Abstract
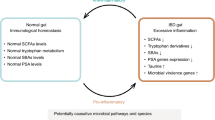
Inflammatory bowel disease (IBD) is a result of chronic inflammation caused, in some part, by dysbiosis of intestinal microbiota, mainly commensal bacteria. Gut dysbiosis can be caused by multiple factors, including abnormal immune responses which might be related to genetic susceptibility, infection, western dietary habits, and administration of antibiotics. Consequently, the disease itself is characterized as having multiple causes, etiologies, and severities. Recent studies have identified >200 IBD risk loci in the host. It has been postulated that gut microbiota interact with these risk loci resulting in dysbiosis, and this subsequently leads to the development of IBD. Typical gut microbiota in IBD patients are characterized with decrease in species richness and many of the commensal, and beneficial, fecal bacteria such as Firmicutes and Bacteroidetes and an increase or bloom of Proteobacteria. However, at this time, cause and effect relationships have not been rigorously established. While treatments of IBD usually includes medications such as corticosteroids, 5-aminosalicylates, antibiotics, immunomodulators, and anti-TNF agents, restoration of gut dysbiosis seems to be a safer and more sustainable approach. Bacteriotherapies (now called microbiota therapies) and dietary interventions are effective way to modulate gut microbiota. In this review, we summarize factors involved in IBD and studies attempted to treat IBD with probiotics. We also discuss the potential use of microbiota therapies as one promising approach in treating IBD. As therapies based on the modulation of gut microbiota becomes more common, future studies should include individual gut microbiota differences to develop personalized therapy for IBD.
Similar content being viewed by others
References
Abraham, B.P. and Quigley, E.M.M. 2017. Probiotics in inflammatory bowel disease. Gastroenterol. Clin. North Am. 46, 769–782.
Ahmad, R., Chaturvedi, R., Olivares-Villagomez, D., Habib, T., Asim, M., Shivesh, P., Polk, D.B., Wilson, K.T., Washington, M.K., Van Kaer, L., et al. 2014. Targeted colonic claudin-2 expression renders resistance to epithelial injury, induces immune suppression, and protects from colitis. Mucosal Immunol. 7, 1340–1353.
Ale, M.T., Mikkelsen, J.D., and Meyer, A.S. 2011. Important determinants for fucoidan bioactivity: a critical review of structurefunction relations and extraction methods for fucose-containing sulfated polysaccharides from brown seaweeds. Mar. Drugs 9, 2106–2130.
Ananthakrishnan, A.N. 2015. Environmental risk factors for inflammatory bowel diseases: a review. Dig. Dis. Sci. 60, 290–298.
Andrianifahanana, M., Moniaux, N., and Batra, S.K. 2006. Regulation of mucin expression: mechanistic aspects and implications for cancer and inflammatory diseases. Biochim. Biophys. Acta 1765, 189–222.
Biagioli, M., Cipriani, S., Carino, A., Distrutti, E., Marchianò, S., and Fiorucci, S. 2017. Variability in industrial production affects probiotics activity: identification of batches of probiotic VSL#3 that increases intestinal permeability and worsens colitis in rodents. Gastroenterology 152, S969.
Boden, E.K. and Snapper, S.B. 2008. Regulatory T cells in inflammatory bowel disease. Curr. Opin. Gastroenterol. 24, 733–741.
Casellas, F., Borruel, N., Torrejon, A., Varela, E., Antolin, M., Guarner, F., and Malagelada, J.R. 2007. Oral oligofructose-enriched inulin supplementation in acute ulcerative colitis is well tolerated and associated with lowered faecal calprotectin. Aliment. Pharmacol. Ther. 25, 1061–1067.
Cherbut, C. 2002. Inulin and oligofructose in the dietary fibre concept. Br. J. Nutr. 87 Suppl 2, S159–S162.
Cinque, B., La Torre, C., Lombardi, F., Palumbo, P., Van der Rest, M., and Cifone, M.G. 2016. Production conditions affect the in vitro anti-tumoral effects of a high concentration multi-strain probiotic preparation. PLoS One 11, e0163216.
