiao, J. Wang, G. Long, Y. Jiang, Sequential treatment of tyrosine kinase inhibitor and platinum-based doublet chemotherapy on EGFR mutant non-small cell lung cancer: a meta-analysis of randomized controlled clinical trials. Onco. Targets Ther. 10, 1279–1284 (2017)
S. Brassart-Pasco, S. Brezillon, B. Brassart, L. Ramont, J.B. Oudart, J.C. Monboisse, Tumor microenvironment: Extracellular matrix alterations influence tumor progression. Front. Oncol. 10, 397 (2020)
S Blanco-Prieto, L Barcia-Castro, M Paez, FJ de la Cadena, L Rodriguez-Berrocal, MI Vazquez-Iglesias, A Botana-Rial, L Fernandez-Villar, De Chiara, Relevance of matrix metalloproteases in non-small cell lung cancer diagnosis. BMC Cancer 17, 823 (2017)
S.D. Shapiro, D.K. Kobayashi, T.J. Ley, Cloning and characterization of a unique elastolytic metalloproteinase produced by human alveolar macrophages. J. Biol. Chem. 268, 23824–23829 (1993)
P Qu, H Du, X Wang, C Yan, Matrix metalloproteinase 12 overexpression in lung epithelial cells plays a key role in emphysema to lung bronchioalveolar adenocarcinoma transition. Cancer Res. 69, 7252–7261 (2009)
P Qu, C Yan, H Du, Matrix metalloproteinase 12 overexpression in myeloid lineage cells plays a key role in modulating myelopoiesis, immune suppression, and lung tumorigenesis. Blood 117, 4476–4489 (2011)
H.S. Hofmann, G. Hansen, G. Richter, C. Taege, A. Simm, R.E. Silber, S. Burdach, Matrix metalloproteinase-12 expression correlates with local recurrence and metastatic disease in non-small cell lung cancer patients. Clin. Cancer Res. 11, 1086–1092 (2005)
F.Z. Lv, J.L. Wang, Y. Wu, H.F. Chen, X.Y. Shen, Knockdown of MMP12 inhibits the growth and invasion of lung adenocarcinoma cells. Int. J. Immunopathol. Pharmacol. 28, 77–84 (2015)
NH Cho, KP Hong, SH Hong, S Kang, KY Chung, SH Cho, MMP expression profiling in recurred stage IB lung cancer. Oncogene 23, 845–851 (2004)
V Mittal, Epithelial mesenchymal transition in aggressive lung cancers. Adv. Exp. Med. Biol. 890, 37–56 (2016)
M.L. Stallings-Mann, J. Waldmann, Y. Zhang, E. Miller, M.L. Gauthier, D.W. Visscher, G.P. Downey, E.S. Radisky, A.P. Fields, D.C. Radisky, Matrix metalloproteinase induction of Rac1b, a key effector of lung cancer progression. Sci. Transl. Med. 4, 142ra195 (2012)
S Singhal, J Mehta, R Desikan, D Ayers, P Roberson, P Eddlemon, N Munshi, E Anaissie, C Wilson, M Dhodapkar, J Zeddis, B Barlogie, Antitumor activity of thalidomide in refractory multiple myeloma. N. Engl. J. Med. 341, 1565–1571 (1999)
MJ Thun, SJ Henley, C Patrono, Nonsteroidal anti-inflammatory drugs as anticancer agents: mechanistic, pharmacologic, and clinical issues. J. Natl. Cancer Inst. 94, 252–266 (2002)
V. Shafiei-Irannejad, N. Samadi, R. Salehi, B. Yousefi, N. Zarghami, New insights into antidiabetic drugs: Possible applications in cancer treatment. Chem. Biol. Drug Des. 90, 1056–1066 (2017)
F.H. Chou, K.Y. Tsai, C.Y. Su, C.C. Lee, The incidence and relative risk factors for developing cancer among patients with schizophrenia: a nine-year follow-up study. Schizophr. Res. 129, 97–103 (2011)
