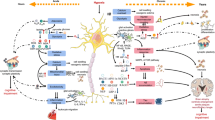
Abstract
Acidic postconditioning by transient CO2 inhalation applied within minutes after reperfusion has neuroprotective effects in the acute phase of stroke. However, the effects of delayed chronic acidic postconditioning (DCAPC) initiated during the subacute phase of stroke or other acute brain injuries are unknown. Mice received daily DCAPC by inhaling 5%/10%/20% CO2 for various durations (three cycles of 10- or 20-min CO2 inhalation/10-min break) at days 3–7, 7–21, or 3–21 after photothrombotic stroke. Grid-walk, cylinder, and gait tests were used to assess motor function. DCAPC with all CO2 concentrations significantly promoted motor functional recovery, even when DCAPC was delayed for 3–7 days. DCAPC enhanced the puncta density of GAP-43 (a marker of axon growth and regeneration) and synaptophysin (a marker of synaptogenesis) and reduced the amoeboid microglia number, glial scar thickness and mRNA expression of CD16 and CD32 (markers of proinflammatory M1 microglia) compared with those of the stroke group. Cerebral blood flow (CBF) increased in response to DCAPC. Furthermore, the mRNA expression of TDAG8 (a proton-activated G-protein-coupled receptor) was increased during the subacute phase of stroke, while DCAPC effects were blocked by systemic knockout of TDAG8, except for those on CBF. DCAPC reproduced the benefits by re-expressing TDAG8 in the peri-infarct cortex of TDAG8-/- mice infected with HBAAV2/9-CMV-TDAG8-3flag-ZsGreen. Taken together, we first showed that DCAPC promoted functional recovery and brain tissue repair after stroke with a wide therapeutic time window of at least 7 days after stroke. Brain-derived TDAG8 is a direct target of DCAPC that induces neuroreparative effects.






Similar content being viewed by others
Data Availability
All data generated or analyzed during this study are included in this published article.
References
Xiong Y, Wakhloo A, Fisher M. Advances in acute ischemic stroke therapy. Circ Res. 2022;130(8):1230–51. https://doi.org/10.1161/CIRCRESAHA.121.319948.
Langhorne P, Bernhardt J, Kwakkel G. Stroke rehabilitation. Lancet (London, England). 2011;377(9778):1693–702. https://doi.org/10.1016/S0140-6736(11)60325-5.
Hugues N, Pellegrino C, Rivera C, Berton E, Pin-Barre C, Laurin J. Is high-intensity interval training suitable to promote neuroplasticity and cognitive functions after stroke? Int J Mol Sci. 2021;22(6):3003. https://doi.org/10.3390/ijms22063003.
Wang J, Liu H, Chen S, Zhang W, Chen Y, Yang Y. Moderate exercise has beneficial effects on mouse ischemic stroke by enhancing the functions of circulating endothelial progenitor cell-derived exosomes. Exp Neurol. 2020;330:113325. https://doi.org/10.1016/j.expneurol.2020.113325.
Sun H, Li A, Hou T, Tao X, Chen M, Wu C, et al. Neurogenesis promoted by the cd200/cd200r signaling pathway following treadmill exercise enhances post-stroke functional recovery in rats. Brain Behav Immun. 2019;82:354–71. https://doi.org/10.1016/j.bbi.2019.09.005.
Al Shoyaib A, Alamri F, Biggers A, Karamyan S, Arumugam T, Ahsan F, et al. Delayed exercise-induced upregulation of angiogenic proteins and recovery of motor function after photothrombotic stroke in mice. Neuroscience. 2021;461:57–71. https://doi.org/10.1016/j.neuroscience.2021.02.023.
Zhao H, Sapolsky R, Steinberg G. Interrupting reperfusion as a stroke therapy: ischemic postconditioning reduces infarct size after focal ischemia in rats. J Cereb Blood Flow Metab. 2006;26(9):1114–21. https://doi.org/10.1038/sj.jcbfm.9600348.