Cloetens, L., Ulmius, M., Johansson-Persson, A., Akesson, B., and Onning, G. 2012. Role of dietary beta-glucans in the prevention of the metabolic syndrome. Nutr. Rev. 70, 444–458.
Costello, S.P., Soo, W., Bryant, R.V., Jairath, V., Hart, A.L., and Andrews, J.M. 2017. Systematic review with meta-analysis: faecal microbiota transplantation for the induction of remission for active ulcerative colitis. Aliment. Pharmacol. Ther. 46, 213–224.
Daou, C. and Zhang, H. 2012. Oat beta-glucan: Its role in health promotion and prevention of diseases. Compr. Rev. Food Sci. F. 11, 355–365.
Derwa, Y., Gracie, D.J., Hamlin, P.J., and Ford, A.C. 2017. Systematic review with meta-analysis: the efficacy of probiotics in inflamma tory bowel disease. Aliment. Pharmacol. Ther. 46, 389–400.
Di Sabatino, A., Biancheri, P., Rovedatti, L., MacDonald, T.T., and Corazza, G.R. 2012. New pathogenic paradigms in inflammatory bowel disease. Inflamm. Bowel Dis. 18, 368–371.
Dos Reis, S.A., da Conceicao, L.L., Siqueira, N.P., Rosa, D.D., da Silva, L.L., and Peluzio, M.D. 2017. Review of the mechanisms of probiotic actions in the prevention of colorectal cancer. Nutr. Res. 37, 1–19.
Ewaschuk, J.B., Diaz, H., Meddings, L., Diederichs, B., Dmytrash, A., Backer, J., Looijer-van Langen, M., and Madsen, K.L. 2008. Secreted bioactive factors from Bifidobacterium infantis enhance epithelial cell barrier function. Am. J. Physiol. Gastrointest. Liver Physiol. 295, G1025–G1034.
Flamm, G., Glinsmann, W., Kritchevsky, D., Prosky, L., and Roberfroid, M. 2001. Inulin and oligofructose as dietary fiber: a review of the evidence. Crit. Rev. Food Sci. Nutr. 41, 353–362.
Forland, D.T., Johnson, E., Saetre, L., Lyberg, T., Lygren, I., and Hetland, G. 2011. Effect of an extract based on the medicinal mushroom Agaricus blazei murill on expression of cytokines and calprotectin in patients with ulcerative colitis and Crohn’s disease. Scand. J. Immunol. 73, 66–75.
Frolkis, A.D., Dykeman, J., Negron, M.E., Debruyn, J., Jette, N., Fiest, K.M., Frolkis, T., Barkema, H.W., Rioux, K.P., Panaccione, R., et al. 2013. Risk of surgery for inflammatory bowel diseases has decreased over time: a systematic review and meta-analysis of population-based studies. Gastroenterology 145, 996–1006.
Fukuda, S., Toh, H., Hase, K., Oshima, K., Nakanishi, Y., Yoshimura, K., Tobe, T., Clarke, J.M., Topping, D.L., Suzuki, T., et al. 2011. Bifidobacteria can protect from enteropathogenic infection through production of acetate. Nature 469, 543–547.
Fung, K.Y., Cosgrove, L., Lockett, T., Head, R., and Topping, D.L. 2012. A review of the potential mechanisms for the lowering of colorectal oncogenesis by butyrate. Br. J. Nutr. 108, 820–831.
Gaffen, S.L., Jain, R., Garg, A.V., and Cua, D.J. 2014. The IL-23-IL-17 immune axis: from mechanisms to therapeutic testing. Nat. Rev. Immunol. 14, 585–600.
Galvez, J. 2014. Role of Th17 cells in the pathogenesis of human IBD. ISRN Inflamm. 2014, 928461.
Gevers, D., Kugathasan, S., Denson, L.A., Vazquez-Baeza, Y., Van Treuren, W., Ren, B., Schwager, E., Knights, D., Song, S.J., Yassour, M., et al. 2014. The treatment-naive microbiome in new-onset Crohn’s disease. Cell Host Microbe 15, 382–392.
