Abstract
Aims
This cohort study investigated the association between treatment cessation and incidence/progression of diabetic retinopathy (DR) in Japanese patients with type 2 diabetes mellitus (T2DM).
Materials and methods
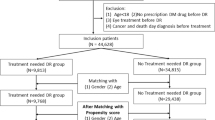
Data were extracted from electronic medical records at the University of the Ryukyu Hospital and the Tomishiro Central Hospital of Okinawa, Japan. We enrolled 417 diabetic patients without DR (N = 281) and with nonproliferative DR (N = 136) at the baseline. Treatment cessation was defined as failing to attend outpatient clinics for at least twelve months prior to the baseline. After a median follow-up of 7 years, we compared the incidence/progression rate of DR including nonproliferative and proliferative DR between patients with and without treatment cessation and calculated the odds ratio (OR) in the treatment cessation group using a logistic regression model.
Results
The overall prevalence of treatment cessation was 13% in patients with T2DM. Characteristics of treatment cessation included relative youth (57 ± 11 years vs. 63 ± 12 years, P < 0.01). Treatment cessation was tightly associated with the incidence of DR (OR 4.20 [95% confidence interval [CI] 1.46–12.04, P < 0.01) and also incidence/progression of DR (OR 2.70 [1.28–5.69], P < 0.01), even after adjusting for age, sex, BMI, duration of T2DM, and HbA1c level.
Conclusions
By considering major confounding factors, the present study demonstrates an independent association between treatment cessation and incidence of DR in patients with T2DM, highlighting treatment cessation as an independent risk for DR in T2DM.


Similar content being viewed by others
Data availability
The data that support the findings of this study are available on request from the corresponding author.
References
Yau JW, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Wong TY, et al. Meta-Analysis for Eye Disease (META-EYE) Study Group. Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012;35:556–64.
Solomon SD, Chew E, Duh EJ, Sobrin L, Sun JK, Gardner TW, et al. Diabetic retinopathy: a position statement by the American Diabetes Association. Diabetes Care. 2017;40:412–8.
Lin KY, Hsih WH, Lin YB, Wen CY, Chang TJ. Update in the epidemiology, risk factors, screening, and treatment of diabetic retinopathy. J Diabetes Investig. 2021;12:1322–5.
Jones CD, Greenwood RH, Misra A, Bachmann MO. Incidence and progression of diabetic retinopathy during 17 years of a population-based screening program in England. Diabetes Care. 2012;35:592–6.
Davies MJ, Aroda VR, Collins BS, Gabbay RA, Green J, Buse JB, et al. Management of hyperglycaemia in type 2 diabetes. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetologia. 2022;65:1925–66.
Griffin SJ. Lost to follow-up: the problem of defaulters from diabetes clinics. Diabet Med. 1998;15(Suppl 3):14–24.
Brewster S, Bartholomew J, Holt RIG, Price H. Non-attendance at diabetes outpatient appointments: a systematic review. Diabet Med. 2020;37:1427–42.
Sun CA, Taylor K, Levin S, Renda SM, Han HR. Factors associated with missed appointments by adults with type 2 diabetes mellitus: a systematic review. BMJ Open Diabetes Res Care. 2021;9: e001819.
Masding MG, Klejdys S, MacHugh B, Gale S, Brown A, McAulay A. Non-attendance at a diabetes transitional clinic and glycaemic control. Pract Diabetes Int. 2010;27:109–10.
McCarlie J, Anderson A, Collier A, Jaap A, McGettrick P, MacPherson N. Who missed routine diabetic review? Information from a district diabetes register. Pract Diabetes Int. 2002;19:283–6.
Garcia Diaz E, Ramirez Medina D, Garcia Lopez A, Morera Porras OM. Determinants of adherence to hypoglycemic agents and medical visits in patients with type 2 diabetes mellitus. Endocrinol Diabetes Nutr. 2017;64:531–8.
Low SK, Khoo JK, Tavintharan S, Lim SC, Sum CF. Missed appointments at a diabetes centre: not a small problem. Ann Acad Med Singapore. 2016;45:1–5.
Karter AJ, Parker MM, Moffet HH, Ahmed AT, Ferrara A, Liu JY, et al. Missed appointments and poor glycemic control: an opportunity to identify high-risk diabetic patients. Med Care. 2004;42:110–5.
Akhter K, Dockray S, Simmons D. Exploring factors influencing non-attendance at the diabetes clinic and service improvement strategies from patients’ perspectives. Pract Diabetes. 2012;29:113–6.