Zhao H. Hurdles to clear before clinical translation of ischemic postconditioning against stroke. Transl Stroke Res. 2013;4(1):63–70. https://doi.org/10.1007/s12975-012-0243-0.
Fan Y, Hu W, Nan F, Chen Z. Postconditioning-induced neuroprotection, mechanisms and applications in cerebral ischemia. Neurochem Int. 2017;107:43–56. https://doi.org/10.1016/j.neuint.2017.01.006.
Ripley A, Jeffers M, McDonald M, Montroy J, Dykes A, Fergusson D, et al. Neuroprotection by remote ischemic conditioning in rodent models of focal ischemia: a systematic review and meta-analysis. Transl Stroke Res. 2021;12(3):461–73. https://doi.org/10.1007/s12975-020-00882-1.
Li C, Ma W, Liu K, Yang J, Wang X, Wu Z, et al. Advances in intervention methods and brain protection mechanisms of in situ and remote ischemic postconditioning. Metab Brain Dis. 2021;36(1):53–65. https://doi.org/10.1007/s11011-020-00562-x.
Fan Y, Shen Z, He P, Jiang L, Hou W, Shen Y, et al. A novel neuroprotective strategy for ischemic stroke: transient mild acidosis treatment by co2 inhalation at reperfusion. J Cereb Blood Flow Metab. 2014;34(2):275–83. https://doi.org/10.1038/jcbfm.2013.193.
Shen Z, Zheng Y, Wu J, Chen Y, Wu X, Zhou Y, et al. Park2-dependent mitophagy induced by acidic postconditioning protects against focal cerebral ischemia and extends the reperfusion window. Autophagy. 2017;13(3):473–85. https://doi.org/10.1080/15548627.2016.1274596.
Tsai Y, Yang Y, Wang P, Wang R. Intermittent hypoxia after transient focal ischemia induces hippocampal neurogenesis and c-fos expression and reverses spatial memory deficits in rats. PloS One. 2011;6(8):e24001. https://doi.org/10.1371/journal.pone.0024001.
Tsai Y, Yang Y, Sun S, Liang K, Wang R. Post ischemia intermittent hypoxia induces hippocampal neurogenesis and synaptic alterations and alleviates long-term memory impairment. J Cereb Blood Flow Metab. 2013;33(5):764–73. https://doi.org/10.1038/jcbfm.2013.15.
Zhao Z, Hood R, Ong L, Pietrogrande G, Sanchez Bezanilla S, Warren K, et al. Exploring how low oxygen post conditioning improves stroke-induced cognitive impairment: a consideration of amyloid-beta loading and other mechanisms. Front Neurol. 2021;12:585189. https://doi.org/10.3389/fneur.2021.585189.
Doeppner T, Zechmeister B, Kaltwasser B, Jin F, Zheng X, Majid A, et al. Very delayed remote ischemic post-conditioning induces sustained neurological recovery by mechanisms involving enhanced angioneurogenesis and peripheral immunosuppression reversal. Front Cell Neurosci. 2018;12:383. https://doi.org/10.3389/fncel.2018.00383.
Okajima F. Regulation of inflammation by extracellular acidification and proton-sensing gpcrs. Cell Signal. 2013;25(11):2263–71. https://doi.org/10.1016/j.cellsig.2013.07.022.
Choi J, Lee S, Choi Y. Identification of a putative g protein-coupled receptor induced during activation-induced apoptosis of t cells. Cell Immunol. 1996;168(1):78–84. https://doi.org/10.1006/cimm.1996.0051.
McGuire J, Herman J, Ghosal S, Eaton K, Sallee F, Sah R. Acid-sensing by the t cell death-associated gene 8 (tdag8) receptor cloned from rat brain. Biochem Biophys Res Commun. 2009;386(3):420–5. https://doi.org/10.1016/j.bbrc.2009.05.133.