Gibson, G.R. and Roberfroid, M.B. 1995. Dietary modulation of the human colonic microbiota: introducing the concept of prebiotics. J. Nutr. 125, 1401–1412.
Gionchetti, P., Rizzello, F., Helwig, U., Venturi, A., Lammers, K.M., Brigidi, P., Vitali, B., Poggioli, G., Miglioli, M., and Campieri, M. 2003. Prophylaxis of pouchitis onset with probiotic therapy: a double-blind, placebo-controlled trial. Gastroenterology 124, 1202–1209.
Goodrich, J.K., Waters, J.L., Poole, A.C., Sutter, J.L., Koren, O., Blekhman, R., Beaumont, M., Van Treuren, W., Knight, R., Bell, J.T., et al. 2014. Human genetics shape the gut microbiome. Cell 159, 789–799.
Gopalakrishnan, A., Clinthorne, J.F., Rondini, E.A., McCaskey, S.J., Gurzell, E.A., Langohr, I.M., Gardner, E.M., and Fenton, J.I. 2012. Supplementation with galacto-oligosaccharides increases the percentage of NK cells and reduces colitis severity in Smad3-deficient mice. J. Nutr. 142, 1336–1342.
Goto, Y., Obata, T., Kunisawa, J., Sato, S., Ivanov, I.I., Lamichhane, A., Takeyama, N., Kamioka, M., Sakamoto, M., Matsuki, T., et al. 2014. Innate lymphoid cells regulate intestinal epithelial cell glycosylation. Science 345, 1254009.
Halfvarson, J., Brislawn, C.J., Lamendella, R., Vazquez-Baeza, Y., Walters, W.A., Bramer, L.M., D’Amato, M., Bonfiglio, F., McDonald, D., Gonzalez, A., et al. 2017. Dynamics of the human gut microbiome in inflammatory bowel disease. Nat. Microbiol. 2, 17004.
Holma, R., Juvonen, P., Asmawi, M.Z., Vapaatalo, H., and Korpela, R. 2002. Galacto-oligosaccharides stimulate the growth of bifidobacteria but fail to attenuate inflammation in experimental colitis in rats. Scand. J. Gastroenterol. 37, 1042–1047.
Hugot, J.P., Chamaillard, M., Zouali, H., Lesage, S., Cezard, J.P., Belaiche, J., Almer, S., Tysk, C., O’Morain, C.A., Gassull, M., et al. 2001. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn’s disease. Nature 411, 599–603.
Imhann, F., Vich Vila, A., Bonder, M.J., Fu, J., Gevers, D., Visschedijk, M.C., Spekhorst, L.M., Alberts, R., Franke, L., van Dullemen, H.M., et al. 2018. Interplay of host genetics and gut microbiota underlying the onset and clinical presentation of inflammatory bowel disease. Gut 67, 108–119.
Isene, R., Bernklev, T., Hoie, O., Munkholm, P., Tsianos, E., Stockbrugger, R., Odes, S., Palm, O., Smastuen, M., Moum, B., et al. 2015. Extraintestinal manifestations in Crohn’s disease and ulcerative colitis: results from a prospective, population-based European inception cohort. Scand. J. Gastroenterol. 50, 300–305.
Jensen, H., Dromtorp, S.M., Axelsson, L., and Grimmer, S. 2015. Immunomodulation of monocytes by probiotic and selected lactic acid bacteria. Probiotics Antimicrob. Proteins 7, 14–23.
Johnston, R.D. and Logan, R.F. 2008. What is the peak age for onset of IBD? Inflamm. Bowel Dis. 14 Suppl 2, S4–S5.
Kamada, N., Chen, G.Y., Inohara, N., and Nunez, G. 2013. Control of pathogens and pathobionts by the gut microbiota. Nat. Immunol. 14, 685–690.
Kaser, A., Martinez-Naves, E., and Blumberg, R.S. 2010. Endoplasmic reticulum stress: implications for inflammatory bowel disease pathogenesis. Curr. Opin. Gastroenterol. 26, 318–326.