B.G. Soares, M.S. Lima, Penfluridol for schizophrenia. Cochrane Database Syst. Rev. Cd002923 (2006)
V. Shaw, S. Srivastava, S.K. Srivastava, Repurposing antipsychotics of the diphenylbutylpiperidine class for cancer therapy. Semin. Cancer Biol. 68, 75–83 (2021)
N.M. Tuan, C.H. Lee, Penfluridol as a candidate of drug repurposing for anticancer agent. Molecules 24, 3659 (2019)
WY Hung, JH Chang, Y Cheng, GZ Cheng, HC Huang, M Hsiao, CL Chung, WJ Lee, MH Chien, Autophagosome accumulation-mediated ATP energy deprivation induced by penfluridol triggers nonapoptotic cell death of lung cancer via activating unfolded protein response. Cell Death Dis. 10, 538 (2019)
A Ranjan, P Gupta, SK Srivastava, Penfluridol: an antipsychotic agent suppresses metastatic tumor growth in triple-negative breast cancer by inhibiting integrin signaling axis. Cancer Res. 76, 877–890 (2016)
H Kim, K Chong, BK Ryu, KJ Park, MO Yu, J Lee, S Chung, S Choi, MJ Park, YG Chung, SH Kang, Repurposing penfluridol in combination with temozolomide for the treatment of glioblastoma. Cancers 11, 1310 (2019)
YH Yu, HA Chen, PS Chen, YJ Cheng, WH Hsu, YW Chang, YH Chen, Y Jan, M Hsiao, TY Chang, YH Liu, YM Jeng, CH Wu, MT Huang, YH Su, MC Hung, MH Chien, CY Chen, ML Kuo, JL Su, MiR-520h-mediated FOXC2 regulation is critical for inhibition of lung cancer progression by resveratrol. Oncogene 32, 431–443 (2013)
Y.W. Lin, L.M. Lee, W.J. Lee, C.Y. Chu, P. Tan, Y.C. Yang, W.Y. Chen, S.F. Yang, M. Hsiao, M.H. Chien, Melatonin inhibits MMP-9 transactivation and renal cell carcinoma metastasis by suppressing Akt-MAPKs pathway and NF-κB DNA-binding activity. J. Pineal. Res. 60, 277–290 (2016)
MH Chien, WJ Lee, YC Yang, P Tan, KF Pan, YC Liu, HC Tsai, CH Hsu, YC Wen, M Hsiao, Hua, N-alpha-acetyltransferase 10 protein promotes metastasis by stabilizing matrix metalloproteinase-2 protein in human osteosarcomas. Cancer Lett. 433, 86–98 (2018)
F.A. Venning, L. Wullkopf, J.T. Erler, Targeting ECM disrupts cancer progression. Front. Oncol. 5, 224 (2015)
C. Gialeli, A.D. Theocharis, N.K. Karamanos, Roles of matrix metalloproteinases in cancer progression and their pharmacological targeting. FEBS J 278, 16–27 (2011)
A.J. Gentles, A.M. Newman, C.L. Liu, S.V. Bratman, W. Feng, D. Kim, V.S. Nair, Y. Xu, A. Khuong, C.D. Hoang, M. Diehn, R.B. West, S.K. Plevritis, A.A. Alizadeh, The prognostic landscape of genes and infiltrating immune cells across human cancers. Nat. Med. 21, 938–945 (2015)
JF Santibanez, H Obradovic, T Kukolj, J Krstic, Transforming growth factor-beta, matrix metalloproteinases, and urokinase-type plasminogen activator interaction in the cancer epithelial to mesenchymal transition. Dev. Dyn. 247, 382–395 (2018)
SL Raza, LC Nehring, SD Shapiro, LA Cornelius, Proteinase-activated receptor-1 regulation of macrophage elastase (MMP-12) secretion by serine proteinases. J. Biol. Chem. 275, 41243–41250 (2000)
G Qin, M Luo, J Chen, Y Dang, G Chen, L Li, J Zeng, Y Lu, J Yang, Reciprocal activation between MMP-8 and TGF-beta1 stimulates EMT and malignant progression of hepatocellular carcinoma. Cancer Lett. 374, 85–95 (2016)
