Abstract
Objectives
To compare the clinical profile and short-term outcome of children with axonal and demyelinating subtypes of childhood Guillain Barré syndrome (GBS).
Methods
This is a prospective observational study conducted in a tertiary care teaching hospital in North India. Consecutive children with Guillain Barré syndrome were recruited to compare the clinical profile and short term outcome among the subtypes.
Results
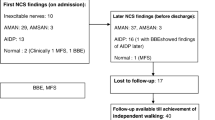
Among 9847 children admitted to the emergency, 95 had acute flaccid paralysis; 57 of whom had GBS. Electrophysiological studies were completed in 57; of whom 20 had acute inflammatory demyelinating polyneuropathy (AIDP); 19 had acute motor axonal neuropathy (AMAN); 12 had non-reactive nerves; five were unclassifiable; 1 had acute motor sensory axonal neuropathy (AMSAN). More children in AMAN group had preceding gastroenteritis (4 vs. 2), while AIDP group had upper respiratory infections (12 vs. 7). Ataxia was only seen in AIDP subtype while wrist drop, foot drop and hyperreflexia were seen only with AMAN subtype. Respiratory muscle involvement (6 vs. 3) and artificial ventilation (5 vs. 2) was more in AMAN. At discharge, children with AIDP were less likely to be non-ambulant (12 vs. 6, p = 0.036). Mean disability scores at hospital discharge (4.9 ± 1.2 vs. 4 ± 0.9, p = 0.015) and at last follow-up (0.7 ± 1.01 vs. 0.05 ± 0.2, p = 0.016) were higher in AMAN. Children with AIDP were more likely to achieve normalcy on follow-up (19 vs. 12, p = 0.023).
Conclusions
Children with AMAN appear to have a more severe clinical course; higher short-term morbidity; and slower recovery than those with AIDP.

Similar content being viewed by others
References
van den Berg B, Walgaard C, Drenthen J, Fokke C, Jacobs BC, van Doorn PA. Guillain-Barré syndrome: pathogenesis, diagnosis, treatment and prognosis. Nat Rev Neurol. 2014;10:469–82.
Yuki N, Hartung H-P. Guillain-Barré syndrome. N Engl J Med. 2012;366:2294–304.
Kalita J, Kumar M, Misra UK. Prospective comparison of acute motor axonal neuropathy and acute inflammatory demyelinating polyradiculoneuropathy in 140 children with Guillain-Barré syndrome in India. Muscle Nerve. 2017;57:761–5.
Kalra V, Sankhyan N, Sharma S, Gulati S, Choudhry R, Dhawan B. Outcome in childhood Guillain-Barré syndrome. Indian J Pediatr. 2009;76:795–9.
Sankhyan N, Sharma S, Konanki R, Gulati S. Childhood Guillain-Barré syndrome subtypes in northern India. J Clin Neurosci. 2014;21:427–30.
van Doorn PA, Ruts L, Jacobs BC. Clinical features, pathogenesis, and treatment of Guillain-Barré syndrome. Lancet Neurol. 2008;7:939–50.
Darras BT, Jones HR, Ryan MM, De Vivo DC. Neuromuscular disorders of infancy, childhood, and adolescence: a clinician’s approach [internet]. 2015 [cited 2017 Nov 7]. Available at: https://www.clinicalkey.com/dura/browse/bookChapter/3-s2.0-C20130000771
Van der Meché FG, Van Doorn PA, Meulstee J, Jennekens FG; GBS-consensus group of the Dutch Neuromuscular Research Support Centre. Diagnostic and classification criteria for the Guillain-Barré syndrome. Eur Neurol. 2001;45:133–9.
Hughes RAC, Cornblath DR. Guillain-Barré syndrome. Lancet. 2005;366:1653–66.
Korinthenberg R, Mönting JS. Natural history and treatment effects in Guillain-Barré syndrome: a multicentre study. Arch Dis Child. 1996;74:281–7.
Nachamkin I, Arzarte Barbosa P, Barbosa PA, et al. Patterns of Guillain-Barré syndrome in children: results from a Mexican population. Neurology. 2007;69:1665–71.
Ramírez-Zamora M, Burgos-Ganuza CR, Alas-Valle DA, Vergara-Galán PE, Ortez-González CI. Guillain-Barré syndrome in the paediatric age: epidemiological, clinical and therapeutic profile in a hospital in El Salvador. Rev Neurol. 2009;48:292–6.
Ye Y-Q, Wang K-R, Sun L, Wang Z. Clinical and electrophysiologic features of childhood Guillain-Barré syndrome in Northeast China. J Formos Med Assoc Taiwan Yi Zhi. 2014;113:634–9.
Nagasawa K, Kuwabara S, Misawa S, et al. Electrophysiological subtypes and prognosis of childhood Guillain-Barré syndrome in Japan. Muscle Nerve. 2006;33:766–70.
Kuwabara S, Yuki N. Axonal Guillain-Barré syndrome: concepts and controversies. Lancet Neurol. 2013;12:1180–8.
Uncini A, Manzoli C, Notturno F, Capasso M. Pitfalls in electrodiagnosis of Guillain-Barré syndrome subtypes. J Neurol Neurosurg Psychiatry. 2010;81:1157–63.
Rajabally YA, Durand M-C, Mitchell J, Orlikowski D, Nicolas G. Electrophysiological diagnosis of Guillain-Barré syndrome subtype: could a single study suffice? J Neurol Neurosurg Psychiatry. 2015;86:115–9.
Author information
Authors and Affiliations
Contributions
PKG: Patient management, data collection and prepared the first draft of the manuscript; PS: Patient management, critical review of manuscript; SS: Patient management, concept of the study, critical review of manuscript; AK: Patient management, review of literature and revision of the manuscript; NS: Concept of the study, supervised data collection, critical review of manuscript and final approval of the version to be published. He will act as guarantor for the paper.
Corresponding author
Ethics declarations
Conflict of Interest
None.
Source of Funding
None.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gupta, P.K., Singhi, P., Singhi, S. et al. How Different is AMAN from AIDP in Childhood GBS? A Prospective Study from North India. Indian J Pediatr 86, 329–334 (2019). https://doi.org/10.1007/s12098-018-2835-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12098-018-2835-5