Khoruts, A., Rank, K.M., Newman, K.M., Viskocil, K., Vaughn, B.P., Hamilton, M.J., and Sadowsky, M.J. 2016. Inflammatory bowel disease affects the outcome of fecal microbiota transplantation for recurrent Clostridium difficile infection. Clin. Gastroenterol. Hepatol. 14, 1433–1438.
Kim, C.H. 2009. FOXP3 and its role in the immune system. Adv. Exp. Med. Biol. 665, 17–29.
Kilinç, B., Cirik, S., Turan, G., Tekogul, H., and Koru, E. 2013. Seaweed for food and industrial applications, In Muzzalupo, I. (ed.), Food Industry. InTech, DOI: 10.5772/53172.
Kolmeder, C.A., Salojarvi, J., Ritari, J., de Been, M., Raes, J., Falony, G., Vieira-Silva, S., Kekkonen, R.A., Corthals, G.L., Palva, A., et al. 2016. Faecal metaproteomic analysis reveals a personalized and stable functional microbiome and limited effects of a probiotic intervention in adults. PLoS One 11, e0153294.
Kravtsov, E.G., Yermolayev, A.V., Anokhina, I.V., Yashina, N.V., Chesnokova, V.L., and Dalin, M.V. 2008. Adhesion characteristics of lactobacillus is a criterion of the probiotic choice. Bull. Exp. Biol. Med. 145, 232–234.
Kristensen, N.B., Bryrup, T., Allin, K.H., Nielsen, T., Hansen, T.H., and Pedersen, O. 2016. Alterations in fecal microbiota composition by probiotic supplementation in healthy adults: a systematic review of randomized controlled trials. Genome Med. 8, 52.
Landy, J., Ronde, E., English, N., Clark, S.K., Hart, A.L., Knight, S.C., Ciclitira, P.J., and Al-Hassi, H.O. 2016. Tight junctions in inflammatory bowel diseases and inflammatory bowel disease associated colorectal cancer. World J. Gastroenterol. 22, 3117–3126.
Lavi, I., Levinson, D., Peri, I., Nimri, L., Hadar, Y., and Schwartz, B. 2010. Orally administered glucans from the edible mushroom Pleurotus pulmonarius reduce acute inflammation in dextran sulfate sodium-induced experimental colitis. Br. J. Nutr. 103, 393–402.
Lean, Q.Y., Eri, R.D., Fitton, J.H., Patel, R.P., and Gueven, N. 2015. Fucoidan extracts ameliorate acute colitis. PLoS One 10, e0128453.
Li, H., Limenitakis, J.P., Fuhrer, T., Geuking, M.B., Lawson, M.A., Wyss, M., Brugiroux, S., Keller, I., Macpherson, J.A., Rupp, S., et al. 2015. The outer mucus layer hosts a distinct intestinal microbial niche. Nat. Commun. 6, 8292.
Licht, T.R., Hansen, M., Poulsen, M., and Dragsted, L.O. 2006. Die tary carbohydrate source influences molecular fingerprints of the rat faecal microbiota. BMC Microbiol. 6, 98.
Liu, T., Zhang, L., Joo, D., and Sun, S.C. 2017. NF-kappaB signaling in inflammation. Signal. Transduct. Target. Ther. 2, 17023.
Losurdo, G., Iannone, A., Contaldo, A., Ierardi, E., Di Leo, A., and Principi, M. 2015. Escherichia coli nissle 1917 in ulcerative colitis treatment: systematic review and meta-analysis. J. Gastrointestin. Liver Dis. 24, 499–505.
Luo, Y., de Lange, K.M., Jostins, L., Moutsianas, L., Randall, J., Kennedy, N.A., Lamb, C.A., McCarthy, S., Ahmad, T., Edwards, C., et al. 2017. Exploring the genetic architecture of inflammatory bowel disease by whole-genome sequencing identifies association at ADCY7. Nat. Genet. 49, 186–192.