X. Zhu, L. Wang, B. Zhang, J. Li, X. Dou, R.C. Zhao, TGF-beta1-induced PI3K/Akt/NF-kappaB/MMP9 signalling pathway is activated in Philadelphia chromosome-positive chronic myeloid leukaemia hemangioblasts. J. Biochem. 149, 405–414 (2011)
L.J. Talbot, S.D. Bhattacharya, P.C. Kuo, Epithelial-mesenchymal transition, the tumor microenvironment, and metastatic behavior of epithelial malignancies. Int. J. Biochem. Mol. Biol. 3, 117–136 (2012)
LM Machesky, Lamellipodia and filopodia in metastasis and invasion. FEBS Lett. 582, 2102–2111 (2008)
J. Dong, B. Zhai, W. Sun, F. Hu, H. Cheng, J. Xu, Activation of phosphatidylinositol 3-kinase/AKT/snail signaling pathway contributes to epithelial-mesenchymal transition-induced multi-drug resistance to sorafenib in hepatocellular carcinoma cells. PLoS One 12, e0185088 (2017)
C. Scheau, I.A. Badarau, R. Costache, C. Caruntu, G.L. Mihai, A.C. Didilescu, C. Constantin, M. Neagu, The role of matrix metalloproteinases in the epithelial-mesenchymal transition of hepatocellular carcinoma. Anal. Cell Pathol. (Amst.) 2019, 9423907 (2019)
SA Illman, K Lehti, J Keski-Oja, J Lohi, Epilysin (MMP-28) induces TGF-beta mediated epithelial to mesenchymal transition in lung carcinoma cells. J. Cell Sci. 119, 3856–3865 (2006)
J. Cathcart, A. Pulkoski-Gross, J. Cao, Targeting matrix metalloproteinases in cancer: Bringing new life to old ideas. Genes Dis. 2, 26–34 (2015)
G.J. Boelen, L. Boute, J. d’Hoop, M. EzEldeen, I. Lambrichts, G. Opdenakker, Matrix metalloproteinases and inhibitors in dentistry. Clin. Oral. Investig. 23, 2823–2835 (2019)
W. Xu, Z. Yang, N. Lu, A new role for the PI3K/Akt signaling pathway in the epithelial-mesenchymal transition. Cell Adh. Migr. 9, 317–324 (2015)
S Julien, I Puig, E Caretti, J Bonaventure, L Nelles, F van Roy, C Dargemont, AG de Herreros, A Bellacosa, L Larue, Activation of NF-kappaB by Akt upregulates Snail expression and induces epithelium mesenchyme transition. Oncogene 26, 7445–7456 (2007)
A. Miyoshi, Y. Kitajima, K. Sumi, K. Sato, A. Hagiwara, Y. Koga, K. Miyazaki, Snail and SIP1 increase cancer invasion by upregulating MMP family in hepatocellular carcinoma cells. Br. J. Cancer 90, 1265–1273 (2004)
K. Yokoyama, N. Kamata, R. Fujimoto, S. Tsutsumi, M. Tomonari, M. Taki, H. Hosokawa, M. Nagayama, Increased invasion and matrix metalloproteinase-2 expression by Snail-induced mesenchymal transition in squamous cell carcinomas. Int. J. Oncol. 22, 891–898 (2003)
J.H. Chang, C.W. Cheng, Y.C. Yang, W.S. Chen, W.Y. Hung, J.M. Chow, P.S. Chen, M. Hsiao, W.J. Lee, M.H. Chien, Downregulating CD26/DPPIV by apigenin modulates the interplay between Akt and Snail/Slug signaling to restrain metastasis of lung cancer with multiple EGFR statuses. J. Exp. Clin. Cancer Res. 37, 199 (2018)
J.H. Chang, S.L. Lai, W.S. Chen, W.Y. Hung, J.M. Chow, M. Hsiao, W.J. Lee, M.H. Chien, Quercetin suppresses the metastatic ability of lung cancer through inhibiting Snail-dependent Akt activation and Snail-independent ADAM9 expression pathways. Biochim. Biophys. Acta Mol. Cell Res. 1864, 1746–1758 (2017)