Alvarez C, Saint-Pierre C, Herskovic V, Sepulveda M. Analysis of the relationship between the referral and evolution of patients with type 2 diabetes mellitus. Int J Environ Res Pub Health. 2018;15:1534.
Campbell-Richards D. Exploring diabetes non-attendance: an inner London perspective. J Diabetes Nurs. 2016;20:73–8.
Snow R, Fulop N. Understanding issues associated with attending a young adult diabetes clinic: A case study. Diabet Med. 2012;29:257–9.
Ngwenya BT, Van Zyl DG, Webb EM. Factors influencing nonattendance of clinic appointments in diabetic patients at a Gauteng hospital in 2007/2008. J Endocrinol Metab Diabetes S Africa. 2009;14:106–9.
Heydarabadi AB, Mehr HM, Nouhjah S. Why rural diabetic patients do not attend for scheduled appointments: Results of a qualitative study. Diabetes Metab Syndr. 2017;11:989–95.
Vijayaraghavan S, O’Shea T, Campbell-Richards D, Sudra R, Morris J, Byrne E, et al. DAWN: Diabetes Appointments via Webcam in Newham. Br J Diabetes Vasc Dis. 2015;15:123–6.
Wilson SJ, Greenhalgh S. Keeping in touch with young people—where have all the DNA’ers gone? Pract Diabetes Int. 1999;16:87–8.
Hardy KJ, O’Brien SV, Furlong NJ. Information given to patients before appointments and its effect on non-attendance rate. BMJ. 2001;323:1298–300.
Weaver KR, Talley M, Mullins M, Selleck C. Evaluating patient navigation to improve first appointment no-show rates in uninsured patients with diabetes. J Community Health Nurs. 2019;36:11–8.
Horny M, Glover W, Gupte G, Saraswat A, Vimalananda V, Rosenzweig J. Patient navigation to improve diabetes outpatient care at a safety-net hospital: a retrospective cohort study. BMC Health Serv Res. 2017;17:759.
Ho ET. Improving waiting time and operational clinic flow in a tertiary diabetes center. BMJ Qual Imp Rep. 2014. https://doi.org/10.1136/bmjquality.u201918.w1006.
Currie CJ, Peyrot M, Morgan CL, Poole CD, Jenkins-Jones S, Evans M, et al. The impact of treatment noncompliance on mortality in people with type 2 diabetes. Diabetes Care. 2012;35:1279–84.
Hammersley MS, Holland MR, Walford S, Thorn PA. What happens to defaulters from a diabetic clinic? Br Med J (Clin Res Ed). 1985;291:1330–2.
Simpson SH, Eurich DT, Majumdar SR, Padwal RS, Tsuyuki RT, Johnson JA, et al. A meta-analysis of the association between adherence to drug therapy and mortality. BMJ. 2006;333:15.
Wilkinson CP, Ferris FL III, Klein RE, Lee PP, Agardh CD, et al. Proposed international clinical diabetic retinopathy and diabetic macular edema disease severity scales. Ophthalmology. 2003;110:1677–82.
Chew EY, Ambrosius WT, Davis MD, Danis RP, Gangaputra S. Effects of medical therapies on retinopathy progression in type 2 diabetes. N Engl J Med. 2010;363:233–44.
Agardh E, Tababat-Khani P. Adopting 3-Year screening intervals for sight-threatening retinal vascular lesions in type 2 diabetic subjects without retinopathy. Diabetes Care. 2011;34:1318–9.
Archibald LK, Gill GV. Diabetic clinic defaulters—who are they and why do they default? Practical Diabetes International. 1992;9:13–4.
Kawasaki R, Tanaka S, Tanaka S, Yamamoto T, Sone H, Ohashi Y, et al. Japan Diabetes Complications Study Group. Incidence and progression of diabetic retinopathy in Japanese adults with type 2 diabetes: 8 year follow-up study of the Japan Diabetes Complications Study (JDCS). Diabetologia. 2011;54:2288–94.
Laiteerapong N, Ham SA, Gao Y, Moffet HH, Liu JY, Karter AJ, et al. The legacy effect in type 2 diabetes: impact of early glycemic control on future complications (the diabetes & aging study). Diabetes Care. 2019;42:416–26.
Takao T, Matsuyama Y, Suka M, Yanagisawa H, Kasuga M. Analysis of the duration and extent of the legacy effect in patients with type 2 diabetes: a real-world longitudinal study. J Diabetes Complications. 2019;33:516–22.