Maldonado-Gomez, M.X., Martinez, I., Bottacini, F., O’Callaghan, A., Ventura, M., van Sinderen, D., Hillmann, B., Vangay, P., Knights, D., Hutkins, R.W., et al. 2016. Stable engraftment of Bifidobacterium iongum AH1206 in the human gut depends on individualized features of the resident microbiome. Cell Host Microbe 20, 515–526.
Marcobal, A., Southwick, A.M., Earle, K.A., and Sonnenburg, J.L. 2013. A refined palate: bacterial consumption of host glycans in the gut. Glycobiology 23, 1038–1046.
Marteau, P. and Flourie, B. 2001. Tolerance to low-digestible carbohydrates: symptomatology and methods. Br. J. Nutr. 85 Suppl 1, S17–S21.
Maslowski, K.M. and Mackay, C.R. 2011. Diet, gut microbiota and immune responses. Nat. Immunol. 12, 5–9.
Matsumoto, S., Nagaoka, M., Hara, T., Kimura-Takagi, I., Mistuyama, K., and Ueyama, S. 2004. Fucoidan derived from Cladosiphon okamuranus Tokida ameliorates murine chronic colitis through the down-regulation of interleukin-6 production on colonic epithelial cells. Clin. Exp. Immunol. 136, 432–439.
Mazurak, N., Broelz, E., Storr, M., and Enck, P. 2015. Probiotic therapy of the irritable bowel syndrome: Why is the evidence still poor and what can be done about it? J. Neurogastroenterol. Motil. 21, 471–485.
McIlroy, J., Ianiro, G., Mukhopadhya, I., Hansen, R., and Hold, G.L. 2018. Review article: the gut microbiome in inflammatory bowel disease-avenues for microbial management. Aliment. Pharmacol. Ther. 47, 26–42.
Mimura, T., Rizzello, F., Helwig, U., Poggioli, G., Schreiber, S., Talbot, I.C., Nicholls, R.J., Gionchetti, P., Campieri, M., and Kamm, M.A. 2004. Once daily high dose probiotic therapy (VSL#3) for maintaining remission in recurrent or refractory pouchitis. Gut 53, 108–114.
Molodecky, N.A., Soon, I.S., Rabi, D.M., Ghali, W.A., Ferris, M., Chernoff, G., Benchimol, E.I., Panaccione, R., Ghosh, S., Barkema, H.W., et al. 2012. Increasing incidence and prevalence of the inflammatory bowel diseases with time, based on systematic review. Gastroenterology 142, 46–54 e42; quiz e30.
Mussatto, S.I. and Mancilha, I.M. 2007. Non-digestible oligosaccharides: A review. Carbohydrate Polymers 68, 587–597.
Najafzadeh, M., Reynolds, P.D., Baumgartner, A., Jerwood, D., and Anderson, D. 2007. Chaga mushroom extract inhibits oxidative DNA damage in lymphocytes of patients with inflammatory bowel disease. Biofactors 31, 191–200.
Ng, K.M., Ferreyra, J.A., Higginbottom, S.K., Lynch, J.B., Kashyap, P.C., Gopinath, S., Naidu, N., Choudhury, B., Weimer, B.C., Monack, D.M., et al. 2013a. Microbiota-liberated host sugars facilitate post-antibiotic expansion of enteric pathogens. Nature 502, 96–99.
Ng, S.C., Tang, W., Ching, J.Y., Wong, M., Chow, C.M., Hui, A.J., Wong, T.C., Leung, V.K., Tsang, S.W., Yu, H.H., et al. 2013b. Incidence and phenotype of inflammatory bowel disease based on results from the Asia-pacific Crohn’s and colitis epidemiology study. Gastroenterology 145, 158–165.e2.
O’Shea, C.J., O’Doherty, J.V., Callanan, J.J., Doyle, D., Thornton, K., and Sweeney, T. 2016. The effect of algal polysaccharides laminarin and fucoidan on colonic pathology, cytokine gene expression and Enterobacteriaceae in a dextran sodium sulfate-challenged porcine model. J. Nutr. Sci. 5, e15.