X. Xiao, Z. He, W. Cao, F. Cai, L. Zhang, Q. Huang, C. Fan, C. Duan, X. Wang, J. Wang, Y. Liu, Oridonin inhibits gefitinib-resistant lung cancer cells by suppressing EGFR/ERK/MMP-12 and CIP2A/Akt signaling pathways. Int. J. Oncol. 48, 2608–2618 (2016)
L Wu, A Tanimoto, Y Murata, T Sasaguri, J Fan, Y Sasaguri, T Watanabe, Matrix metalloproteinase-12 gene expression in human vascular smooth muscle cells. Genes Cells 8, 225–234 (2003)
L Li, L Qi, Z Liang, W Song, Y Liu, Y Wang, B Sun, B Zhang, W Cao, Transforming growth factor-β1 induces EMT by the transactivation of epidermal growth factor signaling through HA/CD44 in lung and breast cancer cells. Int. J. Mol. Med. 36, 113–122 (2015)
S. Mazhar, S.E. Taylor, J. Sangodkar, G. Narla, Targeting PP2A in cancer: Combination therapies. Biochim. Biophys. Acta Mol. Cell Res. 1866, 51–63 (2019)
S.Y. Wu, Y.C. Wen, C.C. Ku, Y.C. Yang, J.M. Chow, S.F. Yang, W.J. Lee, M.H. Chien, Penfluridol triggers cytoprotective autophagy and cellular apoptosis through ROS induction and activation of the PP2A-modulated MAPK pathway in acute myeloid leukemia with different FLT3 statuses. J. Biomed. Sci. 26, 63 (2019)
E Hedrick, X Li, S Safe, Penfluridol represses integrin expression in breast cancer through induction of reactive oxygen species and downregulation of Sp transcription factors. Mol. Cancer Ther. 16, 205–216 (2017)
Acknowledgements
We thank the National RNAi Core Facility, Academia Sinica (Taipei, Taiwan) for providing shRNAs. We also thank Dr. Tsang-Chih Kuo and Dr. Ching-Chow Chen (National Taiwan University, Taipei, Taiwan) for offering the Snail- and Slug-overexpression plasmids and the myr-Akt plasmid, respectively.
Funding
This study was supported by the Taipei Medical University Research Center of Cancer Translational Medicine from The Featured Areas Research Center Program within the framework of the Higher Education Sprout Project by the Ministry of Education in Taiwan (to M.-H. Chien). This study was also supported by a grant (110-eva-14) from Wan Fang Hospital, Taipei Medical University (to J.-H. Chang).
Author information
Authors and Affiliations
Contributions
Conceptualization, M-HC, J-HC and W-YH; methodology, W-JL, G-ZC, C-HT, Y-CY, T-CL and J-QC; writing, original draft preparation, M-HC, J-HC and C-LC; writing, review and editing, M-HC and W-YH. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that no competing interests exist.
Ethics approval and consent to participate
All animal experiments were carried out in accordance with guidelines of a protocol approved by the Taipei Medical University Animal Ethics Research Board.
Consent for publication
Not applicable.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 657 KB)
Rights and permissions
About this article
Cite this article
Hung, WY., Lee, WJ., Cheng, GZ. et al. Blocking MMP-12-modulated epithelial-mesenchymal transition by repurposing penfluridol restrains lung adenocarcinoma metastasis via uPA/uPAR/TGF-β/Akt pathway. Cell Oncol. 44, 1087–1103 (2021). https://doi.org/10.1007/s13402-021-00620-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-021-00620-1