Mogi C, Tobo M, Tomura H, Murata N, He X, Sato K, et al. Involvement of proton-sensing tdag8 in extracellular acidification-induced inhibition of proinflammatory cytokine production in peritoneal macrophages. J Immunol. 2009;182(5):3243–51. https://doi.org/10.4049/jimmunol.0803466.
Onozawa Y, Fujita Y, Kuwabara H, Nagasaki M, Komai T, Oda T. Activation of t cell death-associated gene 8 regulates the cytokine production of t cells and macrophages in vitro. Eur J Pharmacol. 2012;683(1-3):325–31. https://doi.org/10.1016/j.ejphar.2012.03.007.
Jin Y, Sato K, Tobo A, Mogi C, Tobo M, Murata N, et al. Inhibition of interleukin-1β production by extracellular acidification through the tdag8/camp pathway in mouse microglia. J Neurochem. 2014;129(4):683–95. https://doi.org/10.1111/jnc.12661.
Ma X, Hang L, Shao D, Shu W, Hu X, Luo H. Tdag8 activation attenuates cerebral ischaemia-reperfusion injury via akt signalling in rats. Exp Neurol. 2017;293:115–23. https://doi.org/10.1016/j.expneurol.2017.03.023.
Sato K, Tobo A, Mogi C, Tobo M, Yamane N, Tosaka M, et al. The protective role of proton-sensing tdag8 in the brain injury in a mouse ischemia reperfusion model. Sci Rep. 2020;10(1):17193. https://doi.org/10.1038/s41598-020-74372-7.
Lin Y, Dong J, Tang Y, Ni H, Zhang Y, Su P, et al. Opening a new time window for treatment of stroke by targeting hdac2. J Neurosci. 2017;37(28):6712–28. https://doi.org/10.1523/JNEUROSCI.0341-17.2017.
Pietrogrande G, Zalewska K, Zhao Z, Johnson S, Nilsson M, Walker F. Low oxygen post conditioning as an efficient non-pharmacological strategy to promote motor function after stroke. Transl Stroke Res. 2019;10(4):402–12. https://doi.org/10.1007/s12975-018-0656-5.
Fan Y, Wang Y, Guo J, Wu M, Zhang M, Niu B, et al. Delayed metformin treatment improves functional recovery following traumatic brain injury via central ampk-dependent brain tissue repair. Brain Res Bull. 2020;164:146–56. https://doi.org/10.1016/j.brainresbull.2020.08.021.
McDonald M, Dykes A, Jeffers M, Carter A, Nevins R, Ripley A, et al. Remote ischemic conditioning and stroke recovery. Neurorehabil Neural Repair. 2021;35(6):545–9. https://doi.org/10.1177/15459683211011224.
Leconte C, Tixier E, Freret T, Toutain J, Saulnier R, Boulouard M, et al. Delayed hypoxic postconditioning protects against cerebral ischemia in the mouse. Stroke. 2009;40(10):3349–55. https://doi.org/10.1161/STROKEAHA.109.557314.
Yang X, Shi X, Ju J, Zhang W, Liu Y, Li X, et al. 5% CO2 inhalation suppresses hyperventilation-induced absence seizures in children. Epilepsy Res. 2014;108(2):345–8. https://doi.org/10.1016/j.eplepsyres.2013.11.012.
Papassin J, Heck O, Condamine E, Pietras J, Detante O, Krainik A. Impaired cerebrovascular reactivity is associated with recurrent stroke in patients with severe intracranial arterial stenosis: A CO2 bold fmri study. J Neuroradiol. 2021;48(5):339–45. https://doi.org/10.1016/j.neurad.2020.04.005.
Wang T, Zhou G, He M, Xu Y, Rusyniak W, Xu Y, et al. Gpr68 is a neuroprotective proton receptor in brain ischemia. Stroke. 2020;51(12):3690–700. https://doi.org/10.1161/STROKEAHA.120.031479.
Xu Y, Casey G. Identification of human ogr1, a novel g protein-coupled receptor that maps to chromosome 14. Genomics. 1996;35(2):397–402. https://doi.org/10.1006/geno.1996.0377.
