Abstract
Objective
To determine breastmilk sodium changes in the first 72 hours after birth and to correlate maternal and neonatal variables with maternal breastmilk sodium.
Methods
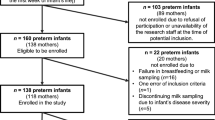
We enrolled 245 mothers and their exclusively breast-fed neonates in this prospective cohort study. Singleton, inborn babies of greater than 34 weeks gestation, who were exclusively breastfed for the first 72 hours were included. Babies who required neonatal intensive care unit (NICU) admission, top up feeds or discharged before 72 hours were excluded. Study outcomes were changes in breast milk sodium in the first 72 hours and association of high maternal breast milk sodium with various maternal and neonatal variables.
Results
Mean (SD) breastmilk sodium steadily declined over the first 72 hours [53.5 (19.2), 38.5 (19.0) and 22.2 (10.6) mmol/L at 24, 48, 72 hours, respectively]. Breastfeeding ≤8 times per 24 hours in the first three days was the only factor significantly associated with high breastmilk sodium (P=0.008). Maternal age, gravida, mode of delivery, significant neonatal weight loss, hypernatremia, neonatal morbidities like fever, irritability, lethargy and poor suck had no significant correlation with high breastmilk sodium.
Conclusion
Breastmilk sodium shows a steady decline in the first 72 hours after delivery. Feeding ≤8 times per day is associated high breastmilk sodium at 72 hours of age.
Similar content being viewed by others
References
Koo WW, Gupta JM. Breast milk sodium. Arch Dis Child. 1982;57:500–2.
Evans K, Evans R, Royal R, Esterman A, James S. Effect of caesarean section on breast milk transfer to the normal term newborn over the first week of life. Arch Dis Child Fetal Neonatal Ed. 2003;88:F380–2.
Sofer S, Ben-Ezer D, Dagan R. Early severe dehydration in young breast-fed newborn infants. Isr J Med Sci. 1993;29:85–9.
Anand SK, Sandborg C, Robinson RG, Lieberman E. Neonatal hypernatremia associated with elevated sodium concentration ofbreast milk. J Pediatr. 1980;96:66–8.
Neville MC, Morton J, Umemura S. Lactogenesis. The transition from pregnancy to lactation. Pediatr Clin North Am. 2001;48:35–52.
Morton JA. The clinical usefulness ofbreast milk sodium in the assessment of lactogenesis. Pediatrics. 1994;93:802–6.
Heldrich FJ, Shaw SS. Case report and review of literature: hypernatremia in breast-fed infants. Md Med J. 1990;39:475–8.
Manganaro R, Marseglia L, Mami C, et al. Breast milk sodium concentration, sodium intake and weight loss in breast-feeding newborn infants. Br J Nutr. 2007;97:344–8.
Neville MC, Morton J. Physiology and endocrine changes underlying human lactogenesis II. J Nutr. 2001;131:3005S–8S.
Neville MC, Allen JC, Archer PC, et al. Studies in human lactation: Milk volume and nutrient composition during weaning and lactogenesis. Am J Clin Nutr. 1991;54:81–92.
Galipeau R, Goulet C, Chagnon M. Infant and maternal factors influencing breastmilk sodium among primiparous mothers. Breastfeed Med. 2012;7:290–4.
Narayan S, Natarajan N, Bawa K. Maternal and neonatal factors adversely affecting breastfeeding in the perinatal period. Med J Armed Forces India. 2005;61:216–9.
Scott JA, Binns CW, Oddy WH. Predictors of delayed onset of lactation. Matern Child Nutr. 2007;3:186–93.
Krishnamurthy S, Debnath S, Gupta P. Breast feeding-associated hypernatremic dehydration: A preventable tragedy in newborn infants. JCR 2011;1:1–5.
Bilgin LK, Akcay F, Altinkaynak K, Altindag H. Hypernatremia in breastfed newborns: A review of 149 cases. J Trop Pediatr. 2012;58:332–4.
Author information
Authors and Affiliations
Corresponding author
Additional information
Ethics clearance
Ethics Committee of Pondicherry Institute of Medical Sciences; No. IEC RC/14/65; dated 30 September, 2014.
Contributors
All authors approved the final version of manuscript, and are accountable for all aspects related to the study.
Funding
None
Competing interests
None stated.
Rights and permissions
About this article
Cite this article
Mathew, M.V., Kumar K, P.P., Sivaa, R. et al. Relationship of Maternal and Neonatal Variables With Breastmilk Sodium. Indian Pediatr 58, 741–744 (2021). https://doi.org/10.1007/s13312-021-2283-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-021-2283-6