O’Sullivan, L., Murphy, B., McLoughlin, P., Duggan, P., Lawlor, P.G., Hughes, H., and Gardiner, G.E. 2010. Prebiotics from marine macroalgae for human and animal health applications. Mar. Drugs 8, 2038–2064.
Ogura, Y., Bonen, D.K., Inohara, N., Nicolae, D.L., Chen, F.F., Ramos, R., Britton, H., Moran, T., Karaliuskas, R., Duerr, R.H., et al. 2001. A frameshift mutation in NOD2 associated with susceptibility to Crohn’s disease. Nature 411, 603–606.
Okolie, C.L., Rajendran, S.R.C.K., Udenigwe, C.C., Aryee, A.N.A., and Mason, B. 2017. Prospects of brown seaweed polysaccharides (BSP) as prebiotics and potential immunomodulators. J. Food Biochem. 41, e12392.
Ouwerkerk, J.P., de Vos, W.M., and Belzer, C. 2013. Glycobiome: bacteria and mucus at the epithelial interface. Best Pract. Res. Clin. Gastroenterol. 27, 25–38.
Pacheco, A.R., Barile, D., Underwood, M.A., and Mills, D.A. 2015. The impact of the milk glycobiome on the neonate gut microbiota. Annu. Rev. Anim. Biosci. 3, 419–445.
Packey, C.D. and Sartor, R.B. 2008. Interplay of commensal and pathogenic bacteria, genetic mutations, and immunoregulatory defects in the pathogenesis of inflammatory bowel diseases. J. Intern. Med. 263, 597–606.
Piche, T., des Varannes, S.B., Sacher-Huvelin, S., Holst, J.J., Cuber, J.C., and Galmiche, J.P. 2003. Colonic fermentation influences lower esophageal sphincter function in gastroesophageal reflux disease. Gastroenterology 124, 894–902.
Pickard, J.M., Maurice, C.F., Kinnebrew, M.A., Abt, M.C., Schenten, D., Golovkina, T.V., Bogatyrev, S.R., Ismagilov, R.F., Pamer, E.G., Turnbaugh, P.J., et al. 2014. Rapid fucosylation of intestinal epithelium sustains host-commensal symbiosis in sickness. Nature 514, 638–641.
Pigneur, B. and Sokol, H. 2016. Fecal microbiota transplantation in inflammatory bowel disease: the quest for the holy grail. Mucosal. Immunol. 9, 1360–1365.
Powrie, F., Leach, M.W., Mauze, S., Menon, S., Caddle, L.B., and Coffman, R.L. 1994. Inhibition of Th1 responses prevents inflammatory bowel disease in scid mice reconstituted with CD45RBhi CD4+ T cells. Immunity 1, 553–562.
Rios-Covian, D., Ruas-Madiedo, P., Margolles, A., Gueimonde, M., de Los Reyes-Gavilan, C.G., and Salazar, N. 2016. Intestinal short chain fatty acids and their link with diet and human health. Front. Microbiol. 7, 185.
Rivero-Urgell, M. and Santamaria-Orleans, A. 2001. Oligosaccharides: application in infant food. Early Hum. Dev. 65 Suppl, S43–S52.
Roberfroid, M.B. 2000. Prebiotics and probiotics: are they functional foods? Am. J. Clin. Nutr. 71, S1682–S1687; discussion S1688–S1690.
Sadowsky, M.J., Staley, C., Heiner, C., Hall, R., Kelly, C.R., Brandt, L., and Khoruts, A. 2017. Analysis of gut microbiota -An ever changing landscape. Gut Microbes 8, 268–275.
Sanchez, B., Delgado, S., Blanco-Miguez, A., Lourenco, A., Gueimonde, M., and Margolles, A. 2017. Probiotics, gut microbiota, and their influence on host health and disease. Mol. Nutr. Food Res. 61, 1600240.
Sanders, M.E. 2008. Probiotics: definition, sources, selection, and uses. Clin Infect Dis 46 Suppl 2, S58–S61; discussion S144–S151.
Sanders, M.E. 2016. Probiotics and microbiota composition. BMC Med. 14, 82.