Wenzel J, Hansen C, Bettoni C, Vogt M, Lembrich B, Natsagdorj R, et al. Impaired endothelium-mediated cerebrovascular reactivity promotes anxiety and respiration disorders in mice. Proc Natl Acad Sci U S A. 2020;117(3):1753–61. https://doi.org/10.1073/pnas.1907467117.
Zha X, Xiong Z, Simon R. Ph and proton-sensitive receptors in brain ischemia. J Cereb Blood Flow Metab. 2022;42(8):1349–63. https://doi.org/10.1177/0271678X221089074.
Thompson S. Reactivity of cerebral blood flow to CO2 in patients with transient cerebral ischemic attacks. Stroke. 1971;2(3):273–8. https://doi.org/10.1161/01.str.2.3.273.
Caldwell H, Carr J, Minhas J, Swenson E, Ainslie P. Acid-base balance and cerebrovascular regulation. J Physiol. 2021;599(4):5337–59. https://doi.org/10.1113/JP281517.
Pekna M, Pekny M, Nilsson M. Modulation of neural plasticity as a basis for stroke rehabilitation. Stroke. 2012;43(10):2819–28. https://doi.org/10.1161/STROKEAHA.112.654228.
Benowitz L, Routtenberg A. Gap-43: an intrinsic determinant of neuronal development and plasticity. Trends Neurosci. 1997;20(2):84–91. https://doi.org/10.1016/s0166-2236(96)10072-2.
Allegra Mascaro A, Cesare P, Sacconi L, Grasselli G, Mandolesi G, Maco B, et al. In vivo single branch axotomy induces gap-43-dependent sprouting and synaptic remodeling in cerebellar cortex. Proc Natl Acad Sci U S A. 2013;110(26):10824–9. https://doi.org/10.1073/pnas.1219256110.
Masliah E, Fagan A, Terry R, DeTeresa R, Mallory M, Gage F. Reactive synaptogenesis assessed by synaptophysin immunoreactivity is associated with gap-43 in the dentate gyrus of the adult rat. Exp Neurol. 1991;113(2):131–42. https://doi.org/10.1016/0014-4886(91)90169-d.
Wang C, Wu Y, Zhang Q, Yu K, Wang Y. An enriched environment promotes synaptic plasticity and cognitive recovery after permanent middle cerebral artery occlusion in mice. Neural Regen Res. 2019;14(3):462–9. https://doi.org/10.4103/1673-5374.245470.
Shen L, Li Y, Gao Q, Savant-Bhonsale S, Chopp M. Down-regulation of neurocan expression in reactive astrocytes promotes axonal regeneration and facilitates the neurorestorative effects of bone marrow stromal cells in the ischemic rat brain. Glia. 2008;56(16):1747–54. https://doi.org/10.1002/glia.20722.
Shin J, Lim S, Jeong S, Kang J, Park E. Noggin improves ischemic brain tissue repair and promotes alternative activation of microglia in mice. Brain Behav Immun. 2014;40:143–54. https://doi.org/10.1016/j.bbi.2014.03.013.
Lindvall O, Kokaia Z. Neurogenesis following stroke affecting the adult brain. Cold Spring Harb Perspect Biol. 2015;7(11):a019034. https://doi.org/10.1101/cshperspect.a019034.
Huang L, Zhang L. Neural stem cell therapies and hypoxic-ischemic brain injury. Prog Neurobiol. 2019;173:1–17. https://doi.org/10.1016/j.pneurobio.2018.05.004.
Hu X, Li P, Guo Y, Wang H, Leak R, Chen S, et al. Microglia/macrophage polarization dynamics reveal novel mechanism of injury expansion after focal cerebral ischemia. Stroke. 2012;43(11):3063–70. https://doi.org/10.1161/STROKEAHA.112.659656.
Perego C, Fumagalli S, De Simoni M. Temporal pattern of expression and colocalization of microglia/macrophage phenotype markers following brain ischemic injury in mice. J Neuroinflammation. 2011;8:174. https://doi.org/10.1186/1742-2094-8-174.