Pothen L, Balligand JL. Legacy in Cardiovascular risk factors control: from theory to future therapeutic strategies? Antioxidants. 2021;22(10):1849.
Folz R, Laiteerapong N. The legacy effect in diabetes: are there long-term benefits? Diabetologia. 2021;64:2131–7.
Jin J, Wang X, Zhi X, Meng D. Epigenetic regulation in diabetic vascular complications. J Mol Endocrinol. 2019;63:103–15.
Ceriello A. Hypothesis: the “metabolic memory”, the new challenge of diabetes. Diabetes Res Clin Pract. 2009;86:2–6.
Ceriello A, Ihnat MA, Thorpe JE. Clinical review 2: The “metabolic memory”: is more than just tight glucose control necessary to prevent diabetic complications? J Clin Endocrinol Metab. 2009;94:410–5.
Simó R, Franch-Nadal J, Vlacho B, Real J, Amado E, Flores J, et al. Rapid reduction of HbA1c and early worsening of diabetic retinopathy: a real-world population-based study in subjects with type 2 diabetes. Diabetes Care. 2023;46:1633–9.
Feldman-Billard S, Larger É, Massin P. Standards for screening and surveillance of ocular complications in people with diabetes SFD study group. Early worsening of diabetic retinopathy after rapid improvement of blood glucose control in patients with diabetes. Diabetes Metab. 2018;44:4–14.
Bain SC, Klufas MA, Ho A, Matthews DR. Worsening of diabetic retinopathy with rapid improvement in systemic glucose control: a review. Diabetes Obes Metab. 2019;21:454–66.
Kim NH, Choi J, Kim NH, Choi KM, Baik SH, Lee J, et al. Dipeptidyl peptidase-4 inhibitor use and risk of diabetic retinopathy: a population-based study. Diabetes Metab. 2018;44:361–7.
Graber AL, Davidson P, Brown AW, McRae JR, Woolridge K. Dropout and relapse during diabetes care. Diabetes Care. 1992;15:1477–83.
Benoit SR, Ji M, Fleming R, Philis-Tsimikas A. Predictors of dropouts from a San Diego diabetes program: a case control study. Prev Chronic Dis. 2004;1:10.
Sone H, Kawai K, Takagi H, Yamada N, Kobayashi M. Outcome of one-year of specialist care of patients with type 2 diabetes: a multi-center prospective survey. Intern Med. 2006;45:589–97.
Kawahara R, Amemiya T, Yoshino M, Miyamae M, Sasamoto K. Dropout of young non-insulin-dependent diabetics from diabetes care. Diabetes Res Clin Pract. 1994;24:181–5.
Acknowledgements
This work was supported in part by Council for Science, Technology and Innovation (CSTI), Cross-Ministerial Strategic Innovation Promotion Program (SIP), “Technologies for Creating Next-Generation Agriculture, Forestry and Fisheries,” New Energy and Industrial Technology Development Organization (NEDO), and Construction of the Okinawa Science & Technology Innovation System. We are also grateful to T. Ikematsu, M. Hirata, and C. Noguchi for excellent secretarial assistance.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study’s conception and design. Material preparations were performed by Yoshiro Nakayama, Moritake Higa, Hideki Koizumi, Michio Shimabukuro, and Hiroaki Masuzaki, data collections were performed by Yoshiro Nakayama and Moritake Higa, and analyses were performed by Yukiko Shinzato, Yoshiro Nakayama, Tsugumi Uema, Hideki Koizumi, Michio Shimabukuro, Koshi Nakamura, and Hiroaki Masuzaki. The first draft of the manuscript was written by Yukiko Shinzato, Yoshiro Nakayama, Jasmine F Millman, Michio Shimabukuro, and Hiroaki Masuzaki, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest to disclose.
Ethical approval
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation (The Ethics Committee of University of the Ryukyus for Medical and Health Research Involving Human Subjects (No.765) on February 27, 2015) and with the Helsinki Declaration of 1964 and later versions. Informed consent or substitute for it was obtained from all patients for being included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
About this article
Cite this article
Shinzato, Y., Nakayama, Y., Okamoto, S. et al. Impact of treatment cessation on incidence and progression of retinopathy in Japanese patients with type 2 diabetes mellitus: a retrospective cohort study. Diabetol Int (2024). https://doi.org/10.1007/s13340-024-00724-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13340-024-00724-7