Sangwan, V., Tomar, S.K., Singh, R.R., Singh, A.K., and Ali, B. 2011. Galactooligosaccharides: novel components of designer foods. J. Food Sci. 76, R103–R111.
Senthilkumar, K., Manivasagan, P., Venkatesan, J., and Kim, S.K. 2013. Brown seaweed fucoidan: biological activity and apoptosis, growth signaling mechanism in cancer. Int. J. Biol. Macromol. 60, 366–374.
Shanahan, F. 2017. Editorial: probiotics in inflammatory bowel disease-wrong organisms, wrong disease, or flawed concepts? Aliment. Pharmacol. Ther. 46, 632–633.
Shang, L., Fukata, M., Thirunarayanan, N., Martin, A.P., Arnaboldi, P., Maussang, D., Berin, C., Unkeless, J.C., Mayer, L., Abreu, M.T., et al. 2008. Toll-like receptor signaling in small intestinal epithelium promotes B-cell recruitment and IgA production in lamina propria. Gastroenterology 135, 529–538.
Shi, L., Lin, Q., Yang, T., Nie, Y., Li, X., Liu, B., Shen, J., Liang, Y., Tang, Y., and Luo, F. 2016. Oral administration of Lentinus edodes beta-glucans ameliorates DSS-induced ulcerative colitis in mice via MAPK-Elk-1 and MAPK-PPARgamma pathways. Food Funct. 7, 4614–4627.
Sicard, J.F., Le Bihan, G., Vogeleer, P., Jacques, M., and Harel, J. 2017. Interactions of intestinal bacteria with components of the intestinal mucus. Front. Cell. Infect. Microbiol. 7, 387.
Slavin, J. 2013. Fiber and prebiotics: mechanisms and health benefits. Nutrients 5, 1417–1435.
Sonnenburg, E.D., Zheng, H., Joglekar, P., Higginbottom, S.K., Firbank, S.J., Bolam, D.N., and Sonnenburg, J.L. 2010. Specificity of polysaccharide use in intestinal bacteroides species determines diet-induced microbiota alterations. Cell 141, 1241–1252.
Staley, C., Kelly, C.R., Brandt, L.J., Khoruts, A., and Sadowsky, M.J. 2016. Complete microbiota engraftment is not essential for recovery from recurrent Clostridium difficile infection following fecal microbiota transplantation. MBio 7, e01965–16.
Strober, W. and Fuss, I.J. 2011. Proinflammatory cytokines in the pathogenesis of inflammatory bowel diseases. Gastroenterology 140, 1756–1767.
Sun, Y. and O’Riordan, M.X. 2013. Regulation of bacterial pathogenesis by intestinal short-chain fatty acids. Adv. Appl. Microbiol. 85, 93–118.
Sunkara, L.T., Jiang, W., and Zhang, G. 2012. Modulation of antimicrobial host defense peptide gene expression by free fatty acids. PLoS One 7, e49558.
Swennen, K., Courtin, C.M., and Delcour, J.A. 2006. Non-digestible oligosaccharides with prebiotic properties. Crit. Rev. Food Sci. Nutr. 46, 459–471.
Takaishi, H., Matsuki, T., Nakazawa, A., Takada, T., Kado, S., Asahara, T., Kamada, N., Sakuraba, A., Yajima, T., Higuchi, H., et al. 2008. Imbalance in intestinal microflora constitution could be involved in the pathogenesis of inflammatory bowel disease. Int. J. Med. Microbiol. 298, 463–472.
Ten Bruggencate, S.J., Bovee-Oudenhoven, I.M., Lettink-Wissink, M.L., Katan, M.B., and Van Der Meer, R. 2004. Dietary fructooligosaccharides and inulin decrease resistance of rats to salmonella: protective role of calcium. Gut 53, 530–535.
Tojo, R., Suarez, A., Clemente, M.G., de los Reyes-Gavilan, C.G., Margolles, A., Gueimonde, M., and Ruas-Madiedo, P. 2014. Intestinal microbiota in health and disease: role of bifidobacteria in gut homeostasis. World J. Gastroenterol. 20, 15163–15176.