Raffaele S, Gelosa P, Bonfanti E, Lombardi M, Castiglioni L, Cimino M, et al. Microglial vesicles improve post-stroke recovery by preventing immune cell senescence and favoring oligodendrogenesis. Mol Ther. 2021;29(4):1439–58. https://doi.org/10.1016/j.ymthe.2020.12.009.
Lian L, Zhang Y, Liu L, Yang L, Cai Y, Zhang J, et al. Neuroinflammation in ischemic stroke: focus on microrna-mediated polarization of microglia. Front Mol Neurosci. 2020;13:612439. https://doi.org/10.3389/fnmol.2020.612439.
Rossi D, Brady J, Mohr C. Astrocyte metabolism and signaling during brain ischemia. Nat Neurosci. 2007;10(11):1377–86. https://doi.org/10.1038/nn2004.
Zamanian J, Xu L, Foo L, Nouri N, Zhou L, Giffard R, et al. Genomic analysis of reactive astrogliosis. J Neurosci. 2012;32(18):6391–410. https://doi.org/10.1523/JNEUROSCI.6221-11.2012.
Li Y, Chopp M, Zhang Z, Zhang R. Expression of glial fibrillary acidic protein in areas of focal cerebral ischemia accompanies neuronal expression of 72-kda heat shock protein. J Neurol Sci. 1995;128(2):134–42. https://doi.org/10.1016/0022-510x(94)00228-g.
Liao R, Jiang L, Wang R, Zhao H, Chen Y, Li Y, et al. Histidine provides long-term neuroprotection after cerebral ischemia through promoting astrocyte migration. Sci Rep. 2015;5:15356. https://doi.org/10.1038/srep15356.
Yiu G, He Z. Glial inhibition of cns axon regeneration. Nat Rev Neurosci. 2006;7(8):617–27. https://doi.org/10.1038/nrn1956.
Vollmer L, Ghosal S, McGuire J, Ahlbrand R, Li K, Santin J, et al. Microglial acid sensing regulates carbon dioxide-evoked fear. Biol Psychiatry. 2016;80(7):541–51. https://doi.org/10.1016/j.biopsych.2016.04.022.
Bortell N, Basova L, Semenova S, Fox H, Ravasi T, Marcondes M. Astrocyte-specific overexpressed gene signatures in response to methamphetamine exposure in vitro. J Neuroinflammation. 2017;14(1):49. https://doi.org/10.1186/s12974-017-0825-6.
Funding
This work was sponsored by the National Natural Science Foundation of China (81872854, 81202520), the Open Fund from the Key Laboratory of Cellular Physiology (Shanxi Medical University, KLCP2019), and the Fund for Shanxi “1331 Project” Key Subjects Construction.
Author information
Authors and Affiliations
Contributions
Conceptualization: Yan-Ying Fan, Ming-Sheng Zhang; methodology: Yu Li, Xiao-Ying Tian, Ying-Jing Wang, Bao-Lu Guo, Jing Huo, Ru Chen, Hui-Feng Zhang; data curation: Yan-Ying Fan, Yan Li, Cai-Hong Yang; formal analysis and investigation: Yan-Ying Fan, Yan Li, Cai-Hong Yang; writing—original draft preparation: Yan-Ying Fan; writing—review and editing: Bao-Long Niu and Ming-Sheng Zhang; funding acquisition: Yan-Ying Fan.
Corresponding authors
Ethics declarations
Ethics Approval
All procedures on animals were approved by the Institutional Animal Care and Use Committee at Shanxi Medical University and conformed to the National Institutes of Health Guide for the Care and Use of Laboratory Animals.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fan, YY., Li, Y., Tian, XY. et al. Delayed Chronic Acidic Postconditioning Improves Poststroke Motor Functional Recovery and Brain Tissue Repair by Activating Proton-Sensing TDAG8. Transl. Stroke Res. (2023). https://doi.org/10.1007/s12975-023-01143-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12975-023-01143-7