Abstract
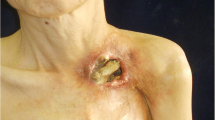
Rib-sternal osteoradionecrosis is a rare but serious complication of chest radiotherapy. No consensus-based method of managing deep sternal wounds that develop after radiotherapy is available. Usually patients require long-term antibiotics. The surgical placement of a muscle, an omental flap, or a prosthesis is described. We report, in pictures, four successful omental flap placements. Between March 2015 and July 2018, four women with deep sternal wound injuries that developed after radiation therapy to treat breast cancer underwent rib-sternal reconstruction with omental flap placement. The first signs of infected radionecrosis developed 28.5 years after radiotherapy. Despite prolonged antibiotic treatment, surgery was necessary. The mean age at surgery was 76 years (range: 62–86 years). All necrotic tissue was excised and debridement was performed before the placement of a pedicled omental flap dissected along the transverse colon and raised through a subcutaneous tunnel. No skin graft or osteosynthesis was required. After surgery, lubricated bandages were applied daily, and antibiotics were prescribed for a few weeks. Complete healing was obtained after surgery without clinical complication. Our experience suggests that a pedicled omental flap is an affordable, simple, and very useful option for reconstructing deep rib-sternal wounds caused by radiation.



Similar content being viewed by others
Availability of Data and Material
Yes
Code Availability
Not applicable
References
Lorette G, Machet L (2001) [Lésions cutanées induites par la radiothérapie: prévention, traitements] French. Cancer/Radiothérapie 5:116s–120s
Wong RKS, Bensadoun R-J, Boers-Doets CB, Bryce J, Chan A, Epstein JB et al (2013) Clinical practice guidelines for the prevention and treatment of acute and late radiation reactions from the MASCC Skin Toxicity Study Group. Support Care Cancer 21(10):2933–2948
Giridhar P, Mallick S, Rath GK, Julka PK (2015) Radiation induced lung injury: prediction, assessment and management. Asian Pac J Cancer Prev APJCP. 16(7):2613–2617
Bledsoe TJ, Nath SK, Decker RH (2017) Radiation Pneumonitis. Clin Chest Med. 38(2):201–208
Darby IA, Laverdet B, Bonté F, Desmoulière A (2014) Fibroblasts and myofibroblasts in wound healing. Clin Cosmet Investig Dermatol 7:301–311
Kiricuta I (1963) The use of the great omentum in the surgery of breast cancer. Presse Med 71:15–17
Ferron G, Garrido I, Martel P, Gesson-Paute A, Classe J-M, Letourneur B et al (2007) Combined laparoscopically harvested omental flap with meshed skin grafts and vacuum-assisted closure for reconstruction of complex chest wall defects. Ann Plast Surg 58(2):150–155
Liebermann-Meffert D (2000) The greater omentum. Anatomy, embryology, and surgical applications. Surg Clin North Am 80(1):275–293 xii
Zhang QX, Magovern CJ, Mack CA, Budenbender KT, Ko W, Rosengart TK (1997) Vascular endothelial growth factor is the major angiogenic factor in omentum: mechanism of the omentum-mediated angiogenesis. J Surg Res 67(2):147–154
Goldsmith HS (1994) Brain and spinal cord revascularization by omental transposition. Neurol Res 16(3):159–162
Sigrist S, Mechine-Neuville A, Mandes K, Calenda V, Legeay G, Bellocq J-P et al (2003) Induction of angiogenesis in omentum with vascular endothelial growth factor: influence on the viability of encapsulated rat pancreatic islets during transplantation. J Vasc Res 40(4):359–367
Hammerman MR (2004) Renal organogenesis from transplanted metanephric primordia. J Am Soc Nephrol JASN 15(5):1126–1132
Bellier J, Jayle C, Sage E, Glorion M, Puyo P, Couturaud B, et al. Épiplooplastie de recouvrement après résection de la paroi thoracique pour ostéoradionécrose sternale. JCTCV:21(1). 2017 [cité 22 nov 2020]; Disponible sur: http://journal.sfctcv.org/2017/03/epiplooplastie-de-recouvrement-apres-resection-de-la-paroi-thoracique-pour-osteoradionecrose-sternale-2/
Rouanet P, Fabre JM, Tica V, Anaf V, Jozwick M, Pujol H (1995) Chest wall reconstruction for radionecrosis after breast carcinoma therapy. Ann Plast Surg 34(5):465–470
Hultman CS, Carlson GW, Losken A, Jones G, Culbertson J, Mackay G et al (2002) Utility of the omentum in the reconstruction of complex extraperitoneal wounds and defects: donor-site complications in 135 patients from 1975 to 2000. Ann Surg 235(6):782–795
Cohen M, Ramasastry SS (1996) Reconstruction of complex chest wall defects. Am J Surg 172(1):35–40
Vairinho A, Al Hindi A, Revol M, Legras A, Rem K, Guenane Y et al (2018) Reconstruction of an anterior chest wall radionecrosis defect by a contralateral latissimus dorsi flap: a case report. Ann Chir Plast Esthet 63(2):182–186
Ha JH, Park SO, Chang H, Jin US (2018) Optimal reconstruction method for large radionecrosis following breast cancer treatment: utility of free transverse rectus abdominis myocutaneous flap using contralateral internal mammary artery as recipient. Ann Plast Surg. 81(5):584–590
Chang EI, Chang EI, Soto-Miranda MA, Nosrati N, Robb GL, Chang DW (2013) Demystifying the use of internal mammary vessels as recipient vessels in free flap breast reconstruction. Plast Reconstr Surg 132(4):763–768
Lee CD, Butterworth J, Stephens RE, Wright B, Surek C (2018) Location of the internal mammary vessels for microvascular autologous breast reconstruction: the « 1-2-3 Rule ». Plast Reconstr Surg. 142(1):28–36
Engel H, Pelzer M, Sauerbier M, Germann G, Heitmann C (2007) An innovative treatment concept for free flap reconstruction of complex central chest wall defects—the cephalic-thoraco-acromial (CTA) loop. Microsurgery. 27(5):481–486
Valença-Filipe R, Horta R, Costa J, Carvalho J, Martins A, Silva Á (2014) Multi-staged flap reconstruction for complex radiation thoracic ulcer. Int J Surg Case Rep 5(12):1210–1213
Aquilina D, Darmanin FX, Briffa J, Gatt D (2009) Chest wall reconstruction using an omental flap and Integra. J Plast Reconstr Aesthet Surg 62(7):e200–e202
Dast S, Assaf N, Dessena L, Almousawi H, Herlin C, Berna P et al (2016) Change of paradigm in thoracic radionecrosis management. Ann Chir Plast Esthét 61(3):200–205
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics Approval
This is an observational study. The Research Ethics Committee has confirmed that no ethical approval is required.
Consent to Participate
Informed consent was obtained from all individual participants included in the study.
Consent for Publication
Patients signed informed consent regarding publishing their data and photographs.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Belaroussi, Y., Hustache-castaing, R., Jougon, J. et al. Management of Osteoradionecrosis of the Anterior Thoracic Wall Using Omental Flaps: a Prospective Case Series and Literature Review. Indian J Surg 84, 110–116 (2022). https://doi.org/10.1007/s12262-021-02835-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12262-021-02835-w