Vahabnezhad, E., Mochon, A.B., Wozniak, L.J., and Ziring, D.A. 2013. Lactobacillus bacteremia associated with probiotic use in a pediatric patient with ulcerative colitis. J. Clin. Gastroenterol. 47, 437–439.
Van den Abbeele, P., Belzer, C., Goossens, M., Kleerebezem, M., De Vos, W.M., Thas, O., De Weirdt, R., Kerckhof, F.M., and Van de Wiele, T. 2013. Butyrate-producing Clostridium cluster XIVa species specifically colonize mucins in an in vitro gut model. ISME J. 7, 949–961.
Van der Sluis, M., De Koning, B.A., De Bruijn, A.C., Velcich, A., Meijerink, J.P., Van Goudoever, J.B., Buller, H.A., Dekker, J., Van Seuningen, I., Renes, I.B., et al. 2006. Muc2-deficient mice spontaneously develop colitis, indicating that MUC2 is critical for colonic protection. Gastroenterology 131, 117–129.
Verghese, M., Walker, L.T., Shackelford, L., and Chawan, C.B. 2005. Inhibitory effects of nondigestible carbohydrates of different chain lengths on azoxymethane-induced aberrant crypt foci in Fisher 344 rats. Nutr. Res. 25, 859–868.
Videla, S., Vilaseca, J., Antolin, M., Garcia-Lafuente, A., Guarner, F., Crespo, E., Casalots, J., Salas, A., and Malagelada, J.R. 2001. Dietary inulin improves distal colitis induced by dextran sodium sulfate in the rat. Am. J. Gastroenterol. 96, 1486–1493.
Weingarden, A., Gonzalez, A., Vazquez-Baeza, Y., Weiss, S., Humphry, G., Berg-Lyons, D., Knights, D., Unno, T., Bobr, A., Kang, J., et al. 2015. Dynamic changes in short-and long-term bacterial composition following fecal microbiota transplantation for recurrent Clostridium difficile infection. Microbiome 3, 10.
Wells, M.L., Potin, P., Craigie, J.S., Raven, J.A., Merchant, S.S., Helliwell, K.E., Smith, A.G., Camire, M.E., and Brawley, S.H. 2017. Algae as nutritional and functional food sources: revisiting our understanding. J. Appl. Phycol. 29, 949–982.
Whelan, K. and Quigley, E.M. 2013. Probiotics in the management of irritable bowel syndrome and inflammatory bowel disease. Curr. Opin. Gastroenterol. 29, 184–189.
Yamamoto, S. and Ma, X. 2009. Role of Nod2 in the development of Crohn’s disease. Microbes Infect. 11, 912–918.
Yamamoto, A., Itoh, T., Nasu, R., and Nishida, R. 2013. Effect of sodium alginate on dextran sulfate sodium-and 2,4,6-trinitrobenzene sulfonic acid-induced experimental colitis in mice. Pharmacology 92, 108–116.
Yang, S.K., Yun, S., Kim, J.H., Park, J.Y., Kim, H.Y., Kim, Y.H., Chang, D.K., Kim, J.S., Song, I.S., Park, J.B., et al. 2008. Epidemiology of inflammatory bowel disease in the Songpa-Kangdong district, Seoul, Korea, 1986-2005: a KASID study. Inflamm. Bowel Dis. 14, 542–549.
Zenewicz, L.A., Antov, A., and Flavell, R.A. 2009. CD4 T-cell differentiation and inflammatory bowel disease. Trends Mol. Med. 15, 199–207.
Zhu, Y., Michelle Luo, T., Jobin, C., and Young, H.A. 2011. Gut microbiota and probiotics in colon tumorigenesis. Cancer Lett. 309, 119–127.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Eom, T., Kim, Y.S., Choi, C.H. et al. Current understanding of microbiota- and dietary-therapies for treating inflammatory bowel disease. J Microbiol. 56, 189–198 (2018). https://doi.org/10.1007/s12275-018-8049-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12275-018